Virtual assessment in Physiotherapy: Examining perceptions, constructs, and tool characteristics
Submitted: 20 April 2023
Accepted: 19 October 2023
Published online: 2 April, TAPS 2024, 9(2), 70-80
https://doi.org/10.29060/TAPS.2024-9-2/OA3044
Xiang Ren Tan1,2, Anthony J Goff1 & Li Whye Cindy Ng1,3
1Health and Social Sciences, Singapore Institute of Technology, Singapore; 2Human Potential Translational Research Programme, Yong Loo Lin School of Medicine, National University of Singapore, Singapore; 3Department of Physiotherapy, Singapore General Hospital, Singapore
Abstract
Introduction: Objective structured clinical examinations have traditionally been used to assess clinical skills. However, these face-to-face clinical assessments were hindered by physical and social restrictions imposed during COVID-19. This created a need to develop novel approaches for reliable assessment of clinical skills. We explored and evaluated a virtual exercise teleconsultation assessment (VETA) to replicate a teleconsultation setting where physiotherapy students were assessed on exercise prescription and coaching skills.
Methods: We conducted a cross-sectional mixed-methods study using convenience sampling. A VETA was implemented for 172 physiotherapy students via Zoom to allow synchronous interaction with standardised patients (SPs). 67 students and 9 SPs completed two separate post evaluation surveys on themes relating to administration, support, authenticity, effectiveness, and value of the VETA. Likert-type responses were categorised as positive, neutral, or negative while coded qualitative responses were consolidated into themes by inductive content analysis.
Results: 76% of students agreed that the assessment was authentic while 93% felt that the SPs were realistic and believable. Responders also highlighted important challenges including the limited camera viewing angle, time and space constraint, adequacy of equipment and reliability of connectivity. Exploratory factor analysis of responses revealed three latent constructs: (1) clarity of assessment, (2) clinical relevance, and (3) value of assessment.
Conclusion: Despite the technical challenges, VETA demonstrated clarity and value as an alternative assessment and showed relevance to future telehealth practice, which is increasingly pervasive in clinical settings. This paper demonstrates a feasible approach for the virtual assessment of clinical competencies.
Keywords: Health Sciences Education, Virtual Assessment, Clinical Skills, OSCE, Physiotherapy, Exercise Prescription
Practice Highlights
- The ability to assess students non-obtrusively allows for fair assessment with reduced anxiety.
- Despite several technical challenges, VETA demonstrated value as an alternative assessment.
- An appropriate context of use, content validity and authenticity of virtual assessment are crucial.
- VETA format may be used for distant learning and remote assessment of clinical competency.
- Virtual care delivery should be included as part of healthcare professionals’ formal training.
I. INTRODUCTION
Objective Structured Clinical Examinations (OSCEs) have traditionally been used to assess clinical competencies and skills important for registration, licensing, and certification with professional bodies. OSCEs were first developed by Harden (Harden et al., 1975) and have commonly been used as an assessment tool for clinical competency in both medical (Gormley, 2011; Jo & An, 2014; Shirwaikar, 2015) and allied health professions (Barra-Ortiz et al., 2021; Edwards & Martin, 1989; Silva et al., 2011; Wessel et al., 2003). OSCEs can be conducted as a formative or summative assessment (Chisnall et al., 2015) and have been described as the gold standard for clinical assessment (Norman, 2002) due to its objective, precise, and reproducible nature which allows for standardised testing across a wide range of clinical skills (Zayyan, 2011). OSCEs can strengthen links between theory and practice, improving the professionalism and readiness of allied health students to perform clinical work (Farahat et al., 2015). Hence, OSCEs form vital assessments in structured health sciences programs.
However, the recent COVID-19 pandemic with strict social distancing measures and lockdowns have posed great challenges to the delivery of teaching and authentic assessments (Kumar et al., 2021; Liang et al., 2020). This is especially pertinent to health sciences education where the use of OSCEs has been limited by physical and social restrictions imposed in response to COVID-19. Therefore, there was a need to explore novel ways to create authentic settings for objective, precise and reproducible assessments of clinical skills, despite the lack of physical contact. Virtual assessments, including virtual OSCEs, have been widely implemented across many educational institutions due to COVID-19 lockdown and restrictions (Pettit et al., 2021). Importantly, virtual OSCEs appear to be effective assessments for clinical skills, notwithstanding some limitations, in medical and pharmacy courses (Blythe et al., 2021; Deville et al., 2021; Grover et al., 2022; Hannan et al., 2021; Major et al., 2020; Prettyman et al., 2018). Virtual OSCEs have been performed using common web-based teleconferencing platform such as Zoom due to its familiarity, convenient features, and stability (Grover et al., 2022; Hannan et al., 2021; Major et al., 2020; Prettyman et al., 2018). Remote proctoring and lock-down browsers can also be employed in virtual OSCEs to ensure integrity of assessment (Deville et al., 2021). However, the conduct of virtual OSCEs varies across institutions and there are no standardised guidelines or format to date.
Virtual OSCEs can be useful to assess some but not all clinical skills required of allied health students ranging from health assessment, diagnostic skills, physical and manual therapy to patient education. During the pandemic, we conceptualised an online synchronous approach, Virtual Exercise Teleconsultation Assessment (VETA), to assess the exercise prescription and coaching skills in undergraduate physiotherapy students (Tan & Ng, 2022). The intention is to replicate a teleconsultation setting where students remotely interact with standardised patients (SPs) to prescribe and coach exercises. Teleconsultation has been defined as “synchronous or asynchronous consultation using information and communication technology to omit geographical and functional distance” (Deldar et al., 2016). With the rapid and drastic changes in COVID-19 restrictions, VETA was designed with streamlined focus on three key guiding principles: (1) validity and authenticity, (2) ease of conduct, and (3) safety. These principles are aligned to the educational principles of OSCE set out in the AMEE guide (Khan et al., 2013) encompassing construct validity, reliability (with the use of rubrics, experienced examiners, and trained SPs), feasibility, and educational impact (relating to authenticity).
To ensure (1) assessment validity and authenticity, the use of standardised patients was retained in the assessment process, as opposed to replacing with case scenarios only or role-play by faculty. The live interactions with trained SPs promote realism and allow students to navigate the complexities of effective patient communication (Lovink et al., 2021; Rickles et al., 2009). The use of trained SPs also enhances the consistency and reliability of testing and at the same time, provides a safe, learner-centred environment (Cleland et al., 2009). Simulating a real clinical setting, the students interacted with the SPs independently without visible presence of examiners. To provide a uniform examination environment, VETA was entirely conducted on campus instead of relying on home-based virtual assessment.
In addition, emphasis has been placed on the (2) ease of conduct where Zoom teleconferencing was used as this is familiar to both the faculty and students who have used the platform extensively for online learning purposes. All assessment-related resources including laptop and exercise equipment were duly provided. This helped to eliminate any potential test anxiety arising from inexperience with the use of new technology or unfamiliar teleconferencing platform. Lastly, the (3) safety of students, SPs and examiners was prioritised under the COVID-19 climate. Students and SPs resided in different parts of the campus during the assessment, and the students followed a prearranged schedule for the exam to avoid any physical interactions. All personnel wore their masks at all times, even when interacting in Zoom. The SPs and examiners were situated in the same room during the assessment, with the examiner seated a safe distance away from the SP while allowing observation. These measures ensured the least interactions across all groups and minimised risk of disease transmission.
VETA was implemented as a summative assessment in an exercise physiology module within the BSc Physiotherapy programme at Singapore Institute of Technology to assess the exercise prescription and coaching skills of physiotherapy students in a simulated teleconsultation setting. We aim to evaluate the perceptions and overall experience of students and SPs towards VETA as a virtual assessment to evaluate its potential strengths and limitations. We further explored latent constructs from students’ responses to understand our survey tool’s characteristics and its reliability in evaluating themes in clinical assessments. In this study, we examined the feasibility and value of an online synchronous approach for assessing clinical skills critical to allied health students, which may provide key insights on the future transformation of clinical skills assessments.
II. METHODS
A. VETA Procedures
As part of the necessary measures to adopt new assessment methods during the COVID-19 pandemic, a convenience sample of Year 1 B.Sc Physiotherapy students underwent a VETA in July 2021. All exam procedures were conducted at the Singapore Institute of Technology Dover campus. Students and SPs situated in two different venues where separate laptops have been set up to connect on Zoom platform for facilitating interactions across the two venues.
Students were instructed to report to the exam venue at their allocated timing where they were ushered to a reading station for 10 minutes. A case scenario was provided for students to conduct planning of exercise prescription for the SP (representing the same patient in the case scenario). After the reading station, the students proceeded to an enclosed room with the laptop connected to the SP. They were given a total of 10 minutes to interact with the SP to (1) conduct Physical Activity Readiness Questionnaire (PAR-Q) to ascertain the patient’s fitness to exercise, (2) provide a cycling exercise prescription and instruct him/her how to use a cycling ergometer bike, and (3) provide a resistance exercise prescription and coach them on how to perform the stated exercise safely. For the latter, similar resistance exercise equipment (resistance bands and dumbbells of different weights) was provided in both venues to facilitate the coaching of exercise. The amount of time left in the assessment (e.g., 5 minutes left), and the end of the assessment were indicated by different ringing bells.
SPs were allowed to seek clarification on the exercise prescription or coaching as necessary. The examiner was seated in the same room as the SP but was out-of-sight from the laptop web camera viewing angle. This is to replicate an authentic teleconsultation environment during the assessment. As compared to other similar virtual OSCE (Grover et al., 2022; Major et al., 2020), VETA goes beyond basic patient communication and consultation as it additionally includes an intervention aspect where SPs follow students’ instructions to perform a prescribed exercise safely.
Students’ performance was evaluated by three trained examiners (teaching faculty) who were experienced assessors for face-to-face OSCE for at least three consecutive years. All examiners used a standardised marking schema which was modelled closely to the existing schema used for physical OSCEs to maintain the same rigour and intent in the assessment of clinical skills.
B. Evaluation of VETA
After the assessment, the students and SPs completed two separate self-administered questionnaires. The students completed the survey on the Qualtrics® platform while SPs were provided with hardcopy forms to fill. Both mixed-methods surveys consist of 5-point Likert-type questions, and open-ended questions to gather qualitative responses. Participation in the surveys was voluntary and anonymous.
Initial design of the surveys was modelled after a recent paper (Fouad et al., 2019) that has conducted similar survey-based evaluation of students, staff and SPs’ perceptions towards an OSCE. After refinement of themes relevant to our VETA format, the student’s survey contained 26 items (23 Likert-type, 3 open-ended) which evaluated their overall experience and perceived difficulty of VETA, and five themes including the (1) administration, (2) support or resources provided, (3) authenticity, (4) effectiveness, and (5) value of VETA as a novel assessment mode. The open-ended questions gathered students’ qualitative inputs on their challenges faced, opinions on effectiveness of VETA and the potential areas of improvement. The SP’s survey contained 10 items (6 Likert-type, 4 open-ended) evaluating their overall experience and three themes including (1) administration, (2) student performance and (3) acceptability of VETA. The open-ended questions gathered SPs’ qualitative inputs on their challenges faced and the potential areas of improvement.
C. Statistical Analysis
Survey responses were coded and exported from Qualtrics® platform or manually input into Microsoft Excel (Microsoft Corporation). For 5-point Likert-type questions, responses such as “strongly agree/disagree” and “somewhat agree/disagree” were combined during analysis to represent a consensus perception (agree, neutral or disagree) towards a subject statement. Descriptive statistics of survey responses in percentages was compiled and displayed in summary tables. Individual open-ended responses were condensed into codes and eventually consolidated into common categorical themes using the inductive content analysis approach (Elo & Kyngäs, 2008; Hsieh & Shannon, 2005). Categorical themes were identified from the codes and were subsequently grouped into two overarching themes of VETA strengths and limitations.
Exploratory factor analysis was performed using SPSS software Version 20 to explore the underlying latent conceptual structure (Watkins, 2018) present in the student’s responses to the survey variables. This allows the assessment of congruency between the pre-identified themes in the survey and the latent constructs. Factor extraction was performed with Principal Axis Factoring analysis with varimax rotation. There were no missing data. Criteria on factor extraction was based on the Kaiser rule with eigenvalues > 1.0. Only subsets of unique factors with individual loadings above 0.4 were retained. Internal consistency of the items was assessed using Cronbach’s alpha coefficient with an alpha value between 0.7 and 0.9 representing a measure of satisfactory internal consistency (Downing, 2004).
III. RESULTS
A total of 172 students completed the VETA. 67 students (39% of cohort) and 9 SPs (100%) completed the respective surveys. Out of all responders, 93% of the students and all SPs expressed an overall positive experience for VETA. 60% of the students felt that the assessment was of moderate difficulty. 22% of the students have expressed that VETA was somewhat difficult while 17% felt it was somewhat easy, with 1 student (1%) responded that it was extremely easy.
A. Perceptions Towards VETA
A summary of response statistics for Likert-type items can be found in Table 1. More than 90% of students agreed that the instructions to perform each activity were clear and that they were aware of the assessment requirements. However, only 77% agreed that the time allocated for teleconsultation was sufficient, with 16% who felt that the time was insufficient. The majority of the students were satisfied with the assessment environment and Zoom setup, however 10% felt that resources and equipment provided were inadequate.
76% of them agreed that the assessment was an authentic reflection of clinical setting while 93% of students felt that the SPs were realistic and believable. More than 90% of the students agreed that VETA was a fair and valid assessment. Most students (79%) concurred that VETA should remain as a form of assessment. 61% of the students agreed that VETA offered more learning opportunities than other exams, with 11% who disagreed with the statement.
All SPs agreed that the administration of VETA (briefing instructions and Zoom setup) was adequate, and they were comfortable with the new VETA format. However, only 78% agree that instructions given by students were clear and they were able to follow the instructions without difficulty. 89% of the SPs felt confident to perform the activities independently with the given instructions. This suggests the inadequacy of some students to effectively communicate, prescribe and coach exercises to the SPs.
|
Items (For Students; n=67) |
Agree |
Neutral |
Disagree |
Themes |
|
1. Briefing instructions and information given prior to the assessment were helpful. |
88 |
8 |
4 |
|
|
2. Instructions to perform each activity were clear. |
91 |
3 |
6 |
|
|
3. I was aware of the information needed for each task in the assessment. |
93 |
3 |
4 |
|
|
4. Tasks asked to perform were fair. |
97 |
2 |
1 |
|
|
5. Time allocated for reading and planning (10 min) was sufficient. |
94 |
6 |
0 |
|
|
6. Time allocated for teleconsultation (10 min) was sufficient. |
78 |
6 |
16 |
|
|
7. The environment where the assessment was conducted was conducive. |
90 |
4 |
6 |
Support |
|
8. The audio/video quality of the Zoom session was adequate. |
94 |
3 |
3 |
|
|
9. Resources and equipment provided for the assessment were adequate. |
82 |
8 |
10 |
|
|
10. The standardised “patients” were believable and realistic. |
93 |
3 |
4 |
Authenticity |
|
11. Settings and context of given case scenario were authentic. |
97 |
1 |
2 |
|
|
12. The interaction with the standardised patient was authentic. |
91 |
5 |
4 |
|
|
13. VETA without the presence of an assessor was helpful. |
90 |
9 |
5 |
|
|
14. The VETA was an authentic reflection of clinical setting. |
76 |
19 |
5 |
|
|
15. The VETA helped to identify gaps in knowledge. |
85 |
12 |
3 |
Effectiveness |
|
16. The VETA helped to identify weaknesses in communication and patient-care skills. |
93 |
6 |
1 |
|
|
17. The VETA tested appropriate skills required for a Physiotherapist. |
87 |
9 |
4 |
|
|
18. The VETA covered a wide knowledge range. |
88 |
9 |
3 |
|
|
19. The VETA should remain as a form of assessment. |
79 |
15 |
6 |
Value |
|
20. The VETA offered more learning opportunities than other exams. |
61 |
28 |
11 |
|
|
21. The VETA was a valuable practice and learning experience. |
93 |
3 |
4 |
|
|
Items (For Standardised Patients; n=9) |
|
|
|
Themes |
|
1. Briefing instructions given before the assessment were helpful and sufficient. |
100 |
0 |
0 |
Administration |
|
2. The quality of the audio/video was adequate. |
100 |
0 |
0 |
|
|
3. Instructions given by students to perform each activity were clear and I was able to follow the instructions without difficulty. |
78 |
22 |
0 |
Student |
|
4. I am confident to perform the activities independently with the given instructions. |
89 |
11 |
0 |
|
|
5. Communication by the students were appropriate and professional. |
100 |
0 |
0 |
|
|
6. I am comfortable to receive instructions from a teleconsult session by a student in an exam setting. |
100 |
0 |
0 |
Acceptability |
Table 1. Response frequency for Likert-type questions
B. Strengths and Limitations
From the inductive content analysis of qualitative responses (Table 2), the VETA strengths were (1) reduced student anxiety, (2) relevance to practice and (3) assessment effectiveness. These were identified from students’ responses where they expressed that having the examiner off-screen helps to reduce their level of anxiety during assessment and they felt that VETA was relevant to their future practice where they may be required to conduct telehealth or telerehabilitation sessions. One key highlight is the authenticity of VETA where a student mentioned that he or she felt like a real physiotherapist giving the prescription, which affirmed that VETA replicates an authentic teleconsultation setting.
The limitations were identified to be related to (1) time and space allocation, (2) environment & equipment provided, (3) assessment effectiveness and (4) technical issues. There were similar sentiments from the SPs and students that the space provided for performing exercise was constrained. Students preferred more time allocated for teleconsultation. Furthermore, the students hoped to have visual feedback on timing during assessment and more exercise equipment to be provided. For assessment effectiveness, some students expressed that more clarity can be provided regarding the assessment rubric and expectations. Some of them felt that VETA was not reflective of a physical clinical setting. Last but not least, there were technical issues faced including the muffling of voices due to mask-wearing, connectivity issues that led to delays, and limited viewing angle of the laptop camera.
|
Themes |
Sub Themes |
|
|
VETA |
Reduced Student Anxiety |
|
|
“Having the assessor off-screen and not physically beside me really helped me focus on what I wanted to deliver to the patient. It also makes me feel less nervous and anxious and it has definitely helped me perform better” |
Students’ |
|
|
“Don’t see any invigilator, not so scary” |
||
|
Relevance to Practice |
||
|
“It is a good alternative assessment especially during Covid or future epidemics…open another option for both clients and PTs to conduct sessions remotely” |
||
|
“It is good to train us in telehealth because it gives us the opportunity to help patients who may have difficulty coming to the clinic even after the pandemic” |
||
|
“VETA was a great innovation with COVID-19… we might have to do telerehab for our patient and this would actually equip us with the skills to do so” |
||
|
Assessment Effectiveness |
||
|
“Felt that the zoom VETA was well organised and helped us cover the main objective of the module” |
||
|
“It is an effective examination tool as it is going to be a very practical thing to do in the near future” |
||
|
“The patients were great. The fact that I’ve never seen them before, coupled with how they responded and interacted with me during the VETA made this “consultation” more believable and I really felt like a physiotherapist giving an exercise prescription” |
||
|
VETA |
Time & Space Allocation |
|
|
“More time can be given to have more interactions with the patient. It felt like i was just instructing the patient without time for the patient to reply back.” |
Students’ |
|
|
“Would have liked more space to move backwards to demo exercise to patient, but chair was a bit in the way” |
||
|
“Maybe allocate more space in student’s room so that if they need to move in order to demo…. they are not restricted by the room size” |
SPs’ quotes |
|
|
“I have to adjust a few times in order to get my whole body into the screen for the candidate to see properly and complete the task assigned” |
||
|
Environment & Equipment |
||
|
“A clock timer to keep track of time would have been helpful” |
Students’ |
|
|
“Put a timer so that students are able to track how much time they have left. the bell was quite soft and some students might have missed it” |
||
|
“The environment can be slightly better as it was rather dark and the papers were messy” |
||
|
“More weights to cater exercises that require two arms” |
||
|
Assessment Effectiveness |
||
|
“Would be nice if rubric was released earlier” |
Students’ |
|
|
“Would be beneficial to give a sample case study…so that we have a clearer expectation of the exam” |
||
|
“…resistance training component of Zoom VETA was limited to upper limb exercises only” |
||
|
“It does not feel reflective of a real clinical setting as physically, we would have to consider many other factors such as conducting proper handrub before and after the activity, cleaning the equipment as well” |
||
Table 2. Qualitative responses for perceptions towards VETA
C. Common Constructs in Survey Evaluation
From the original questionnaire (21 Likert-type items categorised into 5 themes), a smaller subset of 13 items were retained after factor analysis and they were categorised and defined as 3 main latent constructs: (1) Clarity in assessment, (2) Clinical relevance, and (3) Value of assessment. The loadings of individual factor (>0.4) and the Cronbach’s alpha coefficient (>0.7) are displayed in Table 3. It was noted that some of the items previously grouped under the topic of “effectiveness” has been subsumed under either the clinical relevance or value of assessment constructs. Other items were omitted as their loadings were <0.4 or they were not unique in representing any of the latent constructs.
|
Items (n=13) |
C1 |
C2 |
C3 |
Constructs |
|
1. Briefing instructions and information given prior to the assessment were helpful. |
0.743 |
Clarity of Assessment |
||
|
2. Instructions to perform each activity were clear. |
0.785 |
|||
|
3. I was aware of the information needed for each task in the assessment. |
0.796 |
|||
|
10. The standardised “patients” were believable and realistic. |
0.754 |
Clinical |
||
|
11. Settings and context of given case scenario were authentic. |
0.782 |
|||
|
12. The interaction with the standardised patient was authentic. |
0.790 |
|||
|
15. The VETA helped to identify gaps in knowledge. |
0.548 |
|||
|
16. The VETA helped to identify weaknesses in communication and patient-care skills. |
0.681 |
|||
|
14. The VETA was an authentic reflection of clinical setting. |
0.741 |
Value of |
||
|
18. The VETA covered a wide knowledge range. |
0.803 |
|||
|
19. The VETA should remain as a form of assessment. |
0.518 |
|||
|
20. The VETA offered more learning opportunities than other exams. |
0.788 |
|||
|
21. The VETA was a valuable practice and learning experience. |
0.607 |
Table 3. Latent constructs from exploratory factor analysis
IV. DISCUSSION
A. Keeping Pace with the Digital World
With the advent of technology and increasing prevalence of virtual care (Stamenova et al., 2022), there is a need to rethink conventional assessments of clinical competencies in medical and allied health education. Formal exposure, training, and assessment of clinical care delivery over virtual platforms will be important to prepare students for the digital world, beyond traditional face-to-face environments (Fickenscher & Pagliaro, 2021). Many digitally empowered patients have turned to web-based platform for telerehabilitation services (Brennan et al., 2009). This underscores the need for future healthcare professionals to demonstrate clinical competencies that complement the virtual mode of care delivery.
