A safe space to engage: MedTalks, a student-led discussion group on the medical humanities
Submitted: 28 June 2022
Accepted: 16 August 2022
Published online: 3 January, TAPS 2023, 8(1), 54-56
https://doi.org/10.29060/TAPS.2023-8-1/CS2833
Ying Ying Koh* & Caitlin Alsandria O’Hara*
Yong Loo Lin School of Medicine, National University of Singapore, Singapore
*Both authors contributed equally as first authors.
I. INTRODUCTION
Increasing attention has been given to the role of medical humanities in both clinical care as well as in medical education. Medical humanities is defined as an “interdisciplinary perspective that draws on both creative and intellectual methodological aspects of disciplines such as anthropology, art, bioethics, drama and film, history, literature, music, philosophy, psychology, and sociology” (Hoang et al., 2022).
While 80% of health outcomes are related to the social determinants of health (Magnan, 2017), traditional medical education has largely focused on clinical knowledge and skills. Only in recent years have medical schools recognised the importance of medical humanities (Smydra et al., 2021). The strength of medical humanities is the ability to foster a more humanistic clinical practice and build professional social accountability (Pfeiffer et al., 2016).
In Singapore, the Office of Medical Humanities was set up in the SingHealth Duke-NUS Academic Medical Centre to encourage the growth of the medical humanities in the local medical field (Ong & Anantham, 2019). This highlights the growing interest in medical humanities in Singapore.
This paper aims to highlight an innovative approach for medical humanities education through student-led discussion groups, called ‘MedTalks’, conducted in the Yong Loo Lin School of Medicine, Singapore.
II. A GROUND-UP APPROACH TO THE MEDICAL HUMANITIES
MedTalks was started as a student-led platform for medical students to gain exposure to the medical humanities social issues relating to healthcare. Through Socratic seminar-style discussion among students across all three medical schools in Singapore, MedTalks provides a safe space to learn from each others’ thoughts, and crystallise their own ideas and values. In the long term, MedTalks hopes to empower students to take actionable steps towards addressing the social determinants of health in their future clinical practice.
The initiative was inspired by a yearlong liberal arts non-degree programme in a liberal arts university in the United States which the two student-founders of MedTalks had experienced. This yearlong exposure to the liberal arts–particularly medical anthropology, medical history and political science–also informed the approach and development of the content of sessions. For specific sessions, experts or persons with lived experience were invited to be guest co-facilitators. While the liberal arts exposure provided a foundation, the facilitators themselves have made clear during sessions that they are not subject matter experts, but students who are learning from fellow students through discussion.
III. FORMAT OF SESSIONS
MedTalks runs as a series of discussion sessions, which have three key features. Firstly, they are centred around a theme with accompanying pre-session reading materials for participants. These materials consist of excerpts from book abstracts, journal articles, and multimedia sources (e.g speeches, news sites or videos); these act as a primer on the topic and promote questions or ideas which can be raised in the discussions. Preliminary discussion questions are provided for students to ponder and reflect on prior to the session. Secondly, sessions are facilitated by the student-organisers of the programme. These student-organisers also curate the session themes and pre-reading materials prior to the session. Curation of session themes and materials is done based on themes encountered during clinical rotations, national current affairs, and suggestions from student-participants. Thirdly, participants are not required to speak up during the session; they can choose to simply sit in for the discussion. The fact that sessions are student-led and verbal participation is non-obligatory facilitates a more comfortable environment for students in the discussion and allows them to participate in a way that suits their learning.
MedTalks discussions are varied in scope, with several broad subtypes as follows in Table 1:
|
Introductory discussions These provide a first step towards exploring a discipline in the medical humanities. |
Examples of previous introductory discussions include: – An Introduction to Medical History – An Introduction to Medical Anthropology |
|
Sessions which address key ideas, concepts, and theories These explore a concept in greater detail, sometimes through case studies. |
Examples of previous sessions themed around a key concept include: – Social Determinants of Health – Stigma and Health – Intersectionality and Medicine |
|
Sessions which focus on a specific group of patients These dive deeper into a subgroup of patients or an area of health and wellbeing. Guest participants from the patient group are invited to provide their perspective on their lived experience. |
Examples of previous sessions such as these include: – Disability and Medicine – The History of Psychiatry in Singapore |
|
Sessions about the nature of medical practice These explore cultures, norms, and values within medical practice. |
Examples of previous sessions include: – Empathy in Medicine – The Culture of the Medical Profession |
Table 1. Types and formats of MedTalks discussion sessions
IV. A SAFE SPACE TO ENGAGE: OUTCOMES
Since its inception in May 2020, MedTalks has organised 25 peer-to-peer discussion groups, addressing topics which have not been routinely included in the medical school syllabus. Each discussion session is attended by 5 to 15 medical students. Feedback indicated that MedTalks provides an approachable platform for them to engage with topics that they might be new to and which may seem daunting at first, aided by the student-led nature of the sessions and the lack of pressure to verbally participate. Feedback also included that the takeaways from discussions help to shape the way participants understand the patients they encounter in the hospital–to view them in a more holistic manner beyond their presenting medical complaints, and to consider systemic factors that shape their health and wellbeing. In addition, feedback from the programme also demonstrated that participants’ experience with MedTalks contributed to them starting up new community projects to address barriers to healthcare for marginalised groups.
V. TAKEAWAYS AND THE ROAD AHEAD
MedTalks serves as an example of how the medical humanities can be made accessible to medical students, by medical students themselves. MedTalks’ model can be well-replicated by other interested student bodies, to create a culture of discussion and spark interest in the medical humanities among the medical student community. Potential also exists for discussion sessions to be combined with students from other disciplines, such as allied health, the social sciences, or public health, to bring interdisciplinary and interprofessional perspectives to the table and enrich the discussions shared.
Notes on Contributors
Ms Koh Ying Ying is a founding member of the student initiative, MedTalks. She conceptualised this manuscript, and drafted the first and last sections of the manuscript. She read and approved of the final version of the manuscript.
Ms Caitlin O’Hara is a founding member of the student initiative, MedTalks. She conceptualised this manuscript, and drafted the middle sections of the manuscript. She read and approved of the final version of the manuscript.
Acknowledgement
The authors would like to sincerely thank their mentors for caringly supporting MedTalks as a student-led initiative.
Funding
There are no funding sources to declare for this paper.
Declaration of Interest
The authors have no conflict of interest to declare.
References
Hoang, B. L., Monrouxe, L. V., Chen, K.-S., Chang, S.-C., Chiavaroli, N., Mauludina, Y. S., & Huang, C.-D. (2022). Medical humanities education and its influence on students’ outcomes in Taiwan: A systematic review. Frontiers in Medicine, 9, Article 857488. https://doi.org/10.3389/fmed.2022.857488
Magnan, S. (2017). Social determinants of health 101 for health care: Five plus five. NAM Perspectives, 7(10). https://doi.org/10.31478/201710c
Ong, E. K., & Anantham, D. (2019). The medical humanities: Reconnecting with the soul of medicine. Annals of the Academy of Medicine, Singapore, 48(7), 233–237. Retrieved from https://annals.edu.sg/the-medical-humanities-reconnecting-with-the-soul-of-medicine/
Pfeiffer, S., Chen, Y., & Tsai, D. (2016). Progress integrating medical humanities into medical education: A global overview. Current Opinion in Psychiatry, 29(5), 298–301. https://doi.org/10.1097/YCO.0000000000000265
Smydra, R., May, M., Taranikanti, V., & Mi, M. (2021). Integration of arts and humanities in medical education: A narrative review. Journal of Cancer Education. https://doi.org/10.1007/s13187-021-02058-3
*Ying Ying Koh
10 Medical Dr,
Singapore 117597
Email: kohyingying@u.nus.edu
Submitted: 12 April 2022
Accepted: 19 August 2022
Published online: 3 January, TAPS 2023, 8(1), 57-60
https://doi.org/10.29060/TAPS.2023-8-1/CS2791
Caitlin Hsuen Ng, Siaw May Leong, Arumugam Rajesh Kannan & Deborah Khoo
Department of Anaesthesia, National University Hospital (NUH), Singapore
I. INTRODUCTION
Airway management is critical for any anaesthetist. The Coronavirus Disease 2019 (COVID-19) pandemic has brought such skills to the forefront over the last three years. Yet, the outbreak has also disrupted traditional methods of airway skills training and limited the chances of in-person workshops and conferences due to social distancing requirements and demanding manpower needs. To lower the incidence of airway-related morbidity (Joffe et al., 2019), regular and effective instructional methods are needed to maintain airway providers’ skills.
Our Department of Anaesthesia at the National University Hospital (NUH) of Singapore shares our experience conducting small-group refresher sessions, and how that has changed during a pandemic.
II. ASSESSMENT OF CURRENT LEARNING PROGRAMME AND TRAINING NEEDS
Since 2013, our department has been conducting quarter-yearly intra-departmental mini-workshops for airway training. This was to address the airway component of our patient safety strategy, and the unmet need to maintain and upskill airway management techniques for as many anaesthesia providers as possible, who come with an uneven range of seniority and experience with difficult airways. We were challenged to achieve this goal, yet without overly impacting manpower and daily operations. Each session was led by in-house faculty and was open to anaesthesia providers of every level. On occasion, external faculty were invited if they had specific expertise in certain aspects. The syllabus aligned with Difficult Airway Guidelines (Rosenblatt & Yanez, 2022) and was done in a sequential, repeating manner.
III. INTERVENTION: REFRESHER WORKSHOPS IN THE PANDEMIC
As the COVID pandemic came to Singapore around early 2020, our department training was disrupted in many ways. Nationwide social-distancing measures meant that in-person teachings and elective operations were suspended. The increased patient load from the pandemic also meant more manpower redeployed to the frontlines and Intensive Care Units, with an increased focus on infection control and personal protection. In the event airway intervention was required for a patient, the procedure carried significant risks from the aerosol-generating procedures of intubation and mechanical ventilation to both staff and patients. As a result, clinical exposure for airway providers-in-training was severely hampered.
Hence, alterations were made to our existing regular airway training regime. The didactic segment was smoothly transitioned to the videoconferencing platform, Zoom. This had the added benefit of widening the audience to providers who would otherwise have not been able to physically attend. We continued with the hands-on component of the session, but limited participants in the room at any one time in accordance with the room size, ensuring at least one meter between personnel. Strict personal protection was adhered to, requiring all participants to wear N95 masks and perform hand hygiene before and after each station. Participants also assisted in maintaining the cleanliness of the equipment by using Isopropyl Alcohol 70% wipes to decontaminate all surfaces after use. Given the restricted participant size, a call-back system was used when participants had to be turned away. Attendance was tracked using a manual sign-in system. There were no incidences of transmission of COVID-19 because of these workshops.
We focused on airway management while wearing Personal Protective Equipment to better simulate clinical scenarios, bearing in mind the extra physical and cognitive load that airway providers bear in such circumstances (Foong et al., 2020). Specific skills such as how to safely transfer an intubated patient from one ventilator to another were also practiced and video laryngoscope intubation with a limited field of vision. Figure 1 outlines the suggested format, syllabus, and rationale of our mini-workshops, with the intent that it can be modified as needed and replicated in institution-specific settings.
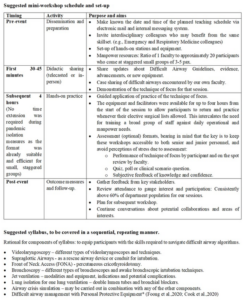
Figure 1. Suggested template and syllabus of in-house refresher workshops
*added from 2020 onwards
IV. EVALUATION OF INTERVENTION DURING THE PANDEMIC
After almost 10 years, we review our airway training refresher sessions, including its adaptation to the COVID pandemic.
Firstly, the sessions were logistically manageable, using pre-existing equipment and a realistic number of faculty. The intimate number of participants not only complied with safe distancing measures but also encouraged more detailed guidance and supervision of practical skills tailored to the participant’s skill level. Flexibility in attendance allowed for continued participation without significantly affecting manpower during the ongoing pandemic.
Simulation-based mini-workshops allowed for continued honing of skills when authentic clinical scenarios were limited. While simulation is unable to replace the actual experience, it has a positive impact on healthcare systems and their patients during times of a pandemic (Santos et al., 2021). The equipment and techniques covered kept abreast of the latest developments and content was curated to help cope with the pandemic by facilitating familiarity and identification of otherwise unexpected problems in managing a COVID airway, prior to real-life encounters and emergent patient care situations. These measures ensure that such high-risk airways are handled in a safe, accurate, and swift manner, maximising first-pass success, and minimising risks to patients and airway providers in the actual situations (Cook et al., 2020).
The workshops were also able to touch on the softer skills required in airway management. The sessions catered to a mix of staff to build teamwork and coordination in a multidisciplinary airway crisis team. Having a shared plan and proper forms of communication are critical in crisis airway situations, even more so with the additional barrier of PPE. Our in-house training has received positive feedback in increasing staff confidence and preparedness for facing airway crises during times of the pandemic.
V. CONCLUSION
As with any skill, practice is essential. During these times of a public health crisis, we need to be adaptable in our instructional methods of continuing training. We believe that our hands-on refresher sessions have been beneficial in enhancing the accessibility of airway management practice even during a pandemic and suggest a syllabus and method that can be replicated and modified to suit the needs and resources of various settings.
Notes on Contributors
Caitlin Ng took lead in drafting and revising of the manuscript, along with aiding in data collection and analysis.
Leong Siaw May contributed to the conceptualisation of the study and revision of the manuscript and was faculty at some of these workshops.
Arumugam Rajesh Kannan contributed to the conceptualisation of the study and revision of the manuscript and was faculty at some of these workshops.
Deborah Khoo conceptualised of study, led the data collection, was faculty at some of these workshops, and contributed to the revision of the manuscript.
Acknowledgement
Our team would like to thank the department of Anaesthesia, NUH, for the provision of equipment, participation, and facilitation of the faculty in the workshops. We were fortunate to have the equipment and facilities at our disposal to conduct such workshops at our convenience. We understand that this privilege may not be generalisable elsewhere.
Funding
There was no funding received for this project, beyond that of the department’s resources.
Declaration of Interest
The authors report no conflict of interest.
References
Cook, T. M., El-Boghdadly, K., McGuire, B., McNarry, A. F., Patel, A., & Higgs, A. (2020). Consensus guidelines for managing the airway in patients with COVID-19: Guidelines from the Difficult Airway Society, the Association of Anaesthetists the Intensive Care Society, the Faculty of Intensive Care Medicine and the Royal College of Anaesthetists. Anaesthesia, 75(6), 785-799. https://doi.org/10.1111/anae.15054
Foong, T. W., Hui Ng, E. S., Wee Khoo, C. Y., Ashokka, B., Khoo, D., & Agrawal, R. (2020). Rapid training of healthcare staff for protected cardiopulmonary resuscitation in the COVID-19 pandemic. British Journal of Anaesthesia, 125(2), e257-e259. https://doi.org/10.1016/j.bja.2020.04.081
Joffe, A. M., Aziz, M. F., Posner, K. L., Duggan, L. V., Mincer, S. L., & Domino, K. B. (2019). Management of difficult tracheal intubation: A closed claims analysis. Anesthesiology, 131(4), 818-829. https://doi.org/10.1097/aln.0000000000002815
Rosenblatt, W. H., & Yanez, N. D. (2022). A decision tree approach to airway management pathways in the 2022 Difficult Airway Algorithm of the American Society of Anesthesiologists. Anesthesia & Analgesia, 134(5), 910-915. https://doi.org/10.1213/ane.0000000000005930
Santos, T. M., Pedrosa, R. B. S., Carvalho, D. R. S., Franco, M. H., Silva, J. L. G., Franci, D., Jorge, B., Munhoz, D., Calderan, T., Grangeia, T. A. G., & Cecilio-Fernandes, D. (2021). Implementing healthcare professionals’ training during COVID-19: A pre and post-test design for simulation training. Sao Paulo Medical Journal, 139(5), 514-519. https://doi.org/10.1590/1516-3180.2021.0190.R1.27052021
*Caitlin Ng
5 Lower Kent Ridge Road,
Singapore 119074
Email: caitlin_ng97@hotmail.com
Submitted: 27 July 2022
Accepted: 21 September 2022
Published online: 3 January, TAPS 2023, 8(1), 61-63
https://doi.org/10.29060/TAPS.2023-8-1/CS2852
Janaka Eranda1, Hewapathirana Roshan2 & Karunathilake Indika3
1Ministry of Health, Sri Lanka; 2Department of Anatomy, Genetics and Biomedical Informatics, Faculty of Medicine, University of Colombo, Sri Lanka; 3Department of Medical Education, Faculty of Medicine, University of Colombo, Sri Lanka
I. INTRODUCTION
Anatomy is considered as one of the key components of undergraduate medical education. Hence, it is important to have a sound knowledge in anatomy to proceed into clinical medicine. Didactic lectures, textbooks, prosected specimens, and cadaveric dissection are the most frequently used anatomy teaching methods. However, with the emergence of COVID-19 pandemic, conventional teaching and learning were challenged. Technology integration for medical education has been increased during COVID-19 in many countries. With the integration of new technologies to the anatomy teaching, the traditional ‘directed self-learning’ started to move towards ‘self-directed learning’. This transformation however, was not without various challenges, especially in low-resource settings such as Sri Lanka (Karunathilake et al., 2020). Augmented reality (AR), Virtual reality (VR), and principles of gamification play an important role in motivation and engagement in medical teaching and learning by enhancing interactivity (Moro et al., 2021). Such technologies also found to have positive impact on students’ spatial understanding and 3D comprehension of anatomical structures.
The objectives of this case study were to identify the context-specific factors in designing AR/VR-based anatomy instructional materials and to assess the student motivation and engagement to use gamification in their studies. The instructional systems design model ADDIE (Molenda, 2003), which is an acronym for Analyze, Design, Develop, Implement, and Evaluate, was used to develop the instructional materials in this study since it found to ensure the appropriateness of the materials used in an optimal manner to bring the maximum educational outcome.
II. METHODS
During the study, mixed-method tradition was followed in a Sri Lankan medical faculty from September 2020 to February 2021. Ethics approval was obtained from the Ethics Review Committee of the Postgraduate Institute of Medicine, University of Colombo where the study was exempted from the review process. Purposive sampling was the method adhered recruiting 92 undergraduate medical students and 20 lecturers with the informed consent of the participants. The methodology was phased out according to the ADDIE model.
A. Analysis
A qualitative study was conducted using semi-structured interviews with the lecturers. The interviews were informed by the six dimensions of the Hexagonal E-Learning Assessment Model – HELAM (Ozkan & Koseler, 2009) which consists of students’ attitudes, teachers’ attitudes, technology-enhanced learning, content quality, service quality and supportive factors in designing effective E-learning materials. This phase revealed lecturers’ suggestions to develop AR/VR contents in terms of graphical user interfaces, modes of navigation, interactivity, and strategies in incorporating modes of gamification into learning materials.
B. Design
The results of the analysis phase were used to develop a blueprint of the instructional materials integrating the modes of gamification. These were instrumentalised to enhance the motivation and engagement in developed learning materials.
C. Development
An AR/VR application was developed using Unity game engine using 3D anatomy models to project 3D anatomy models over 2D reference images to be used with smart phones and generic VR boxes.
D. Evaluation
This phase consisted of a quantitative study offered to undergraduate students. The self-administered questionnaire with 40 questions of the type 5-point Likert-scale was used to assess participants’ self-reported perceptions of motivation and engagement in self-directed learning. The questionnaire assessed the gamification approach, teaching materials, user interfaces, practicability, physical discomfort, student attitudes on PC-based games, AR/VR apps. The developed apps were used by the students prior to complete the survey.
III. RESULTS
A. Qualitative Study
Lecturers expressed their interest in AR/VR technology with gamification and suggested to link the new AR/VR contents to the existing Learning Management System as the students already have a good engagement with it. They highlighted different modes of gamification such as interactive quizzes, animated interactive 3D anatomy models, teleport targets for VR navigation and video clips to enhance interactivity. Furthermore, they emphasized the importance of the quality of the content, reliability of the information technology services and course administration related factors to improve the overall quality of the learning experience and the sustainability of the new approach.
B. Quantitative Study
The results were organized along the dimensions, gamification, teaching materials, user interfaces, practicability, students’ attitudes toward the technology-enhanced learning and AR/VR apps. The gamification dimension indicated the overall acceptance for the AR/VR techniques and tools and adapting the technology-enhanced learning in formal medical curricula. The highest mean value (4.20 out of the scale ranging from 1 to 5) was observed for the use of the augmented reality app indicating that medical students participated were satisfied with the offered interactivity in the AR/VR apps. The average satisfaction score for gamification, practicability, physical discomfort, teaching materials, user interfaces, student attitudes on the technology-enhanced game and AR/VR app were above satisfactory level (score ≥ 4). The student’s satisfaction on the physical discomfort showed the lowest average score compared to the rest of the dimensions. Further to this, the students had lesser variation in the satisfaction score about the dimension attitudes on the technology-enhanced learning (SD 0.41) compared to the other dimensions. The questionnaire included six questions to measure the level of motivation and engagement. On average, 88% of the students have expressed their willingness to engage with the AR/VR learning style and confirmed that the technology-enhanced learning is a beneficial learning style.
IV. DISCUSSION
The study was conducted to identify the measures to improve motivation and engagement in learning anatomy when integrating technology-enhanced interactive learning contents into the undergraduate medical curriculum. The importance of having a systematic approach is necessary when designing instructional content to obtain a better outcome. The use of principles of gamification improved motivation and engagement which is in line with previous studies (Moro et al., 2022). Sustainability of the technology-enhanced learning was a key concern among the lecturers.
V. CONCLUSION
This research attempted to identify the student motivation and engagement towards the gamified anatomy learning with AR/VR technology. The study provided the insight into context-specific factors in designing interactive learning contents and methods. The ability to deliver an immersive experience in AR/VR methods helps the student to study anatomy in self-directed learning even in situations, such as COVID-19 pandemic and mandatory social distancing, which demands strict remote teaching.
Notes on Contributors
Dr G.K.M.E. Janaka, MBBS, MSc, MD was involved in reviewing the literature, formulating the methodological framework, designed the gamified AR and VR learning tools and and writing the original draft.
Dr Roshan Hewapathirana, MBBS, MSc, PhD, MIEE was involved in the study by developing the methodological framework, data curation, formal analysis, and editing the original draft.
Professor Karunathailke Indika, MBBS(Col), CTHE (Col), DMedEd (Dundee), MMedEd (Dundee), FHEA (UK), FCGP( SL), FRCP (Edin.), FCME (SL) was involved in the study by conceptualizing the idea, developing the methodological framework, creviewing the manuscript and supervising the overall study.
Acknowledgement
The authors would like to acknowledge the Head of the Department and the lecturers of the Department of Anatomy, Genetics and Biomedical Informatics, Faculty of Medicine, University of Colombo who supported giving valuable comments and all the students who had volunteered in participating in the study.
Funding
There are no funding sources to declare.
Declaration of Interest
The authors declare that they have no competing interests.
References
Karunathilake, I. M., Dissanayake, V. H. W., Yasawardena, S., Abegunawardena, A., Raviraj, S., Wijesinghe, P. S., Anthony, A. A., Wijesinghe, R. A. N. K., Bowatte, S., Wickramaratne, N., Pathirana, K. D., Pilapitiya, S., Edirisinghe, S., Hettiarachchi, D., Kohombange, C., & Olipeliyawa, A. (2020). The new normal of medical education – Challenges and opportunities. South-East Asian Journal of Medical Education, 14(1), 2. https://doi.org/10.4038/seajme.v14i1.241
Molenda, M. (2003). In Search of the Elusive ADDIE Model. Performance Improvement, 42(5), 34–37.
Moro, C., Birt, J., Stromberga, Z., Phelps, C., Clark, J., Glasziou, P., & Scott, A. M. (2021). Virtual and augmented reality enhancements to medical and science student physiology and anatomy test performance: A systematic review and meta analysis. Anatomical Sciences Education, 14(3), 368–376. https://doi.org/10.1002/ase.2049
Moro, C., Phelps, C., & Birt, J. (2022). Improving serious games by crowdsourcing feedback from the STEAM online gaming community. The Internet and Higher Education, 55, Article 100874. https://doi.org/10.1016/j.iheduc.2022.100874
Ozkan, S., & Koseler, R. (2009). Multi-dimensional students’ evaluation of e-learning systems in the higher education context: An empirical investigation. Computers & Education, 53(4), 1285–1296. https://doi.org/10.1016/j.compedu.2009.06.011
*Janaka Eranda
Ministry of Health,
Sri Lanka
+94714747309
Email: erandajanaka1979@gmail.com
Submitted: 24 May 2022
Accepted: 16 August 2022
Published online: 3 January, TAPS 2023, 8(1), 51-53
https://doi.org/10.29060/TAPS.2023-8-1/CS2818
Teresa Diana B. Bongala
Department of Obstetrics and Gynaecology, Faculty of the College of Medicine, University of the East Ramon Magsaysay Memorial Medical Centre, Philippines
I. INTRODUCTION
The world will never be the same after the COVID-19 pandemic. Education has had to evolve. Evaluation of cognitive skills is still achieved by written examinations administered through learning management systems. However, an integral part of evaluation, the Objective Structured Clinical Examination (OSCE), which assesses the students’ ability to obtain, communicate information, perform physical examination, diagnose, and solve problems, could not be given due to COVID-19 restrictions.
