Perceptions of Team-Based Learning among Periodontic and Endodontic postgraduate residents
Submitted: 7 July 2025
Accepted: 3 November 2025
Published online: 7 April, TAPS 2026, 11(2), 118-126
https://doi.org/10.29060/TAPS.2026-11-2/SC3813
Lean Heong Foo1,3,4, Pei Yuan Chan2,3,4, Jeen Nee Lui2,3,4 & Marianne Meng Ann Ong1,3,4
1Periodontic Unit, 2Endodontic Unit, Department of Restorative Dentistry, National Dental Centre Singapore, Singapore; 3National Dental Research Institute Singapore, National Dental Centre Singapore, Singapore; 4Oral Health Academic Clinical Programme, Duke-NUS Medical School, Singapore
Abstract
Introduction: Team-Based Learning (TBL), grounded in constructivist learning theory, promotes active engagement among learners. This study aimed to explore postgraduate residents’ perceptions and attitudes toward learning about periodontal-endodontic lesions using TBL as an educational method.
Methods: A total of 8 Periodontic residents and 11 Endodontic residents received pre-reading articles related to periodontal-endodontic lesions. On the day of the workshop, they were divided into four mixed-specialty groups. They completed individual and group readiness assurance tests, followed by facilitated discussions on three simulated clinical cases. Feedback was collected through an online anonymous survey that included 32 Team-Based Learning Student Assessment Instrument (TBL-SAI) items, eight on programme content, four on skills contributions, seven on faculty, and four on learning outcomes, all scored on a 5-point Likert scale (1-strongly disagree to 5-strongly agree) and analysed with descriptive and Cronbach’s alpha analysis.
Results: Fifteen of 19 residents attended the workshop. TBL-SAI scores (max 40) reflected strong accountability, with overall mean scores around 29 across both Periodontic and Endodontic residents. Learning preference scores (max 80) averaged approximately 50, and student satisfaction scores (max 40) were similarly positive, averaging just under 30. Programme content, learning outcomes, and faculty performance received high ratings, with mean scores above 4 out of 5. Internal consistency was strong across all subscales (Cronbach’s alpha: 0.69–0.99). Qualitative feedback highlighted the value of clinical case applications in enhancing engagement and understanding.
Conclusion: Residents reported positive perceptions of Team-Based Learning, noting high engagement, accountability, and satisfaction. The findings support its effectiveness as a valuable instructional approach in postgraduate dental education.
Keywords: Dental Education, Endodontics, Periodontics, Residency, Team-Based Learning
I. INTRODUCTION
Team-Based Learning (TBL) is an instructional strategy that promotes active, collaborative learning and encourages students to take responsibility for their education by engaging deeply with content, peers, and instructors. The TBL process includes three core phases: pre-reading, readiness assurance (individual and group), and application. The application phase uses the 4S framework—significant problem, same problem, specific choice, and simultaneous reporting—to drive critical discussion, often resembling a faculty-facilitated debate. TBL has demonstrated positive results in pre-clinical dental education, with improved diagnostic skills and examination scores (Pileggi & O’Neill, 2008). However, most available research focuses on undergraduate learners. There is a lack of data on how TBL impacts dental postgraduate students, who are typically mature, self-directed learners. The aim of this study was to address this gap by exploring residents’ perceptions and attitudes toward learning complex, interdisciplinary topics—specifically periodontal-endodontic lesions—through the Team-Based Learning (TBL) approach, given the diagnostic and treatment challenges these lesions often present in clinical practice.
II. METHODS
A. Study Design and Population
This descriptive study was exempted from formal Centralised Institutional Review Board review by SingHealth Institutional Review Board. The study included all 19 postgraduate residents from the National University of Singapore’s three-year Master of Dental Surgery programme through convenient sampling–11 in Endodontics (four first-year, three second-year, four third-year) and eight in Periodontics (three first-year, three second-year, two third-year), and absentees of the workshop were excluded. No formal sample size calculation was conducted due to the small, fixed cohort size. Despite the small sample size (n=19) limiting generalizability, this pilot study aimed to gain preliminary insights into residents’ perceptions of Team-Based Learning for complex topics like periodontal-endodontic lesions.
B. Team-Based Learning (TBL) Workshop
A 4.5-hour TBL workshop was conducted on 7th December 2022. Two weeks prior, participants received pre-reading materials, including 14 journal articles and a book chapter covering key aspects of periodontal-endodontic lesions, such as diagnosis, radiographic features, and the updated classification system (Herrera et al., 2018).
On the workshop day, participants completed a seven-question Individual Readiness Assurance Test (IRAT) to assess their foundational knowledge in diagnosis, investigation, and management. They were then divided into four teams to complete the same questions as a Team Readiness Assurance Test (TRAT), administered via Google Forms (https://www.google.com/forms/about/) and Fyrebox (www.fyrebox.com) facilitate efficient data collection and real-time feedback during the workshop. This was followed by three clinical case discussions designed using the 4S framework–significant problem, same problem, specific choice, and simultaneous reporting–to apply pre-reading concepts to clinical scenarios.
Verbal consent was obtained, and participants completed an anonymous online survey. Using a 5-point Likert scale (1 = strongly disagree to 5 = strongly agree), they responded to 32 TBL-SAI items (TBL-SAI) (Mennenga, 2012), eight other questions on the course content, four on skills, seven on faculty, and four on learning outcomes. Participants also rated workshop components as ‘Poor’, ‘Fair’, ‘Satisfactory’, ‘Very Good’, or ‘Excellent’, and selected their favourite component. and answered two open-ended questions on the most useful aspects and suggestions for improvement. The TBL-SAI included three subscales: accountability (≥25), learning preference (≥49), and satisfaction (≥28), with a total score >102 indicating positive perception. Permission was obtained to adapt the instrument (Mennenga, 2012), excluding item 31 (“I think Team-Based Learning helped me to improve my grade”) due to the non-graded nature of the workshop. Qualitative data was collected through open-ended questions on valuable workshop moments and suggestions for improvement, and were thematically reviewed to identify common reflections, without formal qualitative analysis. Data was collected anonymously and analysed using descriptive statistics. Cronbach’s alpha assessed the instrument’s reliability.
III. RESULTS
A. Study Population Demographics
Fifteen out of 19 participants attended the workshop, with two absentees from each of the Periodontics and Endodontics residency programmes. The 15 participants were divided into four teams, with balanced representation of year one, two, and three residents in each group. All participants (four males and 11 females, mean age 28.3 ±2.326, range 25-34) responded to the post-workshop survey (100% response rate). The average IRAT score was 67.6±12.6, and the TRAT score was 80.4±6.8 (Appendix 1). All data is deposited at Figshare at
(https://doi.org/10.6084/m9.figshare.28366964).
B. Workshop Ratings
Participants rated the workshop components highly. Pre-reading materials were rated ‘very good’ or ‘excellent’ by 73.3% (11/15), IRAT by 80% (12/15), TRAT by 93.3% (14/15), and clinical case application by 80% (12/15). Most (93.3%) chose the clinical case discussion as their favourite component.
C. TBL-SAI Results
The cohort’s mean TBL-SAI score was 109 ± 0.98, indicating a strong positive perception (Table 1, Appendix 2, Appendix 3 and Appendix 4).
1. Accountability
Periodontic residents scored highest in year 3 (30.5 ± 2.1). Endodontic residents in year 1 (34.0 ± 4.4). Combined cohort mean was 30.1 ± 2.1. Cronbach’s alpha was 0.83 (Periodontics) and 0.75 (Endodontics), indicating good internal consistency. Most residents (86.7%) prepared beforehand and contributed actively.
2. Preference for Lecture or TBL Subscale
Periodontic residents showed consistent preference (mean 50.7 ± 4.1). Endodontic residents varied. Year three scored highest (53.3 ± 6.1). Combined mean: 49.8 ± 13.5. Cronbach’s alpha was 0.69 (Periodontics) and 0.78 (Endodontics). Most (86.7%) reported better understanding and retention through TBL.
3. Student Satisfaction Subscale
Periodontics year three residents had a mean score of 30.0 ± 2.8, resulting in an overall mean of 28.3 ± 1.9, while Endodontics year three scored slightly lower at 29.3 ± 0.0 resulting mean of 29.6 ± 9.5 for the Endodontic residents. The overall cohort mean was 29.1 ± 1.9. Cronbach’s alpha analysis showed 0.69 (Periodontics), 0.68 (Endodontics). Most (86.7%) found the workshop enjoyable and effective; 93.3% preferred learning in teams. Only one participant viewed TBL negatively.
D. Programme Content
Programme content was rated highly for both Periodontic and Endodontic residents (4.3 ± 0.5; 4.6 ± 0.5, total mean 4.6 ± 0.5). Cronbach’s alpha was notably high at 0.94 for Periodontic residents and 0.98 for Endodontic residents, indicating excellent internal consistency. All agreed materials and objectives were appropriate.
E. Programme Learning
Learning subscale scored slightly lower for both groups (Periodontics 3.6 ± 0.8, Endodontics 4.0 ± 1.0, total mean 3.9 ± 0.9), The Cronbach’s alpha values for the programme learning subscale were 0.95 for Periodontic residents and 0.99 for Endodontic residents. Majority of the participants (12/15, 80%) agreed they could apply the knowledge to their work respectively.
F. Faculty
Both Periodontic and Endodontic residents scored highly for the faculty performance (4.5 ± 0.5; 4.4 ± 0.5, total mean 4.4 ± 0.5). Cronbach’s alpha values were 0.98 for Periodontic residents and 0.96 for Endodontic residents, all participants unanimously agreed faculty were engaging and communicated clearly.
G. Qualitative Feedback
Majority (12/15, 80%) of the participants valued clinical cases and group discussion. One participant quoted “enjoyed the interactive sessions”, while another praised the “use of TBL pedagogy for active learning”. One participant said, “Case discussions, hearing from my colleagues as well as supervisors on various treatment options”. Suggestions included more time for discussion and aligning articles discussed with pre-reading.
IV. DISCUSSION
This descriptive study explored postgraduate residents’ perceptions of Team-Based Learning (TBL) in teaching the diagnosis and management of periodontal-endodontic lesions. The positive reception of TBL among residents may be attributed to its focus on clinical relevance, active participation, and peer collaboration.
Both Periodontic and Endodontic residents preferred TBL over traditional lectures (scores>49), consistent with previous studies (Takeuchi et al., 2015). Qualitative feedback emphasized the value of real-life case discussions and interactive sessions, supporting the idea that TBL fosters engagement and critical thinking aligned with adult learning principles. The format encouraged residents to take ownership of their learning while benefiting from team-based decision-making following constructivist learning theory, where exposure to differing viewpoints during discussion facilitates deeper understanding (Hrynchak & Batty, 2012).
Despite overall satisfaction, suggestions for longer discussion time and better alignment of pre-reading with session content indicate a need for improved facilitation and onboarding. Slightly lower preferences among Endodontic residents may reflect differences in prior exposure. High ratings for faculty support and the effectiveness of mixed-level resident teams further highlight the importance of guided facilitation and peer learning. Mixing junior and senior residents within teams promoted mentorship and dynamic learning, reflecting real-world clinical team structures. This structure leverages diverse academic levels to enhance small-group learning outcomes. These findings support TBL as a relevant and effective approach in dental residency education, promoting clinical reasoning, interdisciplinary learning, and professional development.
The 32-item TBL-SAI and 22-item programme surveys may have contributed to survey fatigue and response bias; shortening these in future studies could enhance data quality. Although the study lacked a control group and relied on self-reported data from a small cohort, bias was minimized by assuring participants that responses would not affect exam results. Peer evaluation was excluded due to the single-session format.
|
Items |
Periodontic Residents |
Endodontic Residents |
Whole Cohort |
|
Accountability (Max: 40, mean± s.d.) |
28.3 ± 2.8 |
31.3 ± 3.1 |
30.1 ± 2.1 |
|
Cronbach’s alpha |
0.83 |
0.75 |
0.81 |
|
Preference for Lecture / TBL (Max: 80, mean± s.d.) |
50.7 ± 4.1 |
49.2±6.2 |
49.8 ± 13.5 |
|
Cronbach’s alpha |
0.69 |
0.78 |
0.74 |
|
Student Satisfaction (Max: 40, mean± s.d.) |
28.3 ± 1.9 |
29.3 ± 0.0 |
29.1 ± 1.9 |
|
Cronbach’s alpha |
0.69 |
0.68 |
0.66 |
|
Programme Content (Max: 5, mean± s.d.) |
4.3 ± 0.5 |
4.6 ± 0.5 |
4.6 ± 0.5 |
|
Cronbach’s alpha |
0.94 |
0.98 |
0.96 |
|
Programme Learning (Max: 5, mean± s.d.) |
3.6 ± 0.8 |
4.0 ± 1.0 |
3.9 ± 0.9 |
|
Cronbach’s alpha |
0.95 |
0.99 |
0.98 |
|
Faculty (Max: 5, mean± s.d.) |
4.5 ± 0.5 |
4.4 ± 0.5 |
4.4 ± 0.5 |
|
Cronbach’s alpha |
0.98 |
0.96 |
0.97 |
Table 1. Learners’ feedback and Cronbach’s alpha scores based on Team-Based Learning student assessment instrument, programme content, programme learning and faculty
Future research could incorporate independent faculty follow-up to assess residents’ clinical performance in diagnosing and managing periodontal-endodontic lesions (Kirkpatrick Level 3). Despite its limitations, this study suggested that TBL can be an effective approach for teaching interdisciplinary topics in dentistry. It fostered active engagement, deepened learning, and reinforcing the power of structured peer-supported learning in postgraduate education.
V. CONCLUSION
Residents reported positive perceptions of Team-Based Learning (TBL), with high scores for accountability, engagement, and satisfaction. Consistent quantitative outcomes and corroborating qualitative feedback reinforce its effectiveness. Real-life cases enhanced clinical relevance and critical thinking, while TBL’s collaborative format promoted interdisciplinary learning—ultimately strengthening clinical preparedness and teamwork among dental residents.
Notes on Contributors
Dr Lean Heong Foo is a Consultant Periodontist in Department of Restorative Dentistry, National Dental Centre Singapore. LHF reviewed the literature, contributed to the study conception, data acquisition, data analysis, drafted and critically revised the manuscript.
Dr Pei Yuan Chan is a Senior Consultant Endodontist in Department of Restorative Dentistry, National Dental Centre Singapore and Associate Director, Master of Dental Surgery Endodontic Residency programme. PYC contributed to the study conception, data acquisition, and critically revised the manuscript.
Dr Jeen Nee Lui is a Senior Consultant Endodontist in National Dental Centre Singapore. JNL contributed to the data acquisition and critically revised the manuscript.
Dr Marianne Meng Ann Ong is a Senior Consultant Periodontist in National Dental Centre Singapore Associate Director, Master of Dental Surgery Periodontics Residency programme. MO contributed to the data acquisition and critically revised the manuscript.
All authors gave their final approval and agreed to be accountable for all aspects of the work.
Ethical Approval
This study was exempted from formal Centralised Institutional Board review by SingHealth Institutional Review Board (CIRB Ref: 2024-4153).
Data Availability
Data is deposited at Figshare repository (https://doi.org/10.6084/m9.figshare.28366964).
Acknowledgment
We wish to express our appreciation to the National University of Singapore, Faculty of Dentistry for their support in enabling MDS resident participation in this workshop.
We would also like to thank Ms Geraldine Tan and Ms Liu Yanting from National Dental Centre Singapore, ACP Education, for their help in data preparation and collection.
Funding
There was no funding involved in the preparation of the manuscript.
Declaration of Interest
The authors declare no conflict of interest.
References
Foo, L. H., Chan, P. Y., Lui, J. N., & Ong, M. M. A. (2025). Perceptions of Team-Based Learning among Periodontic and Endodontic postgraduate residents. [Data set]. Figshare. https://doi.org/10.6084/m9.figshare.28182398
Herrera, D., Retamal-Valdes, B., Alonso, B., & Feres, M. (2018). Acute periodontal lesions (periodontal abscesses and necrotizing periodontal diseases) and endo-periodontal lesions. Journal of Clinical Periodontology, 89 Suppl 1, S85-S102. https://doi.org/10.1002/JPER.16-0642
Hrynchak, P., & Batty, H. (2012). The educational theory basis of Team-Based Learning. Medical Teacher, 34(10), 796-801. https://doi.org/10.3109/0142159X.2012.687120
Mennenga, H. A. (2012). Development and psychometric testing of the Team-Based Learning student assessment instrument. Nurse Educator, 37(4), 168-172. https://doi.org/10.1097/NNE.0b013e31825a87cc
Pileggi, R., & O’Neill, P. N. (2008). Team-Based Learning using an audience response system: An innovative method of teaching diagnosis to undergraduate dental students. Journal of Dental Education, 72(10), 1182-1188. https://www.ncbi.nlm.nih.gov/pubmed/18923099
Takeuchi, H., Omoto, K., Okura, K., Tajima, T., Suzuki, Y., Hosoki, M., Koori, M., Shigemoto, S., Ueda, M., Nishigawa, K., Rodis, O. M., & Matsuka, Y. (2015). Effects of Team-Based Learning on fixed prosthodontic education in a Japanese School of Dentistry. Journal of Dental Education, 79(4), 417-423. https://www.ncbi.nlm.nih.gov/pubmed/25838013
*Foo Lean Heong
National Dental Centre Singapore,
5, Second Hospital Avenue,
Singapore 168938
Email: foo.lean.heong@singhealth.com.sg
Submitted: 6 March 2025
Accepted: 27 August 2025
Published online: 7 April, TAPS 2026, 11(2), 114-117
https://doi.org/10.29060/TAPS.2026-11-2/SC3684
Kye Mon Min Swe1,2, Amit Bhardwaj3 & Hnin Pwint Phyu4
1Faculty of Medical Sciences, Newcastle University, United Kingdom; 2Newcastle University Medicine Malaysia (NUMed), Malaysia; 3Sengkang General Hospital, Singapore; 4M Kandiah Faculty of Medicine and Health Science, University Abdul Rahman, Malaysia
Abstract
Introduction: Student motivation in teaching-learning is pivotal in promoting overall well-being, enhancing performance, and nurturing skilled professionals. Knowledge about student motivation allows educators to broaden their understanding, and this study investigates the levels of student motivation at different phases of their medical education.