In our study, VETA was designed as an alternative to traditional OSCEs for the reliable assessment of exercise prescription and coaching skills of physiotherapy students within a simulated teleconsultation setting. Standardised patients were involved to enhance the realism of the consultation session where it allows students to practice patient-centred care and professionalism in patient handling. VETA has garnered largely positive experience from both students and SPs. The qualitative responses from the surveys were supportive of the validity, authenticity, and value of VETA; however, important limitations have been highlighted to consider for improvements in the future. This represents a real-world use case of online synchronous assessment that can be implemented to evaluate clinical skills and competencies in medical or allied health education.
B. Assessment Authenticity and Relevance
In this study, VETA provided a unique opportunity for students to conduct and experience a simulated teleconsultation and it has been largely perceived as a valid and authentic assessment. The content validity of VETA can be assessed from the realistic clinical tasks perceived by students, the test content which represents what the curriculum needs to assess (exercise prescription and coaching skills), and the right domains being tested such as communication and patient-care skills and the safe conduct of exercise (American Educational Research Association, 2014). The authenticity and value of VETA were echoed by both the quantitative and qualitative responses in this study where students felt that it was a good way to equip them with skills necessary for telehealth practice. It is paramount to note that the challenge in conducting physical assessments under COVID-19 climate is not uniquely experienced by students but also, by health practitioners (Chen et al., 2020). Telerehabilitation has been advocated and practiced during the pandemic (Turolla et al., 2020; Werneke et al., 2021) to improve accessibility to care despite the movement restrictions.
The current pandemic may bring forth a new era where telehealth becomes more significant and forms a vital service delivery platform for allied health professionals in the future (Negrini et al., 2020). Hence, this supports the relevance of a teleconsultation setting with standardised patients in our virtual assessment. The lack of exercise equipment provided during examination, albeit perceived as a limitation by students, could present a learning opportunity for students to react and cope in low-resource settings which is valuable to their future professional practice. In addition, the ability to assess students’ performance non-obtrusively allows a fair assessment with introducing unnecessary anxiety with the presence of assessor, which might be unavoidable in conventional OSCE stations (Ferreira et al., 2020). Therefore, VETA serves as a viable alternative that allows remote assessment of clinical competency in physiotherapy students.
C. Challenges with Implementation
VETA was conducted synchronously through Zoom platform within campus with students and SPs residing in different locations. Consequently, a reliable IT support structure and network connectivity was crucial to the success of the online assessment (Hopwood et al., 2021). Indeed, the connectivity issue has been reflected in this study where it has led to the loss of precious time for students to perform their teleconsultation. In this scenario, the examiner had to make a precise judgement to either (1) extend the timing and risk delays to the examination process, or (2) determine if there was enough “interaction content” to assess with and proceed with original scheduled time. Therefore, this underscores the need to include buffer time for similar situations when planning for virtual assessment.
Furthermore, the wearing of masks has resulted in the muffling of voices which prevented effective communication between students and SPs on the teleconferencing platform. Facial gestures and expression are known to play an important role in interpersonal communication, comprehension, and the delivery of intended messages and this can be affected by mask-wearing (Mheidly et al., 2020). To ensure that the SP is able to understand the prescription adequately, transparent face-masks could be worn to facilitate communication. Nonetheless, we advocate that allied health students should learn and master non-verbal communication skills as transparent face-masks may not be commonly used in clinical settings.
Time and space allocation have also been perceived to be inadequate. Based on students’ qualitative feedback, the perceived lack of time was pertaining to the interaction with the SP during exercise prescription, and not the duration for reading and planning. Pacing of speech, ensuring clarity and prioritising of information to convey are instrumental in time-effective clinical communication which students need to master (Laidlaw et al., 2014). Therefore, the timing of teleconsultation has to be optimised, not solely based on students’ expectations, but also on the assessment criteria and desired difficulty level. Furthermore, the time allocated should reflect the duration of an actual teleconsultation session where it has been reported in vascular telemedicine setting to be approximately 10 minutes (Baldwin et al., 2003), similar to the VETA format. Secondly, to ensure that SPs can perform exercise freely and safely, future runs of the assessment should cater for 20 to 50 square feet of space in the rooms, as recommended by American Council on Exercise (American Council on Exercise, 2009).
D. Study Limitations
In our study, only 39% of the total student cohort who undertook the VETA completed the survey. Hence, this may inadvertently create responders’ bias in the survey findings (e.g., those who had a positive experience may feel more motivated to participate). In our study, the evaluation survey was disseminated to students only a day after the conduct of VETA. Future studies may explore administering the survey immediately after the completion of the virtual assessment, via accessible QR codes or weblinks, to encourage greater participation rate.
Additionally, the assessment scope of VETA was limited to only a single domain of skill competency (safe exercise coaching and prescription) of the physiotherapy program and may not represent the relevance of such format for evaluating other competencies. As VETA has only been evaluated in one school setting, it remains to be ascertained if a similar format can be successfully adopted by other universities or a different structured health sciences program. Future studies may explore VETA’s implementation in other settings (i.e., evaluating other clinical competencies or conducted in other programs) and identify the potential facilitators and barriers to its adoption.
Despite the use of self-reported questionnaires to evaluate predetermined themes, the exploratory factor analysis has showed that the “effectiveness” component may not be reliably assessed by the items that were designated. To be an effective assessment, it also implies that the assessment has to mimic actual clinical settings and test skills relevant to a physiotherapist. Therefore, the same items have been correlated to the identified constructs such as clinical relevance (directly linked to assessment authenticity) and the value of assessment. Nonetheless, the distilled 13-item subset survey with good internal consistency can be employed to evaluate other novel assessments related to clinical competency.
E. Implications of a Virtual Approach
Virtual OSCE, while shown to be a useful examination format, cannot entirely replace the traditional OSCE in the assessment of physical skills which is required for allied health professional practice. For instance, hands-on skills such as manual therapy involving the massage, manipulation and mobilisation of muscles and joints, are critical to restore the patient’s functional capabilities and promote their self-efficacy (Bronfort et al., 2010). It is challenging to assess such components using virtual assessments. Specific to therapeutic exercises, it is vital to assess physical facilitation (provision of support and tactile cues) during coaching of exercise to frail individuals or patients with mobility limitations. This cannot be properly assessed without allowing physical close contact with the SPs.
Nonetheless, the success of VETA in this study highlights the feasibility of assessing specific clinical skills reliably using an online synchronous approach. When utilised in an appropriate context (e.g., for assessing online exercise prescription skills), the virtual assessment can help students gain literacy and confidence in online care delivery. At the same time, it allows them to appreciate and navigate the challenges in virtual care settings such as the lack of space or limited camera viewing angle identified in this study. With the COVID-19 pandemic, the demonstration of clinical competency over an online platform may prove to be as, if not more, relevant than traditional face-to-face assessments.
F. Looking Ahead: The Application and Value of Virtual Assessments
To understand how virtual assessments can play a bigger role in medical or allied health education, it is first important to identify which clinical skillsets and competencies are applicable or commonly used in telehealth settings. This can help in the selection of appropriate assessment to be used. Digital literacy and proficiency in the use of telehealth technologies should form a key component of undergraduate clinical education. The use of web-based or teleconferencing platforms for care delivery should also be included as part of their formal training as a healthcare professional. This will help equip the students with the relevant skills for the evolving digital world. There is also a need for a paradigm shift to not just rely on traditional OSCEs for clinical assessments, but to incorporate elements of technology and virtual care delivery relevant to telehealth practice wherever applicable.
V. CONCLUSION
While there are still technical difficulties to consider, our current model and examination setup provides an initial framework for others to adopt as an online synchronous method to assess clinical skills, especially during lockdowns or restricted periods. Furthermore, this VETA format may be used for distant learning and remote assessment of clinical competency for healthcare workers residing in rural areas (Palmer et al., 2015) or students on placement in medically underserved areas. As the use of virtual assessments removes geographical barriers, this allows other experienced teachers and faculty from external institutions to join as assessors or observers to calibrate and align assessment outcomes, thereby enhancing the overall quality of medical education across institutions. Taken together, the use of virtual clinical skills assessment is promising and should be carefully considered for integration into the current medical or allied health education system.
Notes on Contributors
TXR contributed to the study design, conceptualised VETA, conducted data collection and analysis, and drafted the manuscript. AG contributed to assessment design and results interpretation. CN devised the study, innovated the VETA format, conducted data collection and contributed to results interpretation. All authors have read and approved the final manuscript.
Ethical Approval
The study was exempted from ethical review with the use of anonymous surveys with no recording of any identifiable information. In line with the Declaration of Helsinki and the institutional IRB exemption criteria, the study presents minimal risk to participants, does not touch on sensitive topics, does not involve vulnerable population, and does not involve deception or withholding of study’s stated aims and objectives from participants.
Data Availability
Datasets generated and/or analysed during the current study are available from the following DOIs: https://doi.org/10.6084/m9.figshare.22641013
https://doi.org/10.6084/m9.figshare.22641115
https://doi.org/10.6084/m9.figshare.22640998
Acknowledgement
We would like to thank all the students and standardised patients who participated in this study.
Funding
The authors received no specific funding for this study.
Declaration of Interest
The authors report no conflicts of interest.
References
American Council on Exercise. (2009). American council on exercise: How to design a home gym. Retrieved April 4, 2022, from https://www.acefitness.org/resources/everyone/blog/6625/home-gym-design-how-to-design-a-home-gym/
American Educational Research Association. (2014). Standards for educational and psychological testing. American Educational Research Association.
Baldwin, L., Clarke, M., Hands, L., Knott, M., & Jones, R. (2003). The effect of telemedicine on consultation time. Journal of Telemedicine and Telecare, 9 Suppl 1, S71-73.
Barra-Ortiz, H. A. d. l., Gómez-Miranda, L. A., & Fuente-Astroza, J. I. d. l. (2021). Objective structured clinical examination (OSCE) to assess the clinical skills of physical therapy students when using physical agents. Revista de la Facultad de Medicina, 69(3), Article e83545.
Blythe, J., Patel, N. S. A., Spiring, W., Easton, G., Evans, D., Meskevicius-Sadler, E., Noshib, H., & Gordon, H. (2021). Undertaking a high stakes virtual OSCE (“VOSCE”) during Covid-19. BMC Medical Education, 21, Article 221. https://doi.org/10.1186/s12909-021-02660-5
Brennan, D. M., Mawson, S., & Brownsell, S. (2009). Telerehabilitation: Enabling the remote delivery of healthcare, rehabilitation, and self management. Studies in Health Technology and Informatics, 145, 231-248.
Bronfort, G., Haas, M., Evans, R., Leininger, B., & Triano, J. (2010). Effectiveness of manual therapies: The UK evidence report. Chiropractic & Osteopathy, 18, Article 3. https://doi.org/10.1186/1746-1340-18-3
Chen, D. E., Tay, E. K., Tan, P. L., Su, P., Koh, M. M., Ong, P. L., Chew, E., & Ng, Y. S. (2020). The impact of COVID-19 pandemic on rehabilitation in Singapore. Annals of the Academy of Medicine of Singapore, 49(11), 925-927. https://doi.org/10.47102/annals-acadmedsg.2020297
Chisnall, B., Vince, T., Hall, S., & Tribe, R. (2015). Evaluation of outcomes of a formative objective structured clinical examination for second-year UK medical students. International Journal of Medical Education, 6, 76-83. https://doi.org/10.5116/ijme.5572.a534
Cleland, J. A., Abe, K., & Rethans, J. J. (2009). The use of simulated patients in medical education: AMEE Guide No 42. Medical Teacher, 31(6), 477-486.
Deldar, K., Bahaadinbeigy, K., & Tara, S. M. (2016). Teleconsultation and clinical decision making: A systematic review. Acta Informatica Medica, 24(4), 286-292.
Deville, R. L., Fellers, C. M., & Howard, M. L. (2021). Lessons learned pivoting to a virtual OSCE: Pharmacy faculty and student perspectives. Currents in Pharmacy Teaching and Learning, 13(11), 1498-1502. https://doi.org/10.1016/j.cptl.2021.06.046
Downing, S. M. (2004). Reliability: On the reproducibility of assessment data. Medical Education, 38(9), 1006-1012.
Edwards, M., & Martin, A. (1989). The objective structured clinical examination as a method of occupational therapy student evaluation. Canadian Journal of Occupational Therapy, 56(3), 128-131.
Elo, S., & Kyngäs, H. (2008). The qualitative content analysis process. Journal of Advance Nursing, 62(1), 107-115.
Farahat, E., Rice, G., Daher, N., Heine, N., Schneider, L., & Connell, B. (2015). Objective structured clinical examination (OSCE) improves perceived readiness for clinical placement in nutrition and dietetic students. Journal of Allied Health, 44(4), 208-214.
Ferreira, É. d. M. R., Pinto, R. Z., Arantes, P. M. M., Vieira, É. L. M., Teixeira, A. L., Ferreira, F. R., & Vaz, D. V. (2020). Stress, anxiety, self-efficacy, and the meanings that physical therapy students attribute to their experience with an objective structured clinical examination. BMC Medical Education, 20(1), 296. https://doi.org/10.1186/s12909-020-02202-5
Fickenscher, K., & Pagliaro, J. A. (2021). Education in virtual care delivery: Clinician education and digital health literacy. Healthcare Information Technology for Cardiovascular Medicine, 111-125. https://doi.org/10.1007/978-3-030-81030-6_9
Fouad, S., Gouda, E., Nasser, A. A., & Kamal, D. (2019). Perception of students, staff and simulated patients towards objective structured clinical examination (OSCE). Education in Medicine Journal, 11(2), 27-42. https://doi.org/10.21315/eimj2019.11.2.4
Gormley, G. (2011). Summative OSCEs in undergraduate medical education. The Ulster Medical Journal, 80(3), 127-132.
Grover, S., Pandya, M., Ranasinghe, C., Ramji, S. P., Bola, H., & Raj, S. (2022). Assessing the utility of virtual OSCE sessions as an educational tool: A national pilot study. BMC Medical Education, 22(1), 178. https://doi.org/10.1186/s12909-022-03248-3
Hannan, T. A., Umar, S. Y., Rob, Z., & Choudhury, R. R. (2021). Designing and running an online objective structured clinical examination (OSCE) on Zoom: A peer-led example. Medical Teacher, 43(6), 651-655.
Harden, R. M., Stevenson, M., Downie, W. W., & Wilson, G. M. (1975). Assessment of clinical competence using objective structured examination. British Medical Journal, 1, 447-451. https://doi.org/10.1136/bmj.1.5955.447
Hopwood, J., Myers, G., & Sturrock, A. (2021). Twelve tips for conducting a virtual OSCE. Medical Teacher, 43(6), 633-636.
Hsieh, H. F., & Shannon, S. E. (2005). Three approaches to qualitative content analysis. Qualitative Health Research, 15(9), 1277-1288.
Jo, K. H., & An, G. J. (2014). Qualitative content analysis experiences with objective structured clinical examination among Korean nursing students. Japan Journal of Nursing Science, 11(2), 79-86.
Khan, K. Z., Ramachandran, S., Gaunt, K., & Pushkar, P. (2013). The objective structured clinical examination (OSCE): AMEE Guide No. 81. Part I: An historical and theoretical perspective. Medical Teacher, 35(9), e1437-1446.
Kumar, A., Sarkar, M., Davis, E., Morphet, J., Maloney, S., Ilic, D., & Palermo, C. (2021). Impact of the COVID-19 pandemic on teaching and learning in health professional education: A mixed methods study protocol. BMC Medical Education, 21(1), 439. https://doi.org/10.1186/s12909-021-02871-w
Laidlaw, A., Salisbury, H., Doherty, E. M., & Wiskin, C. (2014). National survey of clinical communication assessment in medical education in the United Kingdom (UK). BMC Medical Education, 14, 10. https://doi.org/10.1186/1472-6920-14-10
Liang, Z. C., Ooi, S. B. S., & Wang, W. (2020). Pandemics and their impact on medical training: Lessons from Singapore. Academic Medicine, 95(9), 1359-1361. https://doi.org/10.1097/acm.0000000000003441
Lovink, A., Groenier, M., van der Niet, A., Miedema, H., & Rethans, J. J. (2021). The contribution of simulated patients to meaningful student learning. Perspectives on Medical Education, 10(6), 341-346. https://doi.org/10.1007/s40037-021-00684-7
Major, S., Sawan, L., Vognsen, J., & Jabre, M. (2020). COVID-19 pandemic prompts the development of a web-OSCE using Zoom teleconferencing to resume medical students’ clinical skills training at Weill Cornell Medicine-Qatar. BMJ Simulation & Technology Enhanced Learning, 6(6), 376-377. https://doi.org/10.1136/bmjstel-2020-000629
Mheidly, N., Fares, M. Y., Zalzale, H., & Fares, J. (2020). Effect of face masks on interpersonal communication during the COVID-19 pandemic. Frontiers in Public Health, 8. https://doi.org/10.3389/fpubh.2020.582191
Negrini, S., Kiekens, C., Bernetti, A., Capecci, M., Ceravolo, M. G., Lavezzi, S., Zampolini, M., & Boldrini, P. (2020). Telemedicine from research to practice during the pandemic. “Instant paper from the field” on rehabilitation answers to the COVID-19 emergency. European Journal of Physical and Rehabilitation Medicine, 56(3), 327-330. https://doi.org/10.23736/s1973-9087.20.06331-5
Norman, G. (2002). Research in medical education: Three decades of progress. British Medical Journal, 324(7353), 1560-1562. https://doi.org/10.1136/bmj.324.7353.1560
Palmer, R. T., Biagioli, F. E., Mujcic, J., Schneider, B. N., Spires, L., & Dodson, L. G. (2015). The feasibility and acceptability of administering a telemedicine objective structured clinical exam as a solution for providing equivalent education to remote and rural learners. Rural Remote Health, 15(4), 3399.
Pettit, M., Shukla, S., Zhang, J., Sunil Kumar, K. H., & Khanduja, V. (2021). Virtual exams: Has COVID-19 provided the impetus to change assessment methods in medicine? Bone & Joint Open, 2(2), 111-118. https://doi.org/10.1302/2633-1462.22.BJO-2020-0142.R1
Prettyman, A. V., Knight, E. P., & Allison, T. E. (2018). Objective structured clinical examination from virtually anywhere! The Journal for Nurse Practitioners, 14(8), e157-e163. https://doi.org/10.1016/j.nurpra.2018.05.007
Rickles, N. M., Tieu, P., Myers, L., Galal, S., & Chung, V. (2009). The impact of a standardized patient program on student learning of communication skills. American Journal of Pharmaceutical Education, 73(1), 4.
Shirwaikar, A. (2015). Objective structured clinical examination (OSCE) in pharmacy education – a trend. Pharmacy Practice, 13(4), 627-627. https://doi.org/10.18549/PharmPract.2015.04.627
Silva, C. C., Lunardi, A. C., Mendes, F. A., Souza, F. F., & Carvalho, C. R. (2011). Objective structured clinical evaluation as an assessment method for undergraduate chest physical therapy students: A cross-sectional study. Brazilian Journal of Physical Therapy, 15, 481-486.
Stamenova, V., Chu, C., Pang, A., Fang, J., Shakeri, A., Cram, P., Bhattacharyya, O., Bhatia, R. S., & Tadrous, M. (2022). Virtual care use during the COVID-19 pandemic and its impact on healthcare utilization in patients with chronic disease: A population-based repeated cross-sectional study. PLOS ONE, 17(4), Article e0267218. https://doi.org/10.1371/journal.pone.0267218
Tan, X. R., & Ng, C. L. W. (2022, January 20-21). Perceptions of allied health students and standardised patients towards virtual exercise teleconsultation assessment (VETA) during COVID-19. Applied Learning Conference 2022, Singapore.
Turolla, A., Rossettini, G., Viceconti, A., Palese, A., & Geri, T. (2020). Musculoskeletal physical therapy during the COVID-19 pandemic: Is telerehabilitation the answer? Physical Therapy, 100(8), 1260-1264. https://doi.org/10.1093/ptj/pzaa093
Watkins, M. W. (2018). Exploratory factor analysis: A guide to best practice. Journal of Black Psychology, 44(3), 219-246.
Werneke, M. W., Deutscher, D., Grigsby, D., Tucker, C. A., Mioduski, J. E., & Hayes, D. (2021). Telerehabilitation during the COVID-19 pandemic in outpatient rehabilitation settings: A descriptive study. Physical Therapy, 101(7). https://doi.org/10.1093/ptj/pzab110
Wessel, J., Williams, R., Finch, E., & Gémus, M. (2003). Reliability and validity of an objective structured clinical examination for physical therapy students. Journal of Allied Health, 32(4), 266-269.
