Singapore sees increase in breast cancer cases but fewer deaths
Published: 10 Mar 2026
 ©David Stanciu via Canva.com
©David Stanciu via Canva.com
A new analysis from the Global Burden of Disease (GBD) Study, published in The Lancet Oncology, projects that global breast cancer cases will rise by one-third, from 2.3 million in 2023 to more than 3.5 million in 2050. Annual deaths are expected to increase from 764,000 in 2023 to nearly 1.4 million in 2050, with the heaviest toll falling on lower-resource countries.
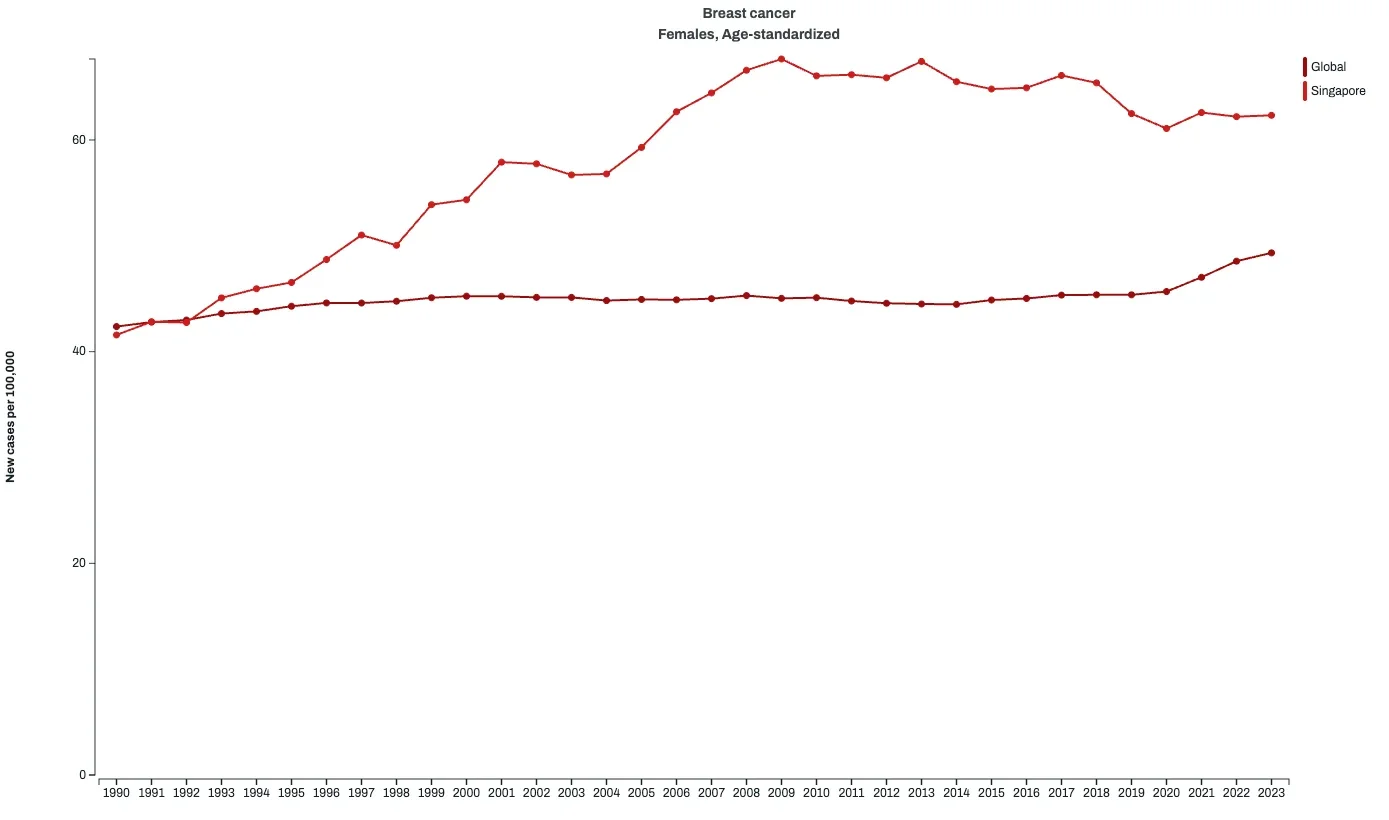
Fig 1: Global & Singapore Breast Cancer Incidence Rate (Age-Standardised)