Simulation during teaching and assessments like the OSCE have been done worldwide, (Nguyen et al., 2015) and have been utilised in our university for more than twenty years. Because of lockdowns due to Covid-19, the OSCE was given online in medical schools worldwide, however the number of students were limited (Boyle et al., 2020; Lara et al., 2020). In the Philippines, by December 2020, immunisation against Covid-19 had not started, and travel was still restrictive, hence face-to-face classes were still limited. (Department of Education, 2020). Hence, the Department of Obstetrics and Gynaecology of our university planned and conducted the first large-scale summative virtual OSCE (VOSCE) for Level III medical students.
II. METHODS
The summative VOSCE was conducted using a Zoom licensed Education account, with features called “Breakout Rooms” and “Screen Share” and the Canvas learning management system. There were 17 faculty, 10 residents, 15 post-graduate interns, 10 Level IV and 440 Level III students who participated. The Level III students had synchronous and asynchronous lectures for four-and-a-half months in Obstetrics, and nine weeks of small group discussions (SGD).
The table of specifications was based on the learning outcomes in Obstetrics and skills taught during SGDs. Six sets of examinations with four stations, were prepared. The first two stations were given in Canvas, while the last two “performance” stations, namely history taking, and Physical Examination (PE) were given over Zoom. The evaluation in OSCE was modified to fit tasks for VOSCE. It underwent an MPL setting by three members of the faculty using the Angoff method. (Livingston & Zieky, 1982)
All participants underwent orientation. The students were informed of the materials they needed: a computer, for Canvas and for zoom in stations 3 and 4; a mobile device, for proctoring, communication and to demonstrate performance /PE in Station 4; and other materials needed for Station 4. The faculty were instructed to Screen Share tasks via Zoom in the “performance” stations and oriented on student evaluation and result submission.
Three days before the VOSCE, a simulation involving clinical clerks, post-graduate interns and residents was conducted. Clarity of video, audio and internet speed were checked. Timing and transfer of examinees between breakout rooms was also rehearsed. The tasks for Stations 3 and 4, and evaluation forms, were sent to the faculty the 12 hours before the VOSCE.
Thirty minutes before the VOSCE, the students underwent identity verification, their gadgets and positions checked. Concurrently, the post-graduate interns, who acted as patients, were given the script.
The examinees, in stations 1 and 2, givenclinical vignette and images of speculum examination, had to diagnose and write a prescription. After Canvas stations, in another breakout room, the students were informed of materials needed for Station 4. In Station 3, they elicited the history from a simulated patient, and in Station 4, they performed PE with annotation.
Communication with students was through Telegram and Zoom, while Viber was used between faculty and residents.
III. RESULTS
Four hundred and forty students took part in the VOSCE. Post-VOSCE survey with 397 respondents showed that 382 (96.2%) students took it in the Philippines, and 15 (0.38%) students were out of the country.
Forty-three (10.8%) had internet speed <10mbps. Thirty (9.0%) had connection problems/unable to view images in stations 1 and/or 2. Thirty students were given another examination, three hours post-VOSCE. Table 1 shows the location and the internet connection of the students, their perception of the VOSCE and the problems they encountered during the examination.
|
Questions |
Number (%) |
|
Location during VOSCE |
|
|
Philippines (except Manila) MetroManila Outside of Philippines |
230 (57.93 %) 152 (38.28%) 15 (3.87%) |
|
Internet speed (mbps) |
|
|
< 10 10-100 > 100 |
43 (10.8%) 328 (82.61%) 26 (6.5%) |
|
Orientation |
|
|
Adequate Inadequate Absent |
336 (84.63%) 47 (11.84%) 14 (3.52%) |
|
SGDs helpful |
|
|
Strongly agree/Agree Neutral Disagree/strongly disagree |
319 (80.3%) 58 (14.6 %) 20 (5.03%) |
|
Canvas rubrics helpful |
|
|
Strongly agree/ Agree Neutral Disagree /Strongly disagree |
335 (84.38%) 49 (12.3 %) 13 (3.3%) |
|
VOSCE problems |
|
|
None Temporary disconnection Disconnection Stations 1/or2 Internet lag Poor audio |
265 (66.75%) 63 (15.86%) 30 (9.00%) 24 (6.04%) 15 (3.77%) |
|
Tension prevented me from performing well |
|
|
Strongly agree/Agree Neutral Disagree/Strongly disagree |
229 (57.68%) 101 (25.4 %) 67 (16.87%) |
|
Internet/gadget prevented me from performing well |
|
|
Strongly agree/Agree Neutral Disagree/Strongly disagree |
129 (32.49%) 94 (23.7 %) 174 (43.83%) |
Table 1. Post-VOSCE Survey n= 397
IV. DISCUSSION
Participants orientation and the simulation were important in ensuring the success of this VOSCE. The students perceived that SGDs 319 (80.3 %), Canvas rubrics 335 (84.4%), and orientation 336 (84.63%), helped in their preparation. However, the students viewed that tension 129 (32.49%) and internet and gadget issues 229 (57.68 %) prevented them from performing well.
Passing rates were comparable, with OSCE 75.68 % and VOSCE 78.9 %. Moreover, the mean score of the VOSCE 81, was only slightly lower than OSCE mean, 82.07.
With ease of restrictions the following year, we continued using VOSCE because we obtained similar results to OSCE, it was less costly and easier to manage. Post-pandemic it will remain an important tool for formative and summative assessments. Among its advantages, there are examiners/faculty available for the VOSCE because it is online. Furthermore, it can be modified to administer some stations online, while conducting the PE stations onsite.
V. CONCLUSION
We have demonstrated that the VOSCE may be given successfully and will continue to play an important role in assessment post-pandemic. It is more convenient and economical to administer. Its main disadvantages include the possibility of internet disruption and gadget malfunction. However, with planning, innovation, orientation, and communication, it may be administered without major problems. It is reassuring that whatever restrictions we may face in the future, the VOSCE, will ensure we can continue to produce competent doctors, who will be part of the solution to the healthcare problems of the world.
Notes on Contributors
The author did the literature review, conceptualised and oversaw the implementation of the VOSCE, created the post exam survey, retrieved previous grades pre-pandemic, analysed the data and wrote the manuscript.
Acknowledgement
The author would like to acknowledge the administration and the faculty of the Department of Obstetrics and Gynaecology of the University of the East Ramon Magsaysay Memorial Medical Centre, for their trust and support in the planning and conduction of the VOSCE. Special thanks to the residents who helped to orient the participants, monitored, and helped in running Canvas and Zoom. The author would also like to extend her gratitude to the clinical clerks and the postgraduate interns, who have given their time during the technical dry run and for serving as standardised patients during the conduct of the VOSCE.
Funding
The author did not receive any funding for this study.
Declaration of Interest
The author does not have any conflict of interest.
References
Boyle, J. G., Colquhoun, I., Noonan, Z., McDowall, S., Walters, M. R., & Leach, J. P. (2020). Viva la VOSCE? BMC Medical Education, 20(1). Article 514. https://doi.org/10.1186/s12909-020-02444-3
Department of Education. (2020, December). Official statement on the pilot implementation of limited face-to-face classes. Retrieved July 20, 2021, from https://www.deped.gov.ph/2020/12/15/official-statement-on-the-pilot-implementation-of-limited-face-to-face-classes/
Lara, S., Foster, C. W., Hawks, M., & Montgomery, M. (2020). Remote assessment of clinical skills during COVID-19: A virtual, high-stakes, summative pediatric objective structured clinical examination. Academic Pediatrics, 20(6), 760-761. https://doi.org/10.1016/j.acap.2020.05.029
Livingston, S. A., & Zieky, M. J. (1982). Passing scores: A manual for setting standards of performance on educational and occupational tests. Educational Testing Service.
Nguyen, L., Tardioli, K., Roberts, M., & Watterson, J. (2015). Development and incorporation of hybrid simulation OSCE into in-training examinations to assess multiple CanMEDS competencies in urologic trainees. Canadian Urological Association Journal, 9(1-2), 32. https://doi.org/10.5489/cuaj.2366
*Teresa Diana B. Bongala
64 Aurora Boulevard,
Quezon City, Metro Manila,
Philippines
+639175776420
Email: tbbongala@uerm.edu.ph
Submitted: 22 February 2022
Accepted: 3 August 2022
Published online: 3 January, TAPS 2023, 8(1), 47-50
https://doi.org/10.29060/TAPS.2023-8-1/SC2764
Kye Mon Min Swe1 & Amit Bhardwaj2
1Department of Population Medicine, University Tunku Abdul Rahman, Malaysia; 2Department of Orthopaedics, Sengkang General Hospital, Singapore
Abstract
Introduction: During the era of COVID-19 pandemic, online learning has become more prevalent as it was the most available option for higher education training which has been a challenging experience for the students and the lecturers especially in the medical and health sciences training. The study was conducted to determine the perceptions of clinical year medical students on online learning environments during the COVID-19 pandemic.
Methods: A cross sectional study was conducted to clinical year medical students at University Tunku Abdul Rahman. The validated Online Learning Environment Survey (OLES) was used as a tool to conduct the study.
Results: Total 84 clinical year students participated in the study. Among four domains of OLES questionnaire, the domain; “Support of online learning” had the highest mean perception scores, 4.15 (0.55), followed by “Usability of online learning tools” 3.89 (0.82), and “Quality of Learning; 3.80 (0.68) and the domain “Enjoyment” was the lowest mean perception scores 3.48 (1.08). Most of the students (52.4%) rated the overall satisfaction of online teaching experiences “Very good” while (13.1) % rated “Excellent”.
Conclusion: In conclusion, the perceptions of clinical year medical students on online learning environments during the COVID-19 pandemic were satisfactory although there were challenging online learning experiences during the pandemic. It was recommended to include qualitative method in future studies to provide more useful in-depth information regarding online learning environment.
Keywords: Online Learning Environment, Perceptions, Medical Students, Malaysia, COVID-19
I. INTRODUCTION
Online learning is defined as learning via web-based technology and students interact with their peers and educators through web-based communication tools (Bonk & Reynolds, 1997). The usability of the web-based learning system is important as are its applications such as interactive video, forums, chat rooms, email, and document sharing systems (Klein et al., 2006).
Online learning is regarded nowadays as a new way of interaction in the educational process and online learning facilities offer various opportunities to get new knowledge and develop students’ skills through engagement and interaction in new learning environments. (Samoylenko et al., 2022)
Due to the novel coronavirus pandemic, all the higher education training has converted to online teaching and assessments including medical programs. To fulfil the student physical learning time requirement, the academic year of MBBS clinical year programmes (Year 3 to Year 5) has been divided into Phase 1; purely online teaching as medical students were not allowed to be posted to hospitals followed by Phase 2; face to face physical clinical training at the hospital. Phase 1 teaching for clinical years include, online task-based learning, online lectures and online case-based discussion, online clinical skill, and procedures. This research study was conducted to evaluate the online learning environment of clinical year students and to find out differences in students’ perceptions between the academic years.
II. METHODS
A cross sectional study was conducted to (total=135) Year 3 to Year 5 clinical year medical students. 43 students were in Year 3, 49 students were in Year 4 and 43 students were in Year 5 at University Tunku Abdul Rahman (UTAR), Selangor, Malaysia. All the clinical year students were invited to participate in the study by sending electronic invitations emails, informed consent was taken. Data was collected via google form and the information was anonymised.
A validated Online Learning Environment Survey (OLES) (Pearson & Trinidad, 2005) was used to evaluate the online learning environment of medical students of UTAR during Phase 1 of purely online teaching. The questionnaire consists of two sessions. Section (I) general demographic information, Section (II) contains 50 items of OLES questionnaires developed by Pearson and Trinidad (2005). The validity of the tool was recorded as Cronbach’s Alpha Coefficient value of 0.79 to 0.90. The OLES consists of nine scales: Computer Usage (CU); Teacher Support (TS); Student Interaction & Collaboration (SIC); Personal Relevance (PR); Authentic Learning (AL); Student Autonomy (SA); Equity (EQ); Enjoyment (EN); and A-synchronicity (AS) which can further classified into four domains: (1) Support for learning; (2) Quality of learning; (3) Usability of online learning tools; and (4) Enjoyment. Responses were recorded against a five-point scale with the following representations: 1- Never; 2- Seldom; 3- Sometimes; 4- Often; and 5- Almost Always. (Pearson & Trinidad, 2005)
Data were analysed by using SPSS (Statistical Package for Social Science) for Windows, version 26.0. The categorical variables were described by frequency and percentage. Student t-test and Analysis of variance (Anova) test was used to compare means between the groups of different academic years. Ethical approval was acquired from the Scientific Ethical Review Committee of the UTAR.
III. RESULTS
A total of 84 clinical year medical students participated from Year 3 to Year 5. There were 27 out of 43 Year 3 students (62.79%), 26 out of 49 Year 4 students (53.06%), 31 out of 43 Year 5 students (72.09%) who completed the questionnaire. Approximately 82 (97.6%) students were aged between 21 to 25 years and (63.1%) were female students.
The online learning environment survey (OLES) tool consists of four domains to evaluate student online learning environments such as “Support of Online learning”, “Usability of online learning tools”, “Quality of Learning” and “Enjoyment”. Among four domains of OLES tool, the domain; “Support of online learning” had the highest mean perception scores 4.15 (0.55), followed by “Usability of online learning tools” 3.89 (0.82), and “Quality of Learning; 3.80 (0.68) and the domain “Enjoyment” was the lowest mean perception scores 3.48 (1.08).
|
Domains of perceptions of online learning environment |
Subscales of perceptions of online learning environment |
Mean (SD) |
Mean (SD) |
|
Support for learning |
Computer Usage |
4.24 (0.64) |
4.15 (0.55) |
|
Teacher Support |
4.09 (0.78) |
||
|
Student Interaction and Collaboration |
4.02 (0.78) |
||
|
Equity |
4.25 (0.82) |
||
|
Quality of learning |
Personal Relevance |
3.60 (0.87) |
3.80 (0.68) |
|
Authentic Learning |
3.66 (0.82) |
||
|
Student Autonomy |
4.16 (0.76) |
||
|
Usability of online learning tools |
A-synchronicity |
3.89 (0.81) |
3.89 (0.82) |
|
Enjoyment |
Enjoyment |
3.48 (1.08) |
3.48 (1.08) |
Table 1: The mean perception scores of domains and subscales of online learning environment
Regarding the relation between academic year and student perception on different domains of the online environment, Year 5 students 3.89 (1.01) enjoyed the online learning as compared to Year 3 3.25(0.95) and Year 4 students 3.22 (1.18) respectively and the difference was statistically significant (P<0.027). Year 4 students perceived more positive on domains support of learning (P=0.658) and quality of learning (P=.396) and Year 5 students perceived online learning tools were useful (P=0.681).
The students were asked to rate their online learning experience via 5 points scale, poor to excellent and (52.4%) of the students found online learning experiences very good followed by (29.4%) good and (13.4%) rated excellent. The data for this research can be accessed at http://doi.org/10.6084/m9.figshare.19322297
IV. DISCUSSION
During COVID-19 pandemic era, medical clinical teaching via online was a challenging experience for both clinical lecturers and clinical year students and this study was to determine the perceptions of clinical year medical students on online learning environments during the COVID-19 pandemic.
A. Evaluating Online Learning Environment
In the literature, there were quite several tools which have been developed to specifically evaluate online learning environments such as Constructivist On-Line Learning Environment Survey (COLLES), Web-Based Learning Environment Inventory (WEBLEI), Technology-Rich Outcomes-Focused Learning Environment Inventory (TROFLEI), and Online Learning Environment Survey (OLES). The OLES instruments have been used to evaluate the university’s online learning environment and found to be a useful tool to evaluate online learning environments as the questionnaires were applicable to our local setting of online teaching. The OLES tool consists of four domains to evaluate student online learning environments such as Support of Online learning, Usability of online learning tools, Quality of Learning and Enjoyment. (Chew, 2015) The scores on scales which received specific attention for online educators to monitor the online learning environment provided for students.
1) Support of online learning: This domain includes four sub scales and it is the most important part for the students to be able to cope with the online learning environment. Regarding support for computer usage, the findings indicate the students received good support from the university regarding online learning such as the providing internet package for students, laptops, online learning tools and platforms such as Microsoft team. The support from lecturers and peers were also important in regarding clinical case discussion and group works. But in some cases, the students need to go and use internet at their relative’s house. On the “Lecturer Support Scale” and “Equity scale”, that the students got support and equivalent chances to contribute in class discussion. (Chew, 2015)
2) Usability of online learning tools: This domain includes asynchronicity subscale. Asynchronicity allows students to learn on their own schedule, within a certain timeframe. In this study, there were high mean scores for the “Asynchronicity” scale which indicates that the students found it easier to communicate online. But the result was contrary to a study by Chew (2015), found out that the students found it challenging to communicate online depends on the availability of internet and usage of social media.
3) Quality of learning: This domain includes three subscales: Personal Relevance, Student Autonomy, and Authenticity learning. The findings indicate that the students were able to manage and play significant roles in their learning in the online learning climates.
4) Enjoyment: The Enjoyment scale was used to evaluate the extent of enjoyment of learning in an online learning environment. Among all four domains, the enjoyment was the least mean perception score which indicated that although the students received support from university and lecturers, they enjoyed less with the online classes as the classes were entirely online. The result was similar to a study by Chew (2015), stated that the students had limited enjoyment in online learning environments due to lack of motivation and technical problems.
B. Limitations of the study
The study was conducted in a private medical university and quantitative approach. A mixed methods approach with larger sample was recommended for future investigations. Validation of the survey recommends carrying out for local setting.
C. Implication of the study
The present study evaluates the online learning environment experienced by clinical year medical students which found to be useful by giving them different learning opportunities and this can be used to implicate future clinical teaching as hybrid mode to create an effective and safe learning environment. The information from this study about the students’ perceptions on online learning, provided significant implications in the field such as implementation of hybrid learning, telemedicine in medical curriculum.
V. CONCLUSION
In conclusion, the perceptions of clinical year medical students on online learning environments during the COVID-19 pandemic were satisfactory although there were challenging online learning experience during the pandemic. It was recommended to include qualitative method in future studies to provide more useful in-depth information regarding online learning environment.
Notes on Contributors
Dr Kye is the corresponding author for this paper. She designed the study, analysed the data, prepared the manuscript working together with the co-author.
Dr Amit Bhardwaj made substantial contributions to the design, editing and preparation of the final manuscript.
Ethical Approval
The research study was approved by Universiti Tunku Abdul Rahman Scientific and Ethical Review committee on 20th July 2020 (Approval number: U/SERC/92/2020).
Data Availability
The data that support the findings of the study are openly available at http://doi.org/10.6084/m9.figshare.19322297
Acknowledgement
We would like to acknowledge the clinical medical students of UTAR (Academic Year 2020/2021) for voluntary participation in this study.
Funding
There was no funding for this research study.
Declaration of Interest
The authors declare that there are no conflicts of interest, including financial, consultant, institutional and other relationships.
References
Bonk, C. J., & Reynolds, T. H. (1997). Learner-centred web instruction for higher order thinking, teamwork, and apprenticeship. In B. H. Khan (Ed.), Web-based instruction (pp.167-178). Englewood Cliffs.
Chew, R. (2015). Perceptions of online learning in an Australian University: Malaysian students’ perspective – Support for Learning. International Journal of Information and Education Technology, 5(8), 587-592. https://doi.org/10.7763/ijiet.2015.v5.573
Klein, H. J., Noe, R. A., & Wang, C. W. (2006). Motivation to learn and course outcomes: The impact of delivery mode, learning goal orientation, and perceived barriers and enablers. Personnel Psychology, 59(3), 665–702. http://doi.org/10.1111/j.1744-6570.2006.00050.x
Samoylenko, N., Zharko, L., & Glotova, A. (2022). Designing online learning environment: ICT tools and teaching strategies. Athens Journal of Education, 9(1), 49-62. https://www.athensjournals.gr/education/2022-9-1-4-Samoylenko.pdf
Pearson, J., & Trinidad, S. (2005). OLES: An instrument for refining the design of e-learning environments. Journal of Computer Assisted Learning, 21(6), 396- 404. https://doi.org/10.1111/j.1365-2729.2005.00146.x
*Kye Mon Min Swe
Jalan Sungai Long, Bandar Sungai Long,
43000 Kajang, Selangor
+601115133799
Email: drkyemonfms@gmail.com
Submitted: 29 May 2022
Accepted: 16 August 2022
Published online: 3 January, TAPS 2023, 8(1), 43-46
https://doi.org/10.29060/TAPS.2023-8-1/SC2807
Kirsty Foster
Academy for Medical Education, Medical School, University of Queensland, Brisbane, Australia
Abstract
Introduction: A series of workshops was held early in our MD curriculum redesign with two aims: gaining stakeholder input to curriculum direction and design; engaging colleagues in the curriculum development process.
Methods: Workshops format included rationale for change and small-group discussions on three questions: (1) Future challenges in healthcare? (2) our current strengths? (3) Future graduate attributes? Small-group discussions were audio-recorded, transcribed and fieldnotes kept and thematically analysed. We conducted a literature review looking at best practice and exemplar medical programs globally.
Results: Forty-seven workshops were held across 17 sites with more than 1000 people participating and 100 written submissions received. Analysis showed alignment between data from workshops, written submissions and the literature review.
The commitment of our medical community to the education of future doctors and to healthcare was universally evident.
Six roles of a well-rounded doctor emerged from the data: (1) Safe and effective clinicians – clinically capable, person-centered with sound clinical judgement; (2) Critical thinkers, scientists and scholars with a thorough understanding of the social and scientific basis of medicine, to support clinical decision making; (3) Kind and compassionate professionals – sensitive, responsive, communicate clearly and act with integrity; (4) Partners and team players who collaborate effectively and show leadership in clinical care, education and research; (5) Dynamic learners and educators – adaptable and committed to lifelong learning; and (6) Advocates for health improvement – able to positively and responsibly impact the health of individuals, communities and populations
Conclusion: Deliberate stakeholder engagement implemented from the start of a major medical curriculum renewal is helpful in facilitating change management.
Keywords: Medical Education, Medical Curriculum, Stakeholder Engagement, Collaboration
I. INTRODUCTION
The quality of the medical education we provide to future doctors is directly related to the quality of care they will provide to their future patients (Torralba & Katz, 2020). It is the responsibility of those involved and of medical schools to promote the highest standards of medical education and medical student learning. At the University of Queensland, a major reimagining of the MD Program is underway to ensure that our already strong medical program remains informed by best practice in both medicine and in education. This is crucial to enabling our medical graduates to be optimally equipped for their internship, pre-vocational and specialist training. It is our responsibility to enable our graduates to be ready for the future medical needs of the people and communities they serve.
Medical programs are complex and involve many people. As well as University academic and professional staff, medical students are taught, supervised and supported by a wide variety of doctors and other health professionals during the four years of our postgraduate degree. At our university we have approximately 4,500 affiliates who may have a role in teaching, supervising or otherwise influencing one or more medical students at some point during their four-year MD program. Many of these are clinical teachers or supervisors who work for the health services with which UQ has a student placement agreement in place. Cognisant that major curricular review is challenging we implemented a deliberate strategy of engagement with as many of our stakeholders as possible from the start of the MD Design project in 2019. In the first stage we planned a series of engagement workshops with key stakeholders and this is the basis of the study.
The purpose of our study was twofold:
Firstly, to gain input from a wide range of stakeholders early in the process to futureproof our curriculum – that is, to inform the vision on what our graduates need to be able to know, do, and be, to succeed in internship and beyond.
Secondly, to involve our key stakeholders in the curriculum design process as a component of change management.
II. METHODS
A series of stakeholder workshops was held. The format of each workshop was to start with a brief outline of the drivers and rationale for curricular change, followed by small-group interactive discussions focusing on three questions:
- What are the major future challenges in relation to healthcare?
- What are our current strengths as a Medical Program, as a university and as a health community?
- What are the important attributes for our future graduates to achieve to best prepare them for their careers?
Ethics approval for the study was granted by the University of Queensland Human Research Ethics Committee (Approval number 2019001725). At the start of each workshop attendees were provided with information about the study and given the opportunity to withdraw. Their participation in the workshop was regarded as consent. All small-group discussions were overseen by KF, audio-recorded and transcribed. KF and the administrative team kept field notes capturing any elements additional to the spoken word such as the general atmosphere of the workshop. KF and JH analysed the transcripts thematically identifying key elements in each focus area. In parallel a literature review was conducted looking at best practice medical education and exemplar medical programs across the globe were explored.
III. RESULTS
Over a period 15 months between July 2019 and January 2021 47 workshops were held across 17 sites with more than 1100 people participating. More than 100 written submissions were received and 5814 people and organisations contacted. Analysis demonstrated general agreement that major change was needed and there was good alignment between feedback received from stakeholder workshops, written submissions and the key findings from the current state analysis as outlined above. There were some stakeholders who felt that they needed to see more substantial evidence that the current curriculum needed refreshing. This group felt reluctant to embark on further change in view of modifications already made in recent years. They were also concerned that ‘change fatigue’ may be a challenge especially among our health service colleagues who contribute to the program.
A key finding was that the passion and commitment of our medical community to the education of future medical doctors and to make a positive contribution to healthcare was universally evident.
The resulting vision for our new MD program is:
To nurture and educate future medical graduates who are clinically capable, team players, kind and compassionate, serve responsibly and are dedicated to the continual improvement of the health of people and communities in Queensland, Australia and across the globe.