Zayyan, M. (2011). Objective structured clinical examination: The assessment of choice. Oman Medical Journal, 26(4), 219-222. https://doi.org/10.5001/omj.2011.55
*Tan Xiang Ren
SIT Dover Campus,
10 Dover Drive,
Singapore 138683
Email: XiangRen.Tan@singaporetech.edu.sg
Submitted: 12 June 2023
Accepted: 24 October 2023
Published online: 2 April, TAPS 2024, 9(2), 81-86
https://doi.org/10.29060/TAPS.2024-9-2/SC3066
Lean Heong Foo1, Nurul Haziqah Binte Suhaimi2, Saudha Binte Sadimin2, Marianne Meng Ann Ong1
1Department of Restorative Dentistry, National Dental Centre, Singapore; 2Dental Assisting, National Dental Centre, Singapore
Abstract
Introduction: An online survey was conducted on 16 National Institute of Technical Education Certificate (NITEC) Dental Surgery Assistant (DSA) trainees in National Dental Centre Singapore to find out their perceptions and understanding of mental well-being.
Methods: The 43-item survey included (i) Psychological General Well-being Index (PGWB) with 22 items based on 6 domains (anxiety, depression, positive well-being, self-control, general health, and vitality); (ii) 5 items on mental health knowledge; (iii) 4 items on lifestyle; and (iv) 12 items on perceptions of mental well-being and working in the dental clinic. Responses were collated for descriptive analysis and Cronbach’s alpha analysis was done for internal consistency for Likert scale items.
Results: The average PGWB score was 61.5 (range 18-89). Fourteen trainees (75%) indicated they were feeling depressed and 31.2% of trainees felt under stress in the past month. The majority (81.3%) of trainees recognised the role of exercise in maintaining mental health and 75% of trainees were able to differentiate between sadness and depression. However, 56.3% and 87.5% of the trainees incorrectly answered that mental and psychological disorders are not preventable conditions and mental disorders are caused by a wrong way of thinking respectively. The Cronbach’s alpha on PGWB (a = 0.87) and trainees’ perception of working in the clinic (a = 0.76) revealed good internal consistency.
Conclusion: The PGWB scores and survey analysis indicate there is a knowledge gap about mental health and the need to improve mental well-being in this cohort of NITEC DSA trainees.
Keywords: Mental Well-being, Dental Surgery Assistant Trainee, Psychological General Well-being Index
I. INTRODUCTION
In National Dental Centre Singapore (NDCS), Dental Surgery Assistant (DSA) trainees are required to complete a 1-year National Institute of Technical Education Certificate (NITEC) DSA programme to be qualified as a DSA. Similar to the training of dental students, DSA trainees undergo a significant transition from learning in a classroom setting (4 weeks pre-clinical didactic and observation) to a high-stress dental clinic work environment (clinical) when they start on-the-job training 1 month after commencing their programme. During this transition period, they need to multi-task and adapt to new clinical responsibilities related to infection control, patient management, and assisting clinicians. It has been reported that 80% of 299 Israeli DSAs suffered from a high level of burnout where the most stressful work-related factors were low income, high workload, and work hazards (Uziel et al., 2019). A survey was thus conducted to gain insights into the perceptions of mental well-being and working in the dental clinic among NDCS’s NITEC DSA trainees. This was a needs analysis survey done in June 2022 for a mental wellness module that aimed to provide support to DSA trainees enrolled in the 1-year NITEC DSA programme.
II. METHODS
An online anonymous survey with written consent was disseminated via Form.SG to the 2022 cohort of DSA trainees to complete three months after starting their 1-year programme. The 43-item survey included (i) Psychological General Well-being Index (PGWB) with 22 items based on 6 domains (anxiety, depressed mood, positive well-being, self-control, general health and vitality) (Dupuy, 1984); (ii) 5 items on knowledge about mental health; (iii) 4 items on lifestyle; and (iv) 2 items on perception of mental well-being (adapted from Puspitasari et al., 2020) and 10 items on working in a dental clinic (crafted based on NDCS context). DSA trainees rated their level of agreement based on a 6-point Likert scale for PGWB (5 -most favourable response to 0 – unfavourable response) and a 5-point Likert scale for the perception of mental health and working in a dental clinic (5 – strongly agree to 1 – strongly disagree). The PGWB score ranges from 0 to 110, effectively representing an individual’s comprehensive subjective well-being. Additionally, the six dimensions of the PGWB index provide valuable insights into the subjective well-being associated with each specific dimension. The survey responses were collated for descriptive analysis and Cronbach’s alpha analysis was done for internal consistency for Likert scale items.
III. RESULTS
The entire cohort of sixteen DSA trainees {all female; age 17-50, mean 28.19 (23.39-32.99)} completed the online survey (100% response rate). The data of this study are openly available in the Figshare repository at http://doi.org/10.6084/m9.figshare.23501136.
Only 25% of trainees (4/16) had more than 1 year of prior working experience in a dental clinic. Their collated responses based on their second-month experience of the 1-year programme are as follows:
A. Psychological General Well-being Index (PGWB)
The average PGWB score for this cohort was 61.5 (range 18-89, 95% CI 52.80 – 70.20), indicating lower than average general well-being in this cohort {normal range 68-83 (Dupuy, 1984)}. No significant correlation was found between age and dental clinic experience on PGWB (r=-0.03; -0.06). The Cronbach’s alpha in PGWB (a = 0.93) indicated good internal reliability with a good individual domain analysis of 0.85 for all the domains (Appendix A: Table 1, Figures 2 and 3).
1) General health: The trainees achieved a mean score of 8.94 (Range 0-15) in general health. The majority (68.75%, 11/16) of trainees agreed they felt healthy enough to function.
2) Positive well-being: The trainees experienced a lower than moderate level of positive emotion and life satisfaction with a mean score of 9.94 (Range 0-20). Only 5 out of 16 trainees (31.25%) were happy with their personal life most of the time.
3) Self-control: The trainees possessed a moderate to higher level of self-control in regulating their behavior and emotions (mean 56, Range 0-15). However, about half of the cohort (56.25%, 9/16) admitted they felt a lack of control over their action in the past month.
4) Vitality: The trainees exhibited a moderate level of energy and vitality (mean 10.31, Range 0-20). However, 7 trainees (43.75%) admitted they felt worn out and exhausted most of the time in the past month.
5) Depressed mood: The trainees, on average, experienced a relatively moderate level of depressive symptoms in the past month (mean:88, Range 0-15). Fourteen trainees (75%) admitted they were feeling depressed and 31.2% of trainees (5/16) had felt under stress in the past month.
6) Anxiety: The trainees exhibited a moderate level of anxiety (mean 12.88, Range 0-25). Majority (81.25%, 13/16) of trainees admitted they felt high-strung quite a good bit of time in the past month.
B. Knowledge about Mental Health
Majority of DSA trainees (81.3%, 13/16) recognised the role of exercise in maintaining mental health and 75% (12/16) of trainees were able to differentiate between sadness and depression. However, 56.3% (9/16) of the trainees incorrectly answered that mental and psychological disorders are not preventable conditions, and a majority (87.5%, 14/16) incorrectly answered that mental disorders are caused by a wrong way of thinking (Appendix B).
C. Lifestyle
Half of the cohort exercised at least once a week. Only 50% of the cohort had self-care activities for themselves. Majority of the trainees (15/16) did not meditate and 50% of the trainees sought help from their friends and family when necessary (Appendix B).
D. Perception of Mental Well-being and Working in a Dental Clinic
Majority of the trainees also gave a neutral response (75%, 12/16) to the statement related to stress from working in the dental clinic. Majority agreed that mental health is important for their general health (87.5%, 14/16). Only half of the cohort indicated they were comfortable to work in the dental clinic (56.3%, 9/16) (Figure 1). About ¾ of the cohort believed they could complete the training programme and were confident to perform the on-the-job training (75%, 12/16). Majority (81.3%, 13/16) were willing to seek help if they encountered problems working in the dental clinic (Figure 1). The Cronbach’s alpha of trainees’ perceptions of working in the clinic (a = 0.76) revealed good internal consistency.

Figure 1. Perceptions of DSA trainees of mental well-being and working in the dental clinic in the second month of their 1-year programme
IV. DISCUSSION
Mental well-being is associated with one’s ability to cope with normal stresses of life and work productivity. This is particularly important in health professionals, including DSAs, to ensure the quality of patient care and professional satisfaction. To our knowledge, this is the first local survey to investigate DSA trainees’ perceptions of mental well-being and working in the dental clinic. The PGWB analysis revealed this cohort of DSA trainees had a lower-than-normal score that was even lower than a group of 320 Japanese dental students (61.5 versus 68.63) (Sugiura et al., 2005). Additionally, the trainees also demonstrated moderate levels of depression and anxiety, with a detailed analysis indicating a significant number experiencing stress. This observation highlighted the transition from pre-clinical to clinical training phase can be challenging and stressful with increased workload and responsibility, as evident among DSAs who demonstrated a moderate level of professional burnout (Uziel et al., 2019). A similar trend was observed in this transition phase for dental students, where stress was associated with increased responsibility and demands associated with caring for real patients (de Souza Ferreira et al., 2023). Despite the difference in curriculum and a larger student cohort, the Japanese dental students (Sugiura et al., 2005) appeared to cope with their training better as their PGWB revealed they were more relaxed (Anxiety 16.43 versus 12.88) and cheerful (Depression 11.24 versus 9.88) compared with our DSA trainees. This finding reflects the need for providing mental well-being support for our DSA trainees in their programme.
The misconceptions about mental health and infrequent self-care practices among trainees suggest a lack of awareness of mental wellness. Implementing a mental wellness module focusing on positive psychology, coping techniques like breathing exercises and meditation, and resource awareness can help address these issues. The Trainees’ willingness to seek help and recognise exercise’s role in mental health shows openness to support and intervention. Our pilot data is constrained by a small sample size and the absence of a control group for comparison, making it insufficient for general population inferences. The limitation of PGWBI includes only 6 dimensions and the potential of bias due to self-reported data. Future recommendations involve re-evaluating the impact of the mental wellness module at the end of the 1-year program, inclusion of qualitative data, and establishing a supportive work environment with accessible mental health resources and mentorship to enhance the well-being and job satisfaction of DSAs.
V. CONCLUSION
In conclusion, the survey findings from this small cohort of DSA trainees underscore the importance of addressing mental health and well-being in this group of learners. The high prevalence of depressive symptoms and reported stress among the trainees highlights the need for targeted interventions and support systems to promote mental well-being. Hence, a mental wellness module will be introduced to this cohort of DSA trainees and this survey will be repeated 3 months after the module completion to assess any changes in this cohort’s perception of mental well-being and working in the dental clinic.
Notes on Contributors
FLH reviewed the literature, contributed to the study conception, data acquisition, and data analysis, drafted, and critically revised the manuscript.
NHS contributed to the data acquisition, data analysis, and critically revised the manuscript.
SS contributed to the data acquisition, data analysis, and critically revised the manuscript.
MO contributed to the study conception, data acquisition and critically revised the manuscript. All authors gave their final approval and agreed to be accountable for all aspects of the work.
Ethical Approval
This study was exempted from the formal Centralised Institutional Review Broad review by SingHealth Institutional Review Board (CIRB Ref: 2022/2122).
Data Availability
The data that support the findings of this study are openly available in the Figshare repository http://doi.org/10.6084/m9.figshare.23501136.
Acknowledgement
We would like to thank Ms Liu Yanting for her help in data preparation and collection.
Funding
There was no funding involved in the preparation of the manuscript.
Declaration of Interest
The authors declare no conflict of interest.
References
de Souza Ferreira, F., Barros, I., da Costa Neves, T., Pazos, J. M., & Garcia, P. P. N. S. (2023). Stress amongst dental students in the transition from preclinical training to clinical training: A qualitative study. European Journal of Dental Education. 27(3), 568-574.
Dupuy, H. J. (1984). The Psychological General Well-Being (PGWB) index. In: Wenger NK, Mattson ME, Furberg CF, & Elinson J (Eds). Assessment of quality of life in clinical trials of cardiovascular therapies. 170-183. Le Jacq.
Puspitasari, I. M., Garnisa, I. T., Sinuraya, R. K., & Witriani, W. (2020). Perceptions, knowledge, and attitude toward mental health disorders and their treatment among students in an Indonesian university. Psychology Research and Behaviour Management, 27(13), 845-854.
Sugiura, G., Shinada, K., & Kawaguchi, Y. (2005). Psychological well-being and perceptions of stress amongst Japanese dental students. European Journal of Dental Education. 9(1),17-25.
Uziel, N., Meyerson, J., Birenzweig, Y., & Eli, I. (2019). Professional burnout and work stress among Israeli dental assistants. Psychology, Health & Medicine, 24(1), 59-67.
*Foo Lean Heong
National Dental Centre Singapore
5, Second Hospital Avenue
168938 Singapore
Email: foo.lean.heong@singhealth.com.sg
Submitted: 30 May 2023
Accepted: 24 October 2023
Published online: 2 April, TAPS 2024, 9(2), 60-69
https://doi.org/10.29060/TAPS.2024-9-2/OA3062
Mary XiaoRong Chen1 & Dora Howes2
1Health and Social Sciences, Singapore Institute of Technology, Singapore; 2Nursing & Health Care School, School of Medicine, Dentistry & Nursing, University of Glasgow, United Kingdom
Abstract
Introduction: Nurses’ professional identity is important for their career orientation and clinical practice. This study explored Singaporean nurses’ perceptions of professional identity. The results provide an understanding of how guided learning and reflection could help nurses in their professional identity formation and development.
Methods: Using an exploratory descriptive qualitative research study and purposive sampling by researchers teaching in the programme, 64 Registered Nurses with a diploma qualification pursuing a Bachelor of Science degree with Honours in Nursing programme in Singapore were invited to participate. They responded to open ended survey questions online, which were analysed using a thematic analysis. Ethical approval was obtained.
Results: All 64 first year students were invited to participate at the start of the module and upon the completion. The response rates were 94% and 81% respectively. Two overarching themes – “nurses as professionals with knowledge and moral character” and “the construction of professional identity” – emerged from the data.
Conclusion: The nurses perceived their professional nursing identity as a construct comprised of knowledge and moral characteristics, which is consistent with international literature. A professional nursing identity, relationships with other healthcare professionals, patients and confidence in practice were all interrelated. Guided reflection and discussion on clinical experiences and social interactions helped students become aware of their professional identity and responsibilities. Such purposive educational effort needs to be started early and supported through the students’ educational journey into clinical practice.
Keywords: Professional Identity of Nursing, Singapore Nurses, Image of Nursing, Social Perception of Nursing in Singapore, Nurse Education
Practice Highlights
- Professional nursing identity can be facilitated by guided reflection.
- Purposive educational effort needs to be started early and continued in clinical practice.
- Awareness of professional identity relates to practice, relationship and professional development.
I. INTRODUCTION
A. Background
Professional identity is ‘one’s professional self-concept based on attributes, beliefs, values, motives, and experiences’ (Slay & Smith, 2011, p85). This study explored the perceived professional identity a group of Registered Nurses (RNs) pursuing a top-up bachelor’s degree in nursing.
The development of professional identity is an ongoing narrative shaped by work, experience and nurses’ sense of ownership (Mao et al., 2021). It is a construct comprised of personal values and beliefs fused with the expectations of society and the profession, which are in turn reflected in the values and ethics of professional practice (Crigger & Godfrey, 2014). It is a difficult concept to define and convey causing confusion for educators in how best to guide novice nurses (Fitzgerald & Clukey, 2022). As research evidence on how nurses can elicit their professional identity through guided reflection is lacking, this study aims to offer educators an important teaching strategy in their toolkit.
Deppoliti (2008) found that nurses with a strong professional identity provided better patient care and developed higher competencies than those nurses who did not. Similarly, Clements et al. (2016) found that affirmation of professional identity facilitated a deeper sense of self-worth and belonging in nurses who were more committed to their careers as a result. Besides job commitment, a strong professional identity enhances job satisfaction and reduces burnout level (Sabanciogullari & Dogan, 2015). All are important in a climate of nursing shortage. In Singapore, the local nurse attrition rate was reported at 7.4% in 2021, the highest in five years due to workload and stress (Goh, 2022).
The transition of pre-registration nurse education to Higher Education Institutes in the 1990’s, reduced opportunities for students to socialise with experienced staff, impacting the development of professional identity (Bartlett, 2015; Marique & Stinglhamber, 2011). In Singapore, other than the twelve-week consolidation Pre-Registration Clinical Practice and the Transition to Practice programme at the National University of Singapore, clinical placements are mostly focused on attaining nursing skills with two to three weeks duration being the norm. These touch and go kinds of clinical placements do not give students sufficient time to form significant relationships with the clinical nurses, thereby affecting their practice experience and perceived professional identity (Chen, 2020).
In recent years, Singaporean nurses have taken roles such as Advanced Practice Nurses (APN), which require more sophisticated knowledge, clinical experience and enhanced autonomy to practice (Ministry of Health, 2012). However, there is a lack of awareness of their training, abilities, and roles by the public and other healthcare professionals (Woo et al., 2020; Xu et al., 2022). Ten Hoeve et al. (2014) highlight that nurses are responsible to project their own public image. When there is a lack of communication from the professionals on their roles, the public is influenced by the media, which often focuses on practice failures (Girvin et al., 2016; Peate, 2016). Mistakes made by a minority of nurses tend to be perceived by the public as the ‘typical nurse’ and nursing practice in general without understanding the context (Hoyle et al., 2017).
Such inertia creates a cyclical situation whereby nurses draw their professional identity from their public image and when portrayed negatively, are less likely to communicate their professionalism in return. As professional identity is such a complicated construct, students need guided reflection on their professional experiences, to develop professional values and affirm their professional identity. Such awareness is necessary to facilitate public dialogue and deliberation and portray professional image in a more positive and accurate manner.
Nurse education, being the catalysing process of converting a layperson into an individual whose values and beliefs are consistent with those of the professionalisation, should take action (Benner et al., 2009; Clouder, 2003; Johnson et al., 2012). Black (2014, p118) discussing the goal of nursing education argued:
“Nursing education is not simply teaching you the tasks of nursing…the overriding goal of your education is to teach you to think like a nurse, to see the world of healthcare through the lens of nursing…”
Fostering a positive professional identity is an imperative within nursing education (Clements et al., 2016). This research offers a strategy to realise such an aim.
B. Study Context
Nursing schools in Singapore follow Singapore Nursing Board’s (SNB) guideline regarding the development of students’ reflective thinking skills and professional identity (Singapore Nursing Board, 2011). However, the character and psychological aspects of nursing professional identity, such as integrity, compassion and courage, are often learnt through the hidden curriculum in practice as opposed to explicit guided reflection in classrooms. Students need guidance to reflect on their clinical practice and social encounters, and hence commit to the process of reflection as an integral feature of professional life (Fitzgerald & Clukey, 2022).
Realising such an educational priority, a module was designed to facilitate students’ professional identity development in a Bachelor of Science degree with Honours in Nursing programme in one of the higher education institutes in Singapore. This post-registration degree programme is offered jointly by a Singapore university and an overseas university, admitting students who have completed their Diploma in Nursing and are registered with the SNB.
To support the students in developing their concepts of nursing professionalism and practice, they were guided in gaining a critical understanding of nursing knowledge, reflective models, and methods. Table 1 shows the teaching and learning activities. Forming small groups, students set ground rules of respect and confidentiality at the initial meeting. Facilitators started by sharing and reflecting on their own critical clinical experiences, including mistakes made and what they learnt from them, to help build trust and make students feel safe to share their stories.
|
Lecture/seminar |
Guided Small Group Discussion |
|
Nursing knowledge, professional development |
Discusses nursing knowledge and theories, professionalisation, history of nursing and Singapore nursing
|
|
Skills and attributes in reflective thinking; Reflective models |
Self-awareness: Johari’s window, clarify values, life map Reflection in clinical teaching and learning
|
|
Reflection, thinking and knowing |
My critical moment: attention to details, emotion and feelings, analysis of the situation, learning points, plan for future
|
|
Purpose, value, reason and ethical issues in practice |
Reflective case-study: description, critical analysis, recognise value and ethical conflicts
|
|
Me, other healthcare professionals, society and self-growth |
Reflect on quality care, patient safety, my role and multidisciplinary team; SNB guidelines and standards, Singapore Medical Council guidelines and Allied Health Professions Council Act
|
|
Professional power and position |
Being a reflective practitioner and collaborate with others
|
Table 1. Teaching and learning activities
Lectures and seminars covered important concepts to prepare the students for group discussions. The group facilitators guided students to first describe their experiences clearly, and then explore and acknowledge their emotions and feelings. Negative emotions such as shame, hurt, resentment and regret were acknowledged and considered integral to the spectrum of human emotions. From there, students were guided to explore the cause of their emotions. Once highlighted, an in-depth literature review was undertaken to help students make decisions on personal and professional learning strategies.
An understanding of self and professional identity can help students affirm their professional role and career commitment (Sather, 2020). These guided reflective thinking activities enabled students to reach a new and deeper understanding of their beliefs and values, as well as the socio-cultural, professional, and personal background underpinning them.
Having created a student-centred module based on their learning experiences, this study was initiated to understand their perceived professional identity and the impact on practice. The research questions were:
(1) What are Singapore Nurses’ perceptions of Professional Identity?
(2) What is the impact of their perceived professional identity on practice?
II. METHODS
A. Methodology
Adopting the exploratory descriptive qualitative approach to explore under researched topics detailed by Hunter et al. (2019), this study explores Singapore nurses’ professional identity, to offer an initial understanding of this concept.
B. Study Sample
A purposive sample of all first-year students in 2018 was invited to participate. Eligibility criteria included: age above 21 years old, having a pre-registration Diploma in Singapore, RN registered with the SNB and enrolled in the module. All 64 students met these criteria. Most students were in their early twenties from Chinese, Malay, Indian and other ethnic groups. Gender split was 73% females to 27% males, while 45% had above six months of clinical experience. Their particulars are shown in Table 2.
|
Gender |
Male |
16 |
|
Female |
48 |
|
|
Age (Years) |
21 – 25 |
42 |
|
26 – 30 |
19 |
|
|
> 30 |
3 |
|
|
Ethnic |
Chinese |
37 |
|
Malay |
18 |
|
|
Indian |
7 |
|
|
Others |
2 |
|
|
In practice as RN |
Fresh graduates |
35 |
|
Less than 1 year |
10 |
|
|
1-3 years |
12 |
|
|
>3 years |
7 |
Table 2. Participant particulars
C. Ethical Consideration
The study was approved by the University’s Ethics Committee. Students were informed of the study and given the opportunity to ask questions. They were assured that their decision to participate was entirely voluntary and not linked to their academic performance in any way. The students were provided with a research information sheet clearly describing the purpose of the study and their involvement along with the consent form. They were given time to consider their decision. Each student was assigned a code which was kept separately from the data in a locked drawer. Any information that could lead to a student’s identification was rephrased or removed.