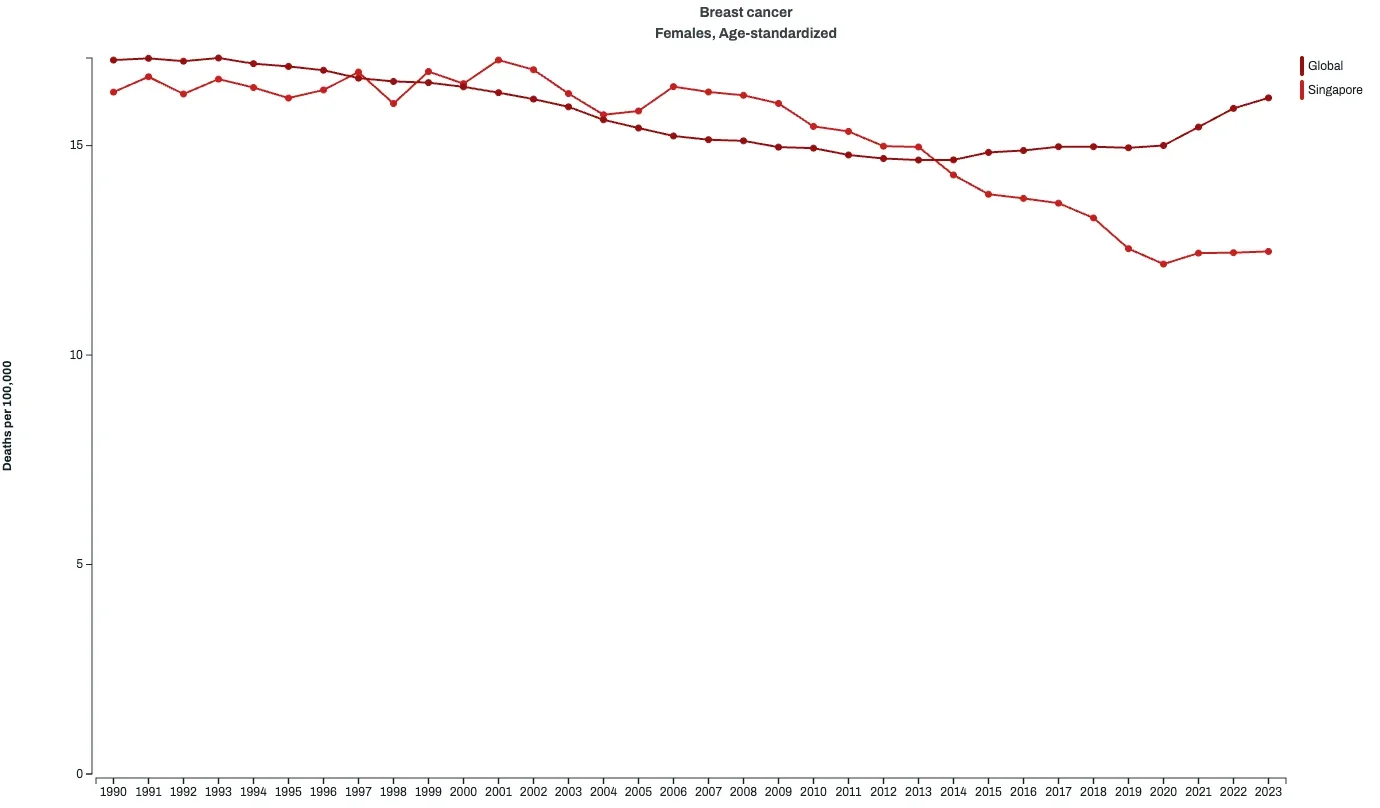
Fig 2: Global and Singapore Mortality Rate (Age-Standardised)
Against this global backdrop, Singapore presents a distinct but instructive picture: rising incidence, but falling mortality. Globally, the estimated age-standardised incidence rate (ASIR) rose modestly from 42.4 per 100,000 women in 1990 to 49.3 per 100,000 women in 2023 (based on both resident and non-resident population), and is projected to remain around this level through 2050. In Singapore, however, incidence has risen more sharply, from 41.58 per 100,000 women in 1990 to 62.33 per 100,000 women in 2023.