To enhance the capability of our graduates to meet the needs of their future patients a set of six roles of the all-round high-quality doctor was developed from the data. These roles map to the four domains that the Australian Medical Council require for primary medical degrees (Australian Medical Council (AMC), 2012), and have been adopted as the vertical themes of the new MD program. They are:
- Critical thinkers, scientists and scholars who have a thorough knowledge and understanding of the social and scientific basis of medicine, and able to apply evidence and research to inform and support clinical decision making.
- Dynamic learners and educators who continue to adapt, are curious, agile, motivated, self-directed, with the ability to honestly and humbly appraise their own learning needs, and have a commitment to lifelong learning.
- Advocates for health improvement who stand with people and are able to positively and responsibly impact the health of individuals, communities and populations. Are able to apply an understanding of health inequalities to strive for health equity, and incorporates prevention and advocacy into clinical practice in all settings.
- Partners and team players who collaborate effectively and show leadership when appropriate in the provision of clinical care and health-related education and research.
- Kind and compassionate professionals who are sensitive, responsive, communicate clearly and act with integrity. Compassion and professionalism are linked not only to improved patient outcomes but to better practitioner outcomes including job satisfaction and to better institutional outcomes.
- Safe and effective clinicians who are clinically capable, person-centred and demonstrate sound clinical judgement – and who can see that they cannot be safe and effective unless they are also capable in all other roles.
The new MD program is structured as five fully integrated courses, three year-long and two semester long courses in final year, with assessment focused on growth and development of knowledge skills and attitudes through active engagement in learning. Assessment for learning as well as of learning is fundamental in enabling all students to reach their full potential. The project has progressed through development of staged learning outcomes for each year of the program and now into detailed and appropriately sequenced learning activities.
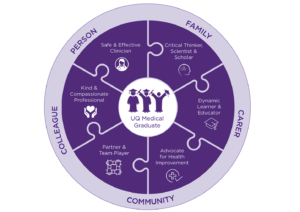
Figure 1. The six roles of a well-rounded doctor
IV. DISCUSSION
Communication throughout a period of major change is challenging especially where there are many diverse stakeholders across a large and complex organisation like a medical school (Velthuis et al., 2018). Our strategy was a deliberate one to retain connection and involvement during a lengthy process. Our initial engagement work reported here gave us a good start by actively involving as many people as possible from the beginning of the project. As the project has progressed stakeholders have remained engaged and have been particularly keen on seeking the detail needed to assist in implementation of the new curriculum. This has, on occasion, been challenging when tension between some specialist discipline areas protecting their ‘patch’ and the needs of medical students at primary medical degree level emerge. We also found that education is not regarded as a specialist field by some of our experienced clinical teachers. A lack of understanding about the iterative process of outcomes-based curriculum development contributed to colleagues seeking answers about what is to be taught being frustrated at what they saw as a laborious process of careful scaffolding and integration. This contesting of curriculum is recognised within institutions where it can inhibit development of more effective curricula which promote learning and are more than simply identification of content to be taught (Prideaux, 2003). By engaging with stakeholders from the earliest stage of the curriculum development process we feel that we have minimised this effect.
V. CONCLUSION
Our experience demonstrates that a deliberate stakeholder engagement strategy implemented from the start of a major curriculum renewal is helpful in maintaining key stakeholder involvement. We found that facilitating a collective discussion about the direction and underpinning values of an innovative medical curriculum was a helpful strategy although some stakeholders felt that, since their wishes had not been adopted, they had not been involved. Despite this, we found that, in most cases, stakeholder involvement from the start led to ongoing collaboration in the change management of implementing a new medical program.
We must ensure that our graduates are optimally prepared to begin their careers as medical practitioners over the next 30 to 40 years, and are ready to meet the needs of the people of Queensland, Australia and globally. We are confident that our early engagement on MD Design will help to achieve that goal.
Notes on Contributors
KF conceptualised, led the workshops where data were collected, contributed to data analysis and wrote the manuscript.
Ethical Approval
Ethics Approval for the study was obtained from the University of Queensland Human Research Ethics Committee, Application number 2019001725 granted June 2019. Potential participants were provided with study information prior to the workshops and their active participation in the ensuing workshop was taken to indicate consent.
Data Availability
Data is not currently stored in the UQ Data repository because of its nature, as transcripts of meeting discussions where the partipants may be identified would breach the conditions of ethics approval.
Acknowledgement
The curriculum design project described in this study is an endeavour involving a large number of people. The author would especially like to thank Professor Stuart Carney, Dean of the Medical School for his support in many of the engagement sessions, Dr Jane Hallos for her assistance with data collection, analysis and literature review, Ms Alexandra Longworth for assistance in data collection and all workshop participants for their input.
Funding
The study was funded as part of the MD Design project led by the Faculty of Medicine at the University of Queensland. There was no specific grant funding but the Mayne Bequest supported medical education research expenses.
Declaration of Interest
The author has no conflict of interest to declare.
References
Australian Medical Council (AMC). (2012). Standards for assessment and accreditation of primary medical programs by the Australian Medical Council 2012. Australian Medical Council Ltd.
Prideaux, D. (2003). ABC of teaching and learning in medicine: Curriculum design. BMJ, 326(7381), 268-270. https://doi.org/10.1136/bmj.326.7383.268
Torralba, K. M. D., & Katz, J. D. (2020). Quality of medical care begins with quality of medical education. Clinical Rheumatology, 39, 617-618. https://doi.org/10.1007/s10067-019-04902-w
Velthuis, F., Varpio, L., Helmich, E., Dekker, H., & Jaarsma, A. D. C. (2018). Navigating the complexities of undergraduate medical curriculum change: change leaders’ perspectives. Academic Medicine, 93(10), 1503-1510. https://doi.org/10.1097/ACM.0000000000002165
*Kirsty Foster OAM
Academy for Medical Education, Medical School,
Level 6, Oral Health Centre,
288 Herston Road
Herston QLD 4006 Australia
+61 7 3346 4676
Email: Kirsty.foster@uq.edu.au
Submitted: 28 July 2022
Accepted: 12 October 2022
Published online: 3 January, TAPS 2023, 8(1), 25-32
https://doi.org/10.29060/TAPS.2023-8-1/OA2850
Choon Peng Jeremy Wee1, Mingwei Ng1 & Pim W. Teunissen2
1Department of Emergency Medicine, Singapore General Hospital, Singapore; 2School of Health Professions Education (SHE), Faculty of Health Medicine and Life Sciences, Maastricht University, Maastricht, The Netherlands
Abstract
Introduction: This study was performed to understand how fixed clinical teams affected informal learning in Emergency Medicine Residents. Better understanding the effects of team dynamics on informal learning may help to optimise learning and improve performance.
Methods: From 8th February 2020 till 27th September 2020, the Singapore General Hospital Emergency Department adopted a fixed team system. Zoom interviews were carried out amongst Emergency Medicine Residents who worked in the fixed team system using a semi-structured iterative interview guide. A qualitative content analysis was used for this exploratory study. The interviews were transcribed verbatim, anonymised and coding via template analysis performed. Data collection and analysis were performed until data sufficiency.
Results: The themes identified centred around relationship dynamics, team composition and motivation for learning. The first was how improved relationships led to improved trust, communications and camaraderie among team members. This improved peer learning and clinical supervision and provided a more personalised learning experience. A balanced team composition allowed learners to be exposed to experts in various subspecialties. Finally, there was an initial increase in motivation, followed by a decrease with time.
Conclusion: In postgraduate medical education, working in a fixed team system with balanced members had positive effects on informal learning by strengthening relationships and communications.
Keywords: Informal Learning, Workplace Learning, Fixed Teams, Medical Education, Postgraduate
Practice Highlights
- Fixed teams can strengthen relationships between members through better trust, familiarity and communication.
- A balanced fixed team with members having different areas of expertise allows a variety of perspectives.
- Rotation of team members may achieve a balance between the stronger relationship and familiarity of the members of fixed teams and the greater variance in perspectives from a non-fixed team system.
I. INTRODUCTION
Fixed teams (FT) and non-fixed teams (NFT) exist in medicine because of differing service requirements and manpower resources. Examples of FTs can exist in ward round teams and operating surgical teams (Eddy et al., 2016; Stepaniak et al., 2012) where personnel stay within the same work team for long periods. In other areas of healthcare like the Emergency Departments (ED), a NFT system is usually employed where teams are formed according to the personnel rostered to work on that shift and team members change every shift. This allows a more flexible system for the team members as they can request off days and leave according to their personal schedule and yet allows for 24-hour coverage in the ED.
High levels of performance are required of medical teams, both fixed and non-fixed, to achieve good patient outcomes. Therefore, team members should learn how to work effectively together to deliver the best patient care. There are studies, both within healthcare and other industries, which showed mixed results when FT were compared with NFT with regards to team performance. A systematic review on minimal invasive surgical teams found that the FTs had better teamwork and had reduced rates of technical mistakes compared to NFTs (Gjeraa et al., 2016). However, an aviation study showed that FTs made more minor errors compared to NFTs due to FT members being too familiar with each other and overlooking errors (Barker et al., 1996). Although it is unclear how transferable specific research findings from non-healthcare domains are, what is clear is that FTs and NFTs are different in the way teams were formed and the amount of time team members spend working together. There is a lack of understanding if and how these differences affect the way learning takes place in FT and NFTs; which could translate to the performance of the team and its members.
Workplace learning occurs through informal learning by experiencing work challenges and via interpersonal relationships. Informal learning can be supported through learner engagement by encouraging active participation in work activities and aligning learners’ interests with that of the organisation’s objectives towards improving the individuals’ and organisation’s capabilities (Billett, 2007). Informal learning is now widely accepted as a form of workplace learning that occurs out of a formal planned teaching program. It usually occurs during work activities which are not primarily aimed towards education, with learning objectives not planned beforehand (Callanan et al., 2011; Rogoff et al., 2016; Watkins et al., 2018). Although informal learning had been studied, there are very few studies looking at how being in FTs affects informal learning. A review on the involvement of employees in workplace learning (Kyndt & Baert, 2013) revealed that there was a paucity of literature on whether any team system improves the involvement of employees in informal learning. Thus, it remains to be studied what effects working in a FT system has on informal learning especially of the more junior team members.
An integrative literature review on informal learning found that some of the important components of informal learning within members of a team and between teams included interpersonal relationships, feedback, networking and leadership (Jeong et al., 2018). Therefore, there may be differences in interpersonal relationships and feedback between the different team systems. It is known that good interpersonal relationships include good supervisor and peer support and both affect whether what is learnt is applied at the workplace (Burke & Hutchins, 2016), there was little published data on whether supervisor and peer support or even the supervisory relationship were affected by the amount of time spent together. Within some healthcare systems both FTs and NFTs consists of members with varying levels of experience, differing expertise and roles. In a FT, the learners are only supervised by supervisors within that team; therefore, each learner’s supervised time is divided within a small group of supervisors as compared to a NFT system where each learner’s supervised time is spread amongst a larger number of supervisors. Thus, despite this increased time spent together in a FT, it is not clear if working in a FT impacts supervisory or interpersonal relationship.
Having a good trusted learner-supervisor relationship can result in the establishment of an “Educational Alliance” (Telio et al., 2015). This is because feedback from a credible trusted source was more readily accepted and feedback is another important component of effective informal learning within a team (Jeong et al., 2018).
Furthermore, a study among social work students and their supervisors in a rotational placement model, found that the longer the amount of time they spent with each other the greater the trust between them (Vassos et al., 2017). On the other hand, being in a FT could restrict networking and socialisation to a smaller group of people as contact with other teams’ members could be reduced however it is not known how this could affect informal learning.
Understanding how informal learning takes place within FT and NFT may allow optimisation of learning within each and perhaps even configure teams to enhance learning and thus ultimately improve performance. Our study aimed to fill this gap in the literature by exploring how fixed clinical teams affected the experience of informal learning for Emergency Medicine (EM) Residents. By doing so we hope to understand how informal learning can be supported via the appropriate implementation of team systems especially where high performance is expected from the teams.
II. METHODS
To study how being in fixed clinical teams affected the experience of informal learning for EM Residents we conducted an exploratory qualitative study based on a constructivism research paradigm using content analysis of individual interviews. This is because informal learning could not be quantified with specific learning outcomes.
A. Setting
EDs teams manage a large number of critically ill patients who may need time sensitive interventions. These teams would comprise of experienced Emergency Physicians (EPs) and more junior Medical Officers (MOs) and Residents. The Residents are postgraduate doctors who are training to graduate as EPs; therefore, informal workplace learning is a crucial part of their training. Hence the residents would be good study subjects to investigate the effect of team systems on informal learning.
The Singapore General Hospital (SGH) ED functioned via NFTs where the composition and number of members in the team differed with each 8 hour shifts accordingly to the anticipated patient load. The COVID-19 pandemic provided a naturalistic setting where the effect of a FT system can be compared to a NFT system which had existed before hand. After COVID-19 was declared a pandemic by the World Health Organisation (WHO) on the 11th March 2020 (World Health Organisation, 2020). There was an emphasis on infection control to contain the pandemic. Many countries had instituted social distancing measures which included curfew-like measures and travel restrictions (Lake, 2020). Similarly, the Singapore government had instituted legislative measures to limit face-to-face interactions. In the ED of SGH, measures were put in place to limit the spread of COVID-19.
Thus, from 8th February till 27th September 2020, as part of infection control measures, doctors were organised into 5 FTs, each having between 5-7 Consultants, 3-5 EM Senior Residents, 2-3 EM Junior Residents and 7-9 non-EM Medical Officers (MO) (Liu et al., 2020; Quah et al., 2020). The Senior Emergency Physicians (SEPs) consisted of certified specialists in EM (Associate Consultants, Consultants and Senior Consultants); they played supervisory and educational roles to the junior doctors (JD) which included MOs, Junior Residents and Senior Residents. Each FT worked 12-hour shifts. Interactions between teams were kept to a minimum and members from different teams were not allowed to mingle. Thus, the residents were only supervised by their team’s SEPs. Informal learning would now occur within these FTs.
Formal learning was converted to a remote online platform because of infection control measures. Lectures and tutorials were held and recorded using software which enabled online asynchronous access e.g. Zoom (Zoom, 2016) as not all residents could be given protected learning time together. Sessions which could not be transferred onto an online platform (e.g. hands on simulation and procedure skills training) were cancelled. Formal summative examinations were also cancelled.
B. Interviews
Interviews were conducted and recorded via Zoom (Zoom, 2016) to maintain social distancing. The primary investigator performed 11 interviews and a coinvestigator performed the remaining 4 out of a total of 15 interviews. A semi-structured iterative interview guide was developed based on Eraut’s typology on informal learning which included team activities, tasks and enabling/disabling factors (Eraut, 2010) was used, and the interviews were audio-recorded and transcribed verbatim and anonymised. The interviews allowed positive and negative aspects to be explored and being semi structured the questions asked varied according to the interviewees’ responses. This helped to focus the interviewees to what informal learning was with examples when it could occur within team activities. The guide was iteratively amended with each interview to enhance clarity which helped to obtain more in-depth data in later interviews.
C. Participants
Twenty-four ED residents were working in the FT system in the ED of SGH during COVID-19. Fifteen were Junior Residents and 9 were Senior Residents. Purposive sampling was carried out with at least two Residents from each team being sampled. This is to ensure that there was good representation for all of the fixed clinical teams. All 24 residents were invited to participate via email and WhatsApp messaging platform with written consent being obtained. Fifteen individual interviews were conducted before data sufficiency was achieved where no new data would change the outcome of the study, thus no further interviews were conducted beyond data sufficiency (Varpio et al., 2017). Eleven interviewees were Junior Residents (4 females and 7 males) and 4 were Senior Residents (3 females and 1 male).
D. Data Analysis
Data analysis was performed via template analysis by the primary and coinvestigator independently (Brooks et al., 2015). Eraut’s typology developed from his research on informal learning was used as a priori themes in the initial coding template (Eraut, 2010). Coding template modifications were made as the analysis of the transcripts continued. Themes were categorised into hierarchical clusters and relationships between them were studied and defined. After final modifications, the coding template was applied to the entire data set. Coding themes were compared and discussed between the primary investigator and the coinvestigator until consensus was reached.
E. Ethics
Waiver for approval was granted by the Singhealth Institutional Ethics Board. The primary investigator was a core faculty within the Singhealth Emergency Medicine Residency Program and although the interview was conducted among EM residents the primary investigator did not conduct the interviews when the interviewees were from the same team as the primary investigator. These were conducted by the coinvestigator. The coinvestigator was an EM Senior Resident who was not involved in the FT system. A reflexivity diary was kept, and peer debrief was done.
III. RESULTS
Three main themes emerged on how working in FTs affected informal learning amongst our participants (Figure 1). These included changes in relationship dynamics between members, effect of FT composition on informal learning of the participants and influence on motivation.
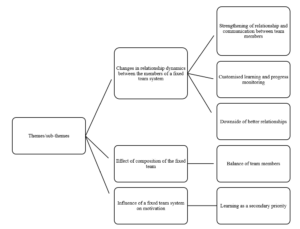
Figure 1. Themes and sub-themes
Theme 1: Changes in Relationship Dynamics between FT Members
From the interviews, the participants felt that the FT system resulted in more familiarity, trust, teamwork and improved communications between team members including SEPs, Residents and MOs. Interviewees felt that this strengthened the relationship dynamics between FT members as compared to a NFT. This meant that FT members were able to coordinate and exchange information better. It led to an increase in familiarity in knowing each member’s style of practice and way of thinking. The team members could understand each other better and how they reasoned.
The strengthened relationship between residents and SEPs changed with dynamics. Having a “closer rapport” and “deeper bond” allowed the residents to “tag along” with SEPs “more often” and gave the residents more insight as to why the SEPs behaved in a certain way as to “how they had practiced medicine” and the rationale behind each step was “more easily communicated to the residents who were tagging along” (Resident A), resulting in residents having a deeper understanding of why things were done in addition to how things were done. This strengthened relationship was also present between the residents and their peers. Therefore, peer learning improved within the FTs as junior residents reported feeling less reservation in asking each other questions.
Resident D felt that peer learning was better within FTs because of the improved relationship, there were less reservations which had prevented him from asking his peers questions in a NFT setting.
He elaborated:
“Fixed team [was] definitely better for peer learning. For the same reasons, because you know each other better, you’re more familiar. We don’t only talk to each other about work… after a while, when you go for meals together… or rather like resting together and no cases around you sit and talk. So there’s a lot more familiarity with the person you’re working with, and… you’re just more comfortable with asking questions… you don’t feel like this is somebody who’s going to judge you if [you] asked a stupid question”
This was not just amongst the residents but also with SEPs. Resident G felt that it was easier for the residents to speak to the SEPs because of familiarity and resulted in less workplace stress:
“Over the time as we knew each other better … the workplace stress was much lower… so I could… work with less stress at workplace… Because if you didn’t really know the consultant you tend to be afraid to talk to them; then of course your stress levels will be higher. But if you know that consultant and you know what kind of person, he or she is then you could be more comfortable to talk to them…”
“…It is more comfortable to… approach the senior because you know every day… we have a fixed team so naturally we feel that our relationship is closer…”
“… so, I won’t be too afraid to speak out or to talk to them to discuss with them.”
Contributing to additional ways of informal learning, communication within FTs even during work took on a more “friendly [and] social” form with greater congeniality and via more “communication platforms” (WhatsApp and Tiger Text) which continued even “outside of work” (Resident H). These platforms were also used as learning tools to facilitate case discussions, share learning points and experiences. This was not previously present in the NFTs. The residents felt that learning was more customised because of the change in relationship dynamics. In FTs, there was closer supervision of residents by SEPs. The residents “spent more time” with the same group of supervisors, thus the supervisors were able to better “assess both strengths, weaknesses and address any particular loopholes” of the residents (Resident A).
However, there were some adverse effects of this change in relationship dynamics. Some residents felt that with a closer relationship between team members, supervisors sometimes were more tolerant of the learners’ shortcomings and be less likely to point it out because of not wanting to affect the relationship. This closer relationship could result in residents taking “shortcuts” and “flying under the radar” because they knew the SEPs could tolerate or would not scrutinise the learners closely once “trust” was established (Resident L). Resident H gave an example of how familiarity could lead to less critical thinking by the learner:
“If… the senior always does like… [Rapid Sequence Intubation] … even though I question the first time I saw him do that… subsequently … every time I work with him I will do [it] this way. I won’t really think does the patient really need this way [of management] or will the patient benefit in a different way… if you are working with different bosses then every case you need to restart your thinking…”
Theme 2: Effect of Composition of the FT
All interviewees felt that the composition of the FT had affected informal learning, and that having a balanced team in terms of a wide range of years of practice amongst both the SEPs as well as the JDs would help improve informal learning. Having a team where the JDs were of differing seniorities of practice could help with peer learning because the senior ones could help the junior ones more. This also applied to the SEPs as that provided a wider perspective to clinical issues due to having different clinical experience and expertise in different subspecialties. Furthermore, if the JDs in a FT were of a similar level of practice, Resident C expressed that they could be “competing with each other for cases and procedures” which adversely affected informal learning with fewer opportunities to perform procedures. In a NFT the members would be constantly changing and it would be unlikely its JD would be always of the same level of practice.
The interviewees expressed concern that within a FT system that, although residents had close contact with a fixed group of supervisors, they lacked contact with the other teams’ SEPs. Many residents felt that this had adversely impacted informal learning because the SEPs were experts in different subspecialties (e.g., Trauma, Toxicology, Ultrasound, etc). By not interacting with many SEPs, residents were unable to learn from them. Furthermore, different supervisors had different perspectives and approaches to patients which the residents may not be exposed to if they were not in the same team as these seniors. However, this was mitigated by having a team with a balanced variation in the areas of specialty of the seniors. Resident F summarised this:
“…a team with… people from different seniorities are essential… (even) juniors can teach seniors… the way that my team was composed… it was a good mix… there are people from different… specialties… from different seniorities even within the juniors … like first posting to… [senior post graduate years]… offers different perspectives, learning of different things… people from different [subspecialties] can offer insight into the systems-based learning or component from other parts of the institution…”
Theme 3: Influence of a FT System on Motivation
Many residents felt that having FTs increased their motivation to learn. This resulted from their supervisors being able to inspire them and follow up with their learning progress more closely. Resident M was motivated to learn because his “friends (FT members) were very motivating” and “enthusiastic”; this encouraged him to learn more. Furthermore, resident C felt more motivated to learn in a FT because he “always sees the same senior” and this more frequent contact results in him being “more likely to take their feedback and opinion more seriously and work harder”
However, “after some time everyone is comfortable with each other” and some participants feared that their motivation “might go down” (Resident N). This was because there was a feeling of complacency as time went on within a FT, hence the motivation to learn started to dwindle after an initial increase.
Other reasons for this decline were related to COVID-19, the focus was more on facing the threat rather than learning and the priority to learn was secondary. The motivation to learn “was a bit less” as “the mood was more to survive than to learn”; Resident L was “less driven to learn” because there was a “general bleakness in the whole situation of [COVID-19] which made his “inner desire to learn… wane a bit”
IV. DISCUSSION
This study explored how working in fixed clinical teams affected informal learning for EM Residents. There are many pros and cons to fixed team rostering however the focus of this study is on informal learning. The findings highlighted the importance of having a balanced team composition where team members were able to establish trust and a strong bidirectional relationship because of the longer time spent working together. Motivation to learn increased initially; however after some time, some felt a decrease. This was consistent with prior work which highlighted team dynamics and commitment and that feedback which was given often and in a socially interactive environment were factors which helped to enable effective work-based learning (Attenborough et al., 2019; Jeong et al., 2018; Kyndt et al., 2016). Unlike in Attenborough’s work where team leadership was one of the factors identified; our respondents did not mention the effect of team leadership on informal learning. Their focus was more on the relationships between the different team members. From this study the predominant factors which positively affected informal learning included teamwork, collaborative task performance, where good communication was needed between different people, and personal development especially in building interpersonal relationships and group decision making.
Limited studies were done on how FTs affect informal learning. Our study found that FTs resulted in more (informal) communication channels (e.g. WhatsApp) being formed which was not present in NFTs, resulting in more learning activities including sharing ideas, resources and experiences. These sharing activities were some of the major forms of informal learning activities identified in the literature (Lohman, 2006). FTs resulted in open communication and quality feedback which was well received, and were found to be beneficial towards informal learning (Jeong et al., 2018). Our study showed that working in a FTs led to more customised learning. Findings of improved communications and strengthened relationships in a bidirectional manner involving teacher and learner alike, supports a shift from a predominantly teacher to learner type of dynamics to a team learning dynamics where all team members can learn with and from one another. This is important because informal learning takes place effectively when learning from past mistakes and feedback exchange occurs, involving both cognitive and social interactions (Jeong et al., 2018).
FTs had negative effects on informal learning as well. Familiarity resulted in supervisors being more tolerant of shortcomings and FTs limited learners’ contact with other teams’ supervisors and adversely affected informal learning. This was because informal learning also takes place when there is sharing of ideas, expertise and experience (Lohman, 2006) and limiting the number of supervisors limits the variance of shared viewpoints.
Our study has limitations. Firstly, interviewee recall bias was possible because 6 months had passed after the FT system was stopped before the interviews. Therefore, some details may not have been accurately recalled given this period which could affect the trustworthiness of results. Secondly, the participants were likely to be comparing their experiences in the FT system during COVID-19 to a NFT system without a pandemic. Thus, some of the experienced changes may be because of the pandemic rather than purely due to the FT system. Thirdly, there are many pros and cons to FTs however the focus of this study is on informal learning thus other factors not investigated with this study may affect the feasibility of FT. Lastly there could be power differential effects between the interviewers and the interviewees because the interviewers performed supervisory and roles to the residents. However, to mitigate this, a reflexivity diary was kept, and peer debrief between the two interviewers was performed. Furthermore, the interviewers did not interview members who had been in the same team as them.