D. Data Collection
The complexity of the concept of professional identity meant it would have been confusing to ask the students the research question verbatim. Consequently, the questions were phrased in a way that was more intuitive for students to understand. They were:
- When you think of professionalism, what image or word comes into your mind?
- What is the effect of professional identity on your practice?
Those who agreed to participate were sent the online survey questions. This approach was adopted as the students were still new to the programme and likely to feel overwhelmed and less inclined to be authentic if interviewed. The online survey was carried out at the start and the end of the module. The purpose of the two-point data collection was to consider the students’ learning and ongoing reflection and to provide them with the opportunity to answer the questions comprehensively. A quiet classroom in school was offered to those wishing to avail themselves of it at each data collection point.
E. Data Analysis
All submitted responses were included for analysis using the thematic analysis approach described by Braun and Clarke (2012). The first author (MC) familiarised herself with the data by reading the narratives and coded the entire data set. Codes were applied to sections with similar meanings, which were then categorised, clustered and organised into themes. The indexed data were linked to the actual transcripts to demonstrate a clear audit trail (Braun & Clarke, 2006).
A second round of data analysis was carried out by the same author four weeks later to allow a more in-depth analysis, identification of consistencies and clarification of any discrepancies. According to Miles et al. (2019), a time lapse between the two analyses allows the researcher to look at the data afresh and minimise the potential for bias and assumptions. In so doing, it enhances the rigour of the analysis and the credibility of the findings.
The second author triangulated the data analysis by synthesising codes into themes and linking them to the original data to contextualise their meaning. The two authors then met to reach a consensus on the themes. The refining process of Theme One is shown in Tables 3 and 4. Table 3 shows the initial thematic analysis, while Table 4 illustrates the finalised themes.
|
Theme |
Subtheme |
Codes |
|
Theme 1: Professional Characteristics |
Knowledgeable and good attributes
|
Expert knowledge Science and the arts Communication Able to teach Intelligent Patient Understanding Caring Control emotion Non-judgmental Sacrifice Gratefulness Positive Trustworthy |
Table 3. Initial theme one with subthemes and codes
|
Themes |
Subthemes |
Codes |
|
Theme 1: Professionals with knowledge and moral character |
Knowledgeable |
Expert knowledge Communication Intelligent |
|
Moral character |
Understanding Caring Control emotion Sacrifice Positive Trustworthy |
|
|
Theme 2: The construction of professional identity
|
A social perception
|
As a ruler Traditional image The classes of professional Being respected (negotiated) Vibes of being superior
|
|
Identity challenges
|
Being watched and monitored Power position Source of negativity Boundary and roles
|
|
|
Realising their role in the construction of professional identity |
Advocate self Long journey learning to be one Hard work in making one Not to lose faith |
Table 4. Finalised themes, subthemes and codes
III. RESULTS
All 64 students agreed to participate and signed the consent form. The response rate at each collection point was 94% and 81% respectively. While the reason for the drop is not clear, it is possible that the demands from competing modules at the time of the second survey were influential.
Two overarching themes emerged (Table 4). The first, “Nursing profession is perceived as a profession with knowledge and moral character” stood out clearly from the responses given. It encompassed the subthemes of knowledge and moral character. The second theme – “The construction of professional identity” – elicited codes that made up the subthemes of social factors, identity challenges and nurses’ role in the construction of their professional identity.
Theme 1. Professionals with Knowledge and Moral Character
Students perceived a professional nurse as someone with a “good character, and capable of knowing” and “doing what was needed with self-control and discipline”. The theme was supported with two subthemes – ‘knowledge’ and ‘moral character’.
1) Knowledge: The students believed a professional nurse needed to engage in learning throughout their professional lifetime. A knowledgeable nurse was described as “knowing the job well” and “having special knowledge and being able to perform well”. The knowledgeable nurse could create new knowledge through study as exemplified in the quote below.
“…Professionalism is the outcome of a work that can have both the elements of arts and science …. been thoroughly sorted out to create knowledge that could be of relevance to the present study or development for future studies.”
(S37)
2) Moral character: The moral character of a professional nurse encompasses the moral agency demonstrated in his/her daily practice. A nurse needed to be “someone with good virtues and moral values” and uphold “ethical conduct and practice contentiously beyond any selfish thoughts”. The quotes below indicate some of these moral characteristics:
“Nursing is a job that is not meant for anyone, it takes dedication, strength and passion to be one.”
(S44)
“Because we work together as a team, it is important to trust each other based on the individual training that we had gone through and are able to carry out our duties well. It also serves as a form of accountability to people in our team and people receiving care from us”
(S08)
Students were clearly aware of the ethical code expected of them, which was reassuring in terms of the pre-registration education received.
Theme 2. The Construction of Professional Identity
This theme illuminated how the students viewed the construction of their professional identity. Three subthemes including ‘a social perception’, ‘identity challenges’ and ‘realising their role in the construction of professional identity’ were elicited.
1) A social perception: The students’ perception of their professional identity was influenced by the images and values directed towards nursing by society in comparison to other professions. The students perceived doctors, lawyers, and teachers as well-respected professionals. Doctors were “in a white coat with a stethoscope around their neck with confidence” while lawyers and teachers had “nice and neat suits” and were deemed to be “a sage or Master Yoda”, or “a confident global speaker”, “the force is within them”, or “have an aura of superiority, authority and power”. In contrast, the students viewed themselves as engaging in a “low skill/dirty job and of lower social status” due to the nature of the essential care they delivered daily. Such socially perceived images of being a professional were internalised resulting in the projection of a poor perception of their care work and image, as indicated here.
“When the word professionalism…the image of a doctor comes to my mind…portrayed as a superior figure as compared to a nurse… they (patients) will usually turn for help from [the] doctors as they perceive that doctor[s] have all the information and knowledge…parents also encourage or advise their children to become doctors…
(S17)
2) Identity challenges: Closely linked to social perception, the students encountered identity challenges from their interactions with people around them. They noted the development of special relationships with patients while remaining deferential to doctors. Some students also felt the process of professionalisation was akin to a sorting method, which differentiated professionals into higher or lower social status. Such relationships caused confusion and challenged their professional identity as the following quotations exemplify.
“I think that by having professional identity…only favours the doctors… Even if nurses make the right decision and doctors are wrong in the case, patients will still think that doctors are always right.”
(S17)
“The effect of professional identity in our practice is that the people around us may or may not get [us] respected. For example, in front of the doctors, we would portray like a maid who just do as what they say. However, in front of patients, we are their healthcare advocates which they listened to. Thus, it is a mixture of set of identity…”
(S28)
3) Realising their role in the construction of professional identity: The guided reflection created a safe space and provided methods for students to learn from their own and others’ experiences. As the module progressed, students came to realise their roles and their relationship with other professionals, as well as their responsibility in constructing their professional identity and how this identity was then portrayed to others. The quotes below offer some examples:
“The effects of the professional identity are how you portray the occupation to the world. People tend to judge the occupation by the way we portray ourselves.”
(S63)
“I value my role as a nurse as I feel that nurses can play a lot of roles…versatile, as nurses have greater knowledge than patients think. Also, nurses have judgment and good assessment skills so that we can identify what is not right with patients right away.”
(S17)
At a wider level, the students portrayed an optimistic outlook on their professional status with reference to the approved prescription rights to APNs in Singapore (Liew, 2018). The students felt their devotion towards patients led to them gaining wider trust and respect, as shown here:
“I valued the fact that my role gave me a sense of responsibility to advocate to the best of my patient’s interest. And the fact that more people are approaching nurses for advice makes me feel that we have slowly gained public trust on nurses.”
(S64)
The students believed that mutual respect was essential for quality patient care, positive relationships, and the affirmation of their professional identity. Student S54 provided an example.
“As a nurse, I feel that mutual respect is vital for nursing. As the nurse respects the patient as an individual to provide the best quality care, the value for respect towards nurses should also be established as professionals.”
(S54)
IV. DISCUSSION
The study demonstrated that students perceived nursing as a professional with knowledge and moral character, which is consistent with the professional requirement by the SNB (2011). However, students perceived a lack of awareness of nurses’ roles and some confusion about nursing identity by the public and other healthcare professionals, which does not reflect the intended development of nursing practice.
The repeated comments of nurses being perceived as inferior to doctors by the public indicated that to them, nursing is still viewed negatively and of lower social status in Singapore, similar to the study done by Tay et al. (2012) ten years ago where nurses felt devalued and disrespected. Internationally, a division in the treatment towards doctors and nurses persists, as people tend to give doctors credit and recognition and view nurses as having a complementary role (de Araujo Sartorio & Pavone Zoboli, 2010; de Meis et al., 2007; Johnson, 2018; Kemmer & Paes da Silva, 2007). The biased perception and treatment contribute to the devaluation of nursing, resulting in a focus solely on nursing functions and categories, rather than profiling nursing’s professional identity.
Despite more nurses pursuing higher education and leading comprehensive patient care roles such as APNs in Singapore, patients still have a poor perception of their roles and lack awareness of the preparation needed (Woo et al., 2020). A study set in a primary care setting found that doctors viewed APNs as competent clinical partners, but their roles were not well understood (Soh et al., 2021). This role confusion is possibly due to the breadth of nurses’ roles and a failure to communicate their professional roles effectively to the public. Pimenta and Souza (2017) reviewed 55 newspapers concerning the professional identity of nursing from 1983 to 2012 and found that nursing was treated as a unified entity. There was no differentiation between “nursing practiced by nurses” from the “nursing practiced by the other workers making up the team” (Pimenta & Souza, 2017, p4) indicating there is still much work to be done to make the roles of nurses more comprehendible and visible.
This study showed how intentional education can help nurses to reflect on their clinical experiences and form a positive professional identity. The finding is consistent with that of a recent study by Fitzgerald and Clukey (2022, p1349) who found that reflection helped students to “think about thinking”, connecting the dots together to know what nursing really is and internalise their professional identity. The educational effort highlighted in both studies can be extended to interprofessional education, to create opportunities for different professional groups to learn together and understand one another’s abilities and roles better. In Singapore, studies on interprofessional learning revealed improved communication, mutual respect, trust and changing the stereotypes and attitudes towards the nurse–physician relationship (Liaw et al., 2014; Liaw et al., 2023). Another study demonstrated how interprofessional virtual rounds helped students from six healthcare courses, including nursing, to gain insights into one another’s professional role and build mutual trust (Liaw et al., 2020). However, these studies were all based in schools with a short duration of learning. Intentional education and long-term studies on professional identity and interprofessional relationships should be continued in clinical settings.
A Singaporean ethnographic study by Chen et al. (2021) exposed the complexity of nurses’ daily work and how nurses navigated their participation and relationships with other healthcare workers. The deliberation of nurses’ professional identity is not a single professional affair, but that of all healthcare professionals. Nevertheless, more action is needed from nurses, nurse educators, and nursing leaders to define, develop, and portray their professional identity. Ben Natan and Becker (2010) urged nurses to let the public know what their work entailed by giving speeches and presenting their work through social media. With the Healthier SG movement (MOH, 2023), it is foreseeable that nurses will play more important roles in preventive and community health. Nurses should seek opportunities to communicate their roles and articulate their abilities to the public.
This study collected data from only one group of nurses undergoing a top-up degree study. Many nurses did not explain their ideas in detail. Future studies can consider using interviews and focus group discussions to explore these ideas in further depth. Nurses from various nursing schools and clinical settings could also be included and views from the public and other healthcare professionals would be welcomed.
V. CONCLUSION
Nursing identity is influenced by multiple factors, which can cause role confusion. The educational effort is vital to nurture nurses’ abilities to reflect, deliberate and communicate their professional identity. Nursing schools in Singapore and further afield need to include such intentional reflective approaches to help nursing students deliberate their professional identity and to nurture their ability to do so throughout their professional careers. Nurses and nursing leaders need to be more proactive in communicating their professional values and roles. More longer-term research is needed in both education and clinical practice settings to understand the sustained effect of education on nurses’ ongoing negotiation of their professional identity.
Notes on Contributors
Dr Mary XiaoRong Chen reviewed the literature, designed the study, conducted the data collection, data analysis and wrote the transcript.
Dr Dora Howes reviewed the data analysis, contributed to the manuscript and gave critical feedback on the final version.
Both authors read and approved the final manuscript.
Ethical Approval
The study was approved by the Singapore Insitute of Technology Ethics Committee (Project 2018007).
Data Availability
The data that support the findings of this study are available in the repository at: https://doi.org/10.25447/sit.23515425
Acknowledgement
We thank all student nurses who participated in the research.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Declaration of Interest
The authors do not have any conflicts of interest. Participation in the research was voluntary and anonymous. Student nurses were assured that their participation or nonparticipation would not affect their learning or academic standing.
References
Bartlett, J. (2015). The profession of nursing. Jones & Bartlett Learning. Retrieved 14 November from http://samples.jbpub.com/9781449649029/46066_CH01_6031.pdf
Ben Natan, M., & Becker, F. (2010). Israelis’ perceived motivation for choosing a nursing career. Nurse Education Today, 30(4), 308-313. https://doi.org/10.1016/j.nedt.2009.08.006
Benner, P., Sutphen, M., Leonard, V., & Day, L. (2009). Educating nurses: A call for radical transformation (Vol. 15). John Wiley & Sons.
Black, B. P. (2014). Professional nursing concepts & challenges (7th ed.). Elsevier.
Braun, V., & Clarke, V. (2006). Using thematic analysis in psychology. Qualitative Research in Psychology, 3(2), 77-101. https://doi.org/10.1191/1478088706qp063oa
Braun, V., & Clarke, V. (2012). Thematic analysis. In H. Cooper (Ed.), APA handbook of research methods in psychology (Vol. 2, pp. 57-71). American Psychological Association.
Chen, M. X. (2020). The evolving identity and competence of new nursing graduates in practice: A community of practice perspective [EdD Thesis, UCL (University College London)]. https://discovery.ucl.ac.uk/id/eprint/10115351/
Chen, M. X., Newman, M., & Park, S. (2021). Becoming a member of a nursing community of practice: Negotiating performance competence and identity. Journal of Vocational Education & Training, 1-15. https://doi.org/10.1080/13636820.2021.2015715
Clements, A. J., Kinman, G., Leggetter, S., Teoh, K., & Guppy, A. (2016). Exploring commitment, professional identity, and support for student nurses. Nurse Education in Practice, 16(1), 20-26. https://doi.org/10.1016/j.nepr.2015.06.001
Clouder, L. (2003). Becoming professional: Exploring the complexities of professional socialisation in health and social care. Learning in Health and Social Care, 2(4), 213-222. https://doi.org/10.1046/j.1473-6861.2003.00052.x
Crigger, N., & Godfrey, N. (2014). From the inside out: A new approach to teaching professional identity formation and professional ethics. Journal of Professional Nursing, 30(5), 376-382. https://doi.org/10.1016/j.profnurs.2014.03.004
de Araujo Sartorio, N., & Pavone Zoboli, E. L. C. (2010). Images of a ‘good nurse’ presented by teaching staff. Nursing Ethics, 17(6), 687-694. https://doi.org/10.1177/0969733010378930
de Meis, C., de Almeida Souza, C., & da Silva Filho, J. F. (2007). House and street: Narratives of professional identity among nurses. Journal of Professional Nursing, 23(6), 325-328. https://doi.org/10.1016/j.profnurs.2007.06.004
Deppoliti, D. (2008). Exploring how new registered nurses construct professional identity in hospital settings. The Journal of Continuing Education in Nursing, 39(6), 255-262. https://doi.org/10.3928/00220124-20080601-03
Fitzgerald, A., & Clukey, L. (2022). Factors influencing nursing professional identity development: A qualitative study. Nursing Forum, 57(6), 1346-1353. https://doi.org/10.1111/nuf.12816
Girvin, J., Jackson, D., & Hutchinson, M. (2016). Contemporary public perceptions of nursing: A systematic review and narrative synthesis of the international research evidence. Journal of Nursing Management, 24(8), 994-1006. https://doi.org/10.1111/jonm.1241 3
Goh, T. (2022, August 3). Resignation rates of nurses in public hospitals at a five-year high in 2021. The Straits Times. https://www.straitstimes.com/singapore/politics/resignation-rates-of-nurses-in-public-hospitals-at-a-five-year-high-in-2021-says-rahayu-mahzam
Hoyle, L. P., Kyle, R. G., & Mahoney, C. (2017). Nurses’ views on the impact of mass media on the public perception of nursing and nurse–service user interactions. Journal of Research in Nursing, 22(8), 586-596. https://doi.org/10.1177/1744987117736 363
Hunter, D., McCallum, J., & Howes, D. (2019). Defining exploratory-descriptive qualitative (EDQ) research and considering its application to healthcare. Journal of Nursing and Health Care, 4(1). https://eprints.gla.ac.uk/180272/
Johnson, M., Cowin, L. S., Wilson, I., & Young, H. (2012). Professional identity and nursing: Contemporary theoretical developments and future research challenges: Nurses, careers and professional identity. International Nursing Review, 59(4), 562-569. https://doi.org/10.1111/j.1466-7657.2012.01013.x
Johnson, S. E. (2018). “Convince your patients and you will convince society”: Career decisions and professional identity among nurses in India. SAGE Open, 8(1). https://doi.org/10.1177/2158244018763014
Kemmer, L. F., & Paes da Silva, M. J. (2007). Nurses’ visibility according to the perceptions of the communication professionals. Revista Latino-Americana de Enfermagem, 15(2), 191-198. https://doi.org/10.1590/S0104-11692007000200002
Liaw, S. Y., Siau, C., Zhou, W. T., & Lau, T. C. (2014). Interprofessional simulation-based education program: A promising approach for changing stereotypes and improving attitudes toward nurse–physician collaboration. Applied Nursing Research, 27(4), 258-260. https://doi.org/10.1016/j.apnr.2014.03. 005
Liaw, S. Y., Tan, J. Z., Lim, S., Zhou, W., Yap, J., Ratan, R., Ooi, S. L., Wong, S. J., Seah, B., & Chua, W. L. (2023). Artificial intelligence in virtual reality simulation for interprofessional communication training: Mixed method study. Nurse Education Today, 122, Article 105718. https://doi.org/10.1016/j.nedt.2023. 105718
Liaw, S. Y., Wu, L. T., Soh, S. L. H., Ringsted, C., Lau, T. C., & Lim, W. S. (2020). Virtual reality simulation in interprofessional round training for health care students: A qualitative evaluation study. Clinical Simulation in Nursing, 45, 42-46. https://doi.org/10.1016/j.ecns.2020.03.013
Liew, I. (2018, July 2). First pharmacists, advanced practice nurses certified to prescribe medicines. The Straits Times. https://www.straitstimes.com/singapore/first-pharmacists-advanced-practice-nurses-now-certified-to-prescribe-medicines
Mao, A., Lu, S.-e., Lin, Y., & He, M. (2021). A scoping review on the influencing factors and development process of professional identity among nursing students and nurses. Journal of Professional Nursing, 37(2), 391-398. https://doi.org/10.1016/j.p rofnurs.2020.04.018
Marique, G., & Stinglhamber, F. (2011). Identification to proximal targets and affective organizational commitment: The mediating role of organizational identification. Journal of Personnel Psychology, 10(3), 107-117. https://doi.org/10.1027/1866-5888/ a000040
Miles, M. B., Huberman, A. M., & Saldaña, J. (2019). Qualitative data analysis: A methods sourcebook (4th ed.). SAGE.
Ministry of Health. (2012). Nursing Careers. https://www.moh.gov.sg/hpp/nurses/career-practices/CareerNPracticesDetails/nursing-careers
Peate, I. (2016). Nursing against the odds. British Journal of Nursing, 25(7), 357-357. https://doi.org/10.12968/bjon.2016.25.7.357
Pimenta, A. d. L., & Souza, M. d. L. d. (2017). The professional identity of nursing in the papers published by Reben. Texto & Contexto Enfermagem, 26(01), e4370015. https://doi.org/10.1590/0104-07072016004370015
Sabanciogullari, S., & Dogan, S. (2015). Relationship between job satisfaction, professional identity and intention to leave the profession among nurses in Turkey. Journal of Nursing Management, 23(8), 1076-1085. https://doi.org/10.1111/jonm.12256
Sather, D. L. (2020). Who Am I? A Case Study of Professional Identity Development in Undergraduates [PhD Thesis, Northcentral University]. ProQuest Dissertations Publishing. https://www.proquest.com/openview/236d1081c0cef0fafcb075a2c36dd183/1?pq-origsite=gscholar&cbl=18750&diss=y
Singapore Nursing Board. (2011). Standard of practice for nurses and midwives. https://www.healthprofessionals.gov.sg/docs/librariesprovider4/publications/snb_standards_of_practices.pdf
Slay, H. S., & Smith, D. A. (2011). Professional identity construction: Using narrative to understand the negotiation of professional and stigmatized cultural identities. Human Relations, 64(1), 85-107. https://doi.org/10.1177/0018726710384290
Soh, B. F. J. R., Ang, W. H. D., De Roza, J. G., Quek, I. P., Lim, P. S., & Lau, Y. (2021). They are partners in care: A qualitative exploration of physicians’ perceptions of primary care Advanced Practice Nurses. Journal of Nursing Scholarship, 53(5), 542-551. https://doi.org/10.1111/jnu.12665
Tay, L. H., Ang, E., & Hegney, D. (2012). Nurses’ perceptions of the barriers in effective communication with inpatient cancer adults in Singapore. Journal of Clinical Nursing, 21(17-18), 2647-2658. https://doi.org/10.1111/j.1365-2702.2011.03977.x
Ten Hoeve, Y., Jansen, G., & Roodbol, P. (2014). The nursing profession: Public image, self-concept and professional identity. A discussion paper. Journal of Advanced Nursing, 70(2), 295-309. https://doi.org/10.1111/jan.12177
Woo, B., Koh, K., Zhou, W., Wei Lim, T., Lopez, V., & Tam, W. (2020). Understanding the role of an advanced practice nurse through the perspectives of patients with cardiovascular disease: A qualitative study. Journal of Clinical Nursing, 29(9-10), 1623-1634. https://doi.org/10.1111/jocn.15224
Xu, C., Koh, K. W. L., & Zhou, W. (2022). The development of advanced practice nurses in Singapore. International Nursing Review. https://doi.org/10.1111/inr.12810
*Mary Chen Xiaorong
10 Dover Drive,
Singapore 138680
Email: Mary.chen@singaporetech.edu.sg / xiaorong8@gmail.com
Submitted: 2 July 2023
Accepted: 17 November 2023
Published online: 2 April, TAPS 2024, 9(2), 51-59
https://doi.org/10.29060/TAPS.2024-9-2/OA3078
Soi Moi Chye1, Rhun Yian Koh1 & Pathiyil Ravi Shankar2
1Department of Applied Biomedical Science and Biotechnology, School of Health Science, International Medical University, Kuala Lumpur, Malaysia; 2IMU Centre for Education, International Medical University, Kuala Lumpur, Malaysia
Abstract
Introduction: People skills play a crucial role in the professional development of Biomedical Scientists. A laboratory management and professional practice module was offered as part of the people skills development for Biomedical Science first-year students. This study aims to describe the use of role-play to teach stress and anger management skills to Biomedical Science students and reports on students’ opinions of role-play as a teaching-learning method.