Methods: A quantitative study explored medical students’ academic motivation using the validated Academic Motivation Scale AMS-C 28, with a rating on a 7-point Likert Scale. IBM-SPSS was used to analyse the data.
Results: A total of 105 students participated in the study. The results indicated that students exhibited higher levels of intrinsic motivation compared to extrinsic motivation. The mean score for intrinsic motivation (M=5.13, SD=0.91) surpassed that of extrinsic motivation (M=4.63, SD=1.00). Regarding the association between academic year and student motivation, second-year and fourth-year medical students exhibited the highest intrinsic motivation (M=5.36, SD=0.8) and (M=5.36, SD=0.68), respectively, and second-year medical students showed the highest extrinsic motivation (M=4.87, SD=0.96) compared to other academic years, but this difference was statistically not significant.
Conclusion: The findings exhibited higher levels of intrinsic motivation, indicating active involvement in learning activities and deriving satisfaction from the course. The MBBS students in the second year displayed more intrinsic motivation, influenced by the challenging nature of successfully completing the first year, which is historically associated with a high failure rate.
Keywords: Motivation, Medical Student, Academic Motivation Scale
I. INTRODUCTION
Student motivation is a critical component of the educational process, significantly influencing academic achievement, retention, and overall student well-being (Ryan & Deci, 2000). Particularly in demanding fields, such as medical education, the quality of motivation can vary substantially among students due to various internal and external factors. Medical education poses unique challenges, necessitating effective strategies to sustain students’ motivation through the rigors of their training.
Prior research highlights the distinction between intrinsic and extrinsic motivation and their different impacts on academic performance. Intrinsic motivation refers to engaging in a task for its inherent satisfaction, while extrinsic motivation involves external rewards or pressures (Ryan & Deci, 2000). Studies have shown that stronger intrinsic motivation is associated with greater persistence, improved learning outcomes, and higher satisfaction (Schunk et al., 2014).
In medical education, motivation can profoundly influence students’ engagement with their coursework and clinical practices. For instance, intrinsic factors such as a passion for medicine and a desire to help others can actively drive students to seek knowledge (Ryan & Deci, 2000). Conversely, extrinsic factors, such as grades and external validation, can enhance motivation to a certain extent but may lead to burnout or disengagement if overemphasised.
A crucial aspect of the student experience in medical education is the transition through various academic years. Each stage presents unique challenges affecting motivation. Understanding these stages and their impact on student motivation is vital for fostering an enriching educational environment (Nadel & Rosenberg, 2020). Exploring the academic motivations of medical students is essential for informing educators and administrators about the various factors affecting student engagement and success. Understanding these motivations can help target interventions for students struggling or disinterested in their studies.
This study aims to explore the levels of student motivation throughout different phases of medical education, utilising a quantitative framework that assesses both intrinsic and extrinsic motivations. By understanding how motivation fluctuates with educational years, educators and administrators can better tailor student interventions and support systems.
II. METHODS
A descriptive quantitative research design was employed to measure academic motivation among medical students. Participants were recruited through classroom announcements, and voluntary consent was obtained.
A. Instrument
The Academic Motivation Scale (AMS-C 28) was used to measure students’ academic motivation levels. The AMS scale (Vallerand et al., 1992) contains 28 items, three domains, further subdivided into seven subscales:
1) Intrinsic motivation:
- Intrinsic motivation—to know
- Intrinsic motivation—toward accomplishment
- Intrinsic motivation—to experience stimulation
2) Extrinsic motivation:
- Extrinsic motivation—Identified
- Extrinsic motivation—Introjected
- Extrinsic motivation—external regulation
3) Amotivation:
Each item was rated on a 7-point Likert scale ranging from 1 (not at all true) to 7 (very true).
The AMS has demonstrated robust internal consistency (Cronbach’s alpha = .81). This scale provides valuable insights into students’ motivations in various educational contexts.
Data were analysed using IBM-SPSS version 25. Descriptive statistics (means and standard deviations) were calculated for each subscale. ANOVA tests were employed to compare intrinsic and extrinsic motivation levels across different academic years. A significance level of p<0.05 was considered statistically significant.
III. RESULTS
A total of 105 MBBS students from years 1 to 5 participated in the study, with a response rate of 47.5%. The majority were aged between 21-25 years, and female participants constituted a significant portion (n=74), (70.5%).
A. Academic Motivation
The data demonstrated that students had higher internal than external motivation, with the “intrinsic motivation to know” achieving the highest mean score (M = 5.58, SD = 1.01). The aggregate score for intrinsic motivation (M = 5.13, SD = 0.91) was significantly higher than the external motivation score (M = 4.36, SD = 1.10). Moreover, the average score for amotivation was (M = 2.5, SD = 1.14). The statement “Because I think that medical education will help me better prepare for the career I have chosen” received the highest mean score (M = 6.07, SD = 0.953).
B. Comparisons of the Academic Motivation Scale Among Different Academic Years
Regarding the association between academic year and student motivation, Analysis of variance (ANOVA) revealed significant differences in amotivation levels across academic years (F = 4.688, p = .002). Post-hoc Tukey HSD tests identified significant differences between MBBS Year 3 and Year 4 (mean difference = 1.54583, p = .003), and between MBBS Year 4 and Year 5 (mean difference = -1.25417, p = .005). MBBS Year 4 students exhibited the lowest amotivation (M = 1.60), while Year 3 students demonstrated the highest (M = 3.15).
Regarding intrinsic motivation, MBBS Year 2 students (M = 5.36, SD = 0.8) and MBBS Year 4 students (M = 5.36, SD = 0.68) displayed the highest levels, whereas MBBS Year 3 students showed the lowest (M = 4.75, SD = 1.28). However, no statistically significant differences in intrinsic motivation were observed across academic years (F = 2.312, p = .063).
For extrinsic motivation, MBBS Year 2 students demonstrated the highest levels (M = 4.87, SD = 0.96), while MBBS Year 4 students exhibited the lowest (M = 4.1333). Nevertheless, no statistically significant differences in extrinsic motivation were found across academic years (F = 2.295, p = .064).
These findings suggest that motivation, particularly amotivation, can fluctuate significantly as students progress through their medical education. While intrinsic and extrinsic motivation levels varied across years, these differences did not reach statistical significance.
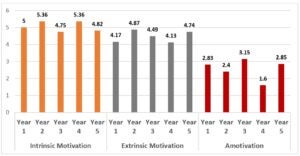
Figure 1. The relation between the academic year and subscales of AMS
IV. DISCUSSION
The findings of this study align with previous research, highlighting the importance of intrinsic motivation as a driver of academic success (Ryan & Deci, 2000). The higher intrinsic motivation among second-year medical students may be attributed to their positive experiences after successfully completing a challenging first year, and the same for the fourth-year medical students who had successfully completed a challenging clinical year 3. This transitional phase often acts as a motivational catalyst, increasing engagement and satisfaction in their studies (Nadel & Rosenberg, 2020).
Conversely, the lower motivation levels observed among third-year students may suggest a possible decline in intrinsic motivation due to the increasing pressures and clinical responsibilities accompanying their first year in clinical training at the hospital setting and clinical campus. This transitional period is often marked by numerous challenges, including stress from clinical evaluations and the need for adaptive learning strategies (Schunk et al., 2014). The study by Lyndon et al. (2023) found that academic motivation indeed fluctuates across different academic years, and several factors contribute to these changes. Changes in the curriculum structure from classroom-based learning to more clinical experiences can affect motivation levels, with some students finding clinical work more engaging and others struggling to adapt. The study emphasises the importance of understanding these fluctuations in academic motivation to develop targeted interventions and support systems for medical students.
A. Limitations
This study has a moderate response rate (47.5%), which may introduce response bias and potentially limit generalisability. The single institution may not represent diverse educational settings or geographical locations. The cross-sectional design prevents the examination of longitudinal changes in student motivation, and potential gender imbalances in the sample could limit generalisability across genders.
B. Implications
This study highlights the importance of medical educators recognising fluctuations in motivation across academic years. Medical schools should implement regular assessments of student motivation and well-being and develop targeted interventions to sustain students’ enthusiasm and engagement. For instance, mentorship programmes, peer support groups, and structured feedback sessions can provide tailored support to help students maintain their motivation throughout their academic journey.
These initiatives can help foster an environment conducive to maintaining high motivation levels.
C. Recommendations
Future research should aim to explore the qualitative aspects of motivation, diving deeper into individual experiences and the psychological factors influencing students’ intrinsic and extrinsic motivation. Additionally, comparing motivation levels with academic performance can provide useful insight into how motivation affects learning outcomes.
A more rigorous randomised approach with a larger sample size is advisable for future research endeavours. Additionally, exploring qualitative approaches to student-faculty interaction, student engagement, and student performance should be included in the investigation.
V. CONCLUSION
In conclusion, this preliminary study reveals that medical students display higher intrinsic than extrinsic motivation, particularly in their second year. Recognising these trends is essential for developing effective educational interventions to support student success throughout their medical education journey. Cultivating an environment that promotes and sustains motivation may lead to better academic performance and enhanced well-being among medical students.
Notes on Contributors
Dr Kye MMS is the corresponding author for this paper. She designed the study, analysed the data, and prepared the manuscript, working with the co-author.
Dr. Amit B. and Dr. Hnin PP contributed substantially to the design, editing, and preparation of the final manuscript.
Ethical Approval
The research study was approved by the Universiti Tunku Abdul Rahman Scientific and Ethical Review Committee on 4 November 2022 (Approval number: U/SERC/228/2022).
Data Availability
The data that support the findings of the study are openly available at https://doi.org/10.6084/m9.figshare.28544321.
Acknowledgment
We would like to acknowledge Newcastle University Medicine Malaysia for the support, and we also would like to acknowledge the students for their voluntary participation in this study.
Funding
There was no funding for this research study.
Declaration of Interest
The authors declare no conflicts of interest, including financial, consultant, institutional, or other relationships.
References
Nadel, B., & Rosenberg, A. (2020). The role of motivation in medical education. Medical Education Journal, 54(9), 883-890. https://doi.org/10.1111/medu.14205
Lyndon, M. P., Henning, M. A., Alyami, H., Krishna, S., Yu, T. C., & Hill, A. G. (2023). Changes in motivation and burnout in medical students over time: A longitudinal study. BMC Medical Education, 23(1), 1-9. https://doi.org/10.1186/s12909-023-04127-1
Ryan, R. M., & Deci, E. L. (2000). Self-determination theory and the facilitation of intrinsic motivation, social development, and well-being. American Psychologist, 55(1), 68-78. https://doi.org/10.1037/0003-066X.55.1.68
Schunk, D. H., Pintrich, P. R., & Meece, J. L. (2014). Motivation in education: Theory, research, and applications (4th ed.). Pearson. https://api.pageplace.de/preview/DT0400.9781292055251_A24621767/preview-9781292055251_A24621767.pdf
Vallerand, R. J., Pelletier, L. G., & Blais, M. R. (1992). The academic motivation scale: A measure of intrinsic, extrinsic, and amotivation in education. Educational and Psychological Measurement, 52(1), 1003-1017. https://doi.org/10.1177/0013164492052004014
*Dr Kye Mon Min Swe
Faculty of Medical Sciences, Newcastle University,
Newcastle upon Tyne, NE1 7RU, United Kingdom;
Newcastle University Medicine Malaysia (NUMed),
1, Jalan Sarjana 1, Kota Ilmu, Educity@Iskandar,
79200 Iskandar Puteri, Johor, Malaysia
601115133799
Email: kye-mon.min-swe@newcastle.edu.my
Submitted: 31 January 2025
Accepted: 16 June 2025
Published online: 6 January, TAPS 2026, 11(1), 74-78
https://doi.org/10.29060/TAPS.2026-11-1/SC3658
Astrid Pratidina Susilo1, Ervin Dyah Ayu Masita Dewi1, Satrio Utomo2 & Jasmine Aulia Sabrina2
1Department of Medical Education and Bioethics, Faculty of Medicine, Universitas Surabaya, Indonesia; 2Bachelor Program of Medical Education, Faculty of Medicine, Universitas Surabaya, Indonesia
Abstract
Introduction: Limited resources have caused many challenges in health care. Health workers faced dilemmas that potentially cause burnout. Medical students must be strengthened with resilience when facing dilemmas. This study aimed to investigate Indonesian students’ strategies for strengthening resilience after participating in a bioethics workshop based on reflective and collaborative principles.
Methods: A bioethics workshop based on reflective and collaborative principles without didactic elements was conducted with 30 medical students. We collected quantitative data from the Adapted Version of the Adult Personal Resilience Questionnaire and qualitative data from the students’ reflections on strategies to strengthen resilience. Descriptive statistics and thematic analysis were used to analyse the quantitative and qualitative data, respectively.
Results: Thirty students participated in the study. The total score of the resilience questionnaire was 4.28 (SD 0.39), indicating that the students perceived themselves as having a moderate-to-high level of resilience for all items. The following four themes from the qualitative analysis were identified: faith, adaptation, self-management, and relationships.
Conclusion: Indonesian students’ strategies for strengthening resilience are related to faith, adaptation, self-management, and relationships. Although without a didactic approach, the reflective and collaborative learning in this workshop can raise medical students’ awareness of strategies for building resilience and provided an opportunity for students to reflect on their resilience level.
Keywords: Resilience, Reflective Learning, Collaborative Learning, Self-Management, Relationships, Faith, Mixed-Method Approach
I. INTRODUCTION
During the corona virus disease 2019 (COVID-19) pandemic, many healthcare professionals worldwide experienced burnout for several reasons, such as a high workload, fear of getting infected, and passing on the infection to family members. They also faced ethical dilemmas, were compelled to make challenging decisions about which patients to focus on during resource scarcity, and experienced hopelessness about not being able to help all the patients. They had to “play God without God’s power,” determine who could be admitted for care, and who had to be left behind. Previous studies have shown that the situation was overwhelming, and healthcare professionals were unprepared to face it (Ningrum & Missel, 2023).
Beyond the COVID-19 pandemic, healthcare resource scarcity is a reality that healthcare professionals frequently encounter. Therefore, it is essential to prepare future healthcare professionals to be able to decide on resource allocation during resource scarcity and build their resilience to face unpredictable situations (Dewi et al., 2023). Resilience refers to one’s ability to “spring back into shape,” that is, recover quickly from challenges by using a positive coping mechanism. Resilience is multidimensional and can be learned. Nurturing resilience is more than a mere one-point process. It is a longitudinal process that requires practice and perseverance (Calo et al., 2024).
Most resilience education includes didactic content that introduces theories and strategies related to resilience, such as mindfulness or meditation practices (Calo et al., 2024).As students naturally have coping mechanisms and can learn from each other, we developed a workshop to raise awareness of resilience based on reflective (Calo et al., 2024) and collaborative learning principles (Yang, 2023). We asked the students to complete a questionnaire to reflect on their resilience levels and subsequently engage in discussions with peers. To investigate whether this educational approach can raise students’ awareness of resilience, we explored the students’ key takeaways from this workshop using the following research question: what are the students’ strategies to strengthen resilience after attending a workshop based on reflective and collaborative principles?
II. METHODS
This study was conducted in a private medical school in East Java, Indonesia. We developed a one-day bioethics workshop tailored to address the gaps highlighted by previous study (Dewi et al., 2023) with three objectives. First, we aimed to improve students’ decision-making skills in ethical decisions. Second, we introduced the communication skills necessary to discuss with patients and their families. Third, we attempted to raise students’ awareness of developing resilience. This study focuses on the third objective. The participants were third- and fourth-year pre-clinical phase medical students who were selected using a random sampling approach. Although they have not yet experienced significant real-patient encounters, they had a basic understanding of bioethics and doctor-patient communication skills, while modules on resilience were not yet included in the curriculum. All participants were informed about the study goals and procedures and signed written consent forms.
During the session on resilience, which lasted one hour, the students engaged in several activities. They reflected on their resilience levels by completing a questionnaire. This activity was based on the principle of reflective learning. Subsequently, considering the ethical dilemma of resource scarcity, the students discussed in pairs how to mitigate burnout due to such a dilemmatic situation and how to strengthen their resilience. The method was based on the collaborative learning principle. Finally, the students shared their strategies to strengthen their resilience as medical students.
We collected the quantitative and qualitative data from the questionnaire and students’ reflections, respectively. This study used the Adapted Version of Adult Personal Resilience Questionnaire, translated to Indonesian, and used in a study to explore physicians’ resilience in remote areas (Handoyo et al., 2021). The questionnaire had a 5-point Likert scale (1=strongly disagree, 2=disagree, 3=neutral, 4=agree, 5=strongly agree). We modified the Indonesian version and validated the content with three experts (two medical educationalists and one psychiatrist). The experts scored the relevance of each item to measure resilience (1=highly irrelevant, 2=irrelevant, 3=relevant, and 4=highly relevant). Only those items for which all experts scored 4 were included. The final questionnaire consisted of 19 items, with a Cronbach’s alpha of 0.848. Data from the questionnaire were descriptively analysed using SPSS 26 while the qualitative data were analysed using a thematic analysis approach. Two researchers independently coded and developed themes and discussed them until a consensus was achieved.