V. CONCLUSION
In conclusion, FTs impact informal learning by building strong relationships with improved team communications and adding a social dimension for learning. A balance of team members as well as rotating the residents across different FTs may be beneficial for improving informal learning for EM Residents.
Notes on Contributors
Dr Wee Choon Peng Jeremy submitted the CIRB application, (with the help of the last author) conceptualised the study and its design. He performed the literature review, recruited and interviewed the participants, collected and transcribed the data, performed the thematic analysis of the data and wrote the manuscript.
Dr Ng Mingwei helped to recruit and interview some of the participants, transcribed and collected the data. Dr Ng helped perform the thematic analysis of the data and helped edit the manuscript.
Prof. Dr. Pim Teunissen was central to the conceptualisation of the study, advised on the design of the study and gave critical feedback to the writing of the manuscript and edited the manuscript extensively
All the authors have read and approved the final manuscript.
Ethical Approval
We have included the letter for waiver of CIRB via email. Ethics approval for waiver of written informed consent was obtained from the Singhealth Institutional Review Board (CIRB Ref: 2020/3114).
Data Availability
As the data set is qualitative in nature, we are not able to upload that in any public repository.
Funding
There is no funding for this paper/study.
Declaration of Interest
The authors report there are no competing interests to declare.
References
Attenborough, J., Abbott, S., Brook, J., & Knight, R. A. (2019). Everywhere and nowhere: Work-based learning in healthcare education. Nurse Education in Practice, 36, 132-138. https://doi.org/10.1016/j.nepr.2019.03.004
Barker, J. M., Clothier, C. C., Woody, J. R., McKinney, E. H., Jr., & Brown, J. L. (1996). Crew resource management: A simulator study comparing fixed versus formed aircrews. Aviation, Space, and Environmental Medicine, 67(1), 3-7.
Billett, S. (2007). Constituting the workplace curriculum. Journal of Curriculum Studies, 38(1), 31-48. https://doi.org/10.1080/00220270500153781
Brooks, J., McCluskey, S., Turley, E., & King, N. (2015). The utility of template analysis in qualitative psychology research. Qualitative Research in Psychology, 12(2), 202-222. https://doi.org/10.1080/14780887.2014.955224
Burke, L. A., & Hutchins, H. M. (2016). Training transfer: An integrative literature review. Human Resource Development Review, 6(3), 263-296. https://doi.org/10.1177/1534484307303035
Callanan, M., Cervantes, C., & Loomis, M. (2011). Informal learning. Wiley Interdisciplinary Reviews Cognitive Science, 2(6), 646-655. https://doi.org/10.1002/wcs.143
Eddy, K., Jordan, Z., & Stephenson, M. (2016). Health professionals’ experience of teamwork education in acute hospital settings: a systematic review of qualitative literature. JBI Database of Systematic Reviews Implementation Reports, 14(4), 96-137. https://doi.org/10.11124/JBISRIR-2016-1843
Eraut, M. (2010). Informal learning in the workplace. Studies in continuing education, 26(2), 247-273. https://doi.org/10.1080/158037042000225245
Gjeraa, K., Spanager, L., Konge, L., Petersen, R. H., & Ostergaard, D. (2016). Non-technical skills in minimally invasive surgery teams: A systematic review, Surgical Endoscopy, 30(12), 5185-5199. https://doi.org/10.1007/s00464-016-4890-1
Jeong, S., Han, S. J., Lee, J., Sunalai, S., & Yoon, S. W. (2018). Integrative literature review on informal learning: Antecedents, conceptualizations, and future directions. Human Resource Development Review, 17(2), 128-152. https://doi.org/10.1177/1534484318772242
Kyndt, E., & Baert, H. (2013). Antecedents of employees’ involvement in work-related learning. Review of Educational Research, 83(2), 273-313. https://doi.org/10.3102/0034654313478021
Kyndt, E., Vermeire, E., & Cabus, S. (2016). Informal workplace learning among nurses. Journal of Workplace Learning, 28(7), 435-450. https://doi.org/10.1108/JWL-06-2015-0052
Lake, M. A. (2020). What we know so far: COVID-19 current clinical knowledge and research. Clinical Medicine, 20(2), 124-127. https://doi.org/10.7861/clinmed.2019-coron
Liu, Z., Teo, T. L., Lim, M. J., Nadarajan, G. D., Segaram, S. S. C., Thangarajoo, S., Wee, L. E., Wee, J. C. P., & Tan, K. B. K. (2020). Dynamic emergency department response to the evolving COVID-19 pandemic: The experience of a tertiary hospital in Singapore. Journal of the American College of Emergency Physicians Open, 1(6),1395-1403. https://doi.org/10.1002/emp2.12264
Lohman, M. C. (2006). Factors influencing teachers’ engagement in informal learning activities. Journal of Workplace Learning, 18(3), 141-156. https://doi.org/10.1108/13665620610654577
Quah, L. J. J., Tan, B. K. K., Fua, T. P., Wee, C. P. J., Lim, C. S., Nadarajan, G., Zakaria, N. D., Chan, S. J., Wan, P. W., Teo, L. T., Chua, Y. Y., Wong, E., & Venkataraman, A. (2020). Reorganising the emergency department to manage the COVID-19 outbreak. International Journal of Emergency Medicine, 13(1), Article 32. https://doi.org/10.1186/s12245-020-00294-w
Rogoff, B., Callanan, M., Gutiérrez, K. D., & Erickson, F. (2016). The organization of informal learning. Review of Research in Education, 40(1), 356-401. https://doi.org/10.3102/0091732×16680994
Stepaniak, P. S., Heij, C., Buise, M. P., Mannaerts, G. H., Smulders, J. F., & Nienhuijs, S. W. (2012). Bariatric surgery with operating room teams that stayed fixed during the day: A multicenter study analyzing the effects on patient outcomes, teamwork and safety climate, and procedure duration. Anesthesia and Analgesia, 115(6), 1384-1392. https://doi.org/10.1213/ANE.0b013e31826c7fa6
Telio, S., Ajjawi, R., & Regehr, G. (2015). The “Educational Alliance” as a framework for reconceptualizing feedback in medical education. Academic Medicine, 90(5), 609-614. https://doi.org/10.1097/ACM.0000000000000560
Varpio, L., Ajjawi, R., Monrouxe, L. V., O’Brien, B. C., & Rees, C. E. (2017). Shedding the cobra effect: Problematising thematic emergence, triangulation, saturation and member checking. Medical Education, 51(1), 40-50. https://doi.org/10.1111/medu.13124
Vassos, S., Harms, L., & Rose, D. (2017). Supervision and social work students: Relationships in a team-based rotation placement model. Social Work Education, 37(3), 328-341. https://doi.org/10.1080/02615479.2017.1406466
Watkins, K. E., Marsick, V. J., Wofford, M. G., & Ellinger, A. D. (2018). The evolving Marsick and Watkins (1990) theory of informal and incidental learning. New Directions for Adult and Continuing Education, 2018(159), 21-36. https://doi.org/10.1002/ace.20285
World Health Organisation. (2020). World Health Organisation emergencies press conference on coronavirus disease outbreak – 11 March 2020. https://www.who.int/director-general/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19—11-march-2020
Zoom. (2016). Security guide. Zoom Video Communications Inc.
*Wee Choon Peng Jeremy
Outram Road,
Singapore 169608
Email: jeremy.wee.c.p@singhealth.com.sg
Submitted: 26 November 2021
Accepted: 21 July 2022
Published online: 3 January, TAPS 2023, 8(1), 33-42
https://doi.org/10.29060/TAPS.2023-8-1/OA2712
Jaime Maria Tan1, Junaidah Binte Badron1 & Sashikumar Ganapathy1,2
1Department of Emergency Medicine, KK Women’s & Children’s Hospital, Singapore; 2Duke-NUS Medical School, Singapore
Abstract
Introduction: Perceptions towards the working and learning environment as well as coping mechanisms have been studied across different healthcare sectors. They have shown to reduce stress and burnout. However, perceptions of the work environment in the Emergency Department (ED) setting have not been studied in depth. The literature surrounding coping mechanisms also mostly focuses on their impacts rather than the mechanisms utilised. In addition, these were often investigated using surveys. This study aimed to use a phenomenological approach to explore the perceptions and coping strategies of junior doctors working in a paediatric ED.
Methods: Sixteen junior doctors working in the Paediatric ED were recruited. Semi-structured interviews were conducted after conducting literature reviews. Data was collected until saturation point. All interviews were recorded and transcribed verbatim manually and subsequently analysed.
Results: The greatest fears of junior doctors starting their paediatric emergency posting were lack of knowledge due to inexperience in the subspecialty; fear of the work environment due to unfamiliarity as well as workload and the intrinsic high-stress environment. The main coping strategies were ensuring clinical safety, obtaining psychosocial support from loved ones and colleagues, and placing focus on spirituality and wellbeing.
Conclusion: In this study, the perceptions and coping strategies of the junior doctors in the Paediatric ED were explored. The findings from this study will help to structure and improve the support given to future junior doctors who rotate to the department as well as better orientate them to allay their pre-conceived notions.
Keywords: Coping Behaviours, Perceptions, Paediatric Emergency Department, Stressors, Interviews
Practice Highlights
- Participants worried about knowledge, workload and responsibilities prior to starting their posting.
- Perceptions were mostly of an anticipatory nature, influenced by seniors’ past experiences.
- In work, support from senior staff was helpful in allaying their fears and increasing patient safety.
- Participants felt psychosocial support, spirituality and wellness were useful coping strategies.
- Maladpative coping strategies did not come up as a main theme in our study.
I. INTRODUCTION
Perceptions toward the work and learning environment can strongly impact experiences and even lead to large amounts of stress (Chan et al., 2016). A poorer perception of the learning environment is also associated with greater levels of burnout (Chew et al., 2019; Sum et al., 2019). Conversely, a positive perception of the work environment helps to alleviate stress (Abraham et al., 2018). Workers’ perception of their work environment contributes significantly to their overall experiences.
Main factors contributing to stress in the ED include heavy workload and critically ill patients. Workplace violence, trauma, abuse and morbidity also add to the stress and burnout experienced (Burbeck et al., 2002; Copeland & Henry, 2018; Healy & Tyrrell, 2011; Xu et al., 2019). In the paediatric setting, added stressors include dealing with sexual abuse and non-accidental injury as well as death and the inability to provide optimal care for children (Alomari et al., 2021; Basu et al., 2016; Durand et al., 2019; Greenslade et al., 2019; Shanafelt et al., 2012; Watson et al., 2019).
Given these significant stressors, individuals utilise different coping mechanisms to mediate these experiences (Howlett et al., 2015).
Some coping strategies discussed in previous studies include socialising with friends and family (Gribben et al., 2019). Focusing on physical wellbeing, clinical variety, reflectivity, and organizational activities were also helpful in alleviating burnout in other areas of healthcare (Barham et al., 2019; Koh et al., 2015).
Several studies also found that the use of maladaptive coping mechanisms, such as alcohol use and self-blame increased with the frequency of burnout (Jackson et al., 2016; Oreskovich et al., 2015; Ryali et al., 2018; Talih et al., 2018).
While many studies studied stressors and the effectiveness of the coping mechanisms used, the actual components of coping mechanisms were not well studied. In studies that did look at coping mechanisms and their effectiveness, these studies were also often done via the survey method and were only evaluated on the surface.
Most studies looked at healthcare workers in general. Few studies looked solely at the doctor population. This makes conclusively evaluating the doctor component of coping mechanisms and their effects difficult.
While other studies looked at an adult emergency perspective, there were also few studies looking at the paediatric ED. It has been reported that dealing with paediatric emergencies causes more stress compared to their adult equivalents. Some of the contributing factors are related to the nature of working with children. These, in itself, are unmodifiable (Guise et al., 2017). Therefore, it is important to study how the paediatric context can affect the experiences of the doctors who care for them.
In our study, we studied the perceptions of junior doctors at the beginning of their posting. We subsequently explored their coping mechanisms in the Singaporean context.
The element of stress in the ED among junior doctors is significant as the ED is often part of many specialist training pathways (Mason et al., 2015). During the time of training, the doctors are still learning and developing. Hence, many doctors experience sharp learning curves during their postings. This brings about more stress (McPherson et al., 2003). In some cases, the stress can even lead to doctors thinking about leaving clinical practice altogether (Degen et al., 2014).
In the Singaporean context, paediatric emergency postings are part and parcel of speciality training for junior doctors (especially for those in emergency medicine and family medicine training). Because of this, junior doctors spend the majority of their paediatric postings in the paediatric emergency. As such, a Singapore-specific context would give light on the challenges of this sizable group.
The nature of the healthcare system in Singapore is unique. Up to 60% of the consultations in the paediatric ED were for nonurgent conditions due to the overall perception of the severity of symptoms and parental preference towards paediatric specialist facilities (Ganapathy et al., 2015). This would lead to an increased workload for the paediatric ED. The distribution in workload may also differ compared to a global perspective, with the load of severe paediatric trauma in Singapore being low (Pek et al., 2019).
These subtleties in the paediatric ED in Singapore can influence the experiences of junior doctors differently. With these key differences in mind, we aimed to investigate the perceptions of junior doctors towards their paediatric ED posting in Singapore and how they subsequently coped with the challenges faced.
II. METHODS
A. Design
In this study, we examined the experiences of doctors in their paediatric ED rotation and how their thoughts and actions influenced their stress during their rotation. We deemed the phenomenological approach to be the most appropriate for this study. Phenomenology is defined as the study of how individuals see and experience a phenomenon and what this means to the individuals in their own experience (Neubauer et al., 2019; Smith, 2021).
The approach we chose was that of an interpretive phenomenological analysis in which we aimed to investigate the experience through the participants’ own experiences and perceptions. With the help of the various participants’ accounts, themes and ideas bound by their experiences were explored (Tuffour, 2017).
B. Methods
The members of the study performed a preliminary literature review on the topic and explored plausible methods of data collection. The study team decided on semi-structured interviews as it promotes sharing and would allow for sufficient privacy.
The team members included a senior consultant, a staff physician and a medical officer. Together, after discussions about concepts that the team was keen to explore, an interview guide was drawn up.
Subsequently, a proposal was submitted to the Hospital Centralised Institutional Review Board for approval.
One-on-one interviews were conducted with the participants by investigator A, a medical officer who was rotating within the department at the time of the study. This was done to reduce the power differential. Interviews were conducted at a location and time convenient to the participant.
Prior to the interviews, consent was sought and all interviews were recorded and subsequently transcribed verbatim. The interviews were conducted over a 1-month period in December 2019.
Questions were open-ended and allowed participants to share ideas that they were keen to raise with no restrictions to the topics brought up. Interview questions were tweaked alongside subsequent interviews so that they were easier to understand and would encourage sharing. Additional questioning in subsequent interviews was adopted to improve clarity. For example, one of the questions that featured early in the interviews was ‘What are some of the coping mechanisms you use?’ During subsequent interviews we noticed some participants utilised coping mechanisms before work to prepare themselves, some used other strategies during work to cope with the stress, while others dealt with their stressors after getting off work. We tweaked the question to include ‘during the shift or outside of the shift’ to help participants widen their perspective about certain coping methods they may have used but were not immediately conscious of when answering the questions. No new questions referring to particular themes were inserted although interviewers were aware of the themes that had been highlighted in previous interviews. This was done in addition to the initial interview guide and ensured the broad nature of questioning was not compromised and the breadth of interviews was maintained.
Themes were identified from the interviews until data saturation was reached. Data saturation was noted at the 12th interview. The team continued to learn from subsequent interviews, with interviews contributing additional depth to the issues explored. Further interviews were conducted to confirm that no new theme was being identified.
The interviews were then transcribed and de-identified. They were subsequently reviewed by 2 reviewers (Investigator A and Investigator B). Data was analysed using a step-by-step thematic analysis method (Braun & Clarke, 2006). Investigators A and B independently analysed the transcripts, identified themes and later reported the common themes. These themes were discussed for concurrence. When any differences in opinion arose, these would be reviewed by investigator C to resolve any disagreement.
C. Setting
The research was conducted within the Paediatric ED in KK Women’s and Children’s Hospital, a tertiary paediatric hospital.
The Children’s Emergency of KK Women’s and Children’s Hospital is the largest paediatric emergency unit in Singapore. During the time of the interviews, the department treated over 400 patients daily. The Children’s Emergency sees all children under the age of 18 years for all medical complaints.
The department is staffed by over 60 junior doctors at a single time. These junior doctors come from various backgrounds and pass through the department for varying amounts of time. Thus, their experience can be very heterogeneous.
The job scope and responsibilities of all the junior doctors are primarily the same despite the different levels of experience. They are expected to treat the patients that present to the ED. These doctors can seek advice from the senior doctors who are on the ground. However, for the majority of the time, they would be tasked to treat patients on their own.
D. Participants
Participants were recruited through an email that was circulated to all junior doctors in the department. Participation in the study was voluntary and participants were not remunerated.
A total of 16 junior doctors were recruited and interviewed over a 1-month period. Due to the busyness of the ED and the limited time frame in which the interviews were conducted, only 16 interviews were conducted. Convenience sampling was chosen for the sampling method. The first 16 volunteers who had volunteered were interviewed. However, it was noted that saturation point was reached prior to the conclusion of the interview process.
The variety within the ED was well represented. The details of participant breakdown are elaborated on in Table 1.
|
Experience & Training Information |
|
|
|
|
|
Mean post-graduate year, 3.6 (2-6)* |
|
|
|
|
|
|
Emergency Medicine |
Family Medicine |
Paediatric Medicine |
Not in a training program at time of study |
|
Training Program (n=16) |
5 |
2 |
1 |
8 |
|
Epidemiological Data |
|
|
|
|
|
|
Chinese |
|
Indian |
|
|
Race (n=16) |
13 |
|
3 |
|
|
|
Male |
|
Female |
|
|
Gender (n=16) |
6 |
|
10 |
|
Table 1: Characteristics of Participants
*Mean (Range)
E. Analysis
All transcripts were reviewed by JT and SG. Coding was done manually using Microsoft Word. During the process, themes were identified and substantiating quotes were recorded. Iterative data analysis was done so that interviewers were aware of themes that were previously mentioned. However, the themes were not specifically explored unless brought up by the subsequent interviews.
III. RESULTS
Through the interviews, we collected information about the experiences within the ED. Interview transcripts collected as a part of this study are openly available on Figshare at http://doi.org./10.6084/m9.figshare.19204761 (Tan et al., 2022). From the interviews conducted, the experience was divided into the initial perceptions and coping mechanisms.
A. Perceptions
The perceptions of the paediatric emergency rotation in the ED were largely contributed by the experiences of the individuals who had previously worked in the department. This was achieved through consultation with friends or colleagues prior to starting the posting to find out more about the rotation.
“Before I started doing the posting, I asked some people who have done or were currently doing the posting…to find out what I was getting myself into”
(P7)
The broad themes elicited about the perceptions and inherent worries of the incoming medical officers were that of being unprepared due to ‘inadequate knowledge’ or ‘unfamiliarity’, as well as the impending ‘work load’ and ‘work factors’.
1) Fear of subject matter: Participants who were not familiar with the paediatric content were worried about their competency and adequacy in treating children. Oftentimes, participants cited that exposure to the paediatric subject matter may have been inadequate or dated and as a result, resulted in fears of being unprepared or being unsafe.
“I’ve not done any paediatric postings before as a doctor so that was a bit worrying.”
(P4)
“I’ve never dealt with paediatrics before so it was quite scary to come onto the posting”
(P14)
In participants who did however have some background in paediatrics, additional fears of specialised emergency knowledge also emerged with participants feeling nervous about the posting.
“Some of the things included technical skills such as doing back slabs, manipulation and reduction, and I guess managing trauma and more complicated acute conditions such as diabetic ketoacidosis and haemophilia and oncological and metabolic related conditions.”
(P11)
“When I started I learnt about resuscitation cases which I felt was a bit nerve-wracking to start with”
(P12)
2) Unfamiliarity: Even though participants may have been at different time points in their careers during the posting, they were all expected to perform mostly the same duties and responsibilities. As a result, a section of the participants cited worries about adjusting to the roles and environment that they may have been new to. These included concerns about being new to the system used. These added to the worries that participants often had about starting a new posting and made participants even more fearful.
“Coming from the UK, this was my first job in Singapore as a MO and thus had close to 0 experience of working in Singapore”
(P8)
“I was also not very familiar with the system. It added to the fear and unpreparedness before starting the posting.”
(P9)
3) Work factors: As a place with high turnover and workload, the picture painted to many of the participants was that it may be difficult to cope with the high workload. This would result in participants being overloaded and overwhelmed. A level of uncertainty was also described. Many participants were left feeling fearful, apprehensive and unsure of what to expect during the upcoming posting. Some were also worried about the expectations they may have to live up to and the nature of the environment being extremely stressful.
“I just heard that it can be quite busy with many patients and at the beginning, it can feel a bit of a throw into the deep end as we often don’t know what to expect and the learning curve can be quite steep”
(P12)
“I was also a bit apprehensive as I heard how busy the posting could get”
(P10)
“It’s quite a stressful working environment because the seniors have a certain working expectation and if you can’t live up to the expectations.”
(P16)
Practically, participants were also worried about the potential to get sufficient rest. Many participants heard that manpower may be tight and would result in having fewer or insufficient off days and would run the risk of feeling tired and burnt out.
“I heard that it was also difficult to get leave that you want and that you would also be really tired during the posting”
(P13)
B. Coping Mechanisms
We then explored the different ways the participants utilised to cope with their experiences in the ED. Participants used a variety of means that we broadly classified into broad themes of ensuring clinical safety, psychosocial support and spirituality.
1) Clinical safety: Participants were inevitably worried about competency and had inherent fears of patient safety in their practice. Coping strategies in this realm could be divided into preparation, senior supervision and collegial opinion.
Preparation was often seen in speaking to doctors who had previously rotated through the posting to allow junior doctors to prepare themselves mentally.
“I asked around and tried to mentally prepare myself for what people told me to expect”
(P3)
In addition, the perceived knowledge gaps and lack of experience were dealt with by many participants through studying and reading up to cover these gaps as well as to prevent them from feeling out of depth.
“I had actually read the guidelines prior especially for the things that I was not familiar with.”
(P10)
On the ground, participants found the availability and approachability of help and support from senior colleagues helpful in easing the worry and anxiety experienced in the emergency department. This also helped participants feel more safe and secure in their practices in the emergency department.
“I appreciate the nice seniors. Most of the seniors are approachable and they treat us like fellow colleagues. They respect our opinions and try to keep it in mind”
(P10)
“I feel very safe at work and very well supported by the seniors. In general, it is easy to ask for help from most of the seniors.”
(P8)
In addition, many participants also felt that their fellow medical officer colleagues were also important in ensuring safety in their practice. With different levels of experience, they could bounce ideas off each other and get a second opinion from their peers. Furthermore, their colleagues also helped to pick up the workload when they felt overwhelmed.
“Everyone is willing to help out when you get stuck. Help is useful and it is easy to come by”
(P1)
“I feel like I have a good relationship with them (peers) and that helps me and I can also get second opinions from them if I’m unsure.”
(P9)
2) Psychosocial support: In the high-strung environment of the emergency department, there is a lot of stress and emotions that come with the job. We found that many participants shared about the social component involved in unpacking these emotions and relieving their stress. The components of the collegial environment and support from loved ones appeared to be crucial coping mechanisms that helped participants.
The work climate was cited to be collegial and relationships between co-colleagues were described as friendly. Many participants felt comfortable with their co-colleagues such that they could ventilate their emotions and experiences with one another. These helped participants process and debrief their experiences.
“We generally laugh about the situation together and it gets better. Sometimes they give advice based on what they have seen and how to avoid such circumstances and we try and help each other.”
(P7)
“It’s useful amongst colleagues because we go through the same things and we get to exchange ideas and I feel we get to debrief this way as well. That helps because we don’t feel like we go through it alone because we have similar experiences.”
(P8)
Apart from the work environment, supportive loved ones and close friends also helped participants cope with difficult days. Participants cited that out of work encounters helped them to get through tough days and relieve their stress.
“Sometimes I also talk about it with someone. Usually that helps and my stress doesn’t usually last beyond the same day.”
(P6)
“I guess these 3 things, my family, friends and colleagues help me with tough days.”
(P7)
3) Spirituality and wellness: Spirituality and wellbeing were also important in dealing with the experiences and stressors the participants faced. Apart from dealing with the clinical stressors and unpacking the experiences with others, participants also spoke about coming to terms with their experiences and emotions on their own. This involved components of religion and reflexivity. Participants also spoke about the role of maintaining their wellbeing with leisure and self-care activities.
Participants spoke about reflecting and reviewing the good as well as the bad moments at work. These helped the participants make sense of their experiences and as a result, helped them improve and learn.
“I usually pray and reflect on my day and think about what are the good points I can get out of the day.”
(P9)
Religion also featured as a means of coping with emotions in the sometimes chaotic environment seen in the ED. These helped participants work better and feel more focused at work.
“I feel like I’m stable when I pray … and I think more thoughts are more ordered. That helps me.”
(P15)
Focusing on physical wellbeing also helped to reduce the stress experienced. Participants cited different activities – food, sleep, exercise, self-care and hobbies that helped them take their minds off work and help them get rejuvenated before the next working day.