Methods: Students were divided into groups with 10 or 11 students per group. Each group of students presented a role-play for 15 to 20 min. This was followed by reflections by the group, feedback from other groups, and the facilitators. At the end of the session, student feedback was taken by a questionnaire using both closed (using a 5‑point Likert scale) and open‑ended questions. Statistical evaluation of the collected data was carried out using SPSS version 28 for Windows.
Results: A total of 96 students from the 2021 and 2022 cohorts participated in the role-plays. The survey was completed by 48 students from the 2021 intake and 33 students from the 2022 intake. The overall response rate was 84.37%. Respondents perceived role-play to be enjoyable, useful, and helpful for developing stress and anger management skills. They wanted role-play to be used as a teaching-learning method in the future.
Conclusions: Role-play can be effective to teach stress and anger management skills to undergraduate Biomedical Science first-year students.
Keywords: Role-Plays, Stress and Anger Management Skills, Biomedical Science, Professional, Questionnaire, Feedback; Undergraduate
Practice Highlights
- Respondents perceived role-play to be enjoyable, useful, and helpful for developing stress and anger management skills.
- Role-play can be effective to teach stress and anger management skills to undergraduate Biomedical Science first-year students.
- Role-play was recommended to be used as a teaching-learning method in the future.
I. INTRODUCTION
People skills are the ability to communicate effectively with others, build relationships, and work collaboratively. People skills include active listening, empathy, conflict resolution, and teamwork. Anger and stress can impact people skills, especially interpersonal communication (Strumska-Cylwik, 2014). It is important to note that people who are easily angered and stressed often come from families that are disruptive, chaotic, and not skilled at emotional communication. Uncontrolled anger and stress can negatively affect physical health and emotional well-being and can lead to problems at work, in personal relationships, and in the overall quality of life (Armstrong, 2012). There is an important link between anger, stress, interpersonal skills, and emotional intelligence (Schutte et al., 2001). Bennett et al. (2016) reported that soft skills (people skills) are more critical for future employment than technical skills, and their enhancement has a lifelong impact. These skills are particularly important for health professionals due to the close relationship between them and their patients.
Health professionals are required to possess a technical background, which includes reasoning and critical judgment, as well as competency in communications, conflict resolution, negotiation, and decision-making (Morrell et al., 2020). A study among undergraduate medical students found a decline in students’ people skills, and a more technical approach replaced a more spontaneous and humane approach (Wahlqvist et al., 2005). Ahmad et al. (2014) concluded that most engineering students possess technical skills but lack people skills. One of the reasons is that teachers lack comprehensive knowledge and experience in teaching soft (people) skills to students (Ahmad et al., 2014). Ministry of Higher Education Malaysia (2005) states that the development of soft (people) skills requires a student-centred approach. Similarly, Mohd-Amin and Mohd-Nor (2010) and Morris (2009) suggest that teachers should be more creative when devising teaching and learning strategies so that students’ people skills can be more effectively organised and developed. Curriculum quality and teachers have an impact on students’ listening, responding, questioning, and formulating abilities (Morris, 2009). These skills acquired by an individual assist them in optimising their performance and include communication skills, teamwork, leadership skills, problem-solving skills, critical thinking skills, time management, and emotional intelligence (Siu et al., 2021). Teachers are therefore vital to implementing people skills relevant to the courses they teach. At our university student evaluations of laboratory management and professional practice module indicated they were not satisfied with the teaching of these skills through lectures. Students indicated that the lectures were boring, not effective, and the content was already known. Thus, we used a different method of role-play to teach stress and anger management skills.
Role-play is defined as an approach to learning in which learners act out roles in case scenarios to provide targeted practice and feedback for the development of skill and competency (Nair, 2019). As a result, they gain a first-hand experience of human interactions and a better understanding of appropriate behavioural approaches to situations like those in real life. This approach emphasizes the learner’s need to know, self-direction, and varied experiences, contributing to the adoption of a problem-centred approach (Shankar et al., 2012). According to Harries and Raban (2012), role-play is a useful technique for engaging students in the learning process and environment. Through role-play, students can communicate and experience different situations and contexts, which can be used by teachers to develop students’ problem-solving, critical thinking, and creative skills. Furthermore, role-play allows students to experience a variety of different domains: cognitive, emotional, physical, and literacy domain (Beard et al., 1995). Additionally, role-play has been proven to be an effective method of developing skills such as active listening, problem-solving, empathy, teamwork, knowledge acquisition, and effective communication in various fields of training (Beard et al., 1995; Harden & Gleeson, 1975; Kim, 2018). Apart from this, role-play is an effective teaching strategy for health science students and is used by medical students to practice communication skills effectively and promote empathy and a more patient-centred approach to care (Ong et al., 2022). Based on the findings of Rønning and Bjørkly (2019), role-play in health sciences education enhances students’ therapeutic and communicative skills and facilitates personal and professional growth as it increases students’ ability to learn what it is like to be in others’ shoes and, through that experience, develop empathy and reflection. Role-play can be an effective tool for developing stress and anger management skills. It allows individuals to practice new behaviours and techniques in a safe and supportive environment, which can help to build confidence and improve overall well-being (Snowden & Rebar, 2018; Sutton, 2022).
The International Medical University (IMU), Bachelor of Science (Hons) in Biomedical Science programme is designed to produce work-ready graduates who are well-equipped with knowledge and are competent in practical, as well as people skills. The curriculum of the programme includes research-based teaching and problem-based learning, and students learn from experienced faculty. In addition to didactic large group teaching sessions (plenaries), the programme is also delivered through small group teaching sessions, such as problem-based learning, workshops, computer-aided learning, tutorials, seminars, presentations, etc. The learning outcomes of stress and anger management sessions are the definition of anger and stress; anger and stress management skills; contributing factors to stress and anger; and approaches to managing stress and anger engagement. The present study was conducted to explore the participants’ perception of the usefulness, understanding, enjoyment, and feedback of using role-play as a teaching-learning method for developing stress and anger management skills.
II. METHODS
Stress and anger management skills are a component of the laboratory management and professional practice module. This module is compulsory for first-year Biomedical Science students. Role-play was chosen to deliver stress and anger management skills because previous students were not satisfied with lectures as the teaching-learning method. Role play serves as a method of experiential learning in which learners assume various roles and engage in interactive experiences in diverse learning environments. The theory of experiential learning underscores the significance of acquiring knowledge through hands-on experience and subsequent reflection, constituting fundamental components of contemporary approaches to adult education (Nestel & Tierney, 2007).
The procedures for the role-play were based on Shankar et al. (2012) article. Shankar et al. had used role-plays to explore issues related to the health humanities among medical students. Here it was used to explore stress and anger management skills among biomedical science students. Table 1 shows the sequence of activities during the sessions. The addition of a guide or facilitator is necessary to maximize the benefits derived from role-plays (Cobo et al., 2011). The facilitators provide guidance to the learners before and after the sessions (Nakamura et al., 2011). First, the faculty explained how to prepare the role-play and gave an example of good quality and poor-quality role-play. Additionally, stress and anger management YouTube videos were also uploaded to the e-Learning portal for reference. Then, students were divided into groups with 10 or 11 students per group. During the third step, students could select the scenarios provided or create their own scenarios. Nevertheless, students were required to consult with faculty members regarding the role-play to address major learning issues. Having determined the topics, students began writing scripts and practicing the role play. Each group of students performed a role-play for 15 to 20 min and a presentation on contributing factors for stress and anger and the correct and incorrect approaches to handling stress and anger based on the scenario for 5 min. Finally, faculty members provided feedback to the students for further improvement.
|
Activities |
Duration |
|
1. A briefing on the role-play preparation procedures as well as YouTube videos on stress and anger management were uploaded to the e-Learning portal. |
1 hour |
|
2. Students were divided into groups with 10 or 11 students per group. |
10 minutes |
|
3. Selection and determination of topics, script preparation, and role-play practice. |
3 weeks |
|
4. Role-play performance, 15-20 minutes per group. Presentation of the contributing factors and correct and incorrect approaches to handling stress and anger, 5 minutes per group. |
3 – 4 hours |
|
5. Faculty members provided feedback to the students for further improvement. |
30 minutes |
Table 1. An overview of the activities and duration of different components of the role-play session
A total of 96 students from the 2021 and 2022 cohorts participated in the role-plays. The sample size calculation is shown below.
The calculator.net (www.calculator.net) sample size calculator was used. The confidence level was 95%, and the margin of error was set at 5%, assuming a population % of 50% and a population size of 96. The recommended sample size using these parameters was 77.
The questionnaire used to obtain student feedback is based on that used by Shankar et al. (2012) with some modifications as shown in Appendix I. In that study, original role-play questionnaires were used by students from the third, fifth, and sixth semesters of the Medical Humanities module. Thus, some of the questions, such as “Have you been exposed to the use of role-plays for educational objectives before?” “Are you aware of the use of role-plays in medical education elsewhere?” were removed. The rest of the questions are similar. Feedback was obtained from the Biomedical Sciences programme first-year students. The questionnaires contained both close-ended (using a 5-point Likert scale) and open questions. The survey was conducted after the students completed the role-play from 18 to 22 October 2022. Participants were informed about the study’s objectives before participating, and they were required to provide written informed consent.
Data were analysed using MS Excel and SPSS version 28. The distribution of the scores for enjoyment, understanding, and usefulness were compared using the one-sample Kolmogorov-Smirnov test (p<0.05). The distributions were not normal and hence median and interquartile range were used as measures of central tendency and variation. The median (interquartile range) scores among the two cohorts and among males and females were compared using the independent samples median test (p<0.05). Each open comment was analysed systematically in an iterative manner by creating a thematic coding structure. As new themes emerged, the coding structure was revised, and the previous comments were reread for consistency. Moreover, the comparison of the difference between cohorts and gender for the perception of enjoyment, understanding, and usefulness was conducted because role-plays for cohort 2021 were conducted online due to Malaysia’s movement control order during the COVID-19 pandemic. However, the cohort 2022 role-plays were conducted physically. Studying gender differences in the perception of different educational interventions may be important because behaviours, styles of social interaction, academic motivations, and choices may be different across genders, and it helps identify disparities and promote equity and inclusivity in the classroom. It allows educators to address any biases or barriers that may hinder students’ educational opportunities and success (Myaskovsky et al., 2005).
III. RESULTS
A total of 96 students from 2021 (56) and 2022 cohorts (40) participated in the role-plays. A total of 81 students (overall response rate of 84.1%) participated in the survey. Our results show forty-eight students were from the 2021 cohort and the cohort response rate was 85.7%, Thirty-three students were from the 2022 cohort and the cohort response rate was 82.5%. The percentage of males was 22.22% and females were 77.78%. According to Figure 1, 65% of students prefer role-play to teach stress and anger management skills, followed by small group discussions (15%), case-based learning (13.3%), and lectures (6.7%). This is based on question 8 of the questionnaire. Figure 2 illustrates the skills students learned during role-play. Communication skills were mentioned by 62.3% of the respondents, followed by teamwork (16.9%), stress and anger management (12.9%), and problem-solving skills (7.8%). This is based on question 4 of the questionnaire. The data that supports the study is available at https://doi.org/10.6084/m9.figshare.23607033.v1.
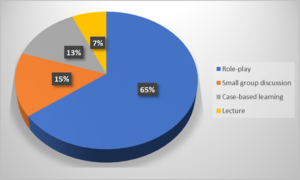
Figure 1. Instructional methods preferred by students to learn stress and anger management skills
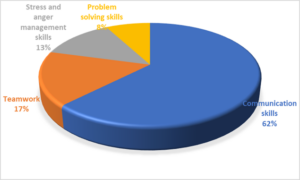
Figure 2. Skills students learned through role-plays
Sixty-six students (90.4%) mentioned role-plays can be used for future topics/modules while 7 students (9.6%) were not in favor (based on question 9 of the questionnaire).
The perceptions of students about the use of role-play in anger and stress management were measured on a scale of 1 to 5 with 1 being the least and 5 being the highest. Table 2 shows the median and interquartile range of the scores for enjoyment, understanding, and usefulness among the two cohorts and among male and female students. There was no statistically significant difference in the scores between the two cohorts and between male and female students.
|
Items |
Categories |
Median (IQR) |
p-value |
|
Enjoyment |
BM121 |
4.00 (1) |
0.948 |
|
BM122 |
4.00 (2) |
||
|
Female |
4.00 (1) |
0.717 |
|
|
Male |
4.00 (1) |
||
|
Understanding |
BM121 |
4.00 (0) |
0.197 |
|
BM122 |
4.00 (1) |
||
|
Female |
4.00 (1) |
0.404 |
|
|
Male |
4.00 (0) |
||
|
Usefulness |
BM121 |
4.00 (1) |
0.954 |
|
BM122 |
4.00 (1) |
||
|
Female |
4.00 (1) |
0.132 |
|
|
Male |
4.00 (0) |
Table 2. Summary of survey results of enjoyment, understanding, and usefulness scores among the two cohorts and among male and female students
|
Theme |
Quotes |
|
Knowledge and understanding |
“By implementing the solutions for anger and stress management to our role-play, we are able to understand its importance and apply it to our daily lives.” “Help students to understand a particular stressful situation by assigning the students to act out, involving in script and coming up with an outcome. Hence, they see the whole picture clearly and more related to it.” “Yes, it covers different aspects including family, peers, and colleagues. So, student get to understand different circumstances.” |
|
Usefulness |
“Yes, all the scenarios showed stress and anger in different possible situations we may encounter.” “Role-play allows us to experience and understand the emotions involved in related scenarios and better prepare us for the future.” |
|
Enjoyable |
“Role play should be considered more than lectures because it is more effective, and students prefer enjoyable way of studying.” “Can relate more by looking at real life acting on situation, more fun and engaging.” “It’s livelier and fun, making it easier to learn.” |
|
Communication |
“It helps us to know that communication skills are important, which certainly helps to clear doubt and can release some stress.” “Communication skills when preparing the role play and presentation skills when acting.” “The communication skill is the soft skill I have learnt from this role-play. It is because our group had several discussions and rehearsals before the role-play. During these times, I need to express my view clearly and fluently, especially the creative ideas and critics. I have learnt how to negotiate with others’ opinions too.” |
|
Teamwork |
“I think because of our teamwork we were able to overcome the difficulties we might have had in the beginning.” “It makes me understand the topic more and helps me be more collaborative with my peers.” |
Table 3. Perception of students regarding the role plays
Regarding students’ perceptions of the appropriateness of the scenarios covered during the role-play the role-play most students answered yes, while only one student answered no. Students stated, “All the scenarios showed stress and anger in different possible situations we may encounter.” “It covers different aspects including family, peers, and colleagues. So, students get to understand different circumstances.” “Because they were those that will occur one way or another in real life be it in a work setting or a school setting. These scenarios were a stepping stone towards the real world and all the possibilities it has to offer.” From the feedback, we concluded that the reasons for the appropriateness of the scenarios covered during the role-play included they were able to see how to manage stress and anger in different situations.
Moreover, 90.4% of the students responded that role-play should be used in future topics/modules. Suggestions for improving the use of role-plays during future sessions were the stage to perform the role-play is too small, and the background is not appropriate. Comments also include improving briefing, marking rubrics, feedback, and expectations for students further. Each group can have a lesser number of participants making fair and equal work distribution, and more real-life case scenarios can be provided.
IV. DISCUSSION
This study explores the contribution of role-play in teaching stress and anger management skills. Results showed that students perceived role-play to be enjoyable, useful, and helpful for developing stress and anger management skills. According to Harries and Raban (2012), role-play engages many brain regions including language, emotion, cognition, and motor functions. It, therefore, stimulates participants’ cognitive and affective engagement while they have fun. In line with this finding, our students found role-play to be a fun, enjoyable, effective, useful, easy, engaging, interactive, and interesting method for learning stress and anger management skills. Eggen and Kauchak (2006) mentioned that the use of a specific teaching & learning method helps encourage students to apply soft skills and further enhance additional skills possessed by students. In agreement with this study, our results showed that role-play provided students with an opportunity to develop communication skills, teamwork skills, and problem-solving abilities. It has been proven by Beard et al. (1995), that role-play allows children to communicate and experience different situations and contexts which teachers can use to develop students’ problem-solving, critical thinking, and creativity skills.
Several studies have demonstrated that providing feedback to students can improve their learning outcomes while providing feedback from teachers can improve their performance in the classroom (Dinkmeyer & Losoncy, 1980; Schutz & Weinstein, 1990). Structured feedback helped students to reflect on both what had taken place in each role-play as well as the value of role-play after participating in the session. This is true for first-year students who previously had no exposure to professional practice and are therefore dependent on feedback and guidance. Further, our experience with role-play is open to improvement in subsequent courses. Based on the feedback, students commented that the marking rubric for role-play can be further improved. A study suggested that the assessment of student role-play learning outcomes could be improved using validated rubrics and published examples (Carlin et al., 2011). Considering this, we will revise our marking rubric in accordance with published examples for the following cohort. According to feedback from the 2021 students, role-play should be conducted physically, while feedback from the 2022 students indicated that the performance stage was too small, and the background and props could be improved. It is important to note that there are differences in feedback from both cohorts because of the COVID-19 pandemic. The role-play for the 2021 cohort was conducted online, whereas the role-play for 2022 was conducted face-to-face. There were no differences in the median scores between males and females and between the two cohorts. With the reduction in the COVID-19 pandemic, the university is slowly moving toward face-to-face teaching-learning. For subsequent cohorts, role-plays will be conducted physically.
Next, it would be beneficial to improve briefings, feedback, and expectations for students. We provided feedback and expectations for students during the module coordinator briefing and uploaded the briefing recorded video to the e-Learning portal and provided feedback to students after the role-play. This can improve further for subsequent cohorts because Al-Hattami (2019) suggests that feedback is constructive if it provides students with clear expectations about their performance, encourages students to increase their efforts, and describes their future learning goals. Feedback should be provided to all students consistently, fairly, and immediately after they have completed the task to enhance their learning (Hattie & Timperley, 2007). Constructive feedback has a significant impact on a student’s learning (Lipnevich & Smith, 2009). Thus, we will provide more effective feedback to the next cohort of students. The other comment is the request for smaller group sizes, making fair and equal work distribution. The current grouping of students is 10-11 students per group. Therefore, it is possible that the distribution of work among students is not equal. For the next cohort, the grouping should be decreased to 5-6 students per group.
The Division of Laboratory Systems of the Centres for Disease Control and Prevention (Division of Laboratory Systems, 2018) and the American Society for Clinical Pathology (ASCP) (American Society for Clinical Pathology, n.d.) have developed guidelines regarding the required competencies for laboratory personnel. Among the different competencies, communication skills, leadership and education of other laboratory personnel, other healthcare professionals and consumers are mentioned. A study showed that stress and anger management skills play an important role in interpersonal communication (Strumska-Cylwik, 2014). According to Prabhu et al. (2016), anger is often a maladaptive reaction to the stress of coping in a stressful environment, which may lead to an increase in conflict and discomfort. A wide range of problems have been linked to anger, including alcohol and substance abuse, emotional of insecurity, and even self-harm. Many students have anger episodes that last for approximately a day, and a significant majority found it difficult to concentrate on academic work and maintain healthy relationships during these episodes (Dollar et al., 2018). In accordance with Safari et al. (2014), training in anger management, stress management, and interpersonal communication skills can significantly improve the emotional intelligence of students. Managing anger and stress effectively can have a significant impact on mental health, academic performance, interpersonal relationships, and overall well-being. Thus, if Biomedical Science students are well-equipped with these techniques, they will be able to better engage with the learning process, improve problem-solving abilities, promote healthy coping mechanisms, cultivate positive interpersonal relationships, maintain physical and mental health, improve academic performance, be able to address physical abuse, criminal behaviour, difficulty concentrating, sleep disturbances, and ensure long-term success.