III. RESULTS
Thirty students (11 male and 19 female) participated in the study. The total score of the resilience questionnaire was 4.28 (SD 0.39), indicating that the students perceived themselves as having a moderate-to-high level of resilience for all items.
|
No. |
Item |
Mean |
Standard Deviation (SD) |
|
Determination |
|||
|
1 |
Once I set a goal, I am determined to achieve it. |
4.10 |
0.89 |
|
2 |
I persevere at the things I decide, despite difficulties. |
4.27 |
0.69 |
|
3 |
Being determined is an important part of my character. |
4.23 |
0.86 |
|
4 |
I keep trying for the things I want until I reach them. |
4.37 |
0.62 |
|
|
Subtotal |
4.24 |
0.54 |
|
Endurance |
|||
|
5 |
I am able to live through difficult times |
4.23 |
0.77 |
|
6 |
I can withstand difficult situations. |
4.30 |
0.84 |
|
7 |
I can endure the problems that life brings. |
4.23 |
0.86 |
|
8 |
I can endure even when I am attacked |
4.00 |
0.87 |
|
|
Subtotal |
4.19 |
0.69 |
|
Adaptability |
|||
|
9 |
I have the ability to adapt to difficult situations. |
3.73 |
1.02 |
|
10 |
I can change to fit into many kinds of circumstances |
3.90 |
0.80 |
|
11 |
I can find ways to adapt to unexpected conditions. |
3.97 |
0.62 |
|
|
Subtotal |
3.87 |
0.67 |
|
Recuperability |
|||
|
12 |
I recover from any misfortune that happens to me. |
3.93 |
0.74 |
|
13 |
I am able to bounce back from any kind of adversity. |
3.93 |
0.74 |
|
14 |
I can recover from any type of problem. |
3.97 |
1.00 |
|
|
Subtotal |
3.94 |
0.66 |
|
Life Calling |
|||
|
15 |
I believe that God has a purpose in placing me here. |
4.80 |
0.48 |
|
16 |
God has always guided me through my life. |
4.73 |
0.58 |
|
17 |
God would never allow me to walk through life alone. |
4.77 |
0.68 |
|
18 |
Even in difficult situations, God has been there to guide me. |
4.83 |
0.46 |
|
19 |
I believe that God is ever-present, in everything I do |
4.93 |
0.25 |
|
|
Subtotal |
4.81 |
0.36 |
|
Total |
4.28 |
0.39 |
Table 1. Participants’ Resilience as Measured in the Adapted Version of the Adult Personal Resilience Questionnaire
Four themes emerged from the qualitative analysis: faith, adaptation, self-management, and relationships. Each theme was described and relevant examples of quotes to illustrate them are provided below.
A. Faith
The participants implied that resilience was related to their faith in God. They believed that God would not give them a “test” that was more difficult than their ability to handle it. The importance of believing that God will give the strength to deal with every problem was strongly emphasised. Additionally, the participants mentioned striving to be “Ikhlas” (sincere) and repeatedly accepting their reality as strategies to improve resilience. For example, Student 3 wrote, “I will accept the reality and handle every situation with sincerity.”
B. Adaptation
Participants believed that they could increase their resilience through ongoing practice. Thus, self-motivation and self-confidence were essential factors. They mentioned strategies, such as stepping out of their comfort zones, trying new things, and improving their perseverance and recoverability. For instance, Student 25 mentioned “Practice to challenge oneself toward change” as a strategy for resilience.
C. Self-Management
Participants reported that self-management is important in achieving resilience. They need to understand their limits as well as learn how to manage stress, emotions, and time. Students also mentioned meditation, journal writing, and rest as self-management strategies that improved resilience. They argued that a balance between logic and feelings increases one’s resilience.
D. Relationship
Students were aware of the fact that they need friends and colleagues to share, collaborate with, and make decisions. They need to have friends with a positive attitude, surround themselves with individuals with a positive outlook, and participate in volunteering activities. Student 8 shared, “Do not push yourself; try to share your problems with your friends.”
IV. DISCUSSION
The study findings revealed that the workshop based on reflective and collaborative learning principles can raise students’ awareness of effective strategies to strengthen their resilience. Two themes were in line with the constructs in the questionnaire: “faith” and “adaptation”. “Faith” is a fairly similar concept to “life calling” while “adaption” reflected other subscales in the questionnaire, such as “determination” and “recuperability” (Handoyo et al., 2021). This resemblance suggested that students were inspired when they reflected on the questionnaire in which they scored themselves on a relatively high scale of 3 or above for all items. The reflection process exposed them to the concept of resilience.
However, “self-management” and “relationships” were not reflected in the questionnaire responses, but found in pair discussions and personal reflections. Beyond what they learned while completing the questionnaire, the students gained new ideas through discussions with their peers. Collaborative learning raised the students’ awareness, as they learned from each other’s perspectives during the discussion (Yang, 2023).
Overall, the students’ ideas were in line with the findings of previous research on strengthening resilience (Calo et al., 2024) and covered diverse aspects. In their writing, they could indicate the dynamics of the strengthening resilience through internal adaptation, relationships with others, and views from a faith perspective. “Adaptation” and “self-management” reflected the strategies for improving resilience which comes from within. The “relationship” aspect suggested the students’ need for other people in their lives as a critical support system in strengthening resilience. Finally, “faith” showed that the students viewed God’s influence as essential for nurturing resilience.
This study has certain limitations. First, the workshop focusing on resilience was short (only one hour) as it was embedded in a larger workshop aimed at enhancing the students’ decision-making skills in ethical dilemmas. A longitudinal workshop may yield different results. Second, the qualitative data were based on the students’ writing, which was influenced by their ability to express themselves. Interviews may have yielded different results.
Despite this constraint, the findings showed that a workshop based on reflective and collaborative learning, without a didactic approach, could raise medical students’ awareness of strategies to build resilience. This finding is important in providing alternative strategies to strengthen resilience in medical education, particularly when time is constrained. Future studies need to explore the transfer of learning, that is, to what extent students apply what they are aware of in actual practice and how it can improve their resilience levels. Additionally, it is essential to examine whether improved awareness of resilience will enhance medical students’ abilities to face ethical dilemmas in future clinical practice.
V. CONCLUSION
Although without a lecture, a workshop based on reflective and collaborative learning could raise medical students’ awareness of strategies to build resilience. Students’ have ideas of strategies which fall into four categories: faith, adaptation, self-management, and relationship.
Notes on Contributors
Astrid Pratidina Susilo conceptualised the study, organised the workshop, collected and analysed the data, and drafted the manuscript.
Ervin Dyah Ayu Masita Dewi conceptualised the study, organised the workshop, analysed the data, and drafted the manuscript.
Satrio Utomo organised the workshop, collected the data, and reviewed the manuscript.
Jasmine Aulia Sabrina organised the workshop, collected the data, and reviewed the manuscript.
Ethical Approval
Ethical approval was obtained from the University Surabaya Ethical Committee (approval no.297/KE/I/2024).
Data Availability
Data were in Indonesian and can be made available upon personal request.
Acknowledgement
We would to thank all the students who participated in the workshops and the experts who validated the questionnaire. We would like to thank Editage (www.editage.com) for English language editing.
Funding
This study was supported by a research grant from the Universitas Surabaya (N0.165/SP-Lit/LPPM-01/Int/FK/XI/2023).
Declaration of Interest
The authors declare no conflicts of interest.
References
Calo, M., Judd, B., & Peiris, C. (2024). Grit, resilience and growth-mindset interventions in health professional students: A systematic review and meta-analysis. Medical Education, 58(8), 902–919. https://doi.org/10.1111/medu.15391
Dewi, E. D. A. M., Matter, L., Susilo, A. P., & Krumeich, A. (2023). A qualitative study on patients’ selection in the scarcity of resources in the COVID-19 pandemic in a communal culture. Developing World Bioethics, 10, 84–92. https://doi.org/10.1111/dewb.12438
Handoyo, N. E., Rahayu, G. R., Claramita, M., Keraf, M. K. P. A., Octrisdey, K., Yuniarti, K. W., Ash, J., & Schuwirth, L. (2021). Developing personal resilience questionnaire for rural doctors: An indigenous approach study in Indonesia. BMC Psychology, 9(158). https://doi.org/10.1186/s40359-021-00666-8
Ningrum, A. P., & Missel, M. (2023). Urip iku urup (life is lit) by service to others: A qualitative study of frontline healthcare workers’ lived experiences providing patient care in Indonesia’s COVID-19-designated hospital. BMC Health Services Research, 23(262). https://doi.org/10.1186/s12913-023-09257-2
Yang, X. (2023). A historical review of collaborative learning and cooperative learning. TechTrends, 67(4), 718–728. https://doi.org/10.1007/s11528-022-00823-9
*Ervin Dyah Ayu Masita Dewi
Faculty of Medicine, Universitas Surabaya
Jalan Raya Kalirungkut, Surabaya,
60293, Indonesia
+62-85865256147
Email: ervin_dyah@staff.ubaya.ac.id
Submitted: 19 September 2024
Accepted: 16 April 2025
Published online: 6 January, TAPS 2026, 11(1), 69-73
https://doi.org/10.29060/TAPS.2026-11-1/SC3524
Eng-Koon Ong1-4,7, April Thant Aung3,8, Min Chiam3, Lalit Kumar Radha Krishna1,3,4, Yingxuan Chen10, Filomar Cortezano Tariao9, Faith Ng11, Jamie Zhou1,4 & Wen-Shan Sim4-6
1Division of Supportive and Palliative Care, National Cancer Centre Singapore, Singapore; 2Office of Medical Humanities, SingHealth Medicine Academic Clinical Programme, Singapore; 3Division of Cancer Education, National Cancer Centre Singapore, Singapore; 4Duke-NUS Graduate Medical School, Singapore; 5Maternal Fetal Medicine, KK Women’s and Children’s Hospital, Singapore; 6PGY1 Programme, SingHealth, Singapore; 7Assisi Hospice, Singapore; 8School of Humanities, Nanyang Technological University, Singapore; 9School of Dance, Nanyang Academy of Fine Arts, Singapore; 10Shaw Heritage Arts and Wellbeing Studios, Singapore; 11Checkpoint Theatre, Singapore
Abstract
Introduction: Through collaborative pedagogical initiatives, the medical humanities (MH) have the potential to support healthcare professionals in developing various competencies in medical education (ME). However, there is a lack of data on faculty development programmes specific to this field.
Methods: Based on our experience in designing a medical humanities workshop for medical students, we conducted two faculty development (FD) workshops that adopted an interdisciplinary approach towards faculty training. These FD workshops served to train fellow clinician educators in the integration of the MH in ME.
Results: A total of 17 participants completed two workshops over two years, with seven participants in 2023 and 6 in 2024 completing pre- and post-workshop surveys that evaluated their experience, knowledge and skills. The survey consisted of six self-rated questions based on a 5-point Likert scale from 1 (strongly disagree) to 5 (strongly agree) with an open-ended question embedded in the post-workshop survey. A paired t-test evaluation of the results suggests that there was an increase in awareness, knowledge, and confidence.
Conclusion: Our MH-based FD programme is limited by the lack of qualitative data and further studies are needed. Similar programmes should include an introduction to the medical humanities and its methodologies so that a train-the-trainers approach is adopted. Programmes should also look beyond teaching effectiveness to include developing systemic awareness and support, assess outcomes such as professional identity formation, and build communities of practice for faculty members.
Keywords: Faculty Development, Medical Humanities, Medical Education, Health Professions Education
I. INTRODUCTION
The role of the medical humanities (MH) in healthcare is multifaceted, supported by its methodologies from the arts and humanities in promoting perspective-taking, reflective practice, and professional identity formation. Specifically, its relevance in aspects of medical education (ME) such as professionalism, communications, and humanistic care has rallied healthcare educators exploring the field to achieve educational goals in developing empathy, improving patient experience, and preventing burnout (Ong et al. 2024).
A vision to integrate MH within ME has gained prominence over the past decade, with articles describing its epistemological functions, guidelines on programme development, and emerging evidence of acceptability and effectiveness of pilot programmes. Despite this, there is a disproportionate lack of data on faculty development (FD) to support this vision. A white paper by Howley et al. (2020) advocates for interdisciplinary collaboration between clinician educators, humanities scholars and creative arts practitioners. However, little guidance was provided on the type of effort, support, and considerations needed to nurture an interdisciplinary team of faculty members to design, implement, and sustain MH programmes.
II. CONTEXT AND PROGRAMME
Since 2022, a one-day theatre-based MH workshop has been conducted for all medical students from Duke-NUS Graduate Medical School (Singapore) rotating through the Division of Supportive and Palliative Care at the National Cancer Centre Singapore. During the workshop held on the final day of their one-week clinical rotation, students watch a full recording of a local theatre play, A Good Death by the playwright Faith Ng, and participate in small group discussions on scenarios that depict pain crises experienced by oncology and hospice patients, difficult conversations about end-of-life care, and moral distress faced by palliative care practitioners and its impact on their mental wellbeing. Students also participate in a “hot-seating” activity where they embody the different characters of the play, and respond to questions from the class while in character. Prior to this core clinical rotation, most students had little prior exposure to end-of-life care and the activities were intended to promote perspective-taking, self-awareness, and professional identity formation through the use of theatre. The workshop is co-facilitated by a specialist palliative care physician with a master’s degree in medical education, a medical humanities doctorate fellow, a medical social worker trained in counselling and narrative therapy, and the director of the play. This interdisciplinary faculty team facilitated dynamic discussions and generated new insights for the students.
Based on our positive experience in developing this programme, we decided to conduct a yearly faculty development (FD) workshop for other educators who were keen on designing arts and humanities programmes within their specialities and settings. The workshop consisted of three segments. Firstly, an introduction to conceptual frameworks and principles within both MH and ME was presented by EKO and YC, listing frameworks such as adult learning, community of practice, and reflective practice. Principles such as the need to create a sense of agency, establish common goals, validate values of faculty members, and promote reflective processes were also identified. Secondly, YC described and explained theatre-based facilitation methods such as improvisation and applied theatre techniques. This provided refreshing insight on how MH programmes could be designed and conducted by arts practitioners like herself. The choice of teaching materials that considered learners’ receptivity, appropriateness to achieve learning objectives, and ease of access were also explored. Lastly, the team demonstrated how learning objectives and lesson plans could be written based on Bloom’s taxonomy and Gagne’s model of instruction respectively. The educators were then asked to practice doing the same in groups of three for an existing or potential MH-based ME programme.
We applied the conceptual framework of adult learning in the design of the FD workshop and the relevance of medical humanities in medical education was regularly alluded to in all three segments. This promoted a sense of agency towards self-directed learning. All staff from the SingHealth Academic Medicine Centre, the largest healthcare cluster in Singapore, were invited to participate in the FD workshops in 2023 and 2024. The same team of faculty members from the original medical students’ workshops conducted the FD workshops.
III. METHODS / RESULTS
A total of 17 participants completed the FD workshops over two years. We found a lack of validated evaluation methods for MH-based ME programmes and thus designed a questionnaire guided by Bloom’s taxonomy for our programme. This was similarly done by Kumagai et al. (2007) who investigated the effects of a forum theatre-based workshop for 29 medical school faculty members that facilitated discussions on race and gender through a self-designed survey pre- and post-workshop that assessed self-awareness and “critical consciousness”.
All 17 participants were invited to complete an online survey within one week before and after the FD workshops. The survey consisted of six self-rated questions based on a 5-point Likert scale from 1 (strongly disagree) to 5 (strongly agree) that alluded to the participants’ experience, knowledge, and skills gained from the workshop.
In total, 7 participants in 2023 and 6 in 2024 consented to and completed the surveys (Ong et al., 2024). The group consisted of seven doctors, a clinical psychologist, a clinical pastoral counsellor, a healthcare education executive, two pharmacists, and an assistant director of community outreach and philanthropy. Table 1 lists the questions and the outcomes of the survey. A paired t-test evaluation of the results suggests that there was an increase in awareness, knowledge, and confidence.
|
|
Questions |
Mean score (n=13) |
t-score difference |
p-value |
|
|
Pre-workshop |
Post-workshop |
||||
|
1. |
I would recommend this workshop to my fellow colleagues. |
3.62 |
4.23 |
2.309 |
0.04 |
|
2. |
I am keen to attend similar workshops again in the future. |
3.85 |
4.62 |
2.993 |
0.011 |
|
3. |
I agree that the arts and humanities have valuable knowledge to offer to medical education. |
4.38 |
4.62 |
0.478 |
0.641 |
|
4. |
I can identify potential content, materials and facilitation needed for medical education programs involving the arts and humanities. |
2.54 |
3.92 |
4.454 |
<0.001 |
|
5. |
I am able to pursue the design and implementation of a medical education program involving the arts and humanities confidently as part of a team. |
2.46 |
3.69 |
6.121 |
<0.001 |
|
6. |
I am able to pursue the design and implementation of a medical education program involving the arts and humanities confidently as an education lead, alongside arts practitioners. |
1.92 |
2.77 |
4.430 |
<0.001 |
Table 1. Survey questions and results
IV. LIMITATIONS
Programme evaluation is limited by the small number of participants and lack of a validated measure. While there may be apparent statistical significance to the improvement of the scores collected, a solely quantitative outcome measure may not be adequate to provide insight on the success of the programme. Future programme evaluations with bigger cohorts coupled with qualitative data are needed.
V. DISCUSSION
Existing publications in FD focus on broader teaching competencies such as facilitation and communication skills, curriculum development, education leadership, and scholarship (Steinert et al. 2016), suggesting that faculty members could translate what they have learnt into individual fields of interest. Based on our experience, we posit that further considerations are needed for FD programmes in the field of the medical humanities.
Firstly, a low awareness of the relevance of the MH in ME (Ong, 2021), the need for faculty members to achieve basic understanding of content from diverse theoretical and practical frameworks from both fields, distinct but complementary roles of co-faculty members from medicine and the arts and humanities (Ong et al. 2024), and a lack of agreement on how teaching effectiveness is defined can affect faculty members’ decision to enrol in FD workshops and subsequently how they experience FD in MH. Thus, equipping faculty members with teaching skills may not be adequate. A “train-the-trainers” approach where teaching competencies are complemented with knowledge about MH’s content, methodologies, theoretical frameworks, and assessment tools may be preferable. This approach ensures that faculty members not only develop the skills required to co-facilitate MH programmes, but also reinforces the value of MH when employed within ME.
Secondly, Steinert et al.’s (2016) Best Evidence Medical Education (BEME) guide on faculty development in ME concludes that the outcomes of FD programmes should include the development of a community of practice that can affect organisational and cultural change towards education. In countries such as Singapore where the field of MH within ME is still in its nascent stage, building a community of practice (COP) is essential. A COP can increase awareness and promote endorsement by both senior leadership and peer educators, ensuring programme sustainability beyond initial “pilot” programmes. We hope that this study can inspire like-minded educators to develop FD programmes in tandem to the novel MH programmes that they implement.