“Eating and relaxing help me after a tough day”
(P4)
“I find exercising is helpful, and it helps me feel fresher and less sleepy”
(P3)
“Listening to music and watching videos and just going about non-work related normal daily life.”
(P11)
“I ensure that I have a good work-life balance… I go for a massage, go for a buffet, watch a movie and enjoy myself.”
(P13)
“I draw, I paint. I learn languages. Sometimes I travel. These things help me relax and cope with stress.”
(P16)
IV. DISCUSSION
We sought to understand the perceptions of junior doctors starting out in the emergency department as well as the subsequent coping strategies they undertook for challenges that they faced. During the process, we interviewed sixteen junior doctors who spoke in detail about their experiences.
The perceptions that the junior doctors in our study described consisted mainly of their worries and concerns prior to the start of the posting. Most of the perceptions and worries were centred on knowledge, workload and responsibilities that came with the posting.
A large proportion of participants expressed worry regarding competency and personal comfort levels in managing children. As the ED is a broad one and knowledge is inexhaustible, the concerns in lack of competency are seen in the other elements of emergency care and not strictly paediatric emergency (Jelinek et al., 2013; Kennelly et al., 2012; Yong & Ng, 2016).
Many of the worries described by the participants were of an anticipatory nature, from hearing their predecessors’ experiences. Anticipation of negative experiences can lead to anxiety and stress in individuals (Carlson et al., 2010; Grupe & Nitschke, 2013). Participants had anxiety about the workload and certain work factors prior to the start of the posting. While predecessors’ recounts are helpful in preparing doctors for their upcoming experience, the anxiety that comes with this preparation may not be. Positive effects can also be seen when a positive picture is painted of the upcoming experience (Gangwal et al., 2014; Luo et al., 2018). As it is difficult to balance the negative anxiety and the positive effects of preparation, it may be helpful for junior doctors to receive a formal handover from existing doctors who themselves have had a positive experience so as to prevent excessive anxiety.
We next explored the coping strategies involved to help the participants through the difficult parts of their experiences.
In areas of safety, participants commented on how the support from the senior staff helped allay their fears and increase patient safety at work. Other studies showed similar themes with HCWs expressing the desire for support, professional help and preventive action in the ED (Mikkola et al., 2019; Povedano-Jimenez et al., 2020; Ruotsalainen et al., 2015). In situations where support was provided, these corresponded to higher levels of satisfaction at work (Hunsaker et al., 2015). This is especially so in HCWs who were exposed to traumatic situations (Zhao et al., 2015).
Social support is an important factor in dealing with stressful situations (Gribben et al., 2019). In our cohort, our participants also engaged in social interactions with family, friends and colleagues in an attempt to deal with stressors in the ED. The collegial environment was also beneficial in dealing with stress and helping participants better process their experiences (Povedano-Jimenez et al., 2020).
Apart from expressing emotions and stressors, participants also sought to ensure mental and physical wellness of oneself. This was done by focusing on their spirituality as well as physical wellness and self-care. These strategies utilised were similar to those seen in other studies (Gribben et al., 2019; Hoonpongsimanont et al., 2013; McPherson et al., 2003; Palmer Kelly et al., 2020; Xu et al., 2019).
Maladaptive coping strategies did not come up as a main theme in our interviews.
A. Limitations
The study was conducted in a single ED at a single time point. Efforts were taken to diversify the population interviewed with participants experiencing different durations within the department. However, interviews of participants who had experienced the ED at different time points could have brought about different views and themes.
The primary investigator was also working within the same department during the time of the study. As the investigator was also a junior doctor during the study, a power dynamic effect was minimised.
The setting was limited to a single centre in the Singapore setting and thus, was extremely specific. Singapore is a city-state with easy access to healthcare. In addition, due to strict legislation, violence is minimal compared to other areas. As such, the patient load and patient type may differ from other ED and may raise the question of applicability in a different setting.
In addition, this study was conducted prior to the COVID-19 pandemic and the findings were representative of the climate at that time. The pandemic has led to multiple changes in workflow and work culture in the paediatric ED, and these may affect the applicability of our findings.
B. Future Research and Practical Implications
The study is the first qualitative in-depth study looking at perceptions and coping strategies in a paediatric emergency setting among junior doctors in a single centre. It is the first study to explore the individual perceptions and coping mechanisms of doctors, with a focus on the subset of junior doctors. The group was relatively small and conducted at a single time point. As such, the study can be expanded to include a larger group of participants across different time points and centres to illustrate a bigger picture.
Many of the participants also talked about the challenges they experienced in the paediatric emergency. They also raised possible improvements that could be made to help with stressors and challenges in the ED. This could be studied further and future research could focus on how we could target these factors and how effective these adjustments can be.
The findings of this research echoed the findings of prior studies. This study also sheds light and gives us more depth in terms of the early perceptions prior to the start of the postings and the coping strategies that were used.
These findings can also help future doctors rotating through the ED picture the experience. This would give doctors an opportunity to decide how best to prepare themselves. It could also help the doctors feel united with their current colleagues and predecessors in their challenges. And that they are not alone in their experiences.
V. CONCLUSION
In this study, the perceptions of junior doctors and coping strategies of junior doctors in an Asian Paediatric ED were studied. We looked at the perceptions and coping strategies utilised. Many factors were established in contributing to the experience. Improvements and suggestions to improve the experience were also brought up. Other HCWs can also understand how to best work with the junior doctors to facilitate an effective and pleasant working environment.
Notes on Contributors
Jaime Tan undertook literature reviews, conducted and analysed interviews and drafted the manuscript. Junaidah Badron reviewed the interviews and drafted and reviewed the manuscript. Sashikumar Ganapathy conceived the idea of the study, reviewed and analysed interview transcripts and advised the manuscript design. All authors have read and approved the final manuscript.
Ethical Approval
This project was submitted to the Centralised Institutional Review Board for approval (CIRB Ref 2019.2772). All participants consented to the research study.
Data Availability
All data collected in this study are openly available on Figshare repository, http://doi.org/10.6084/m9.figshare.19204761
Acknowledgement
We would like to thank all participants for volunteering their time and agreeing to participate in this study.
Funding
No funding was involved in this study.
Declaration of Interest
The authors declare that they have no conflicts of interest.
References
Abraham, L. J., Thom, O., Greenslade, J. H., Wallis, M., Johnston, A. N., Carlström, E., Mills, D., & Crilly, J. (2018). Morale, stress and coping strategies of staff working in the emergency department: A comparison of two different-sized departments. Emergency Medicine Australasia, 30(3), 375-381. https://doi.org/10.1111/1742-6723.12895
Alomari, A. H., Collison, J., Hunt, L., & Wilson, N. J. (2021). Stressors for emergency department nurses: Insights from a cross‐sectional survey. Journal of Clinical Nursing, 30(7-8), 975-985. https://doi.org10.1111/jocn.15641
Barham, D., De Beer, W., & Clark, H. (2019). The role of professional supervision for palliative care doctors in New Zealand: A quantitative survey of attitudes and experiences. The New Zealand Medical Journal, 132(1501), 10–20.
Basu, S., Yap, C., & Mason, S. (2016). Examining the sources of occupational stress in an emergency department. Occupational Medicine, 66(9), 737–742. https://doi.org/10.1093/occmed/kqw155
Braun, V., & Clarke, V. (2006). Using thematic analysis in psychology. Qualitative Research in Psychology, 3(2), 77-101. https://doi.org/10.1191/1478088706qp063oa
Burbeck, R., Coomber, S., Robinson, S. M., & Todd, C. (2002). Occupational stress in consultants in accident and emergency medicine: A national survey of levels of stress at work. Emergency Medicine Journal, 19(3), 234–238. https://doi.org/10.1136/emj.19.3.234
Carlson, J. M., Greenberg, T., Rubin, D., & Mujica-Parodi, L. R. (2010). Feeling anxious: Anticipatory amygdalo-insular response predicts the feeling of anxious anticipation. Social Cognitive and Affective Neuroscience, 6(1), 74–81. https://doi.org/10.1093/scan/nsq017
Chan, C. Y. W., Sum, M. Y., Lim, W. S., Chew, N. W. M., Samarasekera, D. D., & Sim, K. (2016). Adoption and correlates of Postgraduate Hospital Educational Environment Measure (PHEEM) in the evaluation of learning environments – A systematic review. Medical Teacher, 38(12), 1248–1255. https://doi.org/10.1080/0142159x.2016.1210108
Chew, Q. H., Ang, L. P., Tan, L. L., Chan, H. N., Ong, S. H., Cheng, A., Lai, Y. M., Tan, M. Y., Tor, P. C., Gwee, K. P., & Sim, K. (2019). A cross-sectional study of burnout and its associations with learning environment and learner factors among psychiatry residents within a National Psychiatry Residency Programme. BMJ Open, 9(8), e030619. https://doi.org/10.1136/bmjopen-2019-030619
Copeland, D., & Henry, M. (2018). The relationship between workplace violence, perceptions of safety, and professional quality of life among emergency department staff members in a Level 1 Trauma Centre. International Emergency Nursing, 39, 26–32. https://doi.org/10.1016/j.ienj.2018.01.006
Degen, C., Weigl, M., Glaser, J., Li, J., & Angerer, P. (2014). The impact of training and working conditions on junior doctors’ intention to leave clinical practice. BMC Medical Education, 14(1). https://doi.org/10.1186/1472-6920-14-119
Durand, A. C., Bompard, C., Sportiello, J., Michelet, P., & Gentile, S. (2019). Stress and burnout among professionals working in the emergency department in a French university hospital: Prevalence and associated factors. Work, 63(1), 57–67. https://doi.org/10.3233/wor-192908
Ganapathy, S., Lim, S. Y., Kua, J. P., & Ng, K. C. (2015). Non-urgent paediatric emergency department visits: Why are they so common? A Singapore perspective. Annals of the Academy of Medicine, Singapore, 44(7), 269–271. https://doi.org/10.47102/annals-acadmedsg.v44n7p269
Gangwal, R. R., Rameshchandra Badjatia, S., & Harish Dave, B. (2014). Effect of exposure to positive images of dentistry on dental anxiety among 7 to 12 years old children. International Journal of Clinical Pediatric Dentistry, 7(3), 176–179. https://doi.org/10.5005/jp-journals-10005-1260
Greenslade, J. H., Wallis, M., Johnston, A. N. B., Carlström, E., Wilhelms, D. B., & Crilly, J. (2019). Key occupational stressors in the ED: an international comparison. Emergency Medicine Journal, 37(2), 106–111. https://doi.org/10.1136/emermed-2018-208390
Gribben, J. L., Kase, S. M., Waldman, E. D., & Weintraub, A. S. (2019). A cross-sectional analysis of compassion fatigue, burnout, and compassion satisfaction in paediatric critical care physicians in the United States*. Paediatric Critical Care Medicine, 20(3), 213–222. https://doi.org/10.1097/pcc.0000000000001803
Grupe, D. W., & Nitschke, J. B. (2013). Uncertainty and anticipation in anxiety: An integrated neurobiological and psychological perspective. Nature Reviews Neuroscience, 14(7), 488–501. https://doi.org/10.1038/nrn3524
Guise, J. M., Hansen, M., O’Brien, K., Dickinson, C., Meckler, G., Engle, P., Lambert, W., & Jui, J. (2017). Emergency medical services responders’ perceptions of the effect of stress and anxiety on patient safety in the out-of-hospital emergency care of children: A qualitative study. BMJ Open, 7(2), e014057. https://doi.org/10.1136/bmjopen-2016-014057
Healy, S., & Tyrrell, M. (2011). Stress in emergency departments: Experiences of nurses and doctors. Emergency Nurse, 19(4), 31–37. https://doi.org/10.7748/en2011.07.19.4.31.c8611
Hoonpongsimanont, W., Murphy, M., Kim, C. H., Nasir, D., & Compton, S. (2013). Emergency medicine resident well-being: Stress and satisfaction. Occupational Medicine, 64(1), 45–48. https://doi.org/10.1093/occmed/kqt139
Howlett, M., Doody, K., Murray, J., LeBlanc-Duchin, D., Fraser, J., & Atkinson, P. (2015). Burnout in emergency department healthcare professionals is associated with coping style: A cross-sectional survey. Emergency Medicine Journal, 32(9), 722–727. https://doi.org/10.1136/emermed-2014-203750
Hunsaker, S., Chen, H. C., Maughan, D., & Heaston, S. (2015). Factors that influence the development of compassion fatigue, burnout, and compassion satisfaction in emergency department nurses. Journal of Nursing Scholarship, 47(2), 186–194. https://doi.org/10.1111/jnu.12122
Jackson, E. R., Shanafelt, T. D., Hasan, O., Satele, D. V., & Dyrbye, L. N. (2016). Burnout and alcohol abuse/dependence among U.S. medical students. Academic Medicine, 91(9), 1251–1256. https://doi.org/10.1097/acm.0000000000001138
Jelinek, G. A., Weiland, T. J., Mackinlay, C., Gerdtz, M., & Hill, N. (2013). Knowledge and confidence of Australian emergency department clinicians in managing patients with mental health-related presentations: Findings from a national qualitative study. International Journal of Emergency Medicine, 6, Article 2. https://doi.org/10.1186/1865-1380-6-2
Kennelly, S. P., Morley, D., Coughlan, T., Collins, R., Rochford, M., & O’Neill, D. (2012). Knowledge, skills and attitudes of doctors towards assessing cognition in older patients in the emergency department. Postgraduate Medical Journal, 89(1049), 137–141. https://doi.org/10.1136/postgradmedj-2012-131226
Koh, M. Y. H., Chong, P. H., Neo, P. S. H., Ong, Y. J., Yong, W. C., Ong, W. Y., Shen, M. L. J., & Hum, A. Y. M. (2015). Burnout, psychological morbidity and use of coping mechanisms among palliative care practitioners: A multi-centre cross-sectional study. Palliative Medicine, 29(7), 633–642. https://doi.org/10.1177/0269216315575850
Luo, Y., Chen, X., Qi, S., You, X., & Huang, X. (2018). Well-being and anticipation for future positive events: Evidences from an fMRI Study. Frontiers in Psychology, 8. https://doi.org/10.3389/fpsyg.2017.02199
Mason, S., O’Keeffe, C., Carter, A., & Stride, C. (2015). A longitudinal study of well-being, confidence and competence in junior doctors and the impact of emergency medicine placements. Emergency Medicine Journal, 33(2), 91–98. https://doi.org/10.1136/emermed-2014-204514
McPherson, S., Hale, R., Richardson, P., & Obholzer, A. (2003). Stress and coping in accident and emergency senior house officers. Emergency Medicine Journal, 20(3), 230–231. https://doi.org/10.1136/emj.20.3.230
Mikkola, R., Huhtala, H., & Paavilainen, E. (2019). Development of a coping model for work‐related fear among staff working in emergency department in Finland – Study for nursing and medical staff. Scandinavian Journal of Caring Sciences, 33(3), 651–660. https://doi.org/10.1111/scs.12658
Neubauer, B. E., Witkop, C. T., & Varpio, L. (2019). How phenomenology can help us learn from the experiences of others. Perspectives on Medical Education, 8(2), 90–97. https://doi.org/10.1007/s40037-019-0509-2
Oreskovich, M. R., Shanafelt, T., Dyrbye, L. N., Tan, L., Sotile, W., Satele, D., West, C. P., Sloan, J., & Boone, S. (2015). The prevalence of substance use disorders in American physicians. The American Journal on Addictions, 24(1), 30–38. https://doi.org/10.1111/ajad.12173
Palmer Kelly, E., Hyer, M., Payne, N., & Pawlik, T. M. (2020). A mixed-methods approach to understanding the role of religion and spirituality in healthcare provider well-being. Psychology of Religion and Spirituality, 12(4), 487–493. https://doi.org/10.1037/rel0000297
Pek, J. H., Ong, Y. K. G., Quek, E. C. S., Feng, X. Y. J., Allen, J. C., Jr., & Chong, S. L. (2019). Evaluation of the criteria for trauma activation in the paediatric emergency department. Emergency Medicine Journal, 36(9), 529–534. https://doi.org/10.1136/emermed-2018-207857
Povedano-Jimenez, M., Granados-Gamez, G., & Garcia-Caro, M. P. (2020). Work environment factors in coping with patient death among Spanish nurses: A cross-sectional survey. Revista Latino-Americana de Enfermagem, 28. https://doi.org/10.1590/1518-8345.3279.3234
Ruotsalainen, J., Verbeek, J., Mariné, A., & Serra, C. (2015). Preventing occupational stress in healthcare workers. Cochrane Database of Systematic Reviews, 2015(4), CD002892. https://doi.org/10.1002/14651858.cd002892.pub5
Ryali, V. S. R., Sreelatha, P., & Premlal, L. (2018). Burnout and coping strategies among residents of a private medical college in South India: A cross-sectional study. Industrial Psychiatry Journal, 27(2), 213-218. https://doi.org/10.4103/ipj.ipj_53_18
Shanafelt, T. D., Boone, S., Tan, L., Dyrbye, L. N., Sotile, W., Satele, D., West, C. P., Sloan, J., & Oreskovich, M. R. (2012). Burnout and satisfaction with work-life balance among US physicians relative to the general US population. Archives of Internal Medicine, 172(18), 1377-1385. https://doi.org/10.1001/archinternmed.2012.3199
Smith, D. W. (2021). Stanford Encyclopaedia of Philosophy. https://plato.stanford.edu.
Sum, M. Y., Chew, Q. H., & Sim, K. (2019). Perceptions of the learning environment on the relationship between stress and burnout for residents in an ACGME-I accredited national psychiatry residency program. Journal of Graduate Medical Education, 11(4s), 85–90. https://doi.org/10.4300/jgme-d-18-00795
Talih, F., Daher, M., Daou, D., & Ajaltouni, J. (2018). Examining burnout, depression, and attitudes regarding drug use among Lebanese medical students during the 4 years of medical school. Academic Psychiatry, 42(2), 288–296. https://doi.org/10.1007/s40596-017-0879-x
Tan, M. Y., Ng, N. B. H., Aw, M. M., & Lin, J. B. (2022). Perceived stress & sentiments of housemen starting work during the COVID-19 Pandemic in Singapore. The Asia Pacific Scholar, 7(2), 56–60. https://doi.org/10.29060/taps.2022-7-2/sc2686
Tuffour, I. (2017). A critical overview of interpretative phenomenological analysis: A contemporary qualitative research approach. Journal of Healthcare Communications, 2(4). https://doi.org/10.4172/2472-1654.10009
Watson, A. G., Saggar, V., MacDowell, C., & McCoy, J. V. (2019). Self-reported modifying effects of resilience factors on perceptions of workload, patient outcomes, and burnout in physician-attendees of an international emergency medicine conference. Psychology, Health & Medicine, 24(10), 1220–1234. https://doi.org/10.1080/13548506.2019.1619785
Xu, H. G., Johnston, A. N., Greenslade, J. H., Wallis, M., Elder, E., Abraham, L., Thom, O., Carlström, E., & Crilly, J. (2019). Stressors and coping strategies of emergency department nurses and doctors: A cross-sectional study. Australasian Emergency Care, 22(3), 180–186. https://doi.org/10.1016/j.auec.2018.10.005
Yong, A. M. Y., & Ng, J. (2016). Assessing the level of knowledge of emergency department physicians in recognition of common skin lesions. Annals of Clinical and Laboratory Research, 4(1). https://doi.org/10.21767/2386-5180.100073
Zhao, S., Liu, H., Ma, H., Jiao, M., Li, Y., Hao, Y., Sun, Y., Gao, L., Hong, S., Kang, Z., Wu, Q., & Qiao, H. (2015). Coping with Workplace Violence in Healthcare Settings: Social Support and Strategies. International Journal of Environmental Research and Public Health, 12(11), 14429–14444. https://doi.org/10.3390/ijerph121114429
*Jaime Maria Tan
KK Women’s and Children’s Hospital,
100 Bukit Timah Road,
Singapore 229899
+6590303124
Email: jaime.tan@mohh.com.sg
Submitted: 19 May 2022
Accepted: 21 September 2022
Published online: 3 January, TAPS 2023, 8(1), 3-12
https://doi.org/10.29060/TAPS.2023-8-1/OA2817
Junji Haruta1,2, Ayumi Takayashiki2, Ryohei Goto2, Takami Maeno2, Sachiko Ozone2 & Tetsuhiro Maeno2
1Medical Education Center, School of Medicine, Keio University, Japan; 2Department of Primary Care and Medical Education, Faculty of Medicine, University of Tsukuba, Tsukuba, Japan
Abstract
Introduction: The pandemic caused by the novel coronavirus (COVID-19) has produced dramatic changes in the learning environment for clinical practice in medical education, and the impact on medical students has been significant. However, few program evaluation studies involving professional identity, now emphasised in medical education, have compared current with pre-COVID-19 programs. Here, we compared the professional identity recognised by medical students in the years before and during COVID-19.
Methods: Medical students who participated in clinical practice were evaluated using the Japanese version of the Professional Self-Identity Questionnaire (PSIQ), a 9-item inventory rated using 7-point Likert scales. They answered on the first day of a 4-week clinical practice module within a community-based medical education (CBME) program and at graduation in 2018-2019 (pre-COVID-19 pandemic) and in 2019-2020 (during-COVID-19 pandemic). We compared the mean difference in total PSIQ score of the 2019-2020 students to those of the 2018-2019 students as a historical cohort using an unpaired t-test.
Results: Participants were 104 medical students in the 2018-2019 academic year and 92 in the 2019-2020 academic year. PSIQ was increased at graduation. Mean difference in total PSIQ score was statistically higher for the 2019-2020 students (13.5 ± 9.4) than for the 2018-2019 students (10.3 ± 8.1) (t =2.6, df =195, p = 0.01).
Conclusion: Although clinical practice was restricted by COVID-19, this had some positive impact on the strengthening of professional identity recognised by medical students. This finding may have been influenced by the imprinting of professional norms and changes in society.
Keywords: Novel Coronavirus Infection, Professional Identity, Clinical Practice, Questionnaire Survey, Program Evaluation
Practice Highlights
- Professional identity recognised by medical students in Japan was assessed by questionnaire.
- Changes during clinical practice were compared between two grades using a historical cohort.
- Medical students’ recognised professional identity scores improved after one year in both cohorts.
- Medical students experienced the COVID-19 pandemic showed some positive impact on professional identity.
- Medical students internalised their role as healthcare professionals owing to COVID-19 pandemic.
I. INTRODUCTION
The pandemic caused by the novel coronavirus (COVID-19) has caused unprecedented disruption to medical education systems around the world (Kaul et al., 2021; Khasawneh et al., 2020; Lucey & Johnston, 2020; Papapanou et al., 2021). In particular, the pandemic has made it difficult to continue medical educational programs, including regular lectures, and face-to-face lectures, experiments, and clinical practice involving patients (Al Samaraee, 2020; Emanuel, 2020; Shankar & Wilson, 2020). The Association of American Medical Colleges took the unprecedented decision to suspend clinical practice and issued guidance instructing medical students to avoid clinical practice involving direct patient contact (Association of American Medical Colleges, 2020). The many university hospitals in the U.S. have made it a priority to utilise students in controlling the spread of COVID-19 infection. Other countries followed this precedent. Medical students accordingly lost the opportunity to learn through patients in clinical practice. In Japan also, clinical practice was suspended at many universities.
Commonly implemented alternative teaching methods were online interactive discussions and video lectures (Chiodini, 2020; Mian & Khan, 2020). To prevent the spread of COVID-19 from medical students in clinical practice (Alsoghair et al., 2021), students were required to socially distance not only from patients but also from healthcare providers and faculty members. However, implementing the requisite changes to curricula, such as interrupting or drastically postponing clinical practice, was difficult, forcing faculties to develop curricula that provided students with opportunities to supplement their ongoing clinical practice as early as possible, while making use of online devices (Ross, 2020). These changes in the learning environment affected medical students’ learning. For example, a survey of 2nd-6th grade students at the University of Geneva found that 2/3 of the medical students experienced decreased motivation and concentration in distracting learning environments such as home, whereas some medical students who were exposed to clinical practice during the COVID-19 pandemic showed an increased sense of belonging to the profession (Wurth et al., 2022). A change in perception with remote learning in response to the COVID-19 pandemic among Canadian undergraduate students also revealed a significant decrease in students’ achievement goals, engagement, and perceptions of success, and an increase in perceptions of cheating (Daniels et al., 2021). Perceptions of learning due to changes in the curriculum due to COVID-19 have been investigated and controversially reported, but few reports have investigated professional identity as a foundation for becoming a physician.
To be effective clinicians, it is important that medical students acquire not only knowledge and skills but also professional identity formation (Cruess et al., 2014; Hafferty & Franks, 1994). Professional identity is defined as “attitudes, values, knowledge, beliefs, and skills shared with others in a professional group” (Crossley & Vivekananda-Schmidt, 2009). Professional identity formation is noted as an ongoing process influenced by several factors, including practice experience and professional socialisation (Adams et al., 2006). In this study, we adopted a theoretical framework which is based on a concept that illustrates the interplay of professional identity formation and socialisation through a complex conscious and unconscious process centered on role models, mentors, and the accumulation of individual experiences (Cruess et al., 2015). Because clinical practice is a period in which medical students meet role models and mentors and gain their first experiences as a healthcare provider, clinical practice is major contributor to the development of professional identity in medical students (Haruta et al., 2020).
Although studies have reported that medical education programs altered by the COVID-19 pandemic have affected medical students’ perceptions of the role of the physician and their learning strategies (Findyartini et al., 2020; Wurth et al., 2022), little is known about the influence of curricula changes on medical students with regard to their professional identity formation as physicians affected by role models, mentors, and individual experience (Stetson et al., 2020).