There were also limitations to this study. First, the participants are new first-year, semester 1 students. This is their first-time doing role-play, and they do not have any prior experience in this regard. Thus, educational effectiveness could only be determined indirectly. Students’ stress and anger management skills were not measured before or after the role-play, and much of the evidence for its effectiveness is based on anecdotal evidence. Second, in general, role-play alone probably contributes along with other factors to stress management and anger management skills development. Therefore, it is difficult to evaluate the effects of a single educational method. Additionally, it is important to recognize that students learn in different ways. Third, there may have been a certain amount of response bias, as the student is familiar with the researcher and may have subconsciously or consciously given the response that he or she thinks the researcher expects to hear. This study analysed only quantitative data from a structured questionnaire. Although a few open-ended questions were incorporated to analyse students’ perceptions, they were not explored in depth. Moreover, this study was conducted using a modification of an existing questionnaire. No validation was carried out. Future studies should involve more role-plays and participants to clarify the effects of the role-play and examine the long-term effects of repeated role-play.
V. CONCLUSION
Most students found role-play to be enjoyable, useful, and helpful for understanding stress and anger management skills, regardless of their cohort or gender. By using role-play, students gain a better understanding of the objectives and factors contributing to stress and anger and the development of management skills because role-play provides students with an experiential learning opportunity. Students actively engage in simulated situations, allowing them to better grasp the complexities of these emotions. During role-play, students must think critically and make decisions based on the roles they’re portraying. They must analyse situations, identify triggers, and consider appropriate management strategies, promoting higher-order thinking skills. Dealing with stress and anger often involves problem-solving. Role-play challenges students to find effective solutions to conflicts and challenges that arise within the scenarios, encouraging them to develop creative problem-solving skills. After the role-play, students can receive feedback from peers or instructors. This feedback helps them understand the effectiveness of their chosen strategies and encourages reflective thinking about their decisions and actions. Engaging in role-play can lead to increased self-awareness as students reflect on their own emotional responses and behaviours in stressful situations. Thus, it is recommended that role-play be incorporated into future teaching methods.
Notes on Contributors
Soi Moi Chye was involved in facilitating the role-play and providing constructive feedback to students. She was involved in the concept and design of the study, writing and applying for ethical approval from the ethical committee. She helped in revising the manuscript. She implemented the project, conducted data analysis and interpretation, and drafted the manuscript.
Rhun Yian Koh was involved in facilitating the role-play and providing constructive feedback to students. She was also involved in implementing the research project, data analysis and interpretation, and critical review and revision of the manuscript.
Pathiyil Ravi Shankar was involved in the conception and design of the study, data analysis, and interpretation, critical revision of the proposal and manuscript, approved the final manuscript and carefully copyedited the manuscript. He helped in revising the manuscript.
Ethical Approval
This study obtained approval from International Medical University-Joint Committee on Research & Ethics (IMU-JC); the grant number is IMU 558-2022.
Data Availability
The data associated with this study is available at https://doi.org/10.6084/m9.figshare.23607033.v1.
Funding
This study was supported by International Medical University; the grant number is IMU 558-2022.
Declaration of Interest
The authors have no conflict of interest to declare.
References
Ahmad, E., Asri, S., Suhaili, P., & Jamaludin, J. (2014). Applications of soft skills in engineering programme at polytechnic Malaysia. Procedia – Social and Behavioral Sciences, 140, 115-120. https://doi.org/10.1016/j.sbspro.2014.04.395
Al-Hattami, A. (2019). The perception of students and faculty staff on the role of constructive feedback. International Journal of Instruction, 12(1), 885-894. https://doi.org/10.29333/IJI.2019.121 57A
American Society for Clinical Pathology. (n.d.). Personnel standards for laboratory professionals (policy number 04-01). https://www.ascp.org/content/docs/default-source/policy-statements/ascp-pdft-pp-personnel-standards.pdf?sfvrsn=2
Armstrong, M. (2012). Armstrong’s handbook of management and leadership: Developing effective people skills for better leadership and management (3rd ed.). Kogan Page Publisher.
Beard, R. L., Salas, E., & Prince, C. (1995). Enhancing transfer of training: Using role-play to foster teamwork in the cockpit. The International Journal of Aviation Psychology, 5(2), 131–143. https://doi.org/10.1207/s15327108ijap0502_1
Bennett, D., Richardson, S., & Mackinnon, P. (2016). Enacting strategies for graduate employability: How universities can best support students to develop generic skills. Curtin University. https://doi.org/10.13140/RG.2.1.4094.8886
Carlin, N., Rozmus, C., Spike, J., Willcockson, I., Seifert, W., Chappell, C., Hsieh, P., Cole, T., Flaitz, C., & Engebretson, J. (2011). The health professional ethics rubric: Practical assessment in ethics education for health professional schools. Journal of Academic Ethics, 9, 277-290. https://doi.org/10.1007/s10805-011-9146-z
Cobo, A., Conde, O., Quintela, M. Á., Mirapeix, J. M., & López-Higuera, J. M. (2011). On-line role-play as a teaching method in engineering studies. Journal of Technology and Science Education, 1(1). https://doi.org/10.3926/jotse.2011.13
Dinkmeyer, D., & Losoncy, L. E. (1980). The encouragement book: Becoming a positive person. Prentice Hall.
Division of Laboratory Systems. (2018, November 15). Competency guidelines for laboratory professionals. https://www.cdc.gov/csels/dls/competency-guidelines-laboratory-professionals.html
Dollar, J. M., Perry, N. B., Calkins, S. D., Keane, S. P., & Shanahan, L. (2018). Temperamental anger and positive reactivity and the development of social skills: Implications for academic competence during preadolescence. Early Education and Development. 29(5), 747-761. https://doi.org/10.1080/10409289.2017.1409606
Eggen, P. D., & Kauchak, D. P. (2006). Strategies for teacher: Teaching content and thinking skills (5th ed.). Allyn and Bacon.
Harden, R. M., & Gleeson, F. A. (1975). Assessment of clinical competence using an objective structured clinical examination. The BMJ, 1, 447–451. https://doi.org/10.1136/bmj.1.5955.447
Harries, J., & Raban, B. (2012). Play in the early years: Role play. Essential Resources.
Hattie, J., & Timperley, H. (2007). The power of feedback. Review of Educational Research, 77(1), 81-112. https://doi.org/10.3102/003465430298487k
Kim, J. H. Y. (2018). Effects of role-play for problem-solving skills and engagement in online forums. Educational Technology to Improve Quality and Access on a Global Scale, 91-109. https://doi.org/10.1007/978-3-319-66227-5_8
Lipnevich, A. A., & Smith, J. K. (2009). Effects of differential feedback on students’ examination performance. Journal of Experimental Psychology: Applied, 15(4), 319–333. https://doi.org/10.1037/a0017841
Ministry of Higher Education Malaysia. (2005). Modul pembangunan kemahiran insaniah (soft skills). UPM Press. https://upmpress.com.my/product/modul-pembangunan-kemahiran-insaniah-soft-skills-untuk-institusi-pengajian-tinggi-malaysia/
Mohd-Amin, N. F., & Mohd-Nor, S. (2010). Tinjauan terhadap guru di Sekolah Menengah Teknik Negeri Johor terhadap penerapan kemahiran generik dalam proses pengajaran dan pembelajaran mata pelajaran kejuruteraan. Malaysian Academic Library Institutional Repository.
Morrell, B., Eukel, H. N., & Santurri, L. E. (2020). Soft skills and implications for future professional practice: Qualitative findings of a nursing education escape room. Nurse Education Today, 93, Article 104462. https://doi.org/10.1016/j.nedt.2020.104462
Morris, A. (2009). The stretched academy: The learning experience of mature students from under-represented groups. University of Lincoln.
Myaskovsky, L., Unikel, E., & Dew, M. (2005). Effects of gender diversity on performance and interpersonal behavior in small work groups. Sex Roles, 52(9/10), 645–657.
Nair, B. T. (2019). Role play – An effective tool to teach communication skills in pediatrics to medical undergraduates. Journal of Education and Health Promotion, 8, 18.
Nakamura, T., Taguchi, E., Hirose, D., Masahiro, I., & Takashima, A. (2011). Role-play training for project management education using a mentor agent. 2011 IEEE/WIC/ACM International Conferences on Web Intelligence and Intelligent Agent Technology. https://doi.org/10.1109/wi-iat.2011.256
Nestel, D., & Tierney, T. (2007). Role-play for medical students learning about communication: Guidelines for maximising benefits. BMC Medical Education, 7, Article 3. https://doi.org/10.1186/1472-6920-7-3
Ong, C. Y., Yee, M. M., Soe, K. M., Abraham, R. E., Tan, O. J. H., & Ong, E. L. C. (2022). Role-playing in medical education: An experience from public role-players. Educación Médica, 23(6), Article 100767. https://doi.org/10.1016/j.edumed.2022.100767
Prabhu, G. S., Tam, J. M. Y., Amalaraj, J. J. P., Tan, E. Y. J., & Kumar, N. (2016). Anger management among medical undergraduate students and its impact on their mental health and curricular activities. Education Research International, 2016, 1-6. https://doi.org/10.1155/2016/7461570
Rønning, S. B., & Bjørkly, S. (2019). The use of clinical role-play and reflection in learning therapeutic communication skills in mental health education: An integrative review. Advances in Medical Education and Practice, 10, 415-425. http://dx.doi.org/10.2147/AMEP.S202115
Safari, A., Jafary, M. R., & Baranovich, D. L. (2014). The effect of anger management, intrapersonal communication skills and stress management training on students’ emotional intelligence (EQ). International Journal of Fundamental Psychology and Social Sciences, 4(2), 31-38.
Schutte, N. S., Schuettpelz, E., & Malouff, J. M. (2001). Emotional intelligence and task performance. Imagination, Cognition and Personality, 20(4), 347-354. https://doi.org/10.2190/J0X6-BHTG-KPV6-2UXX
Schutz, P. A., & Weinstein, C. E. (1990). Using test feedback to facilitate the learning process. Innovation Abstracts NISOD, 12(6), 1-2.
Shankar, P. R., Piryani, R. M., Singh, K. K., & Karki, B. M. S. (2012). Student feedback about the use of role-plays in Sparshanam, a medical humanities module. F1000Research, 1, 65. http://dx.doi.org/10.12688/f1000research.1-65.v1
Siu, J. L. R., Salazar, R. E. R., & Montaño, L. F. (2021). Habilidades blandas y el desempeño docente en el nivel superior de la educación. Propósitos Y Representaciones, 9(1). https://doi.org/10.20511/pyr2021.v9n1.1038
Snowden, S., & Rebar, S. (2018). Anger management workbook for kids: 50 Fun activities to help children stay calm and make better choices when they feel mad. Althea Press.
Strumska-Cylwik, L. (2014). Expression of fear and anger in the context of interpersonal communication. International Journal of Arts & Sciences, 7(1), 173.
Sutton, J. (2022, July 22). Role play in therapy: 21 scripts & examples for your session. Positive Psychology. https://positivepsychology.com/role-playing-scripts/#google_vignette
Wahlqvist, M., Mattsson, B., Dahlgren, G., Hartwig-Ericsson, M., Henrique, B., Hamark, B., & Hösterey-Ugander, U. (2005). Instrumental strategy: A stage in students’ consultation skills training? Observations and reflections on students’ communication in general practice consultations. Scandinavian Journal of Primary Health Care, 23(3), 164–170. https://doi.org/10.1080/02813430510018646
*Dr Pathiyil Ravi Shankar
IMU Centre for Education,
International Medical University
Jalan Jalil Perkasa 19, Bukit Jalil
Kuala Lumpur, Malaysia 57000
Email: ravi.dr.shankar@gmail.com
Submitted: 1 July 2023
Accepted: 24 October 2023
Published online: 2 April, TAPS 2024, 9(2), 39-50
https://doi.org/10.29060/TAPS.2024-9-2/OA3074
Muhammad Irfan Kamaruddin1,2, Andi Alfian Zainuddin1,3, Berti Nelwan1,4, Sri Asriyani1,5, Firdaus Hamid1,6, Tenri Esa1,7 & Irawan Yusuf1,8
1Department of Medical Education, Faculty of Medicine, Hasanuddin University, Indonesia; 2Department of Ophthalmology, Faculty of Medicine, Hasanuddin University, Indonesia; 3Department of Public Health, Faculty of Medicine, Hasanuddin University, Indonesia; 4Department of Pathology Anatomy, Faculty of Medicine, Hasanuddin University, Indonesia; 5Department of Radiology, Faculty of Medicine, Hasanuddin University, Indonesia; 6Department of Microbiology, Faculty of Medicine, Hasanuddin University, Indonesia; 7Department of Clinical Pathology, Faculty of Medicine, Hasanuddin University, Indonesia; 8Department of Physiology, Faculty of Medicine, Hasanuddin University, Indonesia
Abstract
Introduction: A good learning environment (LE) will affect the quality and standard of the learning process, student performance, and the outcome of the curriculum as well as predictor of the quality of health services. Our study aims to assess residents’ perception of the LE in Ophthalmology training programs for future improvement.
Methods: Mixed method with an explanatory sequential design was implemented in this study using the Post-graduate Hospital Educational Environment Measure (PHEEM) as a quantitative approach and open-ended questions collaborated with focus group discussion (FGD) as a qualitative measurement. A comparison of the quantitative data was made using parametric and non-parametric analyses. Thematic analyses were performed for qualitative data. Integration of quantitative and qualitative data was done by connecting both data.
Results: Fifty-three residents participated in this survey. The mean age was 30.96±2.18 years old, 64.15% were female and 77.36% are at the internship stage. The mean score of overall PHEEM was 123.40 ±12.35, indicated an excellent LE, while the mean score of perceptions of role autonomy, perceptions of teaching, and perceptions of social support were 42.57±4.62, 47.75±4.84 and 33.08±4.15, respectively. There is no significant difference between gender and study period with the perception of LE. Thematic analysis from qualitative data reveals six positive and five negative perception themes. All discovered themes confirmed concordance with the result of LE perception.
Conclusion: Learning environment perception in the ophthalmology residency program was excellent and essential for the student’s skills and performance quality. Some specific areas still need improvement strategies for institutional development.
Keywords: Learning Environment, PHEEM, Ophthalmology, Residency, Mixed Method
Practice Highlights
- Ophthalmology resident has an excellent learning environment.
- Good teacher, learning system and social life will give positive perception on learning environment.
- Lack of learning opportunity, less mentoring time, and suboptimum facilities influence students negative perception of learning environment.
I. INTRODUCTION
A good learning environment (LE) will affect the learning process and student behavior and determine the outcome of the curriculum (Al-Shiekh et al., 2014; Bari et al., 2018; Binsaleh et al., 2015; Ong et al., 2019; Ong et al., 2020). Learners who experience an excellent LE will actively participate in the learning process (Clapham et al., 2007). With an ideal LE, learners can achieve better academic success than learners who perceive the LE negatively (Ong et al., 2019; Ong et al., 2020).
The clinical LE is an essential factor influencing the quality of medical education in residency programs (Sandhu et al., 2018). The resident LE, which mostly took place at the hospital, differs from that of medical students. This environment has many destructive factors that impact residents’ performance and mentality and can result in residents experiencing symptoms of burnout (Prins et al., 2010; Ripp et al., 2017). Suboptimal clinical LE have been associated with poor patient care and learning outcomes (General Medical Council, 2016). Therefore, efforts to improve the quality of the LE not only positively impact the environment in which learners learn and participate in patient care but also affect the practice of graduate doctors in the future.
This study aims to determine the residents’ perception of LE in the ophthalmology training program. Based on current data, there is still no study about ophthalmology residents’ perception of LE and its associated factors. This study is a pioneer and pilot study of LE in Ophthalmology training programs, especially in Indonesia.
II. METHODS
A. Study Design and Subjects
This mixed methods study was conducted with explanatory sequential design with both quantitative and qualitative measurements that were performed from January to May 2023 at two main teaching hospitals for the ophthalmology specialist program (OSP) Faculty of Medicine, Hasanuddin University in Makassar, Indonesia.
The study consists of two phases; the first is an offline survey comprising The PHEEM questionnaire and open questions data collection. The second phase of the study was focus group discussion (FGD).
Total sampling was used to determine the sample for the study’s first phase. Our inclusion criteria for the first phase were ophthalmology residents who have experience training in both main teaching hospitals and have attended a minimum of 6 months of ophthalmology residency training. Sixty residents met the inclusion criterion, and seven were excluded because they could not participate in the offline survey due to personal reasons. Fifty-three residents were included in the first phase of the study.
On the other hand, purposive sampling was employed to decide on phase two study participants. The PHEEM score, open-ended questions responses, and representation for each year of residency training were used to ensure heterogeneity of participants for different perspectives. Residents with high and low PHEEM scores and with exciting and evoking responses to open-ended questions were selected as respondents while considering resident representation for each year of training. Twenty residents were included in phase 2 of the study. The residents were divided into two groups consisting of 10 residents to attend FGD.
B. Study Instruments and Procedure
A cross-sectional survey that included a paper based PHEEM questionnaire, open-ended questions, and sociodemographic data, including age, gender, and year of residency, was distributed to all study subjects. The survey was conducted by single-trained data collector which was not part of the study program. Before administration, the study background, including its purposes and potential impacts, was explained to the residents and the written consent of each resident was obtained. Resident confidentiality and anonymity were also guaranteed.
The PHEEM consists of 40 items regarding LE subdivided into three subscales, each assessing perception of role of autonomy, perceptions of teaching, and perceptions of social support. It is scored on a 5-point Likert scale ranging from “strongly disagree” (0) to “strongly agree” (4), with a maximum score of 160. The findings were interpreted according to the original study shown in Supplement Table 1 (Roff et al., 2005). Four negative questions (questions 7, 8, 11, 13) were scored in reverse. PHEEM has been validated to assess the post-graduate clinical learning environment after the original study, including after translation to different languages, including the Bahasa Indonesia version (Raharjanti & Ramadianto, 2016; Roff et al., 2005). Multiple subsequent studies have shown good internal reliability (Bari et al., 2018; Clapham et al., 2007; Ong et al., 2019). The Bahasa Indonesia version of the PHEEM questionnaire was used to suit the local context. Bahasa Indonesia version of the PHEEM Questionnaire shows good validity and reliability (Raharjanti & Ramadianto, 2016). Eight open questions were added to the questionnaire. The questions were related to 3 subscales on the PHEEM questionnaire. Validation of the open-ended questions was done by expert judgment from two experts.
A semi-structured focus group session was conducted among the selected group of residents to supplement the PHEEM results. Two FGD session was done with a group size of ten. The FGD questions focused on exploring supporting and barrier factors that influence a good LE. The session lasted 60-90 minutes and was guided by a single-trained facilitator experienced in qualitative research methodology. FGD was conducted until new insights were no longer attained, reaching saturation.
Both quantitative and qualitative demographic data were coded by the trained data collector for maintaining the anonymity of the data. The response from both anonymous data were stored securely by the author for further analyses.
C. Statistical Analyses
Quantitative data were analysed using IBM Statistical Package for Social Sciences (SPSS) version 25. Descriptive statistics were presented using percentages, means, and standard deviation (SD). Internal reliability was assessed using Cronbach’s alpha coefficient. Comparison of quantitative data was made using Independent T-Test, Mann–Whitney U-Test, One-way ANOVA, and Kruskal–Wallis H-test. A p-value <0.05 was considered statistically significant.
For qualitative analyses, transcriptions of the open-ended questions answers and the audio and video recording of FGD were made by an independent data collector, and its accuracy was confirmed by the first author and the FGD facilitator. For open-ended questions, participants were coded with “P(Participant Code)-OEQ” (e.g. participant 1:P1-OEQ) while for FGD participants were coded with “P(Participant Code)-FGD(Group)” (e.g. participant 1 in FGD 2: P1-FGD2). The transcripts were coded into common themes independently by two investigators and discussed using thematic analysis using QDA Miner Version 5.0 for open questions and MAXQDA Analytics Pro 2020 for FGD.
III. RESULTS
A. Quantitative Data
Fifty-three ophthalmology residents were included in this mixed-method study, with the majority being female (64.15%). The mean age of residents was 30.96±2.18 years old. The largest age group is aged 30-34 (67.93%). 77.36% of respondents are at the internship stage or in the year 1 to 3 period of study, where respondents in year 3 have the most significant number of residents (32.08%).
Internal reliability of the PHEEM score was good, with Cronbach’s alpha coefficient of 0.872. No significant change with the removal of any of the 40 questions, proving its good internal reliability. Data in the perception of the role of autonomy was not normally distributed (P<0.05), but in the perception of teaching (P=0.200), perception of social support (P=0.200), also overall PHEEM score (P=0.200), the data were distributed normally.
As shown in Table 1, the mean score (SD) of the overall PHEEM score was 123.40±12.35, which is categorised as an excellent learning environment (LE) (>120). The mean perceptions for each subscale were 42.57±4.62 for perceptions of the role of autonomy classified as “more positive than negative”; 47.75±4.84 for perceptions of teaching classified as “model teachers”; 33.08±4.15 for perceptions of social support classified as “more pros than cons.”
|
No |
PHEEM Subscales |
Mean (SD) |
Interpretation |
Maximum Score |
|
1 |
Perceptions of role of autonomy |
42.57±4.62 |
more positive than negative |
56 |
|
2 |
Perceptions of teaching |
47.75±4.84 |
model teachers |
60 |
|
3 |
Perceptions of social support |
33.08±4.15 |
more pros than cons |
44 |
|
4 |
Overall PHEEM |
123.40±12.35 |
Excellent |
160 |
Table 1. The PHEEM scores
Abbreviation: PHEEM, Postgraduate Hospital Environment Measure; SD, Standard Deviation.
From the overall PHEEM item, there are 28 items with an average score >3, nine items in the perception of the role of autonomy, twelve items in teaching perception, and seven items in the perception of social support (Table 2). Only one item has a score >3.5 or is classified as real positive points; that is item number 3 (I have protected educational time in this post) for the perception of teaching. The highest score for the perception of the role of autonomy was item 34 (The training in this post makes me feel ready to be a consultant) and item 24 (I feel physically safe within the hospital environment) in the perception of social support.