Finally, we would also like to remind readers that with its unique methodologies like narrative inquiry, close reading, and experiential learning frameworks, the FD programmes for MH for medical educators have the potential to contribute to professional identity formation and foster wellbeing (Ong et al., 2024). These outcomes though not listed as the learning objectives of our study, have been consistently expressed by the participants during our workshops.
VI. CONCLUSION
In summary, we have described and presented the quantitative outcomes of a faculty development (FD) workshop specific to the field of medical humanities. Qualitative data is still needed for programme evaluation. Addressing gaps in the current literature, we recommend that all MH FD programmes incorporate an introduction to MH and its methodologies, look beyond teaching effectiveness to include systemic awareness and support, assess outcomes such as professional identity formation, and build communities of practice. Future research into these aspects and the development of validated learning outcome measures that include qualitative data will enhance current insight on FD and support the call for integrating MH within the medical education landscape.
Notes on Contributors
OEK conceptualised the outline of the paper and focused mainly on the perspectives from clinicians and clinician educators. He also designed and taught at the faculty development workshops, reviewed and approved the final draft of the manuscript, and agree to be accountable for all aspects of the paper.
LKRK conceptualised the outline of the paper and focused mainly on the perspectives from clinicians and clinician educators. He also designed and taught at the faculty development workshops, reviewed and approved the final draft of the manuscript, and agree to be accountable for all aspects of the paper.
JZ conceptualised the outline of the paper and focused mainly on the perspectives from clinicians and clinician educators. She also designed and taught at the faculty development workshops, reviewed and approved the final draft of the manuscript, and agree to be accountable for all aspects of the paper.
SWS conceptualised the outline of the paper and focused mainly on the perspectives from clinicians and clinician educators. She also reviewed and approved the final draft of the manuscript, and agree to be accountable for all aspects of the paper.
ATA contributed to the layout of the paper and focused on perspectives as medical humanities scholars and teachers. She also designed and taught at the faculty development workshops, reviewed and approved the final draft of the manuscript, and agree to be accountable for all aspects of the paper.
CM contributed to the layout of the paper and focused on perspectives as medical humanities scholars and teachers. She also designed and taught at the faculty development workshops, reviewed and approved the final draft of the manuscript, and agree to be accountable for all aspects of the paper.
FCT contributed to the layout of the paper and focused on perspectives as performing arts practitioners and tutors. He also designed and taught at the faculty development workshops, reviewed and approved the final draft of the manuscript, and agree to be accountable for all aspects of the paper.
CYX contributed to the layout of the paper and focused on perspectives as performing arts practitioners and tutors. She also designed and taught at the faculty development workshops, reviewed and approved the final draft of the manuscript, and agree to be accountable for all aspects of the paper.
NF contributed to the layout of the paper and focused on perspectives as performing arts practitioners and tutors. She also designed and taught at the faculty development workshops, reviewed and approved the final draft of the manuscript, and agree to be accountable for all aspects of the paper.
Ethical Approval
The project was submitted to the SingHealth centralised institutional review board (IRB) but exempted from review due to its nature as a medical education programme evaluation (CIRB number 2023/2036).
Data Availability
The data that support the findings of this study are openly available in the Figshare repository https://doi.org/10.6084/m9.figshare.27038086 (Ong et al. 2024).
Acknowledgement
We would like to thank Ms Eve Seraphina Low for setting up the online survey form and correspondence with the participants, and logistical support of the conduct of the workshop.
Funding
The faculty development workshop was supported by the SingHealth Oncology Academic Clinical Programme Education Support Grant (project number 08/FY2022/P2/09-A75).
Declaration of Interest
All of the authors state no conflicts of interest.
References
Howley, L., Gaufberg, E., & King, B. (2020). The fundamental role of the arts and humanities in medical education. Washington, DC: AAMC.
Kumagai, A. K., White, C. B., Ross, P., Purkiss, J. A., O’Neal, C. M., & Steiger, J. A. (2007). Use of interactive theater for faculty development in multicultural medical education. Medical Teacher, 29(4), 335-340. https://doi.org/10.1080/01421590701378662
Ong, E. K. (2021). HAPPE – A pilot programme using humanities to teach junior doctors empathy in a palliative medicine posting. The Asia Pacific Scholar, 6(1), 83-92. https://doi.org/10.29060/TAPS.2021-6-1/OA2251
Ong, E. K., Tan, E. U., Min, C., & Sim, W. S. (2024). The employment of art therapy to develop empathy and foster wellbeing for junior doctors in a palliative medicine rotation – A qualitative exploratory study on acceptability. BMC Palliative Care, 23(1), 84. https://doi.org/10.1186/s12904-024-01414-6
Ong, E. K., Aung, A. T., Min, C., Krishna, L. K. R., Chen, Y., Tariao, F. C., Ng, F., Zhou, J., & Sim, W. S. (2024). Data from pre- and post-surveys of participants [Dataset]. Figshare. https://doi.org/10.6084/m9.figshare.27038086
Steinert, Y., Mann, K., Anderson, B., Barnett, B.M., Angel., C., Naismith, L., Prideaux, D., Spencer, J., Tullo, E., Viggiano, T., Ward, H., & Dolmans, D. (2016). A systematic review of faculty development initiatives designed to enhance teaching effectiveness: A 10-year update: BEME Guide No. 40. Medical Teacher, 38(8), 769-786. https://doi.org/10.1080/0142159X.2016.1181851
*Ong Eng Koon
National Cancer Centre Singapore
30 Hospital Blvd, Singapore 168583
Email: ong.eng.koon@assisihospice.org.sg
Submitted: 19 February 2025
Accepted: 14 May 2025
Published online: 7 October, TAPS 2025, 10(4), 73-76
https://doi.org/10.29060/TAPS.2025-10-4/SC3672
Astrid Pratidina Susilo1, Lucia Pudyastuti Retnaningtyas1, Lisa Aditama2 & Karunia Wijayanti3
1Faculty of Medicine, Universitas Surabaya, Indonesia; 2Faculty of Pharmacy, Universitas Surabaya, Indonesia; 3Faculty of Medicine, Universitas Negeri Surabaya, Indonesia
Abstract
Introduction: Healthcare professionals need to advocate for mothers and understand breastfeeding challenges, especially in a community-based culture. We developed a breastfeeding management course for healthcare professionals and students in health-related majors on an online platform at our university. This study aimed to explore what participants learned from an experiential learning assignment to interview mothers regarding their breastfeeding challenges, and write a reflection on it.
Methods: In this qualitative study, we analysed the written reflections of 56 participants after they interviewed mothers regarding their breastfeeding challenges. Thematic analysis and triangulation among the researchers were conducted to obtain themes.
Results: Four themes were identified: (1) differences in knowledge and beliefs about breastfeeding among mothers and their families, (2) breastfeeding challenges that can be a threat to breastfeeding, (3) healthcare professionals’ central role in providing education and advocating for breastfeeding, and (4) involvement of the family and community in breastfeeding education.
Conclusion: This interview and reflective writing assignment strengthened the participants’ awareness of how to advocate for breastfeeding mothers, including considering the influence of the community context.
Keywords: Breastfeeding, Communal Culture, Experiential Learning, Reflective Writing
I. INTRODUCTION
Breastfeeding is a natural method of providing the best nutritional intake for babies’ growth and development, and strengthening the emotional bond between the mother and the baby. The low rate of breastfeeding is a global problem because only less than half of babies under six months of age are exclusively breastfed (Balogun et al., 2015).
Several factors influence breastfeeding, including stigma and support from people closest to the mother. These factors are prominent in communal cultures where the influence of family and community is strong (Susilo et al., 2019). Healthcare professionals can encourage the success of breastfeeding programs by providing education to mothers and their families. Therefore, they need to learn about breastfeeding management and strategies to increase public knowledge. Apropos this, mother-centred advocacy tailored to mothers’ needs can be offered by healthcare professional (Mulcahy et al., 2022).
We developed a breastfeeding management training program for healthcare professionals and students through an online course platform. One of the assignments in this course was to interview breastfeeding mothers and write reflections on their experiences. According to Kolb’s Experiential Learning Theory, this learning activity can help learners conceptualise the essential principles they must master (Yardley et al., 2012). Such a learning activity is innovative and scarcely reported in the existing literature. Additionally, this assignment is novel in the field of breastfeeding-related education. A systematic review of breastfeeding training reported that only one breastfeeding training program used reflective writing (Mulcahy et al., 2022). This study aimed to explore what participants learned from an experiential learning assignment of interviewing mothers on their breastfeeding challenges and writing reflections afterwards.
II. METHODS
This qualitative study used an interpretive descriptive approach to identify themes and patterns among subjective perspectives based on the reflections of breastfeeding management training participants. The training was conducted online through our university’s open online course platform Ubaya Global Academy (UGA). This online course consisted of six sessions and targeted healthcare professionals and students from different domains (medicine, pharmacy, and midwifery). The six sessions were basic science of breastfeeding, common challenges in breastfeeding for healthy mothers (part 1), common challenges in breastfeeding for healthy mothers (part 2), supporting breastfeeding in mothers with specific health issues (non-communicable disease), supporting breastfeeding in mothers with specific health issues (communicable disease), and essential principles in breastfeeding (wrap up and reflection). Students should have completed their first year of education to have basic exposure to health sciences. We invited all participants who had attended the training to participate in this study. At the beginning of the second session, each participant interviewed a mother who had breastfeeding experience, following which, they wrote a reflective writing of 200-500 words.
|
No |
Question |
|
1 |
Why did mothers choose to provide breast milk for babies? |
|
2 |
What were the challenges in the breastfeeding process, and how can they be overcome? |
|
3 |
What food, medicines, or activities do they believe facilitate or inhibit breast milk production (examples of beliefs: eating katuk leaves and breast massage can facilitate breastfeeding)? Where did the mother or partner get this information about food, medicine, and activities? |
Table 1. Interview Questions
We analysed the data using a thematic analysis approach by reading and re-reading the reflective writings, selecting relevant ideas, coding and grouping them according to their similarities, and organising them into themes and subthemes based on the results of interviews and participants’ reflections. Atlas.ti version 24 was used to manage the data. Data triangulation was conducted between researchers by discussing themes and differences until a consensus was reached.
III. RESULTS
Fifty-six participants agreed to participate in the study and completed the interviews. Forty-five of them were from medicine, eight from pharmacy, and three from midwifery. There were variations in participants’ reflective writing, and the following four themes emerged:
A. Differences in Knowledge and Beliefs about Breastfeeding among Mothers and Their Families
Participants reflected that mothers’ knowledge and beliefs about breastfeeding varied depending on the information they received from their surroundings. Family members were their main sources of information on ways to overcome breastfeeding challenges.
‘The mother tried to commit to breastfeeding for six months. But when she fell ill and was weak, she had to give formula milk to the child on the advice of her mother-in-law, but after that, the child did not want to drink breast milk.’ (P24)
B. Breastfeeding Challenges that can be a Threat to Breastfeeding
Participants indicated that mothers faced various obstacles in breastfeeding, such as the pain experienced by them during breastfeeding, which may force them to switch to formula milk. Problems that triggered pain included low milk production, swelling of the breasts, and sore nipples. Mother’s health was also a reason for the people around her to support breastfeeding cessation. Another challenge in breastfeeding was mother’s readiness to breastfeed, particularly for working mothers to manage their time for breastfeeding. Therefore, healthcare professionals should explore the challenges of breastfeeding before providing appropriate advice.
‘In the Integrated Services Post (Posyandu), midwives or health workers can open a special session on questions about breastfeeding.’ (P28)
C. Healthcare Professionals’ Central Role in Providing Education and Advocating for Breastfeeding
Healthcare professionals should have adequate knowledge of breastfeeding management, good communication skills, ability to demonstrate breastfeeding techniques, and educational strategies to the public. They should also involve community leaders and use social media platforms to promote breastfeeding.
‘It is essential for healthcare workers to provide proper education, not endorse and recommend products such as breast milk supplements, whose ingredients and side effects are unknown. Instead, they must teach and provide education on benefits of breastmilk, breast massages which can facilitate mother’s breast milk production, and on managing stress which can impact breast milk production.’ (P48)
D. Involvement of the Family and Community in Breastfeeding Education
Participants reflected that breastfeeding is influenced by cultural aspects; if the mother does not have prior breastfeeding experience, she is likely to believe information provided by the people around her. Hence, apart from the mothers, breastfeeding education must also be extended to companions and families. Such education must include factors to support breastfeeding such as preparation and methods for giving breast milk, and appropriate information about lactation.
‘We as healthcare workers must pick up the ball by providing mass education to the community, especially to family members who are “always” supposed to be listened to. Breastfeeding education will be in vain if we do not educate the public. We are also responsible for the health and quality of the nation’s future generations.’ (P25)
IV. DISCUSSION
Healthcare professionals must possess mother-centred advocacy skills to promote breastfeeding. Increasing their understanding through educational measures is a commitment to achieving better breastfeeding coverage and improving maternal and child health (Mulcahy et al., 2022). In line with the principles of Kolb’s Experiential Learning Theory, the interviews provided authentic exposure to the participants where they could practice skills to explore mothers’ beliefs and knowledge, and develop an empathetic attitude towards mothers’ challenges. The reflection process also enabled them to strengthen their understanding and conceptualise their interpersonal skills and professional development (Yardley et al., 2012).
Participants reflected that knowledge and beliefs of mothers are essential factors in sustaining breastfeeding. Mothers’ lack of independence from family influence and low self-confidence in overcoming challenges are considered to be related to short duration of breastfeeding (Balogun et al., 2015). The communal culture often affects mothers’ decision-making regarding breastfeeding as they are dependent on informal information from the surrounding people. Though this information may help them overcome breastfeeding-related problems, it may not necessarily be evidence-based (Susilo et al., 2019).
Hence, participants were aware of the urgency with which healthcare professionals must act to provide appropriate breastfeeding counselling. This assignment helped them critically think about mothers’ perceptions of challenges in breastfeeding and their own future actions to support breastfeeding. This comprehensive understanding will help promote breastfeeding, by providing mother-centred advocacy and breastfeeding counselling with appropriate advice and anticipatory steps to overcome breastfeeding obstacles (Radzyminski & Callister, 2015).
Our study showed that the participants were motivated to play a central role in supporting breastfeeding mothers. This assignment served as a strong trigger to motivate participants to improve the knowledge about breastfeeding management they would obtain throughout the course.
This study has two limitations. First, the analysis of participants’ awareness was based on their reflective writing skills, which may be diverse as they have not been consistently introduced in academic institutions in Indonesia. This may have influenced how the participants expressed their understanding in their reflective writing. Oral reflections can yield different themes. Second, this study focused only on the interviews and reflective writing assignments of the course, as we believe that an intensive look at these would provide valuable lessons. Triangulation with other data is necessary to determine the effectiveness of the entire course.
V. CONCLUSION
An assignment based on experiential learning principles made participants aware of the diversity of knowledge and beliefs of breastfeeding mothers in a communal culture and the potential challenges for mothers deciding to stop breastfeeding. The reflection process motivated them to learn about mother-centred advocacy for breastfeeding mothers and their surroundings.
Notes on Contributors
Astrid Pratidina Susilo designed the study, conducted the data collection and analysis, and drafted the manuscript.
Lucia Pudyastuti Retnaningtyas designed the study, conducted the data collection and analysis, and reviewed the manuscript.
Lisa Aditama designed the study, conducted the data collection, and reviewed the manuscript.
Karunia Wijayanti designed the study, conducted the data analysis, and drafted the manuscript.
Ethical Approval
This study was approved by the institutional ethics committee of Universitas Surabaya (No. 179/KE/VII/2023). All the participants provided written informed consent.
Data Availability
We do not share the raw data as the reflective writing assignments were in Indonesian. Readers who are interested in accessing the data can contact the author.
Acknowledgement
We are grateful to the Ubaya Global Academy (UGA) management team for supporting the development and implementation of this online course. We also thank Santi Desi, Denny Herliana, and Laurentia Audi Agatha for their administrative support for this study. This study was presented at the International Conference of the AMEE 2024.
Funding
This research was supported by the Ministry of Education, Culture, Research, and Technology of Indonesia (Grant Number 109/E5/PG.02.00.PL/2024).
Declaration of Interest
No potential conflicts of interest are relevant to this article.
References
Balogun, O. O., Dagvadorj, A., Anigo, K. M., Ota, E., & Sasaki, S. (2015). Factors influencing breastfeeding exclusivity during the first 6 months of life in developing countries: A quantitative and qualitative systematic review. Maternal & Child Nutrition, 11(4), 433-451. https://doi.org/10.1111/mcn.12180
Mulcahy, H., Philpott, L. F., O’Driscoll, M., Bradley, R., & Leahy-Warren, P. (2022). Breastfeeding skills training for health care professionals: A systematic review. Heliyon, 8(11). https://doi.org/10.1016/j.heliyon.2022.e11747
Radzyminski, S., & Callister, L. C. (2015). Health professionals’ attitudes and beliefs about breastfeeding. The Journal of Perinatal Education, 24(2), 102-109. https://doi.org/10.1891/1058-1243.24.2.102
Susilo, A. P., Marjadi, B., Dalen, J. V., & Scherpbier, A. (2019). Patients decision-making in the informed consent process in a hierarchical and communal culture. The Asia Pacific Scholar, 4(3), 57-66. https://doi.org/10.29060/TAPS.2019-4-3/OA2085
Yardley, S., Teunissen, P. W., & Dornan, T. (2012). Experiential learning: AMEE guide No. 63. Medical Teacher, 34(2), e102-e115. https://doi.org/10.3109/0142159X.2012.650741
*Lucia Pudyastuti Retnaningtyas
Faculty of Medicine, University Surabaya, Indonesia
Jl. Raya Kalirungkut, Surabaya 60293
+628113113338
Email: luciaretnaningtyas@staff.ubaya.ac.id
Submitted: 11 January 2025
Accepted: 11 August 2025
Published online: 7 October, TAPS 2025, 10(4), 77-80
https://doi.org/10.29060/TAPS.2025-10-4/SC3818
Yassar Alamri
Department of Medicine, University of Otago, Christchurch, New Zealand
Abstract
Introduction: Response rates to surveys of medical students and junior doctors have not previously been explicitly examined. Reasons for the observed response rates have not been scrutinised. The aims of the present study were to establish an expected response rate to electronic survey among medical students and junior doctors, and to explore reasons behind non-response.