Here, we aimed to compare professional identity as a physician as perceived by medical students in clinical practice before and during COVID-19 using the Professional Self Identity Questionnaire (PSIQ).
II. METHODS
A. Setting
Japan first faced the challenge of the COVID-19 pandemic in January 2020, and a state of emergency was declared for all regions of Japan on April 16, 2020 (Prime Minister’s Office of Japan, 2020). During that time, some medical universities suspended clinical training and implemented online education instead. The COVID-19 Outline of Measures for COVID-19 formulated by the Japanese Ministry of Education, Culture, Sports, Science and Technology was sent to all higher education institutions, including medical schools, on June 5, 2020 (Hayashi et al., 2022), with the main advice that universities should operate in a resilient manner for experiential educational practices such as clinical practice. Under these circumstances, leaders of Japanese medical schools were asked to consult various stakeholders and make decisions on whether or not to continue clinical practice, often leaving detailed instructions to local operations managers in each field (Hayashi et al., 2022). In contrast, primary care physicians were forced to adapt to local conditions (Haruta et al., 2021).
Students enter medical school in Japan after graduating from high school, and the curriculum is six years long. Clinical training usually takes place in the fourth to sixth years. This schedule is also implemented at the University of Tsukuba in Japan: clinical training is divided into a first half from October of the fourth year to September of the fifth year and a second half from October of the fifth year to June of the sixth year, for a total of 78 weeks. After clinical training, medical students spend time studying for graduation and national exams, in addition to attending lectures.
The first phase of this clinical practice consists of a four-week rotation in basic departments such as internal medicine, surgery, obstetrics and gynecology, pediatrics, and emergency medicine, mainly at affiliated hospitals. The second phase incorporates some elective subjects and includes 4 weeks’ mandatory clinical practice in a CBME curriculum and a further 4 weeks’ clinical practice in a department of interest. Typically, 15 to 17 students rotate every 4 weeks through clinical practice in the CBME curriculum. This clinical training was conducted before the pandemic, but was discontinued in response to it at the end of March 2020. In March, medical students continued clinical training while all elementary and junior high schools were closed. All clinical training was then cancelled in April 2020 and replaced with report assignments only. These were replaced in May and June with online training and on-demand assignments. Sixth-year students in the class of 2020, and subsequently also in 2021 and 2022, were required to adhere to health observation recording and infection prevention behaviors in accordance with the University of Tsukuba Hospital staff behavior guidelines, which had not been previously followed. Similarly, they were also restricted from participating in training hospital tours and extracurricular activities, which were usually a part of their training.
B. Study Design
Training in clinical practice at the University of Tsukuba consists of a first phase for 4th and 5th year students and a second phase for 5th and 6th year students. CBME is included in the latter phase. Data from 5th-year medical students who participated in clinical practice in a 4-week community-based medical education (CBME) program from October 2019 to March 2020 and who graduated in March 2021 were compared to those of the previous year’s students (2018-2019) as a historical cohort. This cohort included 6th-year medical students who graduated in March 2020 and who had participated in a similar clinical practice program the previous year, from October 2018 to May 2019. As in the 2018-2019 academic year, a questionnaire was administered using the PSIQ in the 2019-2020 academic year. The PSIQ, conducted as part of program evaluation of the CBME program, was administered on the first day of the 4-week clinical practice of the program and at graduation. Study participants included 118 fifth- and sixth-year medical students who participated in clinical practice in the CBME program from October 2018 to May 2019 (pre-COVID-19 pandemic) and 100 fifth- and sixth-year medical students who participated from October 2019 to March 2020 (during-COVID-19 pandemic). The 35 participants from April-May 2020, when the 4-week clinical practice in the CBME program was switched to online practice due to COVID-19, were excluded because they could not be pre-evaluated.
C. Instrument: Japanese Version of the Professional Self Identity Questionnaire (PSIQ)
The Professional Self-Identity Questionnaire (PSIQ) is a 9-item inventory which is rated using 7-point Likert scales (Crossley & Vivekananda-Schmidt, 2009). This instrument measures the sense of students in identifying their current position on a continuum between ‘first-day student’ and ‘qualified doctor’ when engaged in each of nine domains of professional activity. These nine domains include “Teamwork,” “Communication,” “Conducting assessment,” “Cultural awareness,” “Ethical awareness,” “Using records,” “Dealing with emergencies,” “Reflection,” and “Teaching”. Each item is rated on a 7-point Likert scale. For this research, we set 1 point as “equivalent to the first day of clinical practice” and 7 points as “equivalent to the first day of initial residency”. The PSIQ is an assessment sheet form originally designed in English. The original study was validated in a sample of 496 medical students across multiple phases of education, and the overall internal reliability (Cronbach’s alpha) was reported to be 0.93 (Crossley & Vivekananda-Schmidt, 2009). Previously, we developed a Japanese version of the PSIQ and operationally defined PSIQ scores as professional identity as a physician as perceived by medical students. Cronbach’s alpha of the Japanese PSIQ was reported to be 0.93 (Haruta et al., 2021), which allows students to measure changes in their own professional identity by tracking each of the nine professional activities over time. We set the total score on this scale as the main outcome of this study. The study showed that this was a reliable and valid tool for program evaluation during clinical practice (Haruta et al., 2021).
D. Participants and Data Collection
In 2018-2019 (pre-COVID-19 pandemic) and 2019-2020 (during-COVID-19 pandemic), we assessed the professional identity of medical students from October of their fifth year to May of the sixth year using PSIQ. The survey was administered on the first day of clinical practice in the CBME program as PSIQ 1 (September 2018 to May 2019 and September 2019 to March 2020) and at graduation as PSIQ 2 (2020 January, and January 2021) (Figure 1).
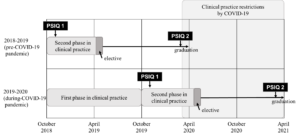
Figure 1. Timing in clinical practice and the PSIQ in 2018-2019 and 2019-2020
On the first day of clinical practice in the CBME program, the authors (JH, TaM, AT) explained the purpose of the study to the students. The authors informed the students that the study would be undertaken as a program evaluation and research, and that their grades would not be influenced in case they did not agree to participate. Those students who agreed to participate signed a consent form giving permission to use their data. Subsequently, the authors asked medical students to fill out the PSIQ as a paper-based, self-administered questionnaire, and to include their student ID number. At graduation, all medical students completed the PSIQ on the internet or on paper as a self-administered questionnaire, again with their student ID number. The study was approved by the Ethics Committee of the University of Tsukuba (No. 1329).
E. Data Analysis
To evaluate the differences in total PSIQ and scores for each item between the first day of clinical practice in the CBME program and the time of graduation, effect sizes (Cohen’s d) were determined for the total PSIQ and scores for each item. In addition, the Shapiro-Wilk test was performed to determine data distribution. For comparison of means for the difference in total PSIQ between 2018-2019 and 2019-2020, an unpaired t-test was applied. The Shapiro-Wilk test confirmed that data distribution for both PSIQ 1 and 2 were not normal. However, since the distribution of PSIQ 2-1 was consistent with normality, a t-test was employed. Missing values were excluded. Data analysis was conducted using SPSS ver. 26 with significance set at the p<0.05 level for total scores as the primary outcome of the PSIQ. Additionally, to deal with the possibility of multiplicity in the simultaneous assessment of each item score, significance levels were Bonferroni corrected, with p< 0.005 (Lee & Lee, 2018).
III. RESULTS
As shown in Table 1, participants analysed in the 2018-2019 academic year (pre-COVID-19 pandemic) included 104 medical students (response rate: 88.1%) who responded at both time points (first day of clinical practice in the CBME program and at graduation), 33 of whom were female. In the 2019-2020 academic year (during-COVID-19 pandemic), 92 medical students (response rate: 92.0%) who responded at both time points were included, 33 of whom were female. One student who did not give consent to have their data used in this study was excluded.
|
2018-2019 (pre-COVID-19 pandemic) |
2019-2020 (during-COVID-19 pandemic) (n=92) |
|
|
Age, mean ± standard deviation |
20.6±1.5 |
21.2±3.4 |
|
Gender, number of persons (%) |
||
|
Male |
66 (63.5) |
51 (55.4) |
|
Female |
33 (31.7) |
33 (35.9) |
|
Unknown |
5 (4.8) |
8 (8.7) |
Table 1. Characteristics of medical students included in the analysis
Table 2 shows that the means of total PSIQ scores and each PSIQ item for 2018-2019 and 2019-2020 were increased at graduation. A comparison of the mean for the difference using the unpaired t-test in total PSIQ score for 2018-2019 and 2019-2020 revealed that it was statistically higher for the 2019-2020 students (13.5 ± 9.4) than for the 2018-2019 students (10.3 ± 8.1) (t =2.6, df =195, p = 0.01). However, there were no statistically significant differences using the unpaired t-test with Bonferronni correction at a 0.005 level of significance in mean scores for 9 items of the PSIQ, namely “Teamwork” (t=0.96 df=195, p=0.341), “Communication” (t=1.84, df=195, p=0.068), “Conducting assessment” (t=2.31, df=195, p=0.24) “Cultural awareness” (t=1.41, df=195, p=0.022), “Ethical awareness” (t=2.25, df=195, p=0.161), “Using records” (t=2.67, df=195, p=0.026), “Dealing with emergencies” (t=2.33, df=195, p=0.008), “Reflection” (t=2.32, df=195, p=0.021) and “Teaching” (t=2.19, df=195, p=0.030). The effect size (Cohen’s d) for total PSIQ scores from the first day of clinical practice in the CBME program to graduation was Δ1.3 in 2018-2019 and Δ1.4 in 2019-2020. The effect size (Cohen’s d) for each item of the PSIQ was Δ1.4 in 2018-2019. Range for items was Δ0.8-1.1 in 2018-2019 and Δ0.9-1.2 in 2019-2020.
|
|
Fiscal year (usually April 1 to March 31) |
First day of the CBME program (1) |
At graduation (2) |
Mean difference in PSIQ (2)-(1) |
t score |
Df |
p-value |
Cohen’s d |
|
Total score (Main outcome) |
2018-2019 (pre-COVID-19 pandemic) |
28.5±7.6 |
38.8±8.5 |
10.3±8.1 |
2.60 |
195 |
0.01 |
1.3 |
|
2019-2020 (during-COVID-19 pandemic) |
28.0±6.6 |
41.6±9.2 |
13.5±9.4 |
1.4 |
||||
|
Sub-analysis |
|
|
||||||
|
Teamwork |
2018-2019 |
3.0±1.2 |
4.4±1.0 |
1.4±1.2 |
0.96 |
195 |
0.341 |
1.1 |
|
2019-2020 |
3.0±1.1 |
4.6±1.1 |
1.6±1.3 |
1.2 |
||||
|
Communication |
2018-2019 |
3.7±1.1 |
4.7±1.1 |
1.0±1.2 |
1.84 |
195 |
0.068 |
0.8 |
|
2019-2020 |
3.5±1.1 |
4.9±1.1 |
1.4±1.3 |
1 |
||||
|
Conducting assessment |
2018-2019 |
3.2±1.0 |
4.4±1.1 |
1.2±1.2 |
2.27 |
195 |
0.024 |
1 |
|
2019-2020 |
3.1±1.0 |
4.7±1.1 |
1.6±1.3 |
1.2 |
||||
|
Cultural awareness |
2018-2019 |
2.9±1.1 |
4.2±1.3 |
1.3±1.3 |
2.31 |
195 |
0.022 |
1 |
|
2019-2020 |
2.8±1.1 |
4.5±1.3 |
1.8±1.5 |
1.2 |
||||
|
Ethics awareness |
2018-2019 |
3.4±1.2 |
4.5±1.1 |
1.1±1.3 |
1.41 |
195 |
0.161 |
0.9 |
|
2019-2020 |
3.5±1.2 |
4.9±1.1 |
1.4±1.4 |
1 |
||||
|
Using record entries |
2018-2019 |
3.4±1.0 |
4.5±1.1 |
1.0±1.1 |
2.25 |
195 |
0.026 |
0.9 |
|
2019-2020 |
3.4±0.9 |
4.8±1.1 |
1.4±1.3 |
1.1 |
||||
|
Dealing with emergencies |
2018-2019 |
2.5±1.1 |
3.8±1.3 |
1.3±1.2 |
2.67 |
195 |
0.008 |
1.1 |
|
2019-2020 |
2.3±1.2 |
4.1±1.4 |
1.9±1.7 |
1.1 |
||||
|
Reflection |
2018-2019 |
3.3±1.1 |
4.3±1.1 |
1.0±1.3 |
2.32 |
195 |
0.021 |
0.8 |
|
2019-2020 |
3.2±0.9 |
4.6±1.3 |
1.4±1.5 |
1 |
||||
|
Teaching |
2018-2019 |
3.1±0.9 |
4.1±1.1 |
0.9±1.1 |
2.19 |
195 |
0. 030 |
0.8 |
|
2019-2020 |
3.2±1.0 |
4.5±1.2 |
1.3±1.4 |
1 |
Table 2. Unpaired t-test analysis and effect sizes for the Professional Identity Self-Assessment Form
IV. DISCUSSION
We found that the means of total and each PSIQ score of medical students who graduated during the COVID-19 pandemic were statistically increased compared to those of students graduating before the pre-COVID-19 pandemic. These findings indicate that, compared with students in the preceding year, the COVID-19 pandemic had a certain positive impact on professional identity formation in medical students with regard to clinical practice.
Considering the framework we used, in which the interaction and reflection of role models, mentors, and individual experiences are key, we believe that all participants were influenced by COVID-19. In addition, professional identity formation is reported to be strongly influenced by environment, context, and other personal variables. (Jarvis-Selinger et al., 2012) The increase in total PSIQ score from the previous year’s medical students may have been due not only to changes in clinical practice, but also to changes in what is expected of medical students by the university hospital and society. In light of these factors, medical students had fewer opportunities to acquire the knowledge and skills required of physicians in the clinical setting directly from role models and mentors, but may nevertheless have been affected by compliance with COVID-19 control measures conducted by the university hospital, and thereby followed the norms of medical professionals communicated through intentional and unintentional messaging. In addition, with the all-engrossing impact of the COVID-19 pandemic throughout society, we speculate that at least some of the students in the COVID-19 group were consulted by family and social contacts as experts and authorities on a daily or more frequent basis, and that such constant reinforcement might also have encouraged PIF. That is, medical students under the COVID-19 pandemic may have internalised the values and norms of the medical professional (Kinnear et al., 2021). Since professional identity formation involves social and relational factors, it is possible that the students’ life and social changes due to COVID-19 reinforced their recognised professional identity (Goldie, 2012).
The more uncertain and ambiguous the period, the more important reflection becomes in PIF. To cope with such uncertainties as the transition from the classroom curriculum to online platforms, rapid changes in the clinical practice environment, and the isolation caused by social distancing, medical students need a well-formed professional identity and socialisation practices (Costello, 2005). Poor PIF is reported to manifest in burnout (Abedini et al., 2018), and depression and anxiety disorders have increased in COVID-19 (Daniels et al., 2021). Since a core component of PIF is the acceptance of uncertainty and ambiguity, medical educators may have provided reflection opportunities for medical students to consciously consider the social factors manifested in COVID-19, such as individual and professional duties, resource priorities, and health disparities, all of which have a positive impact on PIF and socialisation (Stetson et al., 2020). Alternatively, emotion-focused coping strategies (e.g., arts engagement) and problem-solving strategies (e.g., volunteering) to reduce medical students’ anxiety, fear, and stress may be effective (Moula et al., 2022). Students require time and space to reflect on their emergent identity as professionals in these crisis situations (Moula et al., 2022). The extended time for independent learning may have allowed the students to subconsciously reflect on their professional identity, taking seriously the changes in society caused by COVID-19. PIF scores may have accordingly increased in this study.
In general, medical teachers should have made efforts to promote medical students’ professional identity formation even during the COVID-19 pandemic (Goldhamer et al., 2020). Professional identity formation is not a process that should be left to chance; it should be explicitly supported through systematic support and curriculum initiatives (Cruess et al., 2015; Schumacher et al., 2012). In reality, it is necessary to require rapid changes in clinical practice to prevent infection caused by COVID-19, and it has been difficult to promote systematic support for professional identity formation for medical students. However, COVID-19 might not have negatively affected the professional identity recognised by medical students who were in clinical practice immediately after the pandemic. The efforts of Japanese medical educators to implement online and other types of learning to replace clinical practice, and the well-considered efforts of faculty to make clinical practice as feasible as possible may have served as role models or mentors, and influenced medical students’ professional identity formation.
This study has three limitations. First, because there was a difference of 8-17 months between the first day of clinical practice in the CBME program and graduation, given that more clinical practice experience may strengthen the professional identity recognised by medical students, it is possible that differences in clinical practice experience may have affected PSIQ scores. Second, extrapolation from this study should be done with care, since it is a comparison of a one-year questionnaire survey at a single university. Third, a degree of response bias may be present due to the self-reporting design, with inclusion of student ID number. Fourth, evaluation at three or more points may allow a more precise comparison of changes, given that professional identity formation is a dynamic process. Even allowing for these limitations, our findings provide meaningful feedback to medical students and faculty, particularly given the paucity of studies evaluating and comparing changes in professional identity formation – which consists of multiple factors – before and during the COVID-19 pandemic. For the future of medical education, it is imperative to track the professional identity recognised by physicians whose student experience in clinical practice was restricted under the COVID-19 pandemic, and was accordingly significantly changed compared with other years.
V. CONCLUSION
Comparison of the professional identity recognised by medical students whose experience of clinical practice was affected by the COVID-19 pandemic to that of students in the previous year showed some positive impact on professional identity. This lack of negative difference in recognised professional identity even under restricted clinical practice may have been influenced by the imprinting of professional norms and changes in society.
Notes on Contributors
JH, AT, SO, TaM and TeM were involved in the conception and design of this study. JH, AT, and TaM collected the data. JH and RG conducted data analysis. JH mainly wrote the paper. AT, SO, TaM and TeM gave critical feedback on the manuscript. All authors have read and approved the final manuscript.
Ethical Approval
This study was approved by the Ethics Committee of the University of Tsukuba’s Faculty of Medicine and Medical Sciences (No. 1329). All participants have given written consent for their data to be used in the research and for publication.
Data Availability
It is not possible to share data since we did not obtain consent from participants to share all data collected.
Acknowledgement
We thank the faculty staff members Shoji Yokoya, Hisashi Yoshimoto, Shogen Suzuki, Naoto Sakamoto, Yu Yamamoto, Yoshihiro Kataoka, Shoichi Masumoto, Haruka Kuno, Takashi Inaba, Shuhei Hamada, Shogo Kawada, and Sayaka Nin of the Department of Primary Care and Medical Education, Faculty of Medicine, University of Tsukuba. Additionally, we thank the healthcare staff who taught the medical students at the CBME program sites in clinical practice.
Funding
This study was funded by the education/research fund of Department of Primary Care and Medical Education, Faculty of Medicine, University of Tsukuba.
Declaration of Interest
There are no companies or other entities with which the authors have conflict of interest relationships that should be disclosed in relation to the content of the paper.
References
Abedini, N. C., Stack, S. W., Goodman, J. L., & Steinberg, K. P. (2018). “It’s not just time off”: A framework for understanding factors promoting recovery from burnout among internal medicine residents. Journal of Graduate Medical Education, 10(1), 26–32. https://doi.org/10.4300/JGME-D-17-00440.1
Adams, K., Hean, S., Sturgis, P., & Clark, J. M. (2006). Investigating the factors influencing professional identity of first-year health and social care students. Learning in Health and Social Care, 5(2), 55–68. https://doi.org/10.1111/j.1473-6861.2006.00119.x
Al Samaraee, A. (2020). The impact of the COVID-19 pandemic on medical education. British Journal of Hospital Medicine, 81(7), 1-4. https://doi.org/10.12968/HMED.2020.0191
Alsoghair, M., Almazyad, M., Alburaykan, T., Alsultan, A., Alnughaymishi, A., Almazyad, S., Alharbi, M., Alkassas, W., Almadud, A., & Alsuhaibani, M. (2021). Medical Students and COVID-19: Knowledge, preventive behaviors, and risk perception. International Journal of Environmental Research and Public Health, 18(2), 842. https://doi.org/10.3390/ijerph18020842
Association of American Medical Colleges. (2020). Guidance on medical students’ participation in direct in-person patient contact activities. https://www.aamc.org/system/files/2020-08/meded-August-14-Guidance-on-Medical-Students-on-Clinical-Rotations.pdf
Chiodini, J. (2020). Online learning in the time of COVID-19. Travel Medicine and Infectious Disease, 34, Article 101669. https://doi.org/10.1016/j.tmaid.2020.101669
Costello, C. Y. (2005). Professional identity crisis: Race, class, gender, and success at professional schools. Vanderbilt University Press.
Crossley, J., & Vivekananda-Schmidt, P. (2009). The development and evaluation of a professional self identity questionnaire to measure evolving professional self-identity in health and social care students. Medical Teacher, 3(12), e603–e607. https://doi.org/10.3109/01421590903193547
Cruess, R. L., Cruess, S. R., Boudreau, J. D., Snell, L., & Steinert, Y. (2014). Reframing medical education to support professional identity formation. Academic Medicine, 89(11), 1446–1451. https://doi.org/10.1097/ACM.0000000000000427
Cruess, R. L., Cruess, S. R., Boudreau, J. D., Snell, L., & Steinert, Y. (2015). A schematic representation of the professional identity formation and socialization of medical students and residents: A guide for medical educators. Academic Medicine, 90(6), 718–725. https://doi.org/10.1097/ACM.0000000000000700
Emanuel, E. J. (2020). The inevitable reimagining of medical education. JAMA, 323(12), 1127–1128. https://doi.org/10.1001/jama.2020.1227
Findyartini, A., Anggraeni, D., Mikhael Husin, J., & Greviana, N. (2020). Exploring medical students’ professional identity formation through written reflections during the COVID-19 pandemic. Journal of Public Health Research, 9(s1), 1918. https://doi.org/10.4081/jphr.2020.1918
Goldhamer, M. E. J., Pusic, M. V., Co, J. P. T., & Weinstein, D. F. (2020). Can covid catalyze an educational transformation? Competency-based advancement in a crisis. New England Journal of Medicine, 383(11), 1003–1005. https://doi.org/10.1056/NEJMP2018570
Goldie, J. (2012). The formation of professional identity in medical students: Considerations for educators. Medical Teacher, 34(9), e641–e648. https://doi.org/10.3109/0142159X.2012.687476
Hafferty, F. W., & Franks, R. (1994). The hidden curriculum, ethics teaching, and the structure of medical education. Academic Medicine, 69(11), 861–871. https://doi.org/10.1097/00001888-199411000-00001
Haruta, J., Maeno, T., Takayashiki, A., Goto, R., Ozone, S., & Maeno, T. (2021). Validation of the professional self-identity questionnaire for medical students during clinical practice in Japan. International Journal of Medical Education, 12, 160–165. https://doi.org/10.5116/ijme.610d.104b
Haruta, J., Ozone, S., & Hamano, J. (2020). Doctors’ professional identity and socialisation from medical students to staff doctors in Japan: Narrative analysis in qualitative research from a family physician perspective. BMJ Open, 10(7), e035300. https://doi.org/10.1136/bmjopen-2019-035300
Hayashi, M., Saiki, T., Kanter, S. L., & Ho, M. J. (2022). Leaders’ perspectives and actions to manage challenges in medical education presented by the COVID-19 pandemic: A nationwide survey of Japanese medical colleges. BMC Medical Education, 22(1), 144. https://doi.org/10.1186/s12909-022-03193-1
Jarvis-Selinger, S., Pratt, D. D., & Regehr, G. (2012). Competency is not enough: Integrating identity formation into the medical education discourse. Academic Medicine, 87(9), 1185–1190. https://doi.org/10.1097/ACM.0b013e3182604968
Kaul, V., Gallo de Moraes, A., Khateeb, D., Greenstein, Y., Winter, G., Chae, J. M., Stewart, N. H., Qadir, N., & Dangayach, N. S. (2021). Medical education during the COVID-19 pandemic. CHEST, 159(5), 1949–1960. https://doi.org/10.1016/j.chest.2020.12.026
Khasawneh, A. I., Humeidan, A. A., Alsulaiman, J. W., Bloukh, S., Ramadan, M., Al-Shatanawi, T. N., Awad, H. H., Hijazi, W. Y., Al-Kammash, K. R., Obeidat, N., Saleh, T., & Kheirallah, K. A. (2020). Medical students and COVID-19: Knowledge, attitudes, and precautionary measures. A descriptive study from Jordan. Frontiers in Public Health, 8, 253. https://doi.org/10.3389/fpubh.2020.00253
Kinnear, B., Zhou, C., Kinnear, B., Carraccio, C., & Schumacher, D. J. (2021). Professional identity formation during the COVID-19 pandemic. Journal of Hospital Medicine, 16(1), 44–46. https://doi.org/10.12788/jhm.3540
Lee, S., & Lee, D. K. (2018). What is the proper way to apply the multiple comparison test? Korean Journal of Anesthesiology, 71(5), 353-360. https://doi.org/10.4097/KJA.D.18.00242
Lucey, C. R., & Johnston, S. C. (2020). The transformational effects of COVID-19 on medical education. JAMA, 324(11), 1033–1034. https://doi.org/10.1001/jama.2020.14136
Mian, A., & Khan, S. (2020). Medical education during pandemics: A UK perspective. BMC Medicine, 18(1), 100. https://doi.org/10.1186/s12916-020-01577-y
Moula, Z., Horsburgh, J., Scott, K., Rozier-Hope, T., & Kumar, S. (2022). The impact of COVID-19 on professional identity formation: An international qualitative study of medical students’ reflective entries in a global creative competition. BMC Medical Education, 22(1), 545. https://doi.org/10.1186/s12909-022-03595-1
Papapanou, M., Routsi, E., Tsamakis, K., Fotis, L., Marinos, G., Lidoriki, I., Karamanou, M., Papaioannou, T. G., Tsiptsios, D., Smyrnis, N., Rizos, E., & Schizas, D. (2021). Medical education challenges and innovations during COVID-19 pandemic. Postgraduate Medical Journal, 98, 321-327. https://doi.org/10.1136/postgradmedj-2021-140032
Prime Minister’s Office of Japan. (2020). [COVID-19] Declaration of a state of emergency in response to the Novel Coronavirus Disease. https://japan.kantei.go.jp/ongoingtopics/_00020.html
Ross, D. A., & the members of National Neuroscience Curriculum Initiative “Quarantine Curriculum” Committee (2020). Creating a “Quarantine Curriculum” to enhance teaching and learning during the COVID-19 pandemic. Academic Medicine, 95(8), 1125–1126. https://doi.org/10.1097/ACM.0000000000003424
Schumacher, D. J., Slovin, S. R., Riebschleger, M. P., Englander, R., Hicks, P. J., & Carraccio, C. (2012). Perspective: Beyond counting hours: The importance of supervision, professionalism, transitions of care, and workload in residency training. Academic Medicine, 87(7), 883–888. https://doi.org/10.1097/ACM.0b013e318257d57d
Shankar, P. R., & Wilson, I. G. (2020). The COVID-19 pandemic and undergraduate medical student teaching-learning and assessment. Canadian Medical Education Journal, 12(1), e190–e191. https://doi.org/10.36834/cmej.70800
Stetson, G. V., Kryzhanovskaya, I. V., Lomen-Hoerth, C., & Hauer, K. E. (2020). Professional identity formation in disorienting times. Medical Education, 54(8), 765–766. http://doi.org/10.1111/medu.14202
Wurth, S., Sader, J., Cerutti, B., Broers, B., Nadia Bajwa, M., Carballo, S., Escher, M., Galetto-Lacour, A., Grosgurin, O., Lavallard, V., Savoldelli, G., Serratrice, J., Nendaz, M., & Audétat-Voiro, M. C. (2022). Correction to: Medical students’ perceptions and coping strategies during the first wave of the COVID-19 pandemic: Studies, clinical implication, and professional identity. BMC Medical Education, 22(1), Article 232. https://doi.org/10.1186/s12909-022-03307-9
*Junji Haruta
35 Shinanomachi Shinjukuku Tokyo
160-8582, Japan
Email: junharujp@keio.jp
Submitted: 12 May 2022
Accepted: 3 August 2022
Published online: 3 January, TAPS 2023, 8(1), 13-24
https://doi.org/10.29060/TAPS.2023-8-1/OA2810
Audrey Lim1, Vicki Xafis2 & Clare Delany3
1Health and Social Sciences Cluster, Singapore Institute of Technology (SIT), Singapore; 2Graduate School of Humanities and Social Sciences, University of Melbourne, Melbourne, Australia; 3Department of Medical Education, School of Medicine, University of Melbourne, Melbourne, Australia
Abstract
Introduction: Workplace contexts, including political and sociocultural systems influence health professions’ perception and experience of ethical issues. Although established health ethics principles are relevant guiding values, they may be experienced and interpreted differently within different health contexts. How should ethics education account for this? This paper presents ethical dilemmas and concerns encountered by physiotherapists practicing in Singapore and discusses the implications for ethics education.