Only one item with an average score of <2, indicated as a problem area which is item number 26 (There are adequate catering facilities when I am on call) in the perception of social support (Table 2). In the perception of the role of autonomy, item 8 (I must perform inappropriate tasks*) have the lowest score, while item 31 (My clinical teachers are accessible) has the lowest score under the perception of teaching (Table 2).
|
Code |
Item |
Mean±SD |
|
|
Perception of role of autonomy |
|||
|
34 |
The training in this post makes me feel ready to be a consultant |
3.40±0.53 |
|
|
40 |
My clinical teachers promote an atmosphere of mutual respect |
3.34±0.48 |
|
|
30 |
I have opportunities to acquire the appropriate practical procedures for my residency |
3.32±0.51 |
|
|
29 |
I feel part of a team working here |
3.21±0.49 |
|
|
5 |
I have the appropriate level of responsibility in this post |
3.19±0.56 |
|
|
18 |
I have the opportunity to provide continuity of care |
3.19±0.44 |
|
|
1 |
I have an employment contract that provides information about hours of work |
3.15±0.72 |
|
|
32 |
My workload in this job is fine |
3.02±0.50 |
|
|
4 |
I had an informative induction program |
3.00±0.59 |
|
|
14 |
There are clear clinical protocols in this post |
2.98±0.64 |
|
|
17 |
My work hours are in accordance to the national limits of working hours per day and week for physicians |
2.74±0.79 |
|
|
9 |
There is an informative Junior Doctors Handbook |
2.70±0.72 |
|
|
11* |
I am bleeped (called) inappropriately* |
2.68±0.89 |
|
|
8* |
I have to perform inappropriate tasks* |
2.66±0.88 |
|
|
Perception of teaching |
|||
|
3 |
I have protected educational time in this post |
3.51±0.58 |
|
|
2 |
My clinical teachers set clear expectation |
3.47±0.54 |
|
|
37 |
My clinical teachers encourage me to be an independent learner |
3.40±0.49 |
|
|
28 |
My clinical teachers have good teaching skills |
3.38±0.49 |
|
|
12 |
I am able to participate actively in educational events |
3.28±0.53 |
|
|
10 |
My clinical teachers have good communication skills |
3.25±0.55 |
|
|
27 |
I have enough clinical learning opportunities for my needs |
3.23±0.42 |
|
|
15 |
My clinical teachers are enthusiastic |
3.15±0.57 |
|
|
21 |
There is access to an educational program relevant to my needs |
3.15±0.53 |
|
|
23 |
My clinical teachers are well organised |
3.15±0.53 |
|
|
6 |
I have good clinical supervision at all times |
3.06±0.66 |
|
|
33 |
Senior staff utilise learning opportunities effectively |
3.06±0.41 |
|
|
39 |
The clinical teachers provide me with good feedback on my strengths and weaknesses |
2.98±0.57 |
|
|
22 |
I get regular feedback from seniors |
2.92±0.70 |
|
|
31 |
My clinical teachers are accessible |
2.77±0.61 |
|
|
Perception of Social Support |
|
||
|
24 |
I feel physically safe within the hospital environment |
3.36±0.59 |
|
|
13* |
There is sex discrimination in this post* |
3.30±0.99 |
|
|
7* |
There is racism in this post* |
3.28±0.84 |
|
|
35 |
My clinical teachers have good mentoring skills |
3.28±0.53 |
|
|
16 |
I have good collaboration with other doctors in my residency |
3.25±0.52 |
|
|
36 |
I get a lot of enjoyment out of my present job |
3.15±0.53 |
|
|
20 |
This hospital has good quality accommodation for junior doctors, especially when on call |
3.04±0.71 |
|
|
38 |
There are good counselling opportunities for junior doctors who fail to complete their training satisfactorily |
2.98±0.66 |
|
|
19 |
I have suitable access to careers advice |
2.94±0.66 |
|
|
25 |
There is a no-blame culture in this post |
2.53±0.93 |
|
|
26 |
There are adequate catering facilities when I am on call |
1.96±1.02 |
|
Table 2. Mean score in each item on the PHEEM questionnaire
Notes: Ordered by highest score in each subscale; *negative statement.
Abbreviation: SD, Standard Deviation.
In Table 3, an analysis of the relationship between student perception and gender from total PHEEM score showed no significant difference (P= 0.863). The mean scores of females were higher than males for the perception of teaching and social support, although not significantly different (P= 0.209 & P= 0.869). Conversely, in the perception of autonomy, the mean scores of females were lower than males but also not statistically significant (P= 0.212). The biggest difference between male and female perceptions is the perception of teaching.
|
Sample’s Characteristics |
Total PHEEM Scores |
Perception of Role of Autonomy |
Perception of Teaching |
Perception of Social Support |
|||||||
|
Mean±SD |
p |
Mean±SD |
p |
Mean±SD |
p |
Mean±SD |
p |
|
|||
|
Gender |
|
|
|
|
|
|
|
|
|
||
|
Male |
123.00±13.24 |
0.863a |
43.42±5.00 |
0.212b |
46.63±5.20 |
0.209a |
32.95±4.44 |
0.869a |
|
||
|
Female |
123.62±12.03) |
42.09±4.40 |
48.38±4.58 |
33.15±4.05 |
|
||||||
|
Years of Study |
|
||||||||||
|
Year 1 |
123.9±9.39 |
0.273c |
42.40±4.40 |
0.163d |
48.40±3.60 |
0.363c |
33.10±2.81 |
0.444c |
|
||
|
Year 2 |
126.2±12.49 |
43.57±5.32 |
48.43±4.89 |
34.21±3.49 |
|
||||||
|
Year 3 |
122.7±13.87 |
42.65±4.24 |
47.71±5.52 |
32.35±5.50 |
|
||||||
|
Year 4 |
115.7±6.14 |
39.50±2.56 |
44.75±3.28 |
31.50±1.85 |
|
||||||
|
Year 5 or more |
130.50±18.08 |
45.25±6.24 |
50.00±6.38 |
35.25±5.62 |
|
||||||
Table 3. Correlation between sample’s characteristics and perception
Abbreviation: PHEEM, Postgraduate Hospital Environment Measure; SD, Standard Deviation.
aindependent sample t-test; bMann-Whitney test; cOne Way ANOVA test; dKruskall-Wallis test
No significant differences were found for a mean of total PHEEM scores among years of the study group (P= 0.273), as well as in perceptions of the role of autonomy (P= 0.163), perceptions of teaching (P= 0.363) and perceptions of social support (P= 0.444). However, there are similar trends in both total PHEEM scores and perceptions of autonomy, teaching, and social support, in which the score of year 2 was higher than that of year 1, the lowest score in the year four student group, and the highest score in the 5th year student group or above.
The data supporting the quantitative findings of this study are openly available in Figshare at https://doi.org/10.6084/m9.figshare.23606157 (Kamaruddin et al., 2023).
B. Qualitative Data
Six open-ended questions were administered along with the PHEEM questionnaire. Thematic analyses revealed 12 themes in which residents have a positive perception of their LE and 10 themes that could be a barrier because residents have a negative perception of their LE (Appendix 1). Two FGDs were conducted with 10 participants in each group. Eleven participants were from year one and two, and the rest was from year three or more. Eight males and 12 females participated. From FGD results, we could also classify residents’ perceptions into 8 positive and 11 negative perception themes (Appendix 1).
Based on the themes found in both open-ended questions and FGD, we transform and formulate the final theme by connecting and merging themes that occurred from both methods. The final theme’s transformation and formulation are presented in Appendix 1. Even though the number of themes was not significantly different from positive and negative perceptions, we can see from the data transformation (based on % code and count) that the propensity of the theme was towards the positive perception.
There is a total of 11 final themes, of which six themes were positive and five were negative perceptions.
The themes along with supporting statements are as follows:
|
Positive perception themes |
Supporting Statements |
|
1. A good clinical teacher |
“Clinical teachers in Ophthalmology Study Program are very competent, highly dedicated, and respect us as students.” – P52-OEQ |
|
2. Conducive learning atmosphere |
“The learning atmosphere is very conducive.” – P6-FGD1 |
|
3. Well-organised learning system |
“The schedule is in order; everything has been arranged, so it all depends on whether residents want to finish on time or not.” – P6-FGD2 |
|
4. Friendly social environment |
“I feel that the working environment or colleagues here are very good; the sense of family is felt even though I am not originally from this city.” – P29-OEQ |
|
5. Supporting colleague |
“Everything was safe here, delightful; we support each other.” – P5-FGD1 |
|
6. Well-established facilities |
“The facilities is good, all equipment is available and easy to access in the hospital.” – P15-OEQ |
|
Negative perception themes |
Supporting Statements |
|
1. Suboptimal facilities |
“Things that still need improvement are the facilities and infrastructure; the study program should be provided special rooms such as study rooms with libraries and computers to support us to complete our tasks.” – P50-OEQ |
|
2. Inadequate learning opportunities (discrimination issue) |
“There are still teachers who seem to discriminate between residents.” – P46-OEQ |
|
3. Inappropriate tasks |
“all administrative tasks be imposed on the resident, and everything must be sorted out in our hands; the nurse is just left to take care of everything that has been done.” – P8-FGD2 |
|
4. Less mentoring time |
“What is lacking is the supervisor’s time to provide mentoring; there are still several clinical teachers who lack time to provide discussion, and there are even some who directly accept the scientific task without going through discussion.” – P3-FGD2 |
|
5. Lack of teaching hospitals/clinics |
“Maybe there can be an additional teaching hospital or clinic in Makassar.” – P10-FGD2 |
Table 4. Supporting statements of themes
C. Quantitative and Qualitative Data Integration
The integration of quantitative and qualitative data can be shown in Figure 1 and Supplement Table 2. Overall, the mean total PHEEM scores (123.40±12.35), which indicated an excellent LE environment, were confirmed by more positive perception themes compared with negative perception found in qualitative data analyses (Figure 1). Besides, we could also see that in each subscale, the composition of the themes connecting to each subscale could confirm the results of the quantitative data, whether the trend of the graphs is primarily high, average, or low. For example, in the perception of teaching, we could see mostly positive perception themes were connected to the subscale rather than negative perception; from this, we could say that the quantitative data of the perception of teaching in which mostly classified as model’s teacher was confirmed by its connection towards the final themes.

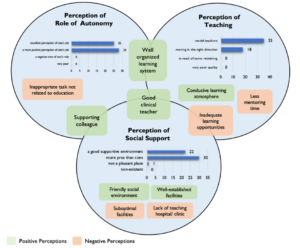
Figure 1. Integration of overall quantitative data classification with qualitative data
Quantitative data represent by graph and qualitative data (positive and negative perceptions) represent by box. Perceptions in the circle area means that it was connected to the area. Overlapping box in the circle means that perception was connected to more than one area.
In each subscale, the high and low items’ scores were confirmed with the final themes, both for positive and negative perception (Supplement Table 2). All positive perceptions confirmed quantitative results by related with a minimum of one item from 3 subscales with mostly high mean scores (>3). Only three negative perceptions related to a minimum of one item from 3 subscales with low scores (<3) confirm these themes’ relation to quantitative results. One negative perception (Inadequate learning opportunities among residents/discrimination issue) is connected to an item with high scores, showing that this theme did not confirm the quantitative finding. Two themes appear contradictory in positive and negative perceptions (well-established facilities and suboptimum facilities). Both themes were related to the same item in which the scores were not high or low, which could confirm the possibility from both perspectives.
IV. DISCUSSION
Our finding shows an excellent perception of LE of ophthalmology residents. Based on previously published articles, this study has the highest score for overall scores and for each subscale among peer-reviewed publications of PHEEM studies worldwide. The highest score from a previous peer-reviewed publication was a study by Ong et al. (2020), which reported a more positive than negative internal medicine residents’ perceptions of their LE in Singapore. On the contrary, Fisseha et al. (2021) and Liaqat et al. (2019) reported a plenty of problems LE from the perception of internal medicine residents in Ethiopia and pediatric surgery residents’ perception in Iran, respectively. Many factors, such as differences in discipline and sites of training, could cause the differences. There is no previous study yet about ophthalmic residents’ perception of LE using PHEEM. However, it is previously proved that some studies evaluated several different training programs reported that there is a difference in overall and subscale PHEEM scores among various training programs (Chan et al., 2016). In line with discipline, studies that evaluated different sites of training mainly reported that there is a different score between sites of training (Chan et al., 2016). Another reason for the difference could be a result of the differences in curriculum and teaching methods. Some studies reported increasing perception of LE after implementing modern curriculum and student-centred learning (Brown et al., 2011; Shankar et al., 2014). The themes found from our qualitative study also supported this excellent perception of residents toward their LE. Most of our themes were positive and related to all aspects of the PHEEM questionnaire. Gruppen et al. (2019) reported a conceptual framework of LE in which all components of the framework, i.e., personal, social, physical, and organisational, supported and covered by our positive perception themes finding, confirming the excellent perception of LE from the residents.
We did not find any different perceptions of LE between gender and year of study. Our findings were similar to some studies that reported no gender differences (Al-Shiekh et al., 2014; Ong et al., 2020; Sandhu et al., 2018). Other studies have different results; some studies reported that males have a better perception than females (Fisseha et al., 2021; Gough et al., 2010); on the contrary, Liaqat et al. (2019) reported a better perception of females than males. Similar to Risberg et al. (2003) that reported, gender issues were more significant and essential during clinical consultation than tutoring. Our qualitative data did not confirm our quantitative results. There is one negative perception theme in which some of our students feel that there is a discrimination issue related to learning opportunities; one of them is gender discrimination. Although our quantitative data show no differences between gender, the negative perception theme regarding discrimination issues must be taken into account by the stakeholder.
Concerning the year of training, we also found no significant difference in perception. The finding regarding different perceptions for different years of training was varied. Our result was the same with some studies (Ong et al., 2019; Sandhu et al., 2018), but other studies also reported higher PHEEM scores for senior to junior (Gough et al., 2010; Khoja, 2015; Liaqat et al., 2019; Pinnock et al., 2009), and some studies also reported that junior has better score than senior (Fisseha et al., 2021; Mahendran et al., 2013). The differences in perception of junior and senior residents could be explained by some reason, such as available access to educational opportunities (Mahendran et al., 2013), greater responsibility with increased seniority (Pinnock et al., 2009), and different training locations for trainees of different seniority (Khoja, 2015).
All subscales show promising results; residents’ perception of teaching was the highest among other subscales. Our qualitative data also support this finding; most of our positive theme was related to the perception of teaching, one of them being a good clinical teacher. Despite good perceptions on teaching, residents also experienced less mentoring time with clinical teachers. Fisseha et al. (2021) also reported the same issue. Inadequate supervision was proved to be a barrier in post-graduate medical education, as reported by Talib et al. (2019). Ong et al. (2019) also reported that focus group data suggested that inadequate supervisor contact and feedback resulted in negative perceptions of the LE. This finding informs us that residents need appropriate supervision, and clinical teachers should be understanding and prepared for their roles in residency training programs (Ramani & Leinster, 2008). Increasing learning time without any addition to supervisor-resident contact time still results in a low perception of LE (Silkens et al., 2018), proving the importance of the supervisor-resident relationship. Besides, good supervisory strategies proved to be contributed to a good LE (Boor, 2009). A good teaching environment influences the standard of the learning process (Al-Shiekh et al., 2014; Bari et al., 2018), satisfaction with education, and determines the outcome of the curriculum (Bari et al., 2018; Binsaleh et al., 2015). Faculty should focus on developing adequate supervision and teaching skills programs for clinical teachers.
Perception of social support has the lowest score among other; it is affirmed by our qualitative finding in which three negative perception was connected to this subscale. Similar results were also reported from studies in intensive care and pediatric training program (Al-Shiekh et al., 2014; Clapham et al., 2007). Related to social support, catering facilities is problem area of this study, other studies also identified this issue as a problem (Al-Shiekh et al., 2014; Binsaleh et al., 2015; Fisseha et al., 2021; Ong et al., 2020). This finding was not specifically appeared on FGD, but the strategy to solve the problem should be considered. Another interesting result related to social support is about facilities. The topic has both perspectives, positive and negative. Quantitative item related to this finding was not had very high or very low scores, supporting that some facilities were good, but there is still area for improvement, especially for diagnostic tools and surgical training facilities, as stated in FGD. Other studies also reported that suboptimal facilities related to hospital diagnostic tools were also a barrier to achieving good LE (Fisseha et al., 2021; Talib et al., 2019). Schönrock-Adema et al. (2012) have highlighted that interaction and collaboration with others were significant in determining the LE. Faculty should pay attention to social support as it has a vital role in a residency program, as it could alleviate the effects of stress, depression, and burnout (Vieira, 2008). Strategy to escalate this area should be considered, especially in providing good facilities for the learning process.
Residents’ perception of the role of autonomy is also satisfying, most of the positive themes confirmed this subscale. Good autonomy can improve decision-making skills, self-confidence, and responsibility, which further influence the readiness of residents to be independent (Allen et al., 2019). It also improves work satisfaction and can reduce burnout (Allen et al., 2019). Although overall autonomy perception was good, there are some areas for improvement. Our finding shows that residents were imposed with inappropriate tasks, such as administrative tasks. Some activities not related to education are also obligated to the residents at a certain level of training. This condition could lead to an excessive, inappropriate workload and interfere with protected educational time. Therefore, the faculty should set precise regulations regarding job descriptions and accountability.
Our study was done in the main teaching hospital which was part of a university-based study program, the results could be benefit for other hospital with same basis. It shows that university-based program has a good teaching area especially for the curriculum and teaching resources including human resources and facilities. University-based teaching hospital could enhance their program by maximising their teaching area also paying attention to some factors that could be a barrier in university-based program such as learning opportunity and inappropriate task.
A mixed method with explanatory sequential design is fundamental in our study as it provides a comprehensive perception of residents. Qualitative data make our finding more solid, show us some weaknesses, and emphasise our areas for improvement which are not easily identified from quantitative analyses. This is also a pioneer study for ophthalmology residents’ perception of LE, making our finding also crucial in adding insight to understanding residency LE from multiple perspectives. On the other hand, several limitations were also identified. First, our study was only done in one centre and discipline, which may limit data generalisability. Second, the study time constraint was cross-sectional, so the causative relation between factors could not be established. Third, differences perceptions in each different training year cannot be ascertained because there can be information bias related to the perceptions of second-year students and so on towards their experiences in previous years. Fourth, the researcher is a clinical lecturer from the program who conducted the study, which could be the subject of bias. However, a single trained data collector was used to collect open-ended questions data and facilitate FGD to reduce the possible bias effect.
V. CONCLUSION
In conclusion, our finding shows that our resident has an excellent perception of their ophthalmology residency training. The program has strong areas such as a good clinical teacher, a well-organised learning system, and a good social environment. Several areas should pay attention to, especially equal learning opportunities, mentoring time, and facilities. Faculty should organise strategies for preserving current LE and to further improve the LE along with monitoring and evaluation. Our finding could be benefit for other university-based teaching hospital especially in Asia regions to enhance their program. Further study involving multiple centres and disciplines should be done to give a more general perspective of LE in residency training.
Notes on Contributors
Muhammad Irfan Kamaruddin involved in conception or design of the work, data collection, data analysis and interpretation, drafting the article, critical revision of the article, and final approval of the version to be published.
Andi Alfian Zainuddin involved in conception or design of the work, data analysis and interpretation, critical revision of the article, and final approval of the version to be published.
Berti Julian Nelwan involved in conception or design of the work, critical revision of the article, and final approval of the version to be published.
Sri Asriyani involved in conception or design of the work, critical revision of the article, and final approval of the version to be published.
Firdaus Hamid involved in conception or design of the work, critical revision of the article, and final approval of the version to be published.
Tenri Esa involved in conception or design of the work, critical revision of the article, and final approval of the version to be published.
Irawan Yusuf involved in conception or design of the work, critical revision of the article, and final approval of the version to be published.
Ethical Approval
Before conducting the research, permission was obtained from Faculty of Medicine, Hasanuddin University Institutional Review Board (Reference number 36/UN4.6.4.5.31/PP36/2023). Participants were informed of the objectives and purpose of the study. They were invited to sign an informed consent if they agreed to be part of the study. Every participant was given a chance to deliberate on their rights to participate, refuse, or withdraw at any time they wished to do so.
Data Availability
The authors confirm that the data supporting the findings of this study are available within the article and its quantitative data along with supplemental tables are openly available in Figshare repository https://doi.org/10.6084/m9.figshare.23606157. Representative qualitative data translated into English are shown in the Result section (Kamaruddin et al., 2023). All qualitative data, open questions, and the FGD protocol which all written in Bahasa, are available from the corresponding author on reasonable request.
Acknowledgement
The authors would like to express our sincere gratitude to Ichlas Nanang Affandi from the Psychology study program, Faculty of Medicine, Hasanuddin University, for his valuable support throughout the research process. His expertise in qualitative study helps us to overcome challenges. In particular, we would like to thank Natalia Widiasih Raharjanti, MD, from the Department of Psychiatry, Faculty of Medicine University of Indonesia, and Assistant Professor Henok Fisseha, MD, from the Department of Internal Medicine, St. Paul’s Hospital Millennium Medical College, Addis Ababa, Ethiopia for their support in allowing us to use their research instrument and study protocol as one of our references in our research. Thank you also to Rusdina Bte Ladju, MD, Ph.D., for her valuable input to our manuscript. We are also grateful to the Department of Medical Education, Faculty of Medicine, Hasanuddin University, and Department of Ophthalmology, Faculty of Medicine, Hasanuddin University, for providing us with the resources and support needed to complete this study.
Funding
None of the authors receive any financial support for this study.
Declaration of Interest
The authors did not have a conflict of interest to be declared in this study.
References
Allen, M., Gawad, N., Park, L., & Raîche, I. (2019). The educational role of autonomy in medical training: A scoping review. Journal of Surgical Research, 240, 1–16. https://doi.org/10.1016/j.jss.2019.02.034
Al-Shiekh, M. H., Ismail, M. H., & Al-Khater, S. A. (2014). Validation of the postgraduate hospital educational environment measure at a Saudi university medical school. Saudi Medical Journal, 35(7), 734–738.