Methods: A follow-up online survey was sent to 93 medical students and junior doctors. The primary method for participants to complete the survey was via the Internet using a well-known and established survey tool. Descriptive and inferential statistics were used to assess response rates and reasons for non-response.
Results: Out of 93 invited medical students and junior doctors, 47 returned the follow-up survey (response rate = 50.5%). The main reasons for non-response were: there were too many surveys (74.4%), lack of time (25.5%), and the original survey being too long (10.6%).
Conclusion: We found a mediocre response rate (50.5%) to electronic surveys by medical students and junior doctors included in this study. Several factors that may impede response to surveys (survey-related, and participant-related) have been identified, and these may be specifically targeted to improve survey response rates.
Keywords: Medical Student, Survey, Response Rate, Research, Methodology
I. INTRODUCTION
Surveys offer an important method of collecting quantitative data from physicians and medical students on various aspects of medical and clinical research. The ease and convenience of online and web-based surveys (compared with telephone or face-to-face interviews) should theoretically enhance response rates. However, the ideal method of surveying the medical workforce (which would yield a high rate of and representative responses) is yet to be identified.
Physicians have traditionally been reported to have poor response rates to surveys in general. Studies that have specifically assessed response rates to surveys among physicians revealed overall rates of 35–50% (Cunningham et al., 2015). Response rates to surveys and reasons for non-response by medical students and junior doctors have seldom been specifically examined. Previous response rates to the National Physician Survey in Canada reported response rates of approximately 28–35% by medical students and junior doctors (Grava-Gubins & Scott, 2008), although these data are almost two decades old now.
Several reasons for non-response emerge from reviewing the pertinent literature; these can be divided into: survey-factors, and respondent-factors. Survey-factors include the length of the questionnaire (Grava-Gubins & Scott, 2008), perceived interest in and sensitivity of the surveyed topic (Cunningham et al., 2015), and the mode of survey delivery (i.e., electronic, telephone or face-to-face) (Grava-Gubins & Scott, 2008; Weaver et al., 2019). Several incentives have been instigated in order to improve response rates by addressing some of these survey-factors, including utilising electronic surveys that can be completed in more than one setting (at the participants’ convenience)(Weaver et al., 2019), monetary gifts or “educational credit” for participation (Grava-Gubins & Scott, 2008; Viera & Edwards, 2012), and employing internal “buy in” from a respected member of the intended sample (e.g., senior clinician or head of department) (Akl et al., 2011). Respondent-factors for non-response include lack of time, demographic differences, and the specialty of the respondent.
The aims of the present study were to establish an expected response rate to electronic survey among medical students and junior doctors, and to explore reasons behind non-response. No previous study has focused on medical students and junior doctors (i.e., junior medical workforce); therefore, addressing these issues would help fill several gaps in our knowledge.
II. METHODS
A. Study Setting
A previous study (Alamri et al, in press) invited all medical students at the University of Otago, and junior doctors at the Christchurch Hospital (both in Christchurch, New Zealand), to complete an electronic ‘index questionnaire’ on their research activities. The overall response rate of the original survey was 36% despite employing an online survey, several reminders and monetary gift vouchers.
B. Study Participants and Instrument
For the present study, eligible participants were medical student and junior doctor who had started the ‘index questionnaire’, but never completed it. The identified ‘non-responders’ were then invited to a secondary follow-up survey which was sent after the allotted time-period for the index questionnaire had lapsed (August–September 2018).
The follow-up survey was intentionally designed to be very brief, and based upon previous similar surveys (Cunningham et al., 2015). It only included four questions: participant age and sex, current career, and “what were the reasons for not completing [the index questionnaire]?”.
C. Statistical Analysis
Descriptive statistics (means ± standard deviations, and percentages) were used to analyse most of the data. Comparisons between medical students and junior doctors (two sub-populations with different responsibilities and time commitments) were conducted using Chi-square analyses for categorical values (e.g., sex, and entry to medical school), and Mann-Whitney U test for nonparametric continuous variables (e.g., age). Statistical significance was determined if type I error rate was < 5% (p-value < 0.05). All analyses were performed using the Statistical Package for Social Sciences software (SPSS Statistics®, version 22.0.0.0).
III. RESULTS
A. Study Participants
A total of 93 eligible participants were identified as potential participants. Following electronic invitation, 47 returned the follow-up survey (response rate: 47/93 = 50.5%). Two thirds (31/47; 66%) of the respondents were female. The median age was 23 years (range, 19–42). Most of the respondents (40/47, 85.1%) were medical students (see Table 1).
|
|
Medical students |
Junior doctors |
p value |
|
N |
40 |
7 |
|
|
Sex (% male, standard error) |
40% (0.08) |
22% (0.09) |
0.15 |
|
Age (mean, SD) |
21.2 ± 3.7 |
24.9 ± 5.5 |
0.01 |
|
Entry to medical school (% post-graduate) |
71.8% |
59.1% |
0.33 |
Table 1. Summary of participant data
B. Non-Response Survey Findings
Reasons for non-response varied among the participants. The most common reasons included: there were too many surveys (74.4%), lack of time (25.5%), the original survey was too long (10.6%), participant erroneously thought they had completed the survey (8.4%), and participant did not think they were eligible (2.1%). Of note, two of the participants (4.3%) responded unfavourably to the offer of the follow-up survey, finding it annoying and offensive.
IV. DISCUSSION
The response rate to the follow-up survey was 50.5% which was lower than anticipated. Non-responders to the index questionnaire were re-contacted to explore reasons behind the observed low response rate. The most common cited reasons were there were too many surveys requests (‘survey fatigue’), and lack of time. Just under 10% of participants had genuinely thought that they completed the original survey, which may indicate an underlying technical problem/lack of clarity. These reasons generally echo those voiced by physician specialists when asked about their response rates (Cunningham et al., 2015), although no studies have examined these reasons in medical students or junior doctors.
Only a handful of previous studies have specifically examined the rates of survey response by medical students and junior doctors. Canadian medical students had response rates of 30.8–31.2% to an electronic version of the Canadian National Physician Surveys in 2004 and 2007 (Grava-Gubins & Scott, 2008). From our experience over several studies in New Zealand, the average response rate from medical students seems to be around 30–35% (Alamri et al, in press). Response rates from junior doctors seem to be even lower, with 27.9–35.6% response rates in Canada (Grava-Gubins & Scott, 2008), and 24.9% in New Zealand (Alamri et al, in press). The range of response rates to surveys by junior doctors varies significantly—at least in part due to the fact that some of the surveys were compulsory to complete (thus, resulting in very high response rates).
Whilst a survey’s response rate ought not be the sole judge of the study’s validity (Cunningham et al., 2015), it is important to understand the reasons behind low survey response rates. We are unaware of any studies that have examined reasons for students’ survey non-response, or factors that would influence them. On the other hand, several randomised trials examined the effect of various factors on the response rates by physicians. Factors that increased response rates by physicians included: contact by regular mail (Akl et al., 2011) (although this finding was inconsistent among studies (Viera & Edwards, 2012), and the availability of the survey in several local languages (Grava-Gubins & Scott, 2008). Factors that worsened response rates included: offering continuing medical education credits for completing a survey (Viera & Edwards, 2012), and surveys on sensitive topics (Cunningham et al., 2015). Finally, factors that had no influence on response rates included: length of the survey (Akl et al., 2011), the day of invitation to the survey (Akl et al., 2011), and monetary compensation for participation (Akl et al., 2011).
V. CONCLUSION
Our findings generally reflect those reported in the literature of the response rates to research surveys by medical professionals; these seem to vary between 25 and 50% (usually at the lower end for junior doctors/medical students, and the higher end for specialists). Several factors that impede response to surveys (survey-related, and participant-related) have been identified, including the number of surveys sent to medical professionals, and the general lack of time.
The current study was limited by the relatively small number of participants, and by the fact that it originates from a single centre in New Zealand which may limit its generalisability. However, it provides a unique perspective by targeting survey non-responders (i.e., the population of interest), offers recent and updated data, and corroborates findings from previous studies in other settings/countries.
Finally, it is imperative to acknowledge that a high response rate may not necessarily be the panacea to the perfect survey study. How factors can be manipulated in order to yield higher response rates remains to be answered. One solution could be the implementation of an advisory body that provides guidance to researchers about how to design surveys, and regulates the number of survey invitations received by medical professionals in order to avoid ‘survey fatigue’.
Notes on Contributors
The sole author conceived the idea, collected and analysed the data and wrote the manuscript.
Ethical Approval
This study was approved by the University of Otago Human Ethics Committee (reference D18/207). All participants provided consent on the electronic survey form.
Data Availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request after completion of data publication as this remains a work in progress.
Acknowledgement
The authors would like to extend their gratitude to the Department of Psychological Medicine, University of Otago, Christchurch, for their financial assistance with participant compensation. The Department had no involvement in the study otherwise.
Funding
The author received financial assistances (NZ $1,500) from the Department of Psychological Medicine, University of Otago, Christchurch in the form of gift vouchers in order to reimburse participants in our study.
Declaration of Interest
The author declares no conflicts of interest, including financial, consultant, institutional and other relationships that might lead to bias or a conflict of interest.
References
Akl, E. A., Gaddam, S., Mustafa, R., Wilson, M. C., Symons, A., Grifasi, A., McGuigan, D., & Schünemann, H. J. (2011). The effects of tracking responses and the day of mailing on physician survey response rate: Three randomized trials. PLoS One, 6(2), e16942. https://doi.org/10.1371/journal.pone.0016942
Cunningham, C. T., Quan, H., Hemmelgarn, B., Noseworthy, T., Beck, C. A., Dixon, E., Samuel, S., Ghali, W. A., Sykes, L. L., & Jette, N. (2015). Exploring physician specialist response rates to web-based surveys. BMC Medical Research Methodology, 15, 32. https://doi.org/10.1186/s12874-015-0016-z
Grava-Gubins, I., & Scott, S. (2008). Effects of various methodologic strategies: Survey response rates among Canadian physicians and physicians-in-training. Canadian Family Physician, 54(10), 1424-1430. https://www.cfp.ca/content/54/10/1424.long
Viera, A. J., & Edwards, T. (2012). Does an offer for a free on-line continuing medical education (CME) activity increase physician survey response rate? A randomized trial. BMC Research Notes, 5, 129. https://doi.org/10.1186/1756-0500-5-129
Weaver, L., Beebe, T. J., & Rockwood, T. (2019). The impact of survey mode on the response rate in a survey of the factors that influence Minnesota physicians’ disclosure practices. BMC Medical Research Methodology, 19(1), 73. https://doi.org/10.1186/s12874-019-0719-7
*Yassar Alamri
Department of Medicine, Christchurch Hospital,
2 Riccarton Avenue, Christchurch 8011,
New Zealand
Email: yassar.alamri@nzbri.org
Submitted: 13 February 2024
Accepted: 28 April 2025
Published online: 1 July, TAPS 2025, 10(3), 75-79
https://doi.org/10.29060/TAPS.2025-10-3/SC3235
Tayzar Hein1 & Susan Somerville2
1Department of Medical Education, Defence Services Medical Academy, Myanmar; 2University of Dundee, Scotland
Abstract
Introduction: Case-Based Learning (CBL) is increasingly used in modern medical schools to improve students’ critical thinking and problem-solving skills. While CBL is established in Western Resource-Structured (WRS) educational settings, its use in Asian-Pacific regions like Myanmar is under explored. This research studied the integration of CBL at the Defence Services Medical Academy (DSMA) in Myanmar, focusing on the perspectives of both students and faculty involved in curriculum reforms.
Methods: This study used constructivist grounded theory to gather data from 24 DSMA participants through four focus group discussions. Twelve students and twelve faculty members, were invited a subgroup of six, and after providing informed consent discussed their experiences of CBL, aiming to assess its effectiveness and relevance in their specific educational and cultural context.
Result: Analysis shows that students valued CBL for enhancing group discussions, reflecting upon real-world situations, and building critical thinking abilities. Faculty members also appreciated CBL for its capacity to create realistic applications and its support for student-centered learning and interpersonal skills development. Both groups acknowledged CBL as an effective method for simulating the complexities of medical practice.
Conclusion: This study found that CBL is well-regarded at DSMA for preparing students competence and confidence for clinical encounters. However, faculty indicated that the extensive time required in preparation of this teaching modality was a significant challenge for the wider adoption of CBL. These insights highlight the adaptability and potential challenges of implementing CBL in non-Western educational settings and suggest possible areas for development for its broader application in the Asia-Pacific region.
Keywords: Medical Education, Case-based Learning, Perceptions, Grounded Theory, Focus Group Discussion
I. INTRODUCTION
In 2017, Defence Services Medical Academy (DSMA) in Yangon, Myanmar, introduced an outcome-based integrated curriculum incorporating Case-Based Learning (CBL) as a key pedagogical approach. This shift from teacher-centered to student-centered learning was aimed at encouraging students to take greater responsibility for their education. However, CBL’s widespread adoption across all subjects at DSMA remains uncertain, highlighting the need for further research. CBL has been established in Western Resource-Structured (WRS) medical education, where it fosters critical thinking, active learning, and problem-solving skills (Thistlethwaite et al., 2012). However, its adoption in the Asian-Pacific context, including Myanmar, has been limited. Cultural and institutional challenges such as insufficient faculty training, resource constraints, and resistance to pedagogical change present unique barriers (McLean, 2016; Yoo & Park, 2015). These challenges underline the importance of research to adapt CBL to resource-constrained settings.
At DSMA, CBL is relatively new, and while the institution can be considered an early adopter within the local context, faculty have faced challenges transitioning from traditional teaching methods due to inadequate training and support (Thistlethwaite et al., 2012). This study aimed to explore how students and faculty perceive the implementation of CBL and to assess the opportunities and challenges of CBL in a resource-constrained, Asian-Pacific context. By addressing gaps in the CBL literature, this research contributes valuable insights for adapting pedagogical practices to diverse cultural and educational settings.
This study aimed to explore:
- How students and faculty at DSMA perceive the implementation of CBL.
- The opportunities and challenges associated with implementing CBL in a resource-constrained, Asian-Pacific context.
By addressing gaps in the CBL literature, particularly in non-WRS settings, this research contributes to a better understanding of how pedagogical practices can be adapted to diverse cultural and educational contexts, offering insights for both early and late adopters within similar settings.
II. METHODS
This qualitative study used a constructivist grounded theory approach, focusing on the experiences and meanings constructed by participants engaged with CBL in the DSMA integrated curriculum.
A. Sampling and Focus Group Composition
Purposive sampling (Patton, 2014) was used to select participants with direct involvement in CBL activities, either as facilitators or active learners. The study included 24 participants, evenly split between 12 students and 12 faculty members. Four focus groups, each containing six participants, were conducted. To reduce power dynamics, the focus groups were divided by role, with separate groups for students and faculty.
B. Participant Demographics
Table 1 below shows the demographic breakdown of participants is for understanding the responses and receptivity to CBL.
|
Participant Type |
Year |
Medicine |
Surgery |
Pediatrics |
Obstetrics and Gynaecology |
Years Study |
|
|
Students (n=12) |
Year 3 |
2 |
1 |
1 |
0 |
4 |
|
|
|
Year 4 |
2 |
1 |
0 |
1 |
4 |
|
|
|
Year 5 |
1 |
0 |
2 |
1 |
4 |
|
|
Faculty (n=12) |
Years of experience |
||||||
|
0-4 years |
3 |
||||||
|
5-9 years |
2 |
||||||
|
10-14 years |
3 |
||||||
|
15-19 years |
2 |
||||||
|
20+ years |
2 |
||||||
Table 1. Participant demographic
C. Theoretical Framework
The constructivist grounded theory approach guided both data collection and analysis. This approach emphasises the co-construction of knowledge, meaning participants not only shared their experiences but actively engaged in interpreting them. The analysis followed a constant comparative method (Patton, 2014), allowing key themes to emerge from the data.
D. Data Analysis
Data were analysed using MAXQDA software, and the constant comparative method was applied to identify recurring themes and refine categories as new insights developed.
E. Ethical Considerations
Ethical approval was granted by the DSMA Ethical Review Board. Informed consent was obtained from all participants, ensuring they were aware of the study’s aims and their rights. Confidentiality and anonymity were maintained throughout the study, and all focus group discussions were audio-recorded with consent.
III. RESULTS
The core category identified in the study was that CBL is a student-centered approach that develops critical thinking, simulates discussion about real-world scenarios, and enhances interpersonal skills, making it a key facet of modern medical education. These findings emphasise the role of CBL in bridging theoretical knowledge with practical application and supporting the development of essential skills for clinical encounters. Both students and faculty members offered different but aligned perspectives, providing valuable insights into the opportunities and challenges associated with CBL.
A. Students’ Perceptions of CBL
1) Theme 1: CBL as group discussion: Students welcomed the collaborative nature of CBL, emphasising the shared learning experience it offers. One student stated, “It’s like a team effort where we learn from each other while solving problems.” This highlights the significance of peer interaction in CBL, which is consistent with research indicating that collaborative learning enhances problem-solving skills.
2) Theme 2: Real-World Relevance: Students appreciated the practical aspects of CBL, particularly its similarity to real-life clinical scenarios. A participant remarked, “It feels like we are preparing for actual hospital situations.” This theme aligns with studies showing how CBL effectively bridges the gap between theoretical knowledge and clinical practice, preparing students for real-world medical challenges.
3) Theme 3: Fostering Critical Thinking: Students frequently mentioned the role of CBL in promoting deeper analytical skills. One student shared, “CBL makes us analyse why things happen instead of just memorising.” This observation reflects the literature that highlights critical thinking as a fundamental outcome of CBL, encouraging students to engage more deeply with the material.
B. Faculty Perceptions of CBL
1) Theme 1: Preparation for Clinical Practice: Faculty members emphasised the effectiveness of CBL in preparing students for real-world medical contexts. One faculty member noted, “CBL allows students to apply their knowledge in realistic medical contexts.” This highlights the need for carefully designed scenarios that accurately mimic clinical challenges, supporting students in applying theoretical knowledge.