Methods: Qualitative methods informed by interpretivism and phenomenology were employed. In-depth interviews with 42 physiotherapists from different workplace settings in Singapore were conducted. Participants described everyday ethical challenges they encountered. Inductive content analysis was used to analyse the interview transcript data.
Results: Ethical issues occurred within and across three spheres of ethics: micro, meso and macro. Ethical issues at the micro sphere centered around physiotherapist-patient relationships, interactions with colleagues, and therapists’ feelings of moral distress. In the meso sphere, ethical challenges related to influences arising from the organizational resources or systems. In the macro sphere, ethical challenges developed or were influenced by sociocultural, religious, economic, and political factors.
Conclusion: The findings reflect current literature indicating that context can influence ethical situations, as experienced and perceived by physiotherapists in their unique settings. Such empirical data might inform the development of ethics curricula to ensure that universal ethical principles are situated within the realities of clinical practice. Locally relevant and realistic ethical case studies will better enable students to recognise and address these situations.
Keywords: Ethics, Physiotherapy, Health Professions Education, Ethics Education, Asian Context, Singapore, Healthcare Principles, Health Ethics Principles
Practice Highlights
- Context can influence the ethical situations experienced and interpreted by healthcare professionals.
- Contextualised cases studies need to be developed to make ethics real and relevant to students.
- Ethics education should incorporate local context and not focus only on ethics epistemic knowledge.
- Ethics education should incorporate the dynamic influence of macro, meso and micro factors.
I. INTRODUCTION
The established health ethics principles articulated by Beauchamp and Childress (2001): autonomy, beneficence, non-maleficence, and justice guide healthcare practice, including physiotherapy (Carpenter & Richardson, 2008; Edwards, Delany, et al., 2011). Although these principles were originally proposed as universally relevant and foundational to health ethics, health professionals interpret them differently, depending on their professional and personal background, their values, and the culture of the community and settings in which they work (Fuscaldo et al., 2013). In physiotherapy ethics scholarship, there is growing recognition that the universal nature of principlism as a supporting ethical decision-making framework, may not be a sufficient guide for physiotherapists in their ethical decision-making, because of the plurality of values and diverse contexts of healthcare practice (Carpenter, 2010; Carpenter & Richardson, 2008; Edwards, Wickford, et al., 2011; Fryer et al., 2021; Greenfield, 2006; Hudon et al., 2019; Oyeyemi, 2011; Souri et al., 2020; Sturm et al., 2022). Consequently, there is increasing pedagogical interest in using case studies drawn from everyday practice to bring authenticity and contextual relevance to ethics education (Aguilar-Rodríguez et al., 2019; Fuscaldo et al., 2013).
In physiotherapy, empirical studies have shown that different work contexts, political and sociocultural systems have a direct influence on physiotherapists’ perception and experience of ethical issues (Delany et al., 2018; Fryer et al., 2021; Sturm et al., 2022). A recent example is the study of ethical issues physiotherapists experienced by Sturm et al. (2022). The authors reported physiotherapists working in specific countries described having to compromise their professional integrity due to overt threats and intimidation by suppressive professional organisations or leaders. They were directed to follow the societal or organisational hierarchies or risk jeopardizing their careers. Studies of ethical experiences of physiotherapists practicing in the African nations (Aderibigbe & Chima, 2019; Chigbo et al., 2015; Nyante et al., 2020; Oppong, 2019; Oyeyemi, 2011) and the Greater Middle East region (Edwards, Wickford, et al., 2011; Qamar et al., 2014; Souri et al., 2020) similarly discussed how cultural influences, such as religion or spirituality can directly affect ethical practice and decision-making. Despite increasing empirical evidence globally, the influence of cultural and societal contexts on ethical decision-making and therapists’ interpretation of health values has not been examined in the East and Southeast Asian regions. There has also been little exploration of how societal and cultural context in which physiotherapy is practiced might be used to inform and shape curricula for ethics education.
In this paper, we present data about the ethical situations physiotherapists in Singapore encounter in their everyday clinical practice. Singapore is multi-racial, multi-religious and multi-cultural. The values of Singaporean people are very much rooted in their Asian heritage, with Confucianism as the prevailing social model (Ong, 2020; Tan, 1989; Yang et al., 2006). This research aims to contribute to knowledge about the influence of context on clinical ethical issues and decision-making, as interpreted by physiotherapists in Singapore. The empirical data will then be used to inform subsequent ethics curricula. Identifying and analysing the factors influencing ethical issues, as they are experienced and interpreted by physiotherapists in the Singaporean context, is an important pedagogical strategy to inform the development of health ethics curricula.
II. METHODS
We used a qualitative methodology drawing on the research paradigm of phenomenology and conducted in-depth interviews. We recruited physiotherapy clinicians using purposive (Palys, 2008) and snowball sampling (Holloway & Galvin, 2016). Written and verbal consent was obtained. Semi-structured interviews were conducted by AL and ranged from 44 to 123 minutes. Audio recordings were professionally transcribed verbatim and were reviewed by AL. Content analysis was used to analyse the transcribed data, with interviewer’s written field notes as supporting reference. Data was systematically coded and categorised with the aim of identifying themes, their frequency, and relationships, through both description and interpretation (Elo & Kyngäs, 2008; Hsieh & Shannon, 2005; Lindgren et al., 2020; Vaismoradi et al., 2013). Assisted by QSR NVivo 12 Software, the data analysis was organised into five steps (Figure 1). Although illustrated as a linear, chronological sequence, analysis occurred in a non-linear, iterative manner till there was clarity and meaning in the themes that were identified.

Figure 1. Sequence of data analysis
III. RESULTS
A total of 42 physiotherapists from four settings: acute, community, specialised institutions, and private practice participated (Table 1). All participants have been practicing physiotherapists in Singapore for the past three years, with 33.3 % in geriatrics and neuro rehabilitation, 45.3% in musculoskeletal and sports, and 21.4% in cardiopulmonary and other niche specialties. Thirty-six participants are Singaporeans and six are from Malaysia, Philippines, Hong Kong, New Zealand, and the UK. Ages ranged from 27 to 54 years old.
|
WORK SETTINGS |
ACUTE
Restructured public hospitals & subsidiaries |
COMMUNITY
Government supported intermediate & long- term care facilities |
SPECIALISED INSTITUTIONS
Government supported facilities for medical specialties/ niche populations
|
PRIVATE
Independent private physio clinics |
TOTAL (n) |
|
Number of Participants (n) |
16 |
13 |
6 |
7 |
42 |
|
Percentage (%) |
38.1 |
31.0 |
14.3 |
16.6 |
100 |
|
Gender (n) |
|
||||
|
Female |
9 |
12 |
5 |
2 |
28 |
|
Male |
7 |
1 |
1 |
5 |
14 |
|
Age Group in Years (n) |
|
||||
|
26-35 |
10 |
5 |
2 |
2 |
19 |
|
36-45 |
4 |
5 |
3 |
3 |
15 |
|
46-55 |
2 |
3 |
1 |
2 |
8 |
|
Professional Qualifications (n) |
|
||||
|
Diploma/Degree |
7 |
9 |
2 |
1 |
19 |
|
Postgraduate |
9 |
4 |
4 |
6 |
23 |
|
Number of Years in Healthcare (n) |
|
||||
|
< 10 |
9 |
6 |
1 |
2 |
18 |
|
10-20 |
5 |
5 |
4 |
3 |
17 |
|
> 20 |
2 |
2 |
1 |
2 |
7 |
n = number of participants
Table 1. Participants demographics
Six key themes were identified from the ethical situations described by the participants in their everyday physiotherapy practice: 1) managing healthcare resource constraints – encompassing ethical situations regarding the financial cost of healthcare, resource limitations and healthcare system inadequacies, 2) conforming to healthcare norms in Singapore – covering particular ethical challenges related to Singapore’s sociocultural context, including healthcare norms, 3) negotiating the complexity of the work environment – comprising challenges participants encountered in fulfilling their multiple obligations, especially in a negative work environment, 4) adapting to the intricacies of different healthcare settings – representing the unique ethical issues specific to the four different settings in Singapore, 5) balancing professional obligations and personal wellbeing – emerging from the participants’ struggle with their duty as moral agents, entrusted with the care of their patients while safeguarding their personal wellbeing and 6) advocating for patients: the predicament of relationships – exploring the relational aspects of a physiotherapist’s role, including defining professional boundaries, advocating for patients while managing their responsibilities to patients’ family and their colleagues. Complete quotes (QN1- QN18) illustrating the six themes are presented in Table 2.
|
Themes |
Quotations (QN) |
|
Managing healthcare resource constraints |
QN1: “I feel that these boundaries are set…because… at the end of the day it’s [healthcare] a business … we have to meet our finances. We have to balance our cheque books”. (P25) QN2: “If it’s something beyond our control, like the health system in Singapore itself, it can also be a potential barrier to our ethical practice. Because it’s not that we don’t want to do it. But … our hands are tied and it’s because of all these external factors that is affecting us.” (P38) |
|
Conforming to healthcare norms in Singapore |
QN3: “The subsidized cases actually are more complex than the private patients because private patients once they have a problem, they will get medical attention immediately… Whereas the subsidized patients…they usually drag…if they are being managed by a fresh grad that has no idea what is going on, then I think is unfair for them. And so, the cases that they [juniors] see, a lot of time is much more complex than the cases that the seniors see.” (P15) QN4: “I think insisting on certain types of equipment that we don’t feel or don’t agree with, that the patient really needs, but we do have to give because the doctor will keep on insisting on it, no matter how much we tell them that it may not be beneficial to the patient and all that. I think that’s one of the ethical things that I feel that I encounter.” (P33) QN5: “Breaking bad news seems to be also a bit of a two-way thing, where you have to go around to the family member first, before telling the patient even now. I mean, 20 years ago when I first started work it was like that, and I thought it would have moved on right? No. So I think is the education and is the perception of our Asian values, of the very paternalistic values that I think our families, or our patient’s families have.” (P09) |
|
Negotiating the complexity of the work environment |
QN6: “Because all you [i.e. the organisation] care about is earning money, all you [i.e. the organisation] care about is how many patients I can see a day and not caring whether I see it well, I’m seeing it correctly, whether I have provided value to the client.” (P13) QN7: “I see a patient, I read the history and I do the minimum, I do no harm. Patient may not get very well or recover as fast as they should…In terms of assessment, we need to be a bit more holistic, we need to assess thoroughly, but we don’t have the time…to me is clinically not ethical, but that’s how we’ve been working in a clinical setting because of time constraint, resources constraint.” (P22) QN8: “When I see something, I will just say it out to my superior, hoping that something can be done. And I can say it a few times, but once I see this is not going to work, because simply nobody responds to you, then just have to let it be, or if you really cannot take it, then you leave the organization.” (P15) |
|
Adapting to the intricacies of different healthcare settings |
QN9: “So, the proper procedure is that we refer them back to the doctor and get a new referral for the new problem. I find it quite silly to do that, the patient is right in front of me, and I know what’s the problem. I can instantly give a solution to the problem, why do I need to go and get a referral, and then delay for another three months before the patient can come back and see me for another problem?” (P26 – in acute setting) QN10: “If I make this person too mobile, family member cannot cope, he’s falling down, so this is my moral dilemma. I want him to be better, physically better. But he’s moving all over the place and he’s prone to fall and he’s much bigger size than the carer, (who) is only 40kg. I’m in a moral dilemma, how much should I give? How much should I train, or should I just give a little bit more just to maintain him? Must see from carer’s perspective. I don’t live with the person. I can come in once in a while, that one hour or just 45 minutes. But this person stays 24 hours, that’s where I’m stuck.” (P02 – in community setting) QN11: “However, then comes to work organisation that you need to understand the needs of the organisation and even the greater picture, therefore, you may not give the patient the best anymore.” (P03 – in specialised institution setting) QN12: “It’s very correlation or causation, or whatever. Often the treatment plan will miraculously be the same length as the [number] of sessions given by insurance, which you know is coincidence right? That it always happens to be the same length. You’ve got 10 sessions via insurance. That’s how long it’s going to take you to get better.” (P29 explained in a satirical manner – in private practice clinic) |
|
Balancing professional obligations and personal wellbeing
|
QN13: “Yes, so every day, we’ll carry him out on a chair for two hours… we’ll carry him back to bed and it’s two to three times max assist…this actually gave my senior some backache…because every day, is every day…because for such heavy patient, there’s no real technique already… So, this is a dilemma.” (P36) QN14: “Because I thought it was like part of my job. Probably he accidentally touched…when we do transfer, it tends to like, hands go flare anywhere. So, I thought never mind because I need to do my job. I need to transfer him. Of course, I don’t want him to fall down. So, I have to do all this contact.” (P34) QN15: “If it is a young female patient, then you try to have the female TA (therapy assistant) to be in as your chaperon. If it’s Ah Ma (older lady), then just keep the door open. It’s okay. I don’t know how is that right or wrong. But so far, it doesn’t give me any problem with that kind of practice. Usually, the Ah Ma doesn’t complain.” (P11) |
|
Advocating for patients: the predicament of relationships |
QN16: “Of course, the patient did give verbal consent. So, by right, by legal standpoint, it means that it’s fine. Then you start thinking a little bit deeper, sometimes when you’re in a clinic, patient will actually feel that they have to do that. If they don’t agree to your examination, then they are here for no purpose…Does it make the patient feel that we are coercing them? And they don’t really have a choice to really say, I don’t want it in that sense.” (P41) QN17: “I’m trying to fight for my client’s welfare. But a lot of times, if the family do not seek that welfare for the client, there is nothing I can do…. Do I train the caregiver who’s not willing to learn? Do I charge this family when the family has already expressed interest in no longer paying for equipment, or even therapy? Do I force it down their throat?” (P04)
QN18: “I guess maybe to me it really depends on the extent of that incident, how bad of that it is to the profession as a whole. If it is something that is minor and understandable, then probably I will not. But if it is something that is…pretty bad, maybe I would. I don’t know, it’s still a struggle, I can’t because it’s my fellow friends and colleagues. So, it’s a bit tough to be honest.” (P27) |
Table 2. Quotes to illustrate the six themes
A. Managing Healthcare Resource Constraints
Participants were aware of their ethical responsibility to act in the patient’s best interest in the provision of care but felt the pressure of finite resources and financial constraints (QN1). They described how they struggled to fulfill their professional obligations whilst at the same time managing patients’ expectations about availability of resources. Some therapists found loopholes to bypass government funding requirements. One participant (P26) summarised it as being a “discrepancy between the ideal care for the nation as a whole versus what is ideal for the patient’s health right before my eyes”. Some participants spoke about how key performance indicators (KPIs) intended to manage healthcare costs can drive change in organisational and clinician behaviour to practice defensively rather than using evidence-based practice to meet patients’ needs. Participant 09 described it as “funding drives behaviour” and gave the example of how a KPI that tracks fall rates may sway clinicians to be overly conservative to prevent falls, rather than challenging patients’ balance to maximise recovery. A lack of clear workflows and integration between different clinical settings was another ethical challenge preventing best available care for patient. Community and private practice physiotherapists indicated that they lack access to medical records and diagnostic results to seek clarity on a patient’s condition. This resulted in therapists feeling frustrated, as they had to delay treatment or proceed without a clear understanding of the patient’s medical status (QN2).
B. Conforming to Healthcare Norms in Singapore
For some participants, the allocation of only senior clinicians to private patients and junior clinicians to subsidised patients was viewed as unjust practice, where allocation of clinicians’ expertise is not based on the needs of patients. Participant 15 shared that the subsidised patients tended to be more complex cases as they may not have the resources to seek medical attention early (QN3). Most participants acknowledged this as an accepted practice in Singapore’s healthcare system and not just specific to physiotherapy, with participant 39 highlighting that “no one addresses it”. Adding to the social class differentiation, nearly all participants commented on the acceptance of hierarchical differentiation in healthcare with doctors at the top. Many participants spoke about paternalism being widely practiced and accepted by patients, and shared incidents where doctors dictated treatment plans, and even overrode patients’ wishes. Participants felt obliged to comply regardless of their own professional judgement (QN4).
Familialism may also compromise patients’ autonomy. Participants shared stories where family members dominated decision-making or demanded withholding information from patients. There were also geriatric patients who chose to relinquish their autonomy to their children. Many participants viewed this as an accepted part of Asian norms (QN5). A few participants stressed that many Singaporeans still hold conservative views and highlighted the importance of remaining sensitive to racial, religious, and cultural differences. For example, participant 22 disclosed that it is not accepted practice for male physiotherapists to place electrocardiogram (ECG) leads on a female patient even with the patient’s consent and a chaperon present.
C. Negotiating the Complexity of the Work Environment
Organisations have to manage the financial cost of patient care and ensure business sustainability. With resource limitations, clinicians face the challenge of conflicting obligations to their organisation and their patients. Participant 13 expressed her frustration and resentment that physiotherapy outcomes are determined by organisational financial values (QN6). Another participant (P31) shared how she had to discharge patients “prematurely” to meet organisational expectations. Other participants coped by settling for minimum treatment and doing no harm to patients (QN7).
Adding to this complexity was a negative work culture, expressed by participants as the pressure to conform to the organisation’s expectations, norms, and practices. Examples given included unreasonable workloads, biasness towards preferred staff, belittling remarks, fault-finding, and masked threats of poor appraisals. Staff were expected to conform and follow the rules, leading to a culture of fear, where safety incidents went unreported for fear of repercussions. This was further perpetuated by the lack of supervisors’ moral courage, who ignored such ethical infringements, thus normalizing ethical silence as accepted behaviour. Participant 13 disclosed her moral distress when her concerns regarding fraudulent behaviour by a colleague who falsely documented and charged for services, were disregarded by her seniors. Some participants dispiritedly added that often no action was taken and they either learnt to accept the status quo and found their own solutions or left the organisation (QN8).
D. Adapting to the Intricacies of Different Healthcare Settings
1) Acute settings: The different organisational structure and systems in each setting gave rise to specific ethical concerns. Many ethical issues in the acute settings related to the structured systems, established practices and workflows. One such practice was physiotherapists not being allowed as first contact practitioners in public institutions. Patients can only be seen with a referral from doctors and only be treated for the problem for which they were referred. This was ethically challenging for physiotherapists wanting to manage patients holistically (QN9). Several participants also raised concerns regarding minimal charging per session. In some acute settings, the on-call duty was rostered for all physiotherapists, regardless of their inpatient competency or speciality. Concerns were raised about whether this was ethically good clinical practice and in patients’ best interests.
2) Community settings: Some participants commented that community settings have varied and diverse services, making it difficult to implement guidelines that are applicable and fair to all services. This can encourage clinicians to circumvent the rules to benefit their patients. In integrating a patient back to their community, the patient’s psychological, social, and family issues can become the major consideration. Participant 02 shared her dilemma in having to factor in the caregiver’s coping ability when progressing a patient with mental health issues, who had little comprehension of fall risks, to independent mobility (QN10). A few participants commented that community physiotherapists generally have greater independence and flexibility in their work schedule, but this can engender accountability issues in terms of documentation and the standard of services provided. Some participants felt that the lack of awareness of community services available and an unsubstantiated perception that community physiotherapists are not as skilled, may deter some patients from continuing their care in the community and could have contributed to a shortage of community allied health professionals.
3) Specialised institutions: For some specialised institutions where healthcare is not the core business, physiotherapists reported being constrained by the organisational goals when caring for their patients. The needs of the organisation and the deliverables expected factored greatly in both the patient’s and clinician’s decision-making. Consequently, the best interest of the patient may not take precedence (QN11). Participants commented that the hierarchical order in such institutions tended to be more overt, with instructions directed by leaders in charge rather than team discussions.
4) Private practice clinics: Participant 27 described the business aspect of private practice as having to wear two hats: one as a clinician and one as a businessman. This can lead to maximising profits through overcharging, overservicing and maximising insurance claims. Participant 27 further disclosed that most people kept it hushed, “it’s one of those things that everyone knows is happening, but no one wants to rock the boat”. Participant 29 shared how he had to see post-op cases twice weekly, regardless of whether it was necessary, “because that’s just the way things are done” and how the cost of treatment or number of sessions needed for recovery consistently matched the insurance claim limits (QN12). Other participants raised issues which bordered on being illegal. One common example shared was fee-splitting, whereby commission was given for the referral of patients. Private clinicians commented that private practice is loosely regulated, with no standardisation or best practice guidelines and that there is little collaboration or accountability to the profession. They further elaborated that private practice is very competitive, with some clinicians making exaggerated claims about their skills or effectiveness of their treatment.
E. Balancing Professional Obligations and Personal Wellbeing
Participants described conflicts between their work responsibilities and their personal wellbeing. They shared their insecurities about whether they had positively fulfilled their professional obligations. Demanding expectations or long working hours imposed by organisations forced some participants to sacrifice their personal life, compromise their mental health and even sustain work-related injuries. Participants detailed episodes of transferring or ambulating patients without equipment or sufficient manpower (QN13). The nature of physiotherapy often requires close physical contact with patients. Participant 34 disclosed her distressing encounter with a patient with mental health issues, who repeatedly touched her inappropriately but denied it. On why she continued treatment, she replied that she needed to do her job and convinced herself that it was probably accidental (QN14). Participant 11 shared his dilemma with regard to treating female patients when there was a lack of chaperones. To protect staff from allegations of misconduct, it is accepted practice to leave the consultation room door open, leading to a possible violation of patients’ privacy (QN15). Participants also disclosed unethical and even illegal incidents which reflected the therapists’ conflict between protecting themselves and their professional responsibilities. These included false documentation of clinical notes, dishonesty about treatment errors, or not reporting safety violations.
Having self-doubt about one’s competency, whether it is due to inexperience, being out of practice or due to a lack of access to resources led some participants to question whether they had done patients a disservice or whether they were practicing beyond their capability. At times, clinicians also found it challenging to bill patients for physiotherapy services, especially if patients had financial difficulties.