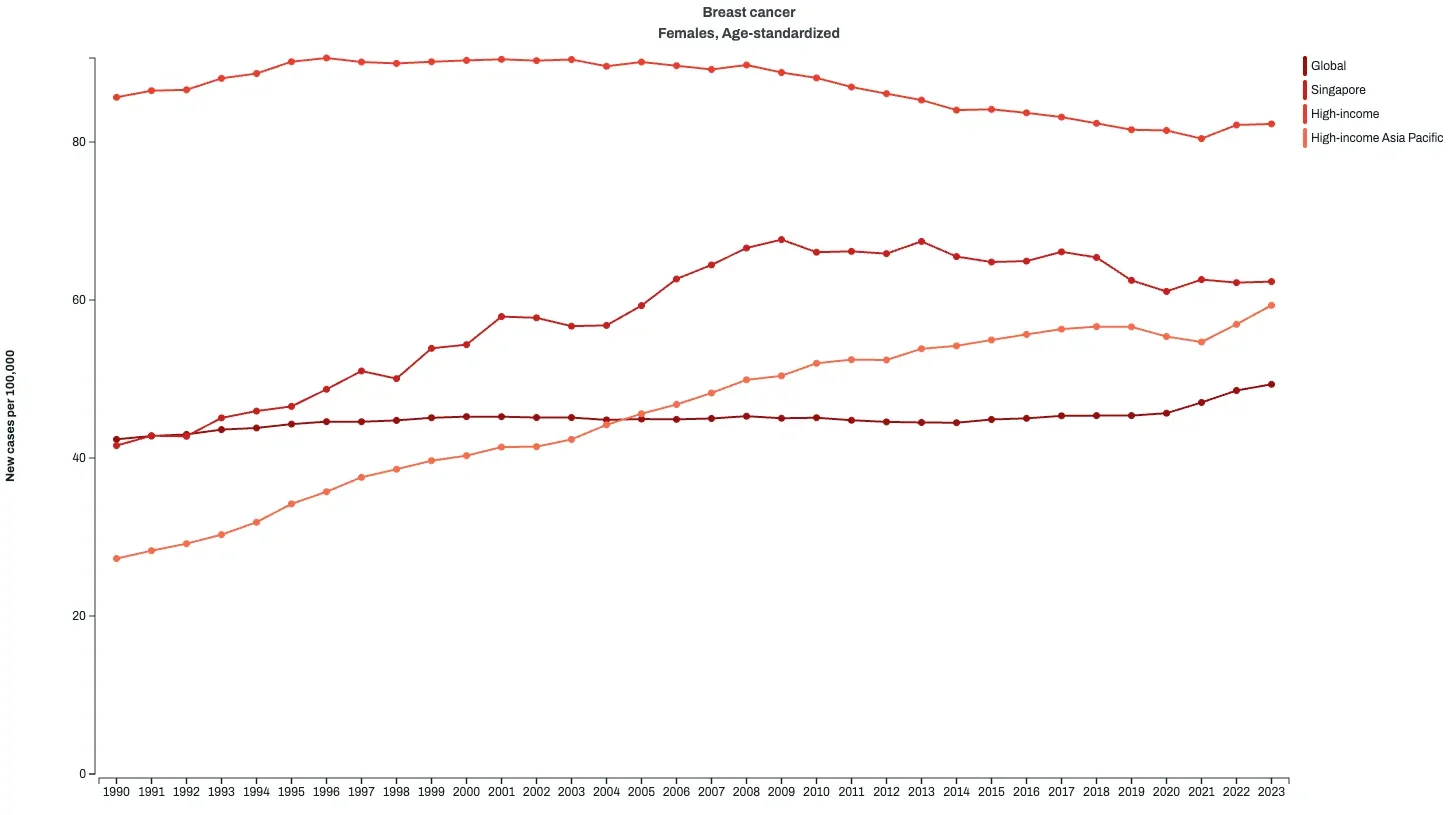
Fig 3: Global, High-Income Countries, High-Income Countries in Asia Pacific, and Singapore Breast Cancer Incidence Rate (Age-Standardised)
Although Singapore’s incidence rate is below the World Bank high-income group average, it ranks lower than Japan but higher than Brunei and South Korea within the High-Income Asia Pacific group. Singapore’s breast cancer trends mirror global findings: ASIR tends to be higher in high-income countries, where screening coverage and longer life expectancy increase detection. Age-specific trends in Singapore show notable rises among women aged 65 and above, which is consistent with Singapore’s ageing population.