2) Theme 2: The Role of Facilitator: Faculty highlighted the critical role of facilitators in guiding effective CBL sessions. A faculty member stated, “Guiding discussions and asking the right questions is key to effective CBL sessions.” This underscores the importance of facilitator training, as their competence significantly impacts the success of CBL in achieving its objectives.
3) Theme 3: Development of Personal Skills: Faculty also emphasised the role of CBL in cultivating essential personal skills for medical practice, such as communication and empathy. One faculty member remarked, “CBL is instrumental in teaching students how to communicate effectively and empathise with patients, which are essential skills in medicine.” This theme reflects a structured focus on skill development, complementing students’ emphasis on the experiential aspects of learning.
IV. DISCUSSION
This study identified both the opportunities and challenges of adopting CBL in a resource-constrained, Asian-Pacific context. Students recognised CBL’s role in fostering teamwork and critical thinking, consistent with previous research (Ferguson & Lee, 2012; Thistlethwaite et al., 2012). Faculty highlighted its effectiveness in preparing students for clinical practice and developing essential interpersonal skills. However, both groups noted challenges, such as the time-intensive nature of CBL and the varying levels of facilitator preparedness.
A. Student Perspectives
Students appreciated the collaborative nature of CBL, noting that it enhanced communication and problem-solving skills. They also valued its practical relevance, which bridged the gap between theory and clinical practice. However, challenges related to the time commitment and inconsistent preparation for case studies were identified.
B. Faculty Perspectives
Faculty acknowledged the value of CBL in preparing students for real-world challenges but emphasised the importance of facilitator training. Inconsistent facilitation was cited as a barrier to effective implementation, suggesting the need for structured training programs focusing on communication and group management skills.
C. Adapting CBL for the Asian-Pacific Context
Cultural dynamics at DSMA, including hierarchical relationships, were seen as barriers to open dialogue and peer-led activities. Strategies such as peer-led activities and anonymous feedback could help mitigate these issues, creating a more inclusive and collaborative environment. Although hierarchical relationships are common across educational settings, these challenges may be viewed as institutional factors rather than unique cultural issues. Thus, the solutions proposed peer-led activities and feedback are relevant for various contexts beyond Asian-Pacific.
D. Core Category and Future Directions
The findings underscore the need for ongoing research to explore facilitation models and cultural adaptations that can optimise CBL in diverse settings. Future studies should examine how CBL can be further refined to address institutional factors like hierarchical relationships, and how these adaptations can be applied in resource-limited settings.
V. CONCLUSION
This study highlights both the strengths and challenges of implementing CBL at DSMA. Students valued CBL for its relevance to clinical scenarios and its emphasis on clinical reasoning, while faculty recognised its potential in fostering interpersonal skills. However, challenges such as inconsistent facilitation, insufficient faculty training, and the lack of localised case studies were identified. Moving forward, DSMA should focus on enhancing faculty development, particularly in facilitation skills, and integrate case studies that reflect local clinical realities. Additionally, leveraging technology to support CBL in resource-limited settings could improve access and engagement.
For the broader health education community, this study underscores the importance of adapting CBL to local contexts, considering cultural dynamics and institutional constraints. Successful implementation of CBL in resource-constrained settings requires flexibility in adapting global pedagogical methods to meet the needs of local learners and educators. Expanding CBL at DSMA, with a focus on faculty training, case study development, and the use of technology, will better prepare students for the challenges of medical practice. This study contributes to the growing body of literature on CBL and provides actionable recommendations for institutions in similar settings.
Notes on Contributors
Dr. Tayzar Hein contributed significantly to the manuscript’s conception, design, and writing, leveraging his expertise to shape its content.
Dr. Susan Somerville provided essential support during the research process, particularly in data collection and analysis, contributing to the manuscript’s presentation.
Ethical Approval
Ethics approval was granted by the Ethical Review Committee of the DSMA, Ethical Review Board (2/ ERB/ 2022).
Data Availability
The data that support the findings of this study are openly available in https://doi.org/10.6084/m9.figshare.26550262.v1.
Acknowledgement
The author would like to express sincere gratitude to their supervisor, Dr Susan Somerville, for her thoughtful guidance throughout the research project. Dr Susan Somerville provided invaluable suggestions, constant encouragement, and generously dedicated her time during video chats, despite being on the other side of the world. The support of the Ethical Review Committee at DSMA is also deeply appreciated. Their rigorous adherence to ethical standards ensured that the study met the highest research ethics guidelines, which is essential to both advancing medical knowledge and protecting human subjects.
Special thanks are extended to the Phase II medical students and faculty members who participated in interviews and provided honest, insightful discussions that significantly contributed to the research. Phase II students, typically in the years of medical education, engage in more clinical-based learning and were crucial in offering perspectives on applying Case-Based Learning (CBL) to real-world medical scenarios. Faculty members from both basic science and clinical practice domains also played an integral role in facilitating these discussions. The assistance of the Medical Education Department faculty in facilitating these interviews was also instrumental, and their support is gratefully acknowledged.
Finally, the author wishes to express heartfelt thanks to his wife and son for their unwavering support and encouragement throughout the academic journey. Without their constant love and understanding, this research project would not have been possible.
Funding
This research is entirely self-funded, as there is currently no external financial support available for the project, necessitating the coverage of all expenses independently.
Declaration of Interest
The author conducted original research and wrote this dissertation, which was not previously submitted for a degree. The author has the copyright to the dissertation according to UK Copyright Acts and University of Dundee’s rules. Any use of material from this thesis should be acknowledged.
References
Ferguson, A., & Lee, E. (2012). Desperately seeking… relevant assessment? A case study on the potential for using online simulated group based learning to create sustainable assessment practices. Legal Education Review, 22(1), Article 6. https://doi.org/10.53300/001c.6258
McLean, S. F. (2016). Case-based learning and its application in medical and health-care fields: A review of worldwide literature. Journal of Medical Education and Curricular Development, 3, S20377.
Patton, M. Q. (2014). Qualitative research & evaluation methods: Integrating theory and practice (4th ed.). SAGE Publications.
Thistlethwaite, J. E., Davies, D., Ekeocha, S., Kidd, J. M., MacDougall, C., Matthews, P., Purkis, J., & Clay, D. J. (2012). The effectiveness of case-based learning in health professional education. A BEME systematic review: BEME Guide No. 23. Medical Teacher, 34(6), e421-e444. https://doi.org/10.3109/0142159X.2012.680939
Yoo, M. S., & Park, H. R. (2015). Effects of case‐based learning on communication skills, problem‐solving ability, and learning motivation in nursing students. Nursing & Health Sciences, 17(2), 166-172. https://doi.org/10.1111/nhs.12151
*Tayzar Hein
Defence Services Medical Academy,
Pyay Road, Mingalardon Township,
Yangon, Myanmar
+9595188093
Email: dr.tayzarhein@gmail.com
Submitted: 30 October 2024
Accepted: 8 April 2025
Published online: 1 July, TAPS 2025, 10(3), 89-92
https://doi.org/10.29060/TAPS.2025-10-3/SC3562
Shanya Shanmugam1, Rajeswari Kathirvel1,2, Kayda Soh2 & Xinyi Li1,2
1Lee Kong Chian School of Medicine, Singapore; 2Division of Obstetrics and Gynaecology, KK Women’s and Children’s Hospital, Singapore
Abstract
Introduction: The Objective Structured Clinical Examination (OSCE) is a popular method for assessing medical students’ clinical proficiency. Mock OSCEs are often incorporated into medical curricula to help students familiarise themselves with the examination format. While the impact of mock OSCEs on academic performance has been studied, their perceived utility remains less explored. This study aimed to assess the effectiveness of a mock OSCE in preparing medical students for their final examinations.
Methods: A prospective study was conducted at a tertiary hospital in Singapore, involving medical students undergoing their Obstetrics and Gynaecology posting. The mock OSCE consisted of five stations and included immediate feedback from examiners. Students completed three questionnaires: pre-mock OSCE, post-mock OSCE and post final examinations, rating the utility of the session and their confidence levels.
Results: Of the cohort of 147 students, 121 responded to the pre-mock OSCE survey, 132 responded to the post-mock OSCE survey, and 105 to the survey after their final examinations. The percentage of students who found the mock OSCE useful/very useful increased significantly from 97.5% before to 98.5% after the session, and significantly decreased to 96.2% after the examinations. Confidence levels rose significantly from a mean score of 2.34/5 pre-mock to 3.89/5 post-mock, to 4.67/5 post-exam. Qualitative feedback was positive, highlighting the benefit of familiarisation with examination mark schemes.
Conclusion: The mock OSCE was well-received by students and perceived as a valuable tool in preparation for examinations. Despite the limited sample size, these findings support the implementation of mock OSCEs to enhance students’ learning and exam preparedness.
Keywords: OSCE, Undergraduate, Medical Education, Medicine, Students’ Perception
I. INTRODUCTION
The Objective Structured Clinical Examination (OSCE) is a well-established, widely utilised method for assessing the clinical proficiency of medical students. This format comprises multiple stations where students perform clinical tasks, including history taking, physical examination, and discussing clinical management. Despite being a crucial assessment tool, OSCEs can be a daunting experience for medical students. Educational institutions often incorporate mock OSCEs into curricula to alleviate this stress, allowing students to familiarise themselves with the format and receive feedback. These sessions aim to mimic the actual OSCE, allowing students to familiarise themselves with the format and requirements, and offer an opportunity to receive feedback.
The correlation between mock OSCE practice and performance in the actual OSCE has yielded mixed results in literature. Studies on medical students (Townsend et al., 2001), and residents from internal medicine (Pugh et al., 2016), paediatrics (Hilliard et al., 1998), and emergency medicine (Lee et al., 2021) have established positive correlations between mock OSCE scores and final examination scores. Conversely, a study on second-year medical students concluded that while the mock OSCE led to improved performance in individual stations, it did not cause a significant change in the pass rate of the final examinations (Chisnall et al., 2015).
While the impact of mock OSCEs on students’ academic performance has been examined, the perception of their utility among participants has not been extensively analysed. As OSCE is viewed as a stressful component of medical assessments, the introduction of mock OSCE sessions is thought to mitigate this stress by fostering confidence and familiarity among students (Chisnall et al., 2015).
We performed a study to determine the perceived effectiveness of a mock OSCE in preparing its participants for their final examinations. More specifically, the study aimed to assess whether participation in the mock OSCEs improved students’ understanding of the domain-based exam scoring system employed by markers, enhanced their time management skills, delivered valuable content, helped them develop effective approaches to OSCE stations, and boosted their confidence levels.
II. METHODS
This prospective study evaluated students’ perceptions of the mock OSCE’s utility. This was conducted at KK Women’s and Children’s Hospital (KKH), which is a tertiary hospital in Singapore. KKH caters to students from the three different medical schools in Singapore including Lee Kong Chian School of Medicine (LKC), Yong Loo Lin School of Medicine and Duke-NUS Medical school.
A mock OSCE programme was organised by the Obstetrics and Gynaecology (O&G) department for the fourth-year medical students from LKC during their O&G posting from 2022-2023. The mock OSCE was conducted three times as the students attended in three streams. This is the first of such a programme in the O&G curriculum and was introduced as this cohort had reduced clinical exposure due to COVID-19 restrictions during their clinical years.
The mock OSCE included five 10-minute stations covering history taking, physical examination, and clinical management in O&G. Students were evaluated according to the domain-based scoring system used by LKC for their final examinations. The assessment was designed to be formative in nature and the students received immediate feedback at the conclusion of each station.
The students were asked to complete anonymous questionnaires before and after participating in the mock OSCE, and after completing their final year examinations. A 4-point Likert scale was used to gauge the usefulness of the mock OSCE session, with 1 being “not useful at all” and 4 being “very useful” and a 5-point Likert scale was used to gauge confidence for final examinations, where 1 represented “not confident” and 5 represented “very confident”. The responses collected before and after the mock OSCE session were compared. The study also examined the impact of the mock OSCE on insight into exam scoring system, time management, and content relevance through Likert scale questions. Qualitative feedback was obtained through open-text responses. The data obtained through the Likert scales were combined into nominal categories. Statistical significance was determined by performing Chi-square tests, with p<0.05 being considered significant. Informed consent was implied through the voluntary participation of individuals in the questionnaires.
The study was approved and given exempt status by the Nanyang Technological University Institutional Review Board for research (IRB 2023-677).
III. RESULTS
There were 147 fourth-year medical students for the academic year 2022–2023. 121 students responded to the questionnaire prior to the mock OSCE (82.3%), 122 (83.0%) after the mock OSCE, and 105 (71.4%) after their final examinations.
Before the mock OSCE, 97 (80.8%) students believed that it would be very useful for their exam preparation, while 20 (16.7%) believed it would be useful, and 3 (2.5%) were unsure. After the mock OSCE, 120 (91.6%) students thought it was very useful for their exam preparation, with 9 (6.9%) believing it was useful, 1 (0.8%) being unsure, and 1 (0.8%) believing it was not useful. After the final examinations, 77 (74.8%) students found it to be very useful for their exam preparation, 22 (21.4%) found it was useful, 3 (2.9%) were unsure, and 1 (1.0%) found it was not useful (Figure 1). Overall, the percentage of students who found the mock OSCE useful/very useful increased from 97.5% before to 98.5% after the session and decreased to 96.2% after the examinations. The difference in perceived utility of the mock OSCE, as determined by the combining “very useful” and “useful” into one category and “unsure” and “not useful” into another, from before the OSCE, after the OSCE, and after the examinations, was statistically significant at p<0.05, with a p-value of 0.0147.

Figure 1. Comparison of perceived utility of mock OSCE
When asked to rate their confidence regarding their final examinations, the overall score improved from 2.34/5 before the mock OSCE to 3.89/5 after, to 4.67/5 after the examinations. This rise in confidence levels was statistically significant, with a p-value of <0.00001.
We asked the students to rate the domain that they found the mock OSCE helped them with the most, including improved insight into domain-based exam scoring system, improved time management, useful content, prepare an approach for OSCE stations, and improved confidence. Almost a third (n = 32, 30.5%) of the students found that the mock OSCE helped them to prepare an approach for OSCE stations the most. This was followed by improved confidence (28, 26.7%), improved insight into exam scoring system (21, 20.0%), useful content (15, 14.3%), and lastly, time management (9, 8.6%). Furthermore, a majority of students (n=70, 66.7%) felt that the O&G mock OSCE was helpful not only for the O&G component, but for the entire OSCE examination.
Qualitative feedback obtained from the students was largely positive. The common theme that surfaced was how the mock OSCE allowed students to familiarise themselves with what to expect from the final examination. Examples include:
“Helped to give us a broader understanding of how 1) clinician thinks and how 2) an examiner grades.”
“It was a great opportunity for medical students to learn about history taking and physical examination in a controlled environment.”
IV. DISCUSSION
Overall, the mock OSCE was well-received by students as a useful tool in preparation for final examinations. The differences in the perceived utility of the mock OSCE from before the OSCE, after the OSCE, and after their final examinations was statistically significant. This supports the value of the mock OSCE programme, given the students’ lack of exposure to clinical scenarios and examination structure as previously outlined. Interestingly, the proportion of students who found the mock OSCE programme useful/very useful decreased from 98.5% after the OSCE to 96.2% after final examinations. This drop can be explained by the qualitative feedback obtained, which cites the examination’s increased complexity and variations in content.
Most students felt that the mock OSCE helped them prepare their approach to OSCE stations, consistent with previous studies showing that mock OSCEs help students familiarise themselves with the format. (Lee et al., 2021, Chisnall et al., 2015) These sentiments are echoed in the qualitative feedback obtained. Furthermore, the difference in confidence levels before and after the mock OSCE was statistically significant.
This study is limited by its small sample size, ranging from 105 to 132 students. As participation was voluntary and the questions were not compulsory, some students did not complete the survey, leading to discrepancies in response rates. Furthermore, due to the anonymous nature of the surveys, we are unable to monitor for survey drop-offs. Using Likert scales to assess the utility of the mock OSCE may not fully capture participants’ opinions. Students may have interpreted the scales differently, as utility is subjective to the individuals’ standards for themselves. This could have resulted in less reliable data due to the diversity in how participants understood the scales.
V. CONCLUSION
The results of this study indicate that a mock OSCE is perceived to be an important part of examination preparation for medical students. Despite being a single-specialty mock OSCE, most students felt it was useful for preparing for their entire final exam.
These findings suggest that there is great potential in using mock OSCEs as a revision tool for medical students and support the implementation of such programmes to guide students in their learning and examination preparation.
Notes on Contributors
Shanya Shanmugam is a medical student at Lee Kong Chian School of Medicine, who is interested in medical education. She reviewed the literature, analysed data and wrote the manuscript.
Dr Rajeswari Kathirvel is a senior consultant at KK Women’s and Children’s Hospital and the principal lead for Obstetrics and Gynaecology at Lee Kong Chian School of Medicine. She, alongside with Dr Li Xinyi, designed the study, developed the questionnaire, and developed the manuscript.
Kayda Soh is an executive in KK Women’s and Children’s Hospital OBGYN Academic Clinical Programme. She was involved in administering the questionnaires and collating the data.
Dr Li Xinyi is a consultant at KK Women’s and Children’s Hospital and the posting lead for Obstetrics and Gynaecology at Lee Kong Chian School of Medicine. She, alongside with Dr Rajeswari Kathirvel, designed the study, developed the questionnaire, and developed the manuscript.
Ethical Approval
The study was approved and given exempt status by the Nanyang Technological University Institutional Review Board for research (IRB 2023-677).
Data Availability
The data that support the findings of this study are openly available in the Figshare repository, at https://doi.org/10.6084/m9.figshare.25903786.
Acknowledgement
We would like to thank the students at Lee Kong Chian School of Medicine who participated in this study.
Funding
The authors report that there is no funding associated with the work featured in this article.
Declaration of Interest
The authors report there are no competing interests to declare.