F. Advocating for Patients: The Predicament of Relationships
Several participants highlighted the crossing of professional boundaries as an ethical concern. This included patients constantly calling or messaging, asking for free advice or personal favours. The nebulous zone where a professional relationship crossed over into friendship or even a dependency worried many participants. Numerous participants shared their turmoil when dealing with special populations such as patients with mental health conditions. The dilemma of overriding a patient’s autonomy became harder to resolve when the patient’s safety was at risk or where there was a possibility of detrimental consequences. Participant 41 pondered about the unspoken power differential between the patient and the healthcare professional, which can lead to patients feeling pressured to consent to treatment (QN16).
Another common dilemma expressed by participants was gaining caregivers’ and families’ support. Family members felt justified in their demands as the payer and viewed themselves as the spokesperson. Some participants expressed their helplessness with family members unwilling to pay for needed services or equipment (QN17).
Participants shared views about maintaining collegiality and not disrespecting colleagues’ viewpoints, specifically when there were conflicting patient management strategies. Some participants resented the loss of their professional autonomy but yielded to maintain harmony, and to avoid confusion for the patient. A number of participants reinforced this strong sense of fraternity, including unwillingness to expose wrongdoing even if colleagues had crossed ethical and legal boundaries (QN18). Some participants spoke about the move towards transdisciplinary practice in Singapore and the blurring of professional boundaries. One participant (P04) elaborated on resource limitations in home-based therapy, prompting her to take on other healthcare roles to prescribe home equipment and even change patients’ wound dressings. She expressed her dilemma in having to consider the patient’s perspective, her organisation’s views, and her own competency as well as the professional and legal implications of providing the wrong advice.
Further analysis revealed that the ethical challenges encountered mapped to the three overall spheres of ethics previously identified by Glaser (2005) and Sippel et al. (2015), namely the micro, meso and macro spheres. Ethical issues at the micro sphere centered around physiotherapist-patient relationships, physiotherapist’s interactions with colleagues and their own needs. The meso sphere consists of four quarters that represented the four settings, and issues included structural problems and challenges related to organizational resources or systems. The macro sphere comprises ethical issues rooted in the influence of cultural, sociological, religious, economic, and political contexts (Sippel et al., 2015). The modified illustration of spheres of ethics with the meso sphere encircling the micro sphere and the macro sphere encircling the meso sphere, show the connection and interdependence of all three spheres (Figure 2).
Figure 2. Spheres of ethics (six themes)
IV. DISCUSSION
This study is the first to report on the clinical ethics issues faced by physiotherapists practicing in Singapore. It also provides some insights into the influence of context in ethical decision-making. The six themes identified were further organised into micro, meso and macro spheres or contexts of ethics. The micro sphere themes included ethical issues that have previously been identified in other physiotherapy study findings (Delany et al., 2018; Fryer et al., 2021; Praestegaard & Gard, 2013; Sturm et al., 2022). The notable points of difference specific to Singapore were themes residing in the meso and macro spheres. These themes offered potential insights into the particular context of physiotherapy practice in Singapore. One example in the meso sphere is the influence of different healthcare settings (acute, community, specialised institutions, and private practice) on ethical dimensions of physiotherapy practice within Singapore’s healthcare system. There were differences in the predominance or perceived importance of certain ethical issues due to each setting’s unique organisational structure and systems. These findings appear to reflect current literature which reported on differences in physiotherapists’ ethical experiences due to the influence of healthcare settings (Cantu, 2018, 2019; Hudon et al., 2015).
At the macro sphere, participants reported that fulfilling government set KPIs or outcome measures which determined healthcare funding exerted indirect pressure on them. They grappled with patients’ expectations of advocacy on their behalf and societal expectations of cost containment (Dronberger, 2003). In meeting the requirements, participants had to balance their view about what was a good enough treatment constrained by the system, versus the best treatment available. The findings suggest that having to meet quantitative statistical numbers such as discharge rates was interpreted by some therapists as neglecting the quality of care and negatively affecting the therapist-patient relationship. This finding is consistent with that of Hudon et al. (2015), who highlighted institutional and economic influence on the quality of physiotherapy service and public trust. Another theme in the macro sphere concerned the negative effects of hierarchies and power differentials, which therapists believed led to paternalistic practice. Factors contributing to paternalism can include time limitations on treatment, patient’s literacy levels, societal values of respecting seniority and the accepted practice of patients handing over decision-making to authority or their family. Familialism is prevalent in Singaporean culture, where a family centric approach or interest will outweigh individual’s autonomy (Krishna, 2012). It is viewed as an accepted part of Asian values and needs to be acknowledged in order to provide the best possible care for the patient. Ethical issues related to familialism have also been reported by studies in the African context (Chigbo et al., 2015; Nyante et al., 2020; Sippel et al., 2015).
A. Relevance to Ethics Education
There is agreement that ethics cannot be taught independent of context, with a focus only on the epistemic knowledge, but that it needs to incorporate the dynamic influence of macro, meso and micro factors (Barradell, 2017; Cantu, 2018; Greenfield et al., 2015; Ladeira & Koifman, 2017). The themes in this study can directly inform the ethics curriculum, highlighting to students the influence of resource constraints, local healthcare norms, organisational culture, challenges of different settings, as well as balancing multiple obligations. Beyond awareness, students must be equipped with the abilities and skillsets to address and navigate these ethical situations. Elaboration on each theme’s implications for the local ethics curriculum is outlined in Table 3.
|
Spheres of ethics |
Themes |
How understanding of spheres of ethics can inform physiotherapy ethics curricula |
|
MACRO: Conflict of ethical principles versus societal expectations, culture, and practices |
Managing healthcare resource constraints |
· Incorporate understanding of financial aspects of healthcare and its influence on physiotherapy practice (Finch et al., 2005). · Learn to anticipate and navigate the potential conflicts between equitable use of resources (justice) and best care for each patient (beneficence). |
|
Conforming to healthcare norms in Singapore |
· Be consciously aware of local cultural and practices. Acknowledging and respecting both universal health ethics principles and culturally based differences in values by taking into account relevant contextual considerations in application of ethical principles (Fuscaldo et al., 2013). · Learn to reason and negotiate for common moral ground without compromising one’s moral integrity (Fuscaldo et al., 2013). |
|
|
MESO: Contention between ethical principles and organisational values and norms |
Negotiating the complexity of the work environment |
· Recognise the complexities of the work environment, including managing obligations to employers versus professional duty to their patients. · Develop strategies and skillsets to overcome negative work culture (e.g. by building an advisory support system and network within the organisation or the national professional body). |
|
Adapting to the intricacies of different healthcare settings |
· Understand the strengths and limitations of different workplace settings in Singapore and potential ethical challenges. |
|
|
MICRO: Conflict of ethical principles or the struggle between self-interest versus altruism |
Balancing professional obligations & personal wellbeing |
· Reinforce importance of personal integrity and learn coping strategies for self -care to prevent professional burn out or moral distress. |
|
Advocating for patients: the predicament of relationships |
· Appreciate that relational aspects of physiotherapy practice go beyond patient-therapist interactions to include colleagues and caregivers. · Emphasise physiotherapists’ role as a moral agent and advocate for patients. |
Table 3. Implications for ethics curricula
The study findings can be used to inform the development of realistic and contextualised case studies that have the potential to resonate with students’ clinical experience and improve the relevance of ethics education (Barnitt & Roberts, 2000; Fuscaldo et al., 2013; Triezenberg & Davis, 2000). The data in this study highlighted therapists’ emotions of frustration, anger, and concern. Disregarding contextual differences may create indifference, cynicism, or even moral distress when students begin practice and experience the realities of clinical practice (Greenfield & Jensen, 2010; Mohr & Mahon, 1996; Nalette, 2010). Students may dismiss ethics as irrelevant or feel disrespected that their culture and practices have not been considered in the materials taught (Fuscaldo et al., 2013).
Developing realistic case studies for ethics curricula has four possible effects: 1) it assists in dispelling the notion that ethics is based on abstract and idealist considerations (Seedhouse, 1995), 2) it can stimulate practical reflection and be action guiding to help students reason and navigate ethical challenges (Geddes et al., 2009; Swisher et al., 2012), 3) it can address the dissonance between what they learn in the classroom and what they experience in clinical practice (Dutton & Sellheim, 2017), 4) it can assist to increase ethics literacy and ethical courage. Case studies based on local experiences can provide the physiotherapy community with the ethical language to express their thoughts (Barnitt & Partridge, 1997). This shared language may enable students and clinicians to share experiences and learn how to speak up or seek help. Only when ethical issues that are pertinent to the local physiotherapy community are voiced, articulated, and discussed, can there be engagement of the community to confront identified ethical concerns, commit to creating change, and to strive towards ethical clinical practice.
B. Limitations
Participant recruitment and interviews were completed under the permeating influence of the global COVID crisis amidst shortage of healthcare staff. Due to the sensitivity of the topic, participants may have been guarded and not freely shared their views.
V. CONCLUSION
This study explored the ethical issues experienced and interpreted by physiotherapists across a range of practice settings in Singapore and examined how these experiences could inform ethics education. Our results have further substantiated current literature that context plays a critical influencing role on ethical situations, as they are experienced and perceived by physiotherapists in their unique geographical and clinical settings. The ability to act ethically has to be understood within the context and complexity of the sociocultural and political framework, along with the explicit and implicit influences, obligations, and commitments as part of a community, in order to directly address the everyday frustrations and concerns that clinicians face in trying to provide the best care for patients. With this knowledge, ethics educators and clinical supervisors will be better equipped to prepare students for clinical practice in Singapore.
Notes on Contributors
AL reviewed the literature, conceptualised and designed the study, conducted the interviews, analysed and interpreted the data, drafted the manuscript and wrote the final version submitted. This study is part of her PhD thesis.
CD is the first author’s primary PhD supervisor, who is involved in finalising the study and manuscript conceptualisation, and supervised the study from the beginning to the final version of the manuscript.
VX is the first author’s local PhD supervisor for data collection and supervised the study from the beginning to the final version of the manuscript.
Both CD and VX gave critical feedback on the direction and writing of the manuscript.
Ethical Approval
Ethics approval for this study was obtained from the University of Melbourne, Medicine and Dentistry Human Sub-Committee on 25 October 2019 (ID 1955123), and from the Singapore Institute of Technology, Institutional Review Board on 25 November 2019 (Project 2019146).
Data Availability
As the topic is of a sensitive nature and part of a larger PhD study, transcripts from the interviews are confidential and the authors do not have consent to upload onto a repository.
Acknowledgement
The authors would like to thank the 42 participants who have consented and graciously gave their time to participate in this study.
Funding
This study was completed with support from Singapore Institute of Technology (SIT) SEED grant (R-MOE-E103-C019).
Declaration of Interest
The authors declare that they have no competing interests.
References
Aderibigbe, K. S., & Chima, S. C. (2019). Knowledge and practice of informed consent by physiotherapists and therapy assistants in Kwazulu-Natal Province, South Africa. South African Journal of Physiotherapy, 75(1), a1330. https://doi.org/10.4102/sajp.v75i1.1330
Aguilar-Rodríguez, M., Marques-Sule, E., Serra-Añó, P., Espí-López, G. V., Dueñas-Moscardó, L., & Pérez-Alenda, S. (2019). A blended-learning programme regarding professional ethics in physiotherapy students. Nursing Ethics, 26(5), 1410–1423. https://doi.org/10.1177/0969733017748479
Barnitt, R., & Partridge, C. (1997). Ethical reasoning in physical therapy and occupational therapy. Physiotherapy Research International, 2(3), 178–194. https://doi.org/10.1002/pri.v2:3
Barnitt, R. E., & Roberts, L. C. (2000). Facilitating ethical reasoning in student physical therapists. Journal of Physical Therapy Education, 14(3), 35–41. https://doi.org/10.1097/00001416-200010000-00007
Barradell, S. (2017). Moving forth: Imagining physiotherapy education differently. Physiotherapy Theory & Practice, 33(6), 439–447. https://doi.org/10.1080/09593985.2017.1323361
Beauchamp, T. L., & Childress, J. F. (2001). Principles of biomedical ethics. Oxford University Press.
Bengtsson, M. (2016). How to plan and perform a qualitative study using content analysis. NursingPlus Open, 2, 8–14. https://doi.org/10.1016/j.npls.2016.01.001
Boeije, H. (2002). A purposeful approach to the constant comparative method in the analysis of qualitative interviews. Quality and Quantity, 36, 391–409. https://doi.org/10.1023/a:1020909529486
Cantu, R. (2018). Physical therapists’ perception of workplace ethics in an evolving health-care delivery environment: A cross-sectional survey. Physiotherapy Theory and Practice, 35(8), 724–737. https://doi.org/10.1080/09593985.2018.1457744
Cantu, R. (2019). Physical therapists’ ethical dilemmas in treatment, coding, and billing for rehabilitation services in skilled nursing facilities: A mixed-method pilot study. Journal of the American Medical Directors Association, 20(11), 1458–1461. https://doi.org/10.1016/j.jamda.2019.06.013
Carpenter, C. (2010). Moral distress in physical therapy practice. Physiotherapy Theory & Practice, 26(2), 69–78. https://doi.org/10.3109/09593980903387878
Carpenter, C., & Richardson, B. (2008). Ethics knowledge in physical therapy: A narrative review of the literature since 2000. Physical Therapy Reviews, 13(5), 366–374. https://doi.org/10.1179/174328808×356393
Chigbo, N. N., Ezeome, E. R., Onyeka, T. C., & Amah, C. C. (2015). Ethics of physiotherapy practice in terminally ill patients in a developing country, Nigeria. Nigerian Journal of Clinical Practice, 18(7), S40–S45. https://doi.org/10.4103/1119-3077.170826
Delany, C., Edwards, I., & Fryer, C. (2018). How physiotherapists perceive, interpret, and respond to the ethical dimensions of practice: A qualitative study. Physiotherapy Theory and Practice, 35(7), 663–676. https://doi.org/10.1080/09593985.2018.1456583
Dronberger, J. (2003). Fraud and negligence in physical therapy practice: A case example. Physiotherapy Theory and Practice, 19(3), 151–159. https://doi.org/10.1080/09593980307961
Dutton, L. L., & Sellheim, D. O. (2017). Academic and clinical dissonance in physical therapist education: How do students cope? Journal of Physical Therapy Education, 31(1), 61–72. https://doi.org/10.1097/00001416-201731010-00009
Edwards, I., Delany, C. M., Townsend, A. F., & Swisher, L. L. (2011). New perspectives on the theory of justice: Implications for physical therapy ethics and clinical practice. Physical Therapy, 91(11), 1642–1652. https://doi.org/10.2522/ptj.20100351.10
Edwards, I., Wickford, J., Adel, A. A., & Thoren, J. (2011). Living a moral professional life amidst uncertainty: Ethics for an Afghan physical therapy curriculum. Advances in Physiotherapy, 13(1), 26–33. https://doi.org/10.3109/14038196.2010.483015
Elo, S., & Kyngäs, H. (2008). The qualitative content analysis process. Journal of Advanced Nursing, 62(1), 107–115. https://doi.org/10.1111/j.1365-2648.2007.04569.x
Finch, E., Geddes, E. L., & Larin, H. (2005). Ethically-based clinical decision-making in physical therapy: Process and issues. Physiotherapy Theory and Practice, 21(3), 147–162. https://doi.org/10.1080/09593980590922271
Fryer, C., Sturm, A., Roth, R., & Edwards, I. (2021). Scarcity of resources and inequity in access are frequently reported ethical issues for physiotherapists internationally: An observational study. BMC Medical Ethics, 22, Article 97. https://doi.org/10.1186/s12910-021-00663-x
Fuscaldo, G., Russell, S., Gillam, L., Delany, C., & Parker, M. (2013). Addressing cultural diversity in health ethics education: Final Report 2013. http://www.research-matters.com.au/publications/FinalReport.pdf
Geddes, E. L., Salvatori, P., & Eva, K. W. (2009). Does moral judgement improve in occupational therapy and physiotherapy students over the course of their pre-licensure training? Learning in Health and Social Care, 8(2), 92–102. https://doi.org/10.1111/j.1473-6861.2008.00205.x
Glaser, J. W. (2005). Three realms of ethics:An integrating map of ethics for the future. In R. B. Purtilo, G. M. Jensen, & C. B. Royeen (Eds.), Educating for moral action: A sourcebook in health and rehabilitation ethics (pp. 169-184). F.A. Davies.
Graneheim, U. H., Lindgren, B. M., & Lundman, B. (2017). Methodological challenges in qualitative content analysis: A discussion paper. Nurse Education Today, 56, 29–34. https://doi.org/10.1016/j.nedt.2017.06.002
Greenfield, B., & Jensen, G. M. (2010). Beyond a code of ethics: Phenomenological ethics for everyday practice. Physiotherapy Research International, 15(2), 88–95. https://doi.org/10.1002/pri.481
Greenfield, B. H. (2006). The meaning of caring in five experienced physical therapists. Physiotherapy Theory and Practice, 22(4), 175–187. https://doi.org/10.1080/09593980600822859
Greenfield, B. H., Jensen, G. M., Delany, C. M., Mostrom, E., Knab, M., & Jampel, A. (2015). Power and promise of narrative for advancing physical therapist education and practice. Physical Therapy, 95(6), 924-933. https://doi.org/10.2522/ptj.20140085
Holloway, I., & Galvin, K. (2016). Data analysis: Procedures, practices and use of computers. In Qualitative research in nursing and healthcare(4th ed., 287–302).Wiley-Blackwell.
Hsieh, H. F., & Shannon, S. E. (2005). Three approaches to qualitative content analysis. Qualitative Health Research, 15(9), 1277–1288. https://doi.org/10.1177/1049732305276687
Hudon, A., Drolet, M. J., & Jones, B. W. (2015). Ethical issues raised by private practice physiotherapy are more diverse than first meets the eye: Recommendations from a literature review. Physiotherapy Canada, 67(2), 124–132. https://doi.org/10.3138/ptc.2014-10
Hudon, A., Ehrmann Feldman, D., & Hunt, M. (2019). Tensions living out professional values for physical therapists treating injured workers. Qualitative Health Research, 29(6), 876–888. https://doi.org/10.1177/1049732318803589
Krishna, L. R. (2012). Best interests determination within the Singapore context. Nursing Ethics, 19(6), 787–799. https://doi.org/10.1177/0969733011433316
Ladeira, T. L., & Koifman, L. (2017). Interface entre fisioterapia, bioética e educação: revisão integrativa [Interface between physical therapy, bioethics and education: Integrative review]. Revista Bioética, 25(3), 618–629. https:/doi.org/10.1590/1983-80422017253219
Lindgren, B. M., Lundman, B., & Graneheim, U. H. (2020). Abstraction and interpretation during the qualitative content analysis process. International Journal of Nursing Studies, 108. https://doi.org/10.1016/j.ijnurstu.2020.103632
Mohr, W. K., & Mahon, M. M. (1996). Dirty hands: The underside of marketplace health care. Advances in Nursing Science, 19(1), 28–37. https://doi.org/10.1097/00012272-199609000-00005
Nalette, E. (2010). Constrained physical therapist practice: An ethical case analysis of recommending discharge placement from the acute care setting. Physical Therapy, 90(6), 939–952. https://doi.org/10.2522/ptj.20050399
Nyante, G. G., Andoh, C. K., & Bello, A. I. (2020). Patterns of ethical issues and decision-making challenges in clinical practice among Ghanaian physiotherapists. Ghana Medical Journal, 54(3), 179–185. https://doi.org/10.4314/gmj.v54i3.9
Ong, E. K. (2020). The impact of sociocultural influences on the COVID-19 measures—reflections from Singapore. Journal of Pain and Symptom Management, 60(2), e90–e92. https://doi.org/10.1016/j.jpainsymman.2020.04.022
Oppong, S. (2019). When the ethical is unethical and the unethical is ethical: Cultural relativism in ethical decision-making. Polish Psychological Bulletin, 50(1), 18–28. https://doi.org/10.24425/ppb.2019.126014
Oyeyemi, A. (2011). Ethics and contextual framework for professional behaviour and code of practice for physiotherapists in Nigeria. Journal of the Nigeria Society of Physiotherapy, 19(1–2), 49–53. https://academicjournals.org/journal/JNSP/article-full-text -pdf/0AA592B65221
Palys, T. (2008). Purposive sampling. In L. M. Given (Ed.), The sage encyclopedia of qualittaive research methods (Vol. 2, pp. 697–698). Los Angeles: Sage.
Praestegaard, J., & Gard, G. (2013). Ethical issues in physiotherapy – Reflected from the perspective of physiotherapists in private practice. Physiotherapy Theory & Practice, 29(2), 96–112. https://doi.org/10.3109/09593985.2012.700388
Qamar, M. M., Basharat, A., Rasul, A., Basharat, S., & Ijaz, M. J. (2014). Perception of physical therapy students and professionals about the importance of professional ethics. International Journal of Medicine and Applied Health., 2(2), 57–61. https://www.academia.edu/11604067/perception_of_physical_therapy_students_and_professionals_about_the_importance_of_professional_ethics
Seedhouse, D. (1995). There’s Logic, and then there’s what we do around here. Health Care Analysis, 3(2), 87–90. https://doi.org/10.1007/BF02198208
Sippel, D., Marckmann, G., Atangana, E. N., & Strech, D. (2015). Clinical ethics in Gabon: The spectrum of clinical ethical issues based on findings from in-depth interviews at three public hospitals. PLoS ONE, 10(7), e0132374. https://doi.org/10.1371/journal.pone.0132374
Souri, N., Moghadam, A. N., & Shahbolaghi, M. (2020). Iranian physiotherapists’ perceptions of the ethical issues in everyday practice. Iranian Rehabilitation Journal, 18(2), 125–136. https://doi.org/10.32598/irj.18.2.221.5
Sturm, A., Edwards, I., Elizabeth Fryer, C., & Roth, R. (2022). (Almost) 50 shades of an ethical situation-international physiotherapists’ experiences of everyday ethics: A qualitative analysis. Physiotherapy Theory and Practice. https://doi.org/10.1080/09593985.2021.2015812
Swisher, L. L., Kessel, G. V., Jones, M., Beckstead, J., & Edwards, I. (2012). Evaluating moral reasoning outcomes in physical therapy ethics education: stage, schema, phase, and type. Physical Therapy Reviews, 17(3), 167–175. https://doi.org/10.1179/1743288X12Y.0000000011
Tan, C. H. (1989). Confucianism and nation building in Singapore. International Journal of Social Economics, 16(8), 5–16. https://doi.org/10.1108/03068298910133106
Triezenberg, H. L., & Davis, C. M. (2000). Beyond the code of ethics: Educating physical therapists for their role as moral agents. Journal of Physical Therapy Education, 14(3), 48–58. https://doi.org/10.1097/00001416-200010000-00009
Vaismoradi, M., Turunen, H., & Bondas, T. (2013). Content analysis and thematic analysis: Implications for conducting a qualitative descriptive study. Nursing and Health Sciences, 15(3), 398–405. https://doi.org/10.1111/nhs.12048
Yang, S., Shek, M. P., Tsunaka, M., & Lim, H. B. (2006). Cultural influences on occupational therapy practice in Singapore: a pilot study. Occupational Therapy International, 13(3), 176–192. https://doi.org/10.1002/oti.217
*Audrey Lim
Health and Social Sciences Cluster
Singapore Institute of Technology (SIT)
10 Dover Road
Singapore 138683
+65 6592 3390
Email: Audrey.Lim@SingaporeTech.edu.sg
Announcements
- Best Reviewer Awards 2025
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2025.
Refer here for the list of recipients. - Most Accessed Article 2025
The Most Accessed Article of 2025 goes to Analyses of self-care agency and mindset: A pilot study on Malaysian undergraduate medical students.
Congratulations, Dr Reshma Mohamed Ansari and co-authors! - Best Article Award 2025
The Best Article Award of 2025 goes to From disparity to inclusivity: Narrative review of strategies in medical education to bridge gender inequality.
Congratulations, Dr Han Ting Jillian Yeo and co-authors! - Best Reviewer Awards 2024
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2024.
Refer here for the list of recipients. - Most Accessed Article 2024
The Most Accessed Article of 2024 goes to Persons with Disabilities (PWD) as patient educators: Effects on medical student attitudes.
Congratulations, Dr Vivien Lee and co-authors! - Best Article Award 2024
The Best Article Award of 2024 goes to Achieving Competency for Year 1 Doctors in Singapore: Comparing Night Float or Traditional Call.
Congratulations, Dr Tan Mae Yue and co-authors! - Best Reviewer Awards 2023
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2023.
Refer here for the list of recipients. - Most Accessed Article 2023
The Most Accessed Article of 2023 goes to Small, sustainable, steps to success as a scholar in Health Professions Education – Micro (macro and meta) matters.
Congratulations, A/Prof Goh Poh-Sun & Dr Elisabeth Schlegel! - Best Article Award 2023
The Best Article Award of 2023 goes to Increasing the value of Community-Based Education through Interprofessional Education.
Congratulations, Dr Tri Nur Kristina and co-authors! - Best Reviewer Awards 2022
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2022.
Refer here for the list of recipients. - Most Accessed Article 2022
The Most Accessed Article of 2022 goes to An urgent need to teach complexity science to health science students.
Congratulations, Dr Bhuvan KC and Dr Ravi Shankar. - Best Article Award 2022
The Best Article Award of 2022 goes to From clinician to educator: A scoping review of professional identity and the influence of impostor phenomenon.
Congratulations, Ms Freeman and co-authors.