“Breast cancer is a significant challenge for women marked by global inequity. Its impact is felt the most in lower-income countries, where diagnoses tend to occur later and access to care is more limited, which leads to higher mortality,” said Associate Professor Marie Ng from the Yong Loo Lin School of Medicine, National University of Singapore (NUS Medicine) and Director, NUS-IHME GBD Research Centre, based at NUS Medicine. Assoc Prof Marie Ng is the co-senior author of the study.
Demographic and reproductive shifts also help explain the rise in breast cancer rates:
- Median age at first birth increased from 27.5 years (1990) to 31.6 years (2024)
- Total fertility rate declined from 1.77 (1990) to 1.02 (2023)
Later pregnancies and fewer births could be linked to increased breast cancer risk factors. These shifts are typical of advanced economies, reinforcing Singapore’s alignment with broader high-income epidemiological patterns. Globally, however, the fastest growth in incidence is occurring in low-income countries, where age-standardised incidence has risen by 147% (on average) since 1990, which highlights widening global inequalities.
Mortality: Singapore’s divergence from global inequalities
Globally, age-standardised mortality rates (ASMR) declined slightly from 17.0 per 100,000 in 1990 to 16.1 in 2023, but this masks divergence:
- In high-income countries, mortality fell by about 30%
- In low-income countries, mortality nearly doubled
Singapore’s mortality trajectory aligns with the positive high-income trend. Between 2013 and 2023, Singapore’s ASMR fell from 14.97 to 12.47 per 100,000, a 16.7% decline. In 2023, Singapore’s mortality rate of 12.47 was substantially lower than the global average of 16.14 per 100,000. Across nearly every five-year age group, Singapore’s mortality rates were below global levels, reflecting earlier diagnosis and better access to treatments and interventions.
Long-term survival gains are striking. The five-year relative survival rate improved from 49.9% (1973–1977) to 84.2% (2019–2023).
The launch of BreastScreen Singapore in 2002 marked a turning point. Today, 56.3% of cases are diagnosed at Stage I, compared to 33% a decade earlier. While globally the burden of years of healthy life lost has doubled to 24 million years since 1990, with low- and lower-middle-income countries accounting for a disproportionate share, Singapore’s data suggest that strong and robust health systems can mitigate mortality even when incidence rises.
The GBD study also highlights prevention opportunities. Globally, 28% of breast cancer burden (~6.8 million healthy life years lost) in 2023 was linked to six modifiable risk factors:
- High red meat consumption (largest contributor)
Encouragingly, the global burden linked to tobacco and alcohol has declined since 1990, but other metabolic risk factors have not shown similar progress. These findings carry relevance for Singapore, where rising rates of obesity, diabetes, and sedentary lifestyles remain public health concerns. As a highly urbanised society undergoing rapid lifestyle transitions, Singapore sits at the intersection of demographic and metabolic risk trends identified globally.
Breast cancer remains the leading cause of cancer death among women in Singapore. However, the country’s declining mortality and improved survival contrast sharply with worsening outlook in lower-resource areas. A combination of sustained screening participation, early stage detection, modification of lifestyle risk factors and access to treatment have enabled Singapore’s breast cancer survival rates to increase.
“Singapore’s experience offers two important lessons. As countries undergo economic development and demographic transition, breast cancer incidence can rise. However, strong screening programmes and universal access to high-quality care are shifting the burden from mortality to morbidity, people are living longer, but with suboptimal health,” said Assoc Prof Ng.
“To curb the growing burden of breast cancer in Singapore and globally, we must address known risk factors through effective public health policies, making healthier choices more accessible, and supporting individuals to act against obesity and high blood sugar. Mammography is widely available in both public and private primary care settings across Singapore, with increased accessibility through Healthier SG efforts. Prevention, early detection, and access to care must go hand in hand,” added Dr Alicia Ong Huiying, Adjunct Lecturer from the Division of Family Medicine, Department of Medicine, NUS Medicine, and Family Physician, Associate Consultant at National University Polyclinics. Dr Ong is a co-author of the study.
The message from both Singapore and the global data is clear: rising incidence does not have to mean rising mortality, but preventing widening global disparities will require coordinated public health action, investment in health systems, and sustained political will.
If you’re interested in the datasets that IHME has for this, head here: https://ghdx.healthdata.org/record/ihme-data/gbd-2023-breast-cancer-forecasts-2024-2050
View the press release here.