References
Chisnall, B., Vince, T., Hall, S., & Tribe, R. (2015). Evaluation of outcomes of a formative objective structured clinical examination for second-year UK medical students. International Journal of Medical Education, 6, 76–83. https://doi.org/10.5116/ijme.5572.a534
Hilliard, R. I., & Tallett, S. E. (1998). The use of an objective structured clinical examination with postgraduate residents in Pediatrics. Archives of Pediatrics & Adolescent Medicine, 152(1). https://doi.org/10.1001/archpedi.152.1.74
Lee, M. H., Phua, D. H., & Heng, K. W. (2021). The use of a formative OSCE to prepare emergency medicine residents for summative OSCE: A mixed-methods cohort study. Research Square. https://doi.org/10.21203/rs.3.rs-495003/v1
Pugh, D., Bhanji, F., Cole, G., Dupre, J., Hatala, R., Humphrey-Murto, S., Touchie, C., & Wood, T. J. (2016). Do OSCE progress test scores predict performance in a national high-stakes examination? Medical Education, 50(3), 351–358. https://doi.org/10.1111/medu.12942
Townsend, A. H., Mcllvenny, S., Miller, C. J., & Dunn, E. V. (2001). The use of an objective structured clinical examination (OSCE) for formative and summative assessment in a general practice clinical attachment and its relationship to final medical school examination performance. Medical Education, 35(9), 841–846. https://doi.org/10.1046/j.1365-2923.2001.00957.x
*Shanya Shanmugam
Lee Kong Chian School of Medicine,
11 Mandalay Road,
Singapore
Email: shanya001@e.ntu.edu.sg
Submitted: 19 October 2024
Accepted: 28 April 2025
Published online: 1 July, TAPS 2025, 10(3), 84-88
https://doi.org/10.29060/TAPS.2025-10-3/SC3547
Eranthi Weeratunga, Shashika Karunanayaka, Pramudika Kariyawasam & Bimba Wickramarachchi
Department of Nursing, Faculty of Allied Health Sciences, University of Ruhuna, Sri Lanka
Abstract
Introduction: Palliative care nursing (PCN) supports individuals with life-threatening illnesses, aiming to improve the quality of life (QoL) for patients and families. The objective was to assess the necessity of establishing an Advanced Certificate Course in PCN at University of Ruhuna, Sri Lanka.
Methods: A descriptive cross-sectional study was conducted among 220 registered nurses (RNs) using purposive sampling, working at National Hospital Galle. A pre-tested, interviewer-administered questionnaire was used, including questions on prior education or training experiences on palliative care (PC), and its principles, services, and management. Descriptive statistics and the chi-square test were used to analyse.
Results: The majority of the RNs were aged 31-40 years (45.2%), females (86.0%), and married (55.7%). A higher proportion of RNs were nursing diploma holders (67.4%), with 55.7% having less than ten years of nursing experience. Only 11.3% of the RNs had formal additional training on PC, such as workshops and a few training hours. Most RNs correctly identified PC aims: improving survival (59.7%), improving QoL of patients and their families (91.4%), providing relief and pain (93.7%), understanding PC (80.1%), etc. The majority (84.6%) had a good attitude toward palliative caregiving, though only 20.4% had average knowledge of PC. Formal PCN training was significantly associated with PC knowledge (p=0.004).
Conclusion: Limited educational exposure, average knowledge levels, and good attitudes toward PC suggest the need for a PCN course for nurses. Providing a special education programme reduces the current gaps in PC by equipping RNs with the respective knowledge, skills, and attitudes to deliver complex management for patients requiring PC.
Keywords: Palliative Care Nursing, Sri Lanka, Educational Needs, Registered Nurse
I. INTRODUCTION
Palliative care (PC) is an approach that aims to improve the quality of life (QoL) of patients and their families facing the physical, psychosocial, and spiritual problems associated with life-threatening illnesses (World Health Organization [WHO], 2022). About forty million people need a PC every year in the world, but the majority are from lower-middle-income countries (LMICs) (WHO, 2022). PC is offered by a range of professionals comprising physicians, nurses, support workers, etc., who are equally important, in addition to family members (WHO, 2022).
The major obstacle to improving PC among healthcare professionals (HCPs) and policymakers in LMICs is a lack of education/training (WHO, 2022) and a need for knowledge on PC for nursing professionals, which emphasised in previous findings in Sri Lanka (Meegoda et al., 2018) in addition to less PC content in the undergraduate curriculum (Pesut & Greig, 2018). Further, less awareness of PC, cultural/social barriers, and misconceptions was found among HCPs; PC education improved nurses’ knowledge, confidence, attitudes, and communication abilities (WHO, 2022). In Sri Lanka, there is a growing number of non-communicable diseases (NCDs), such as cancers, end-stage renal disease, HIV/AIDS, motor neuron disease, etc., that require comprehensive PC at every stage of the disease process in addition to the rapidly aging population.
PC services in Sri Lanka remain limited due to a shortage of trained HCPs. In response to the rising burden of NCDs, the Ministry of Health has emphasised the need to strengthen PC across all levels of the healthcare system. However, gaps in knowledge, skills, and attitudes among HCPs hinder effective implementation. While universities have introduced theoretical PC education, nursing undergraduates receive minimal practical exposure. Although a one-year post-basic diploma in palliative care nursing (PCN) has been launched for registered nurses (RNs), it is insufficient to meet the growing national demand. The initiation of a new course is of paramount importance, as specialisation in PCN has become an urgent necessity both nationally and internationally. The rising number of patients requiring PC, driven by demographic transitions, underscores this need. In developed countries such as Japan and Australia, the demand for PCN is expected to increase due to aging populations. Nationwide studies in Japan estimated that PC needs will continue to rise. Evidence suggests a growing demand for PC services in Australia, in particular, as the number of Australians aged over 85 continues to increase, the need for PC services has also surged. As a result, the demand for Sri Lankan RNs specialising in PC is expected to rise in these developed countries.
To address the existing gaps in PC knowledge and skills among RNs, we sought to quantify RN’s readiness for specialisation in PCN. The key objective was to assess the necessity of establishing an Advanced Certificate Course in PCN at the Department of Nursing, Faculty of Allied Health Sciences (FAHS), University of Ruhuna (UoR), Sri Lanka, to enhance professional competency and meet the growing demand for PC services.
II. METHODS
This descriptive cross-sectional study was conducted at the National Hospital Galle (NGH), Sri Lanka. The study participants were 220 RNs purposively selected based on having at least one year of experience, surveyed from June to December 2023. Data were collected using a content-validated and pre-tested questionnaire, which had been previously utilised in a Sri Lankan study (Fernando & Prathapan, 2019). The questionnaire comprised sections designed to assess socio-demographic characteristics and knowledge of four distinct domains: basic principles, service organisation, clinical management, and ethical considerations. Additionally, participants’ attitudes were evaluated after obtaining written informed consent. Statistical Package for Social Science (SPSS) 26 software was used; the descriptive statistics, frequencies, and percentages were checked. Further, a chi-square test was used. All results were regarded as statistically significant at p < 0.05.
III. RESULTS
The majority of the RNs were aged 31-40 years (45.2%). The mean±SD age was 36.61 ± 7.47 years. The majority were female (86.0%) and married (55.7%). Of the RNs, 35.7% had a monthly income between Sri Lankan Rupees 50,000 and 74,999. A higher proportion of RNs were nursing diploma holders (67.4%), with 55.7% having less than ten years of nursing experience. Emergency trauma care was the special training received by the RNs (4.5%). Only 11.3% of the RNs had formal additional training on PCN, such as workshops and a few training hours. Most RNs correctly identified PC aims (Table. 1). However, the majority gave incorrect answers regarding general knowledge/concepts of PC principles, such as increasing the life expectancy of terminally ill patients (59.7%) and consultants as ideal coordinators for PC (87.8%). Most RNs agreed that PC offers hope to patients (47.1%) and considered it a basic human right (79.6%). The majority (84.6%) had a good attitude toward PC, though only 20.4% had average knowledge of PC. Knowledge of PC was significantly associated with formal PCN training (p=0.004).
|
No. |
Statements on General Principles of PC among RNs |
Correct option |
True % |
False % |
Do not know % |
|
1 |
It is aimed at increasing the life expectancy of terminally ill patients. |
F |
57.9 |
40.3 |
1.8 |
|
2 |
It may improve survival. |
T |
59.7 |
37.1 |
3.2 |
|
3 |
PC was provided for patients of any age. |
T |
85.1 |
10 |
5.0 |
|
4 |
Aims to improve the QoL of patients. |
T |
91.4 |
6.3 |
2.3 |
|
5 |
Aims to increase the QoL of their families facing the physical, psychosocial, and spiritual problems associated with life-threatening illnesses. |
T |
91.4 |
5.0 |
3.6 |
|
6 |
Aim to provide relief from pain and control symptoms in patients. |
T |
93.7 |
5.0 |
1.4 |
|
7 |
Aim to provide psycho-social and spiritual care for patients and families. |
T |
95.0 |
2.7 |
2.3 |
|
8 |
The goal of PC is to help people better understand their treatment options. |
T |
72.4 |
20.4 |
7.2 |
|
9 |
PC could be provided together with other treatments aimed at prolonging life. |
T |
58.4 |
33.5 |
8.1 |
|
10 |
PC could be provided early in the course of illness. |
F |
34.8 |
48.9 |
16.3 |
|
11 |
Bereavement support to the loved ones following the death of the patient concerned comes under the purview of PC. |
T |
64.3 |
9.0 |
26.7 |
|
12 |
Patients with cancer, cardiovascular diseases, chronic respiratory diseases, Acquired Immune Deficiency Syndrome/AIDS, and diabetes may need PC. |
T |
81.4 |
13.6 |
5.0 |
|
13 |
Other diseases are major organ failure (kidney failure), chronic liver disease, multiple sclerosis, Parkinson’s disease, rheumatoid arthritis, neurological disease, dementia, congenital anomalies, drug-resistant tuberculosis, severe burns, extreme frailty of old age, and chronic obstructive pulmonary disease. |
T |
74.7 |
12.2 |
13.1 |
|
No. |
Statements on Service Organisation |
Correct option |
True % |
False % |
Do not know % |
|
1 |
The relevant consultant is the ideal coordinator of the multidisciplinary team involved. |
F |
87.8 |
7.7 |
4.5 |
|
2 |
PC is provided exclusively in hospices and not in tertiary healthcare institutions. |
F |
39.4 |
48.4 |
12.2 |
|
3 |
Include inpatient centers or hospice, hospital-based, community-based, and homecare. |
T |
80.1 |
8.1 |
11.8 |
|
4 |
The main duty of the “Lasting Power of Attorney” is to construct the “Advanced Care Directive”. |
F |
46.6 |
10.4 |
43.0 |
|
5 |
Pastoral caregivers are involved with the social domain of palliation. |
F |
51.6 |
12.2 |
36.2 |
|
No. |
Statements on Drugs and Management Aspects |
Correct option |
True % |
False % |
Do not know % |
|
1 |
The preferred routes of administration of drugs in the most terminal stages of life are “oral” and “rectal” (non-invasive). |
F |
60.6 |
29.4 |
10.0 |
|
2 |
Steroids improve the QoL of palliative patients. |
T |
48.9 |
34.4 |
16.7 |
|
3 |
Anti-convulsants may be added to step one of the WHO analgesic ladder. |
T |
36.2 |
30.8 |
33.0 |
|
4 |
Hyperkalaemia is the most common life-threatening metabolic emergency in palliative patients. |
T |
52.5 |
25.8 |
21.7 |
|
5 |
Due to the development of tolerance, the dosage of morphine for otherwise healthy adults is allowed up to a maximum of 600mg per day. |
F |
34.8 |
31.2 |
33.9 |
|
No. |
Statements on Ethical Concerns |
Correct option |
True % |
False % |
Do not know % |
|
1 |
PC should be incorporated into the care plan of a patient with a terminal diagnosis only after treatments with curative intent have failed. |
F |
55.7 |
27.6 |
16.7 |
|
2 |
Although “Palliative Sedation” usually hastens death, it is not considered a serious issue in the terminal stages of a patient’s life. |
F |
44.3 |
31.2 |
24.4 |
|
3 |
“Death rattle” (noisy respiratory secretions), noticed closer to the patient’s death, is one of the most distressing symptoms suffered by the patient. |
F |
59.3 |
15.8 |
24.9 |
|
4 |
Evidence shows that most patients with terminal diagnoses wish that only their next-of-kin/family understands the prognosis. |
F |
61.1 |
19.0 |
19.9 |
|
Ethical principles are concerned when applying the following PC practices. |
|
|
|
|
|
|
5 |
Have you heard about Do Not Resuscitate? (DNR) |
T |
80.1 |
7.7 |
12.2 |
|
6 |
Understanding advanced care planning in PC |
T |
62.9 |
16.3 |
20.8 |
Table 1. General principles of PC among RNs, service organisation, drug management aspects, and ethical concerns
IV. DISCUSSION
This study assessed PC knowledge, management, ethical concerns, and attitudes among RNs in the NHG, Sri Lanka. RNs reported average knowledge and satisfactory attitudes, with age and prior PC training significantly influencing knowledge levels. Compared to the current study, Fernando and Prathapan (2019) reported higher satisfactory scores.
Sri Lankan medical graduates showed limited PC knowledge (37.23%), lower than RNs (20.4%), likely due to curriculum gaps (Fernando & Prathapan, 2019; Prem et al., 2012). While young medical graduates had adequate knowledge of general principles (63%), ethics was the weakest area (19.55%), mirroring findings among RNs.
PC is a relatively new discipline in Sri Lanka, contributing to limited ethical awareness. Cultural norms favor “hiding bitter truths” over transparency rather than “telling the truth,” which is a fundamental principle in Western healthcare practices, influencing attitudes and ethical concerns (Fernando & Prathapan, 2019).
The medical graduates studied by Fernando and Prathapan (2019) were younger than the RNs in this study. Despite some PC exposure, RNs had fewer opportunities for specialised training, impacting knowledge levels. Nevertheless, their positive attitudes likely stem from empathy-based patient care within the Asian context.
A previous study highlighted insufficient PC preparedness among nurses, attributing it to curriculum deficiencies and inadequate training in pain management (Prem et al., 2012). Female RNs performed better than males, but knowledge gaps remain a global issue. Student nurses and new RNs often feel inadequately prepared to discuss end-of-life issues, death, and other ethical concerns.
Meegoda et al. (2018) emphasised the need for adequate PC knowledge among nurses, as limited PC services worsen cancer care challenges. Heavy workloads and time constraints hinder learning, and 96% of RNs had not attended PC training. In-service programmes were considered beneficial, but specialised training is mainly available in Colombo, restricting accessibility. Distance learning could bridge this gap.
Nurses are vital in PC across various healthcare settings. Skilled PCNs provide essential support to patients and families. WHO (2022) stresses PC’s role in alleviating suffering and advocates its integration into national healthcare. However, LMICs face educational and awareness barriers.
Although Sri Lankan nurses have access to higher education, PC specialisation remains limited, especially in remote areas. With rising NCDs and aging populations, introducing PCN courses is crucial. Establishing a PCN programme aligned with national priorities would enhance patient care and improve career opportunities, particularly for nurses seeking employment abroad. A PCN course at FAHS, UoR, outside Colombo, could improve access to PC education.
A. Limitations
This study highlights the need for PC training, but it has limitations. Sampling bias may affect validity, and self-reported data could introduce response bias.
V. CONCLUSION
Limited educational exposure, average knowledge, and positive attitudes toward PC indicate a need for PCN courses to address existing gaps. RNs at NHG support an Advanced Certificate Course in PCN, emphasising the necessity for specialised training. Expanding PC education will enhance patient care and create new professional opportunities. Future research should assess the impact of PC training on HCP competencies and patient outcomes. Collaboration between the University of Ruhuna and the Ministry of Health is essential for establishing a sustainable PCN course.
Notes on Contributors
EW was involved in conceptual development, data collection/entry/analysis, manuscript drafting, editing, and final correction. SK was incorporated into conceptual development, data collection/entry/analysis, and editing. Data entry/analysis, editing, and final correction were done by PK, and BW was involved in manuscript draft editing.
Ethical Approval
Ethical approval (Ref. No. 83.11.2021) and institutional approval were obtained from the Ethics Review Committee of the FAHS, UoR, and the relevant institutions/authorities.
Data Availability
Data analysed during the current study will be available from the corresponding author upon reasonable request.
Acknowledgment
The authors are grateful to the Dean, FAHS, UoR, Galle, Sri Lanka, and the Head, Department of Nursing, FAHS, UoR, Galle, Sri Lanka. The Director, Chief Grade Nursing Officer, and all in-charge nursing sisters of the National Hospital Galle are acknowledged for their permission. Ms. Nimesha and Mr. Dilan (11th batch/nursing graduates) are appreciated for their enormous contribution while collecting data despite their busy schedules. All consented RNs were further acknowledged for giving their true opinions and great support to uplift nursing education in the PCN field.
Funding
The authors received no funding for this study.
Declaration of Interest
The authors declare that they have no competing interests.
References
Fernando, G. V. M. C., & Prathapan, S. (2019). What do young doctors know of palliative care; How do they expect the concept to work? BMC Research Notes, 12(1), 1–6. https://doi.org/10.1186/s13104-019-4462-2
Meegoda, D. L., Fernando, D. M. S., Atulomah, N., Sivayogan, S., & Marasinghe, R. B. (2018). Improvement of nurses’ skills following a hybrid model educational intervention on cancer palliative care. International Journal of Health Sciences & Research, 8(5), 196–203. http://www.ijhsr.org/IJHSR_Vol.8_Issue.5_May2018/IJHSR_Abstract.031.html
Pesut, B., & Greig, M. (2018). Resources for educating, training, and mentoring nurses and unregulated nursing care providers in palliative care: A review and expert consultation. Journal of Palliative Medicine, 21(S1), S50–S56. https://doi.org/10.1089/jpm.2017.0395
Prem, V., Karvannan, H., Kumar, S. P., Karthikbabu, S., Syed, N., Sisodia, V., & Jaykumar, S. (2012). Study of nurses’ knowledge about palliative care: A quantitative cross-sectional survey. Indian Journal of Palliative Care, 18(2), 122–127. https://doi.org/10.4103/0973-1075.100832
World Health Organization. (2022). Palliative care. https://www.who.int/news-room/fact-sheets/detail/palliative-care
*Eranthi Weeratunga
Department of Nursing,
Faculty of Allied Health Sciences,
University of Ruhuna
Galle, 80 000, Sri Lanka
+94 71 440 2662, +94 77 225 8519
Email: eranthiw@ahs.ruh.ac.lk,
eranthiweeratunga@yahoo.com
Submitted: 22 July 2024
Accepted: 4 February 2025
Published online: 1 July, TAPS 2025, 10(3), 80-83
https://doi.org/10.29060/TAPS.2025-10-3/SC3470
Zaitunnatakhin Zamli1, Rohaini Ramli2, Hidayah Sulaiman2, Mohd Zulfaezal Che Azemin3, Wan Muhamad Salahudin Wan Salleh4, Nurul Asyiqin Yusof5, Imran Mahalil2 & Azmi Mohd. Yusof2
1Department of Biomedical Science, Kulliyyah of Allied Health Sciences, International Islamic University Malaysia, Malaysia; 2Department of Informatics, College of Computing & Informatics, Universiti Tenaga Nasional, Malaysia; 3Department of Optometry and Visual Sciences, Kulliyyah of Allied Health Sciences, International Islamic University Malaysia, Malaysia; 4Department of Basic Medical Sciences, Kulliyyah of Medicine, International Islamic University Malaysia, Malaysia; 5Department of Basic Medical Sciences, Kulliyyah of Pharmacy, International Islamic University Malaysia, Malaysia
Abstract
Introduction: Virtual reality (VR) has been widely used in medical and health sciences education since the late twentieth century. VR complements the conventional teaching and learning (T&L) approach by providing an engaging and immersive 3D spatial learning environment, especially for understanding the orientation of anatomical structures. Despite these advantages, the usability and student preference of highly immersive head-mounted display-based (HMD) and less immersive desktop-based (DB) VR in human anatomy courses have yet to be determined.
Methods: In a cross-sectional study, 49 Year-2 medical students were recruited through a convenient sampling. The participants were asked to identify 15 skeletal system components using the HMD and DB platform with human anatomy VR application. Both applications’ System Usability Scale (SUS) and preference scores were obtained via a self-administered questionnaire. The data were expressed as median [IQR] and statistically analysed using MATLAB R2022b.
Results: Most participants preferred the HMD over the DB platform (p=0.04), especially the male participants (p=0.01). There was no significant difference in overall SUS scores between both platforms (p=0.14). However, when compared within and between genders, females scored significantly higher in the DB than HMD (p=0.02) and higher than males’ DB SUS scores (p=0.03).
Conclusion: The overall usability of HMD was comparable with the DB platform for learning human anatomy. Although most participants prefer to use the HMD, further exploration of why females prefer the DB is needed. Subsequently, VR application developers must consider gender-related adaptions to promote the equitability and inclusivity of the technology for all users.
Keywords: Human Anatomy, Virtual Reality, Head-mounted Display, Desktop-based Application, Usability, Preference
I. INTRODUCTION
Virtual reality (VR) is a simulated three-dimensional (3D) environment that enables users to explore and interact with virtual surroundings, perceiving them through their senses as if they were in the real world. It has been widely used in various fields, including education, to provide users with immersive, engaging, and experiential learning experiences.
In medical education, VR allows students to manipulate anatomical structures into different planes, sections and orientations in a simulated environment, benefiting learners with low-spatial ability. VR also helps students better grasp the relative size differences of organs and allows students to relate the location and position of the organs with their surroundings, resulting in better memorisation and learning outcomes, with VR groups outperforming control groups in post-test assessments (Kurul et al., 2020). As the current generation is more digitally savvy, most students are easily adapted to VR simulation, which enables them to grasp knowledge from a new perspective. For instance, students can dissect a muscle from the human body, gaining insight into the interaction and innervation of individual muscles during exercise.
However, despite the high acceptability of use in anatomy courses among students, some participants reported simulator sickness symptoms like headaches, dizziness, and blurred vision. These symptoms are more pronounced in females, who tend to experience discomfort in a VR environment (Stanney et al., 2020), potentially due to differences in spatial awareness, sensitivity to sensory stimuli, or physiological responses. In addition, regardless of gender, the mismatch between visual motion and the body’s sensory feedback in VR environments can lead to sensory conflict and an increased likelihood of discomfort.
While VR modalities show great potential in anatomy education, research comparing highly immersive head-mounted display-based (HMD) with less immersive desktop-based (DB) VR platforms, particularly regarding gender differences in usability and preferences, remains limited. In addition, considering the high cost of VR applications for HMD, addressing this knowledge gap before its development is crucial to ensuring optimal and cost-effective learning outcomes for a diverse student population. Therefore, this study aimed to compare the usability and preferences between DB and HMD platforms in exploring the VR anatomy applications, within and between genders, among medical students.
II. METHODS
Upon their written consent, forty-nine undergraduate medical students (23 males and 26 females, aged 19-21 years) were recruited through a convenience sampling. They were second-year medical students and participated in this study in two sessions. The participants were asked to identify 15 skeletal components (i.e. skull, vertebrae, hyoid bone, sternum, ribs, scapula, clavicle, humerus, radius, ulna, hip bone, femur, patella, tibia, and fibula) using two platforms: a head-mounted display-based (HMD) virtual reality system with the human anatomy VR application (BodyMap v3.2, https://www.mai.ai/bodymap), and a desktop-based (DB) application (Zygote Body, https://www.zygotebody.com/). BodyMap v3.2 is a VR application for exploring the human body in 3D using the Oculus Quest 2 headset, which provides an immersive and interactive experience for anatomy education. Meanwhile, Zygote Body is a web-based platform that offers detailed 3D anatomical models for desktop or laptop exploration.
Each platform was given a time limit of 15 minutes for the participants to complete the task. After completing the task, the participants completed the System Usability Scale (SUS), a 10-item questionnaire designed to measure the perceived usability of both platforms. The SUS score ranges from 0 (very poor usability) to 100 (perfect usability). In addition, the participants were also asked to rate their preference for using each platform on a scale from 1 (do not prefer at all) to 10 (most preferred). The data were expressed as median (interquartile range, IQR), which best represents the central tendency for non-normally distributed data. Normality was assessed using the Kolmogorov-Smirnov test, and the Wilcoxon signed-rank tests were used to compare the median scores of SUS / Preferences within and between genders. All statistical analyses were performed using MATLAB R2022b, with a p-value < 0.05 considered statistically significant.
III. RESULTS
A. Demographic Data
Forty-nine Year-2 IIUM medical students participated in this study. Most of the students were female (n=26, 53%), with a mean age of 20.10 ± 0.37 years old.
B. Comparison of SUS and Preference Scores between the HMD and DB
There was no significant difference between the median SUS scores between the HMD and DB applications (p=0.14). However, most students preferred the HMD (90, IQR 80.0-100.0) rather than the DB (80, IQR 75.0-90.0) applications (p=0.04).
C. Comparison of SUS and Preference Scores of the HMD and DB within and between Gender
The SUS and preference scores of the HMD and DB applications within and between genders are shown in Figure 1, and individual scores are accessible at https://doi.org/10.6084/m9.figshare.26711965. Based on gender, significantly higher median SUS scores were observed for the DB (85, IQR 77.5-95.0) than the HMD application (75, IQR 59.4-85.6) among the female students (p=0.02). In contrast, the male students had a significantly higher preference score for the HMD (100, IQR 85.0-100.0) than the DB application (80, IQR 70.0-90.0) (p=0.01). A significant difference between gender was only observed in the SUS score, in which the female students scored 85 (IQR, 77.5 – 95.0), and the male students scored 75 (IQR, 58.1 – 86.9; p=0.03) for the DB application.
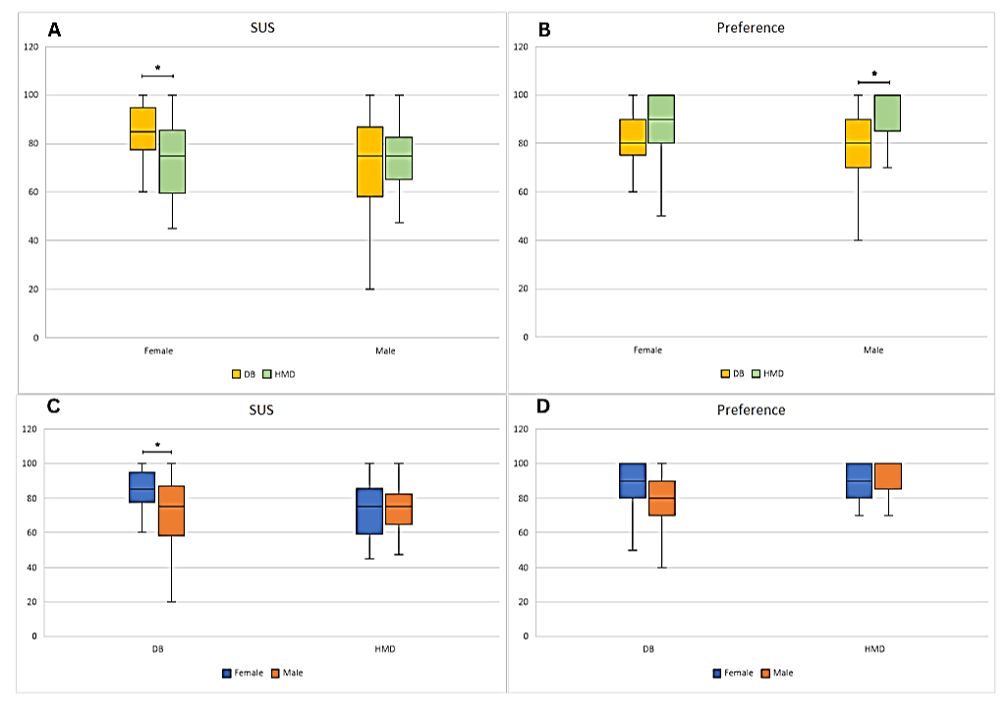
Figure 1. Comparison of SUS and Preference median scores of the HMD and DB application within (A-B) and between genders (C-D). A significant difference of p≤0.05 is denoted as *.
IV. DISCUSSION
This study found that the overall usability scores of the head-mounted display-based (HMD) and the desktop-based (DB) in human anatomy VR applications are comparable. However, a significant gender-related difference was observed in the reported usability scores of the HMD. Female participants reported significantly better usability with the DB than the HMD, likely due to their unfamiliarity with the HMD modality and disadvantage in the 3D spatial ability than males in visualising and manipulating objects in the navigating space. While traditional explanations link these gender differences to brain lateralisation, Bartlett and Camba (2023) challenge this view, suggesting societal expectations and gender roles may shape spatial skills.
Despite this, the study also found that most participants, especially males, prefer the HMD over the DB. This preference might be due to males’ active engagement and early adaptation to the technology, particularly in online gaming, making it more intuitive. This aligns with Deisinger et al. (1997), who found that inexperienced users favoured screen-based projection due to their familiarity with the conventional technology over the HMD. Interestingly, although females perceived DB as more usable, this did not significantly affect their preference for HMD. Many females acknowledged needing more technical help with the HMD but believed they would quickly adapt and prefer it over time. The study’s findings resonate with prior research in medical education, where HMDs are favoured for their immersive experience, enhancing spatial or physical presence and interaction as compared to DB (Yamazaki et al., 2021). However, the effectiveness of HMDs in improving learning outcomes compared to traditional methods remains inconclusive.
Given HMDs’ potential to enhance anatomy education, further research is crucial, especially in complex topics like embryology and neuroanatomy. Developers must focus on high content quality, intuitive user interfaces, and user comfort to ensure a positive learning experience. Gender-related adaptations can promote inclusivity, ensuring that the educational benefits of HMDs are accessible to all users.
Three main limitations of the present study also warrant mention. First, we used the available human anatomy VR applications from two developers, which may have different image quality of VR. However, both VR applications are comparable in terms of content quality. Second, we have not explored their reasons for high preference for utilising HMD when exploring human anatomy VR, potentially limiting our understanding of the user experience (e.g. comfort, immersion, satisfaction, and overall interaction) related to HMD usage. Third, participants’ previous experience using HMD in other platforms, such as gaming, virtual tours, etc, was not determined. Future studies should consider these limitations to understand user experiences with the HMD platform better and identify factors influencing user preferences.
V. CONCLUSION
In summary, this study concluded that the usability of both HMD and DB in exploring the human anatomy VR application is almost similar. As seen in other studies, students tend to favour HMD over DB because of its immersive, interactive, and engaging features. However, at an individual level, gender may influence their perception of its usability and preference. Therefore, it is essential to take gender-related adaptations into account when developing VR applications.
Notes on Contributors
Zaitunnatakhin Zamli reviewed the literature, designed the study, performed data collection and analysis, and developed the manuscript. The author has read, given critical feedback and approved the final manuscript.
Nurul Asyiqin Yusof reviewed the literature, designed the study, performed data collection and analysis, and developed the manuscript. The author has read, given critical feedback and approved the final manuscript.
Azmi Mohd Yusof reviewed the literature, designed the study, performed data collection and analysis, and developed the manuscript. The author has read, given critical feedback and approved the final manuscript.
Wan Muhamad Salahudin Wan Salleh designed the study and performed data collection, analysis and interpretation. The author has read, given critical feedback and approved the final manuscript.
Mohd Zulfaezal Che Azemin designed the study and performed data collection, analysis and interpretation. The author has read, given critical feedback and approved the final manuscript.
Rohaini Ramli advised on study design and data interpretation. The author has read, given critical feedback and approved the final manuscript.
Hidayah Sulaiman advised on study design and data interpretation. The author has read, given critical feedback and approved the final manuscript.
Imran Mahalil facilitated the data collection process. The author has read, given critical feedback and approved the final manuscript.
Ethical Approval
Ethical approval of this study was granted by the Kulliyyah Postgraduate and Research Committee (IIUM/305/20/4/1/7) and IIUM Research Ethics Committee (IREC) (IIUM/504/14/11/2/IREC2022-194). All participants involved in the study had given their written consent, and their participation was voluntary.
Data Availability
The data of this study data are available at a Figshare repository, https://doi.org/10.6084/m9.figshare.26711965
Acknowledgement
The authors would like to thank the Department of Informatics, College of Computing & Informatics, Universiti Tenaga Nasional, Selangor, Malaysia, for providing equipment, software and logistics support.
Funding
This study did not receive any funding or financial support.
Declaration of Interest
The authors declare that there are no conflicts of interest regarding the publication of this paper.
References
Bartlett, K. A., & Camba, J. D. (2023). Gender differences in spatial ability: A critical review. Educational Psychology Review, 35(1), Article 8. https://doi.org/10.1007/s10648-023-09728-2
Deisinger, J., Cruz-Neira, C., Riedel, O., & Symanzik, J. (1997). The effect of different viewing devices for the sense of presence of immersion in virtual environments: A comparison of stereoprojections based on monitors, HMDs and screens. Proceedings of the Seventh International Conference on Human-Interaction Computer, (2), 881-884. https://www.usu.edu/math/symanzik/papers/1997_HCI_Int.html
Kurul, R., Ögün, M. N., Narin, A. N., Avci, Ş., & Yazgan, B. (2020). An alternative method for anatomy training: Immersive virtual reality. Anatomical Sciences Education, 13(5), 648-656. https://doi.org/10.1002/ase.1959
Stanney, K., Fidopiastis, C., & Foster, L. (2020). Virtual reality is sexist: But it does not have to be. Frontiers in Robotics and AI, 7, 476417 https://doi.org/10.3389/frobt.2020.00004
Yamazaki, A., Ito, T., Sugimoto, M., Yoshida, S., Honda, K., Kawashima, Y., Fujikawa, T., Fujii, Y., & Tsutsumi, T. (2021). Patient-specific virtual and mixed reality for immersive, experiential anatomy education and for surgical planning in temporal bone surgery. Auris Nasus Larynx, 48(6), 1081-1091. https://doi.org/10.1016/j.anl.2021.03.009
*Azmi Mohd. Yusof
Jalan IKRAM-UNITEN,
43000 Kajang,
Selangor, Malaysia
Email: azmiy@uniten.edu.my
Announcements
- Best Reviewer Awards 2025
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2025.
Refer here for the list of recipients. - Most Accessed Article 2025
The Most Accessed Article of 2025 goes to Analyses of self-care agency and mindset: A pilot study on Malaysian undergraduate medical students.
Congratulations, Dr Reshma Mohamed Ansari and co-authors! - Best Article Award 2025
The Best Article Award of 2025 goes to From disparity to inclusivity: Narrative review of strategies in medical education to bridge gender inequality.
Congratulations, Dr Han Ting Jillian Yeo and co-authors! - Best Reviewer Awards 2024
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2024.
Refer here for the list of recipients. - Most Accessed Article 2024
The Most Accessed Article of 2024 goes to Persons with Disabilities (PWD) as patient educators: Effects on medical student attitudes.
Congratulations, Dr Vivien Lee and co-authors! - Best Article Award 2024
The Best Article Award of 2024 goes to Achieving Competency for Year 1 Doctors in Singapore: Comparing Night Float or Traditional Call.
Congratulations, Dr Tan Mae Yue and co-authors! - Best Reviewer Awards 2023
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2023.
Refer here for the list of recipients. - Most Accessed Article 2023
The Most Accessed Article of 2023 goes to Small, sustainable, steps to success as a scholar in Health Professions Education – Micro (macro and meta) matters.
Congratulations, A/Prof Goh Poh-Sun & Dr Elisabeth Schlegel! - Best Article Award 2023
The Best Article Award of 2023 goes to Increasing the value of Community-Based Education through Interprofessional Education.
Congratulations, Dr Tri Nur Kristina and co-authors! - Best Reviewer Awards 2022
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2022.
Refer here for the list of recipients. - Most Accessed Article 2022
The Most Accessed Article of 2022 goes to An urgent need to teach complexity science to health science students.
Congratulations, Dr Bhuvan KC and Dr Ravi Shankar. - Best Article Award 2022
The Best Article Award of 2022 goes to From clinician to educator: A scoping review of professional identity and the influence of impostor phenomenon.
Congratulations, Ms Freeman and co-authors.