Bari, A., Khan, R. A., & Rathore, A. W. (2018). Postgraduate residents’ perception of the clinical learning environment; use of postgraduate hospital educational environment measure (PHEEM) in Pakistani context. The Journal of the Pakistan Medical Association, 68(3), 417–422.
Binsaleh, S., Babaeer, A., Alkhayal, A., & Madbouly, K. (2015). Evaluation of the learning environment of urology residency training using the postgraduate hospital educational environment measure inventory. Advances in Medical Education and Practice, 6, 271–277. https://doi.org/10.2147/AMEP.S81133
Boor, K. B. (2009). The clinical learning climate. [PhD-Thesis – Research external, graduation internal, S.I.]. s.n. https://research.vu.nl/en/publications/the-clinical-learning-climate
Brown, T., Williams, B., & Lynch, M. (2011). The Australian DREEM: Evaluating student perceptions of academic learning environments within eight health science courses. International Journal of Medical Education, 2, 94–101. https://doi.org/10.5116/ ijme.4e66.1b37
Chan, C. Y. W., Sum, M. Y., Lim, W. S., Chew, N. W. M., Samarasekera, D. D., & Sim, K. (2016). Adoption and correlates of postgraduate hospital educational environment measure (PHEEM) in the evaluation of learning environments – A systematic review. Medical Teacher, 38(12), 1248–1255. https://doi.org/10.1080/0142159X.2016.1210108
Clapham, M., Wall, D., & Batchelor, A. (2007). Educational environment in intensive care medicine—use of postgraduate hospital educational environment measure (PHEEM). Medical Teacher, 29(6), e184–e191. https://doi.org/10.1080/01421590701288580
Fisseha, H., Mulugeta, B., Argaw, A. M., & Kassu, R. A. (2021). Internal medicine residents’ perceptions of the learning environment of a residency training program in ethiopia: A mixed methods study. Advances in Medical Education and Practice, 12, 1175–1183. https://doi.org/10.2147/AMEP.S335205
General Medical Council. (2016). The state of medical education and practice in the UK. London (UK): General Medical Council. https://www.gmc-uk.org//media/documents/SOMEP_2016_Full_ Report_Lo_Res.pdf_68139324.pdf
Gough, J., Bullen, M., & Donath, S. (2010). PHEEM “Downunder.” Medical Teacher, 32(2), 161–163. https://doi.org/10.3109/01421590903509036
Gruppen, L. D., Irby, D. M., Durning, S. J., & Maggio, L. A. (2019). Conceptualizing learning environments in the health professions. Academic Medicine, 94(7), 969–974. https://doi.org/10.1097/ACM.0000000000002702
Kamaruddin, M. I., Zainuddin, A. A., Nelwan, B., Asriyani, S., Hamid, F., Esa, T., & Yusuf, I. (2023). Perceptions of the learning environment in ophthalmology residency training: A mixed method study [Data set]. Figshare.https://doi.org/10.6084/m9.figshare.23606157
Khoja, A. (2015). Evaluation of the educational environment of the Saudi family medicine residency training program. Journal of Family and Community Medicine, 22(1), 49. https://doi.org/10.4103/2230-8229.149591
Liaqat, N., Iqbal, A., & Dar, S. H. (2019). Assessment of environment of pediatric surgery residents of Pakistan using PHEEM. Iranian Journal of Pediatric Surgery, 5(1), 11–20. https://doi.org/10.22037/irjps.v5i1.22773
Mahendran, R., Broekman, B., Wong, J. C. M., Lai, Y. M., & Kua, E. H. (2013). The educational environment: Comparisons of the British and American postgraduate psychiatry training programmes in an Asian setting. Medical Teacher, 35(11), 959–961. https://doi.org/10.3109/0142159X.2013.815707
Ong, A., Fong, W., Chan, A., Phua, G., & Tham, C. (2020). Evaluating the educational environment in a residency programme in Singapore: can we help reduce burnout rates? Singapore Medical Journal, 61(9), 476–482. https://doi.org/10.11622/smedj.2019094
Ong, A. M.-L., Fong, W. W.-S., Chan, A. K.-W., Phua, G.-C., & Tham, C.-K. (2019). Using the postgraduate hospital educational environment measure to identify areas for improvement in a Singaporean residency program. Journal of Graduate Medical Education, 11(4s), 73–78. https://doi.org/10.4300/JGME-D-19-00234
Pinnock, R., Reed, P., & Wright, M. (2009). The learning environment of paediatric trainees in New Zealand. Journal of Paediatrics and Child Health, 45(9), 529–534. https://doi.org/10.1111/j.1440-1754.2009.01553.x
Prins, J. T., Hoekstra-Weebers, J. E. H. M., Gazendam-Donofrio, S. M., Dillingh, G. S., Bakker, A. B., Huisman, M., Jacobs, B., & van der Heijden, F. M. M. A. (2010). Burnout and engagement among resident doctors in the Netherlands: a national study. Medical Education, 44(3), 236–247. https://doi.org/10.1111/j.1365-2923.2009.03590.x
Raharjanti, N. W., & Ramadianto, A. S. (2016). Validity and reliability od postgraduate hospital educational environment measure – bahasa indonesia version. Jurnal Pendidikan Kedokte- ran Indonesia: The Indonesian Journal of Medical Educa- tion, 5(3), 157. https://doi.org/10.22146/jpki.25375
Ramani, S., & Leinster, S. (2008). AMEE Guide no. 34: Teaching in the clinical environment. Medical Teacher, 30(4), 347–364. https://doi.org/10.1080/01421590802061613
Ripp, J. A., Privitera, M. R., West, C. P., Leiter, R., Logio, L., Shapiro, J., & Bazari, H. (2017). Well-being in graduate medical education: A call for action. Academic Medicine, 92(7), 914–917. https://doi.org/10.1097/ACM.0000000000001735
Risberg, G., Johansson, E. E., Westman, G., & Hamberg, K. (2003). Gender in medicine – An issue for women only? A survey of physician teachers’ gender attitudes. International Journal for Equity in Health, 2(1), Article 10. https://doi.org/10.1186/1475-9276-2-10
Roff, S., McAleer, S., & Skinner, A. (2005). Development and validation of an instrument to measure the postgraduate clinical learning and teaching educational environment for hospital-based junior doctors in the UK. Medical Teacher, 27(4), 326–331. https://doi.org/10.1080/01421590500150874
Sandhu, A., Liaqat, N., Waheed, K., Ejaz, S., Khanum, A., Butt, A., Randhawa, F. A., & Dar, S. H. (2018). Evaluation of educational environment for postgraduate residents using Post Graduate Hospital Educational Environment Measure. The Journal of the Pakistan Medical Association, 68(5), 790–792.
Schönrock-Adema, J., Bouwkamp-Timmer, T., van Hell, E. A., & Cohen-Schotanus, J. (2012). Key elements in assessing the educational environment: Where is the theory? Advances in Health Sciences Education, 17(5), 727–742. https://doi.org/10.1007/s10459-011-9346-8
Shankar, P. R., Balasubramanium, R., Dwivedi, N. R., & Nuguri, V. (2014). Student feedback about the integrated curriculum in a Caribbean medical school. Journal of Educational Evaluation for Health Professions, 11, 23. https://doi.org/10.3352/jeehp.2014.11.23
Silkens, M. E. W. M., Chahine, S., Lombarts, K. M. J. M. H., & Arah, O. A. (2018). From good to excellent: Improving clinical departments’ learning climate in residency training. Medical Teacher, 40(3), 237–243. https://doi.org/10.1080/0142159X.2017.1398821
Talib, Z., Narayan, L., & Harrod, T. (2019). Postgraduate medical education in Sub-saharan Africa: A scoping review spanning 26 years and lessons learned. Journal of Graduate Medical Education, 11(4s), 34–46. https://doi.org/10.4300/JGME-D-19-00170
Vieira, J. E. (2008). The postgraduate hospital educational environment measure (PHEEM) questionnaire identifies quality of instruction as a key factor predicting academic achievement. Clinics, 63(6), 741–746. https://doi.org/10.1590/S1807-59322008000600006
*Muhammad Irfan Kamaruddin
Department of Medical Education,
Faculty of Medicine, Hasanuddin University,
Jalan Perintis Kemerdekaan KM 10
Makassar 90245
Email: iphenk_tampo@yahoo.com
Submitted: 6 October 2023
Accepted: 6 December 2023
Published online: 2 April, TAPS 2024, 9(2), 28-38
https://doi.org/10.29060/TAPS.2024-9-2/OA3151
Sinead Kado1, Simon Clarke2 & Sandra Carr1
1Division of Health Professions Education, School of Allied Health, University of Western Australia, Australia; 2Graduate School of Education, University of Western Australia, Australia
Abstract
Introduction: Health Professions Education (HPE) leadership development is advocated for success at the individual, team, and institutional levels. Many leadership theories exist informed mainly by Western perspectives, however, Pacific HPE leadership has not been investigated. Therefore, this research aimed to understand Pacific HPE leaders’ perspectives to develop substantive theory to guide faculty development in this setting and add nuanced perspectives to the international HPE leadership discourse.
Methods: Using an interpretivist case-study methodology, seven HPE leaders were purposefully recruited. Data collection tools included Rich Pictures, Talanoa Zoom interviews, and reflective journals. Participants drew a picture on ‘Being an HPE leader’, subsequently explaining their depiction, and then reflected on leadership events in their journals over six months. Codes and themes were identified using Miles, Huberman and Saldaña’s approach.
Results: Metaphors were assigned to three HPE leadership styles identified: The ‘Bridge’- helping students from novice to competent; the ‘Coconut Tree’- multiple roles and sturdy in the storm; and the ‘Boat’ – navigating towards the vision.
Conclusions: Rich Pictures, interviews and reflective journals allowed HPE leaders to reflect on ‘Being an HPE Leader’ and revealed tacit perspectives. This study suggests there are different styles of leadership, pertinent to the Pacific context, depending on the aims, strategies, and attributes of different HPE leaders. Although grounded in the Pacific, certain aspects may resonate in similar contexts. Notwithstanding that many facets of leadership identified align with current leadership models, intrapersonal emotional intelligence and cultural aspects of HPE leadership should be considered when designing contextually embedded faculty development.
Keywords: Medical Education, Health Professions Education, Leadership, Qualitative Research, Case Study, Pacific
Practice Highlights
- Rich Pictures assist revealing tacit perspectives by facilitating reflection on leadership.
- Many aspects of contemporary leadership are practiced in HPE leadership in the Pacific.
- Development of intrapersonal emotional intelligence is required to thrive in this challenging context.
- A better understanding of HPE Leadership in the Global South is required to inform a Global HPE leadership framework.
I. INTRODUCTION
Effective leadership is advocated to foster growth in the ever-evolving Health Professions Education (HPE) landscape and ensure success at the individual, team, and institutional levels (Lieff & Yammarino, 2016; McKimm & Swanwick, 2013; Sandhu, 2019; Steinert et al., 2012). However, Health Professions Education (HPE) leadership is a complex social phenomenon encompassing relationships, cultural and personal influences (Steinert et al., 2012; van Diggele et al., 2020), making it difficult to define, and then guide development. Whilst many leadership development initiatives exist purporting to enhance leadership capabilities, multiple systematic reviews investigating leadership development at the undergraduate (Evans et al., 2023; Lyons et al., 2018; Rodríguez-Feria et al., 2023), graduate (Lyons et al., 2021; Onyura et al., 2019; Sadowski et al., 2018; Sultan et al., 2019) and faculty (Steinert et al., 2012) level found that leadership development is rarely grounded in theoretical frameworks and that evaluation of interventions remains superficial. Similar issues occur in other HPE disciplines including pharmacy (Reed et al., 2019) and interprofessional (Brewer et al., 2016) education. These systematic reviews recommend that leadership development needs grounding in theoretical frameworks and capabilities assessed over a longitudinal period.
Additionally, across the reviews there was a dearth of studies from the global south informing their conclusions; most studies originated from the United States followed by the UK, Canada, Europe and Australia. Although established frameworks exist for physician leadership, including CanMEDS, NHS medical leadership competency framework, and ACGME, (Onyura et al., 2019) there is only one recently proposed for health professions educators (McKimm et al., 2022), based on the authors’ expertise and contemporary leadership theories, but not on empirical literature around HPE leadership. However, recommendations are that to develop tomorrow’s HPE leaders an empirically informed, culturally sensitive, leadership framework for health professions educators is required (Ramani et al., 2020; Sandhu, 2019).
Empirical research around HPE leadership has mainly been deductively analysed, using Western leadership frameworks, including Yukl’s power model (Sundberg et al., 2015), Bolman and Deal’s four frames model of leadership (Lieff, 2010), Goleman’s six leadership styles (Saxena et al., 2017), and character-based leadership (Torti et al., 2022). This deductive analysis potentially misses important aspects of leadership, indeed one example of subsequent inductive analysis identified different themes including reflection and feedback not included in the original deductive analysis (Lieff & Albert, 2012; Lieff, 2010). Additionally, most empirical research has relied on semi-structured interviews alone (Lieff et al., 2013; Lieff, 2010; Saxena et al., 2017; Sundberg et al., 2015; Torti et al., 2022), which may not have encapsulated all aspects of leadership, and have been conducted in Western contexts. Spoken language may not convey all the cultural contexts and meanings (Amazonas et al., 2019; Brocklesby & Beall, 2018; Lyon, 2020) and therefore it is recommended considering complementary data collection tools to further our understanding of HPE leadership (Lieff & Albert, 2012; Varpio et al., 2017). Furthermore, there are consistent calls to investigate HPE leadership in different cultural contexts to inform a faculty development framework (Dujeepa et al., 2019; Steinert et al., 2012; Varpio et al., 2017).
From a Pacific perspective, HPE leadership development is required (Kado et al., 2022; Sweet et al., 2018), however, HPE leadership from the cultural perspective of contemporary leaders in the Pacific is not currently described. Thus, this research reported here embarked on understanding the perspectives of current HPE leaders from this Pacific global south context to provide empirical evidence towards a framework for HPE leadership in this setting to guide faculty development. Furthermore, it contributes a diverse perspective to the current HPE leadership literature to assist building a more nuanced global HPE leadership theory.
This article describes the empirical research conducted at a major Pacific University utilizing an interpretivist case study approach. It then outlines three styles of leadership identified and discusses how these relate to competencies purported to be needed at different levels of leadership and the current theoretical and empirical discourse around HPE leadership. Implications from this discussion will provide recommendations for Pacific faculty development. Through rich, deep description it is hoped that others in similar settings will resonate with the findings, drawing on insights to apply in their own contexts.
II. METHODS
To understand Pacific perspectives around HPE leadership an interpretivist case study was undertaken at a major Pacific University (Denzin & Lincoln, 2000; Silverman, 1997). A qualitative methodology facilitated participants’ perspectives to be fully explored, and using several innovative data sets through a case study approach enabled tacit perspectives to be revealed and triangulated (Merriam, 1988; Merriam & Tisdell, 2016). The case was bound by health professionals who had completed a health education degree and had an active University HPE leadership role. Seven of ten eligible HPE leaders volunteered following purposeful recruitment and ethics approval. Written consent was provided and then data were collected through Rich Pictures, Talanoa interviews, and reflective journals over a one-year period (April 2021 to April 2022), with each participant assigned a pseudonym to maintain anonymity. Each data collection method was chosen to provide rich data to complement and build the interpretation of Pacific HPE leadership guided by the central research question ‘What are the perspectives of Pacific GCME graduates on being an HPE leader?’
First, Rich Pictures (Cristancho & Helmich, 2019; Gisby et al., 2023; Kado et al., 2023a) were used to reveal tacit perspectives on being an HPE leader. Participants drew a picture depicting ‘Being an HPE leader’ and then a subsequent Talanoa interview (Hindley et al., 2020; Tunufa’i, 2016) explored the deeper meanings of the picture and how they enacted leadership. Talanoa is a Pacific way of communicating where people are free to ‘tala’- talk ‘noa’- around the subject (Hindley et al., 2020). Thus, similar to semi-structured interviews, a set of guiding questions was used such as ‘Tell me about your picture’ and ‘How do you see yourself as an educational leader in this picture’, nevertheless the participants were allowed to ‘talanoa’ or talk around these questions in a culturally comfortable manner. These Talanoa interviews were held via Zoom (Gray et al., 2020) as the research was conducted in the midst of the Covid-19 pandemic. Next, following an orientation session on reflection (Schön, 1987), participants were requested to use a reflective journal with guiding questions and reflective prompts over six months. The reflective journals (Filep et al., 2018; Milligan & Bartlett, 2018) provided an avenue for the HPE leaders to reflect on doing leadership contemporaneously and with minimal influence from the researcher (Alaszewski, 2006). Finally, the second Talanoa interview was conducted, as planned after initial data analysis, exploring aspects of motivation and the influence of culture more deeply, with questions such as: ‘What motivates you to continue in your role as an HPE leader?’ and ‘How do you think the culture has shaped your leadership journey?’
A. Data Analysis
Data analysis was guided by Bell et al.’s (2019) framework for the Rich Pictures and Miles, Huberman and Saldaña’s (2014) approach for the textual data. Bell et al.’s (2019) framework comprises seven steps including:
- Locating the style – context of the Rich Picture
- Descriptive features – colour, shapes, and drawings
- Primary features – which aspects are bold or central
- Value features – linkages between images
- Low-level interpretation – overall picture
- High-level interpretation – interpretation from the artist
- Critical judgement – has the participant reflected and engaged with the drawing?
For this research, we relied primarily on the high-level interpretation and other aspects were asked in the Talanoa interview as the research was based on the participants’ perspectives.
Data analysis began immediately after the interviews with the primary researcher (SK) noting initial impressions in her research journal and then transcribing the interviews verbatim. Data were anonymised and entered into NVivo for further analysis, copies of the transcripts were also stored in the University’s data management system. The data were further analysed using Miles, Huberman and Saldaña’s (2014) approach which consists of three linked stages:
1) Data Condensation:
Data condensation involves ensuring relevant data to answer the research question is captured and synthesised through coding, memoing and developing concepts.
2) Data Display:
Data is displayed using data summaries and pictorial illustrations to convey the main ideas.
3) Drawing and Verifying Conclusions:
Conclusions illustrate the themes and propositions abstracted from the data display.
This article focuses on the results of the second stage of data analysis, data display, which illustrated three styles of leadership identified through data interpretation. Initial coding was done by the primary researcher (SK) and discussed with the principal supervisor (SC) to refine. Concepts were developed together and the data summaries were compiled by SK and then revised through discussion (SK, SC & SC). The process was iterative where new codes and concepts were discussed and transcripts re-read to ensure alignment. Finally, composite narratives were produced for each leadership style, consisting of the participants’ voices combined to maintain anonymity, (Willis, 2018) and a synopsis of each style of leadership was interpreted by the primary researcher, providing rich data summaries for the leadership styles identified. These can be accessed through Figshare: https://doi.org/10.6084/m9.figshare.24241195.v1 (Kado et al., 2023b)
B. Researcher Positionality
The primary researcher is a white, Anglo-Saxon, medical educator who had completed medical training in the UK and then subsequently lived and worked in a Pacific culture for over 20 years. She completed the health education degree with the research participants and was known to them. At the time of the research, she was not employed at the Pacific University and had no authority over them. Whilst having a deep understanding of the culture and context in which the research was conducted, there is the possibility that her Western upbringing will have influenced the interpretation. This was minimised by taking steps to ensure trustworthiness.
C. Trustworthiness
Trustworthiness was maintained through several avenues. First, the primary researcher practised reflexivity by maintaining a diary throughout the research process to note ideas and meanings from the data. Second, triangulation of the results occurred through data analysis discussions with the research team and differences agreed to. Third, member checking was utilised at each step of the analysis whereby research participants were asked to confirm the transcripts, composite narratives and summaries, and the leadership styles.
D. Ethics Approval
Ethics approval was granted by the University of Western Australia (UWA – 2019/RA/4/20/6529) and the Fijian Ministry of Health (Fiji – FNHRERC 31/2020). Furthermore, the University ethics department was consulted and they gained access to the participants ensuring they felt under no obligation to participate in the research.
III. RESULTS
Seven HPE leaders participated, their academic positions, ethnicities, specialities, years of service and age range are depicted in Figure 1. One participant had originated from a Global South country outside the Pacific but had resided in the Pacific for over 25 years.
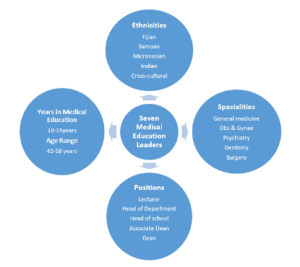
Figure 1. Demographics of Pacific HPE Leaders
Three styles of leadership were interpreted from the data and assigned visual metaphors, which were conceptualised based on the participants’ drawings, the Pacific culture and the participants’ perspectives of being an HPE leader. First, ‘Being a Bridge’ – HPE leaders focusing on being effective educators and clinicians. Second, ‘Being a Coconut Tree’ – HPE leaders aiming to develop faculty whilst also maintaining their clinical and educator identities. Third, ‘Being a Boat’ HPE leaders who were mostly aiming for organisational change. Interestingly, only the ‘Boats’ had received any form of leadership development and this was not directly related to HPE leadership. Each of these styles of leadership is now examined in turn.
A. Being a Bridge
Three HPE leaders, Jasmine, John, and Jeremiah, identified as ‘Being a Bridge’, illustrated by Jasmine’s Rich Picture and Talanoa interview excerpt (Figure 2).

Figure 2. Being a Bridge
Being a Bridge encompassed being passionate about clinical education and having a love of teaching. These HPE leaders’ aims were to develop the next generation of health professionals to be competent and caring. To achieve these aims they nurtured their students helping them cross the bridge from novice to competent by understanding their students, scaffolding learning, enabling practice and being a good role model.
‘We expect them to go into the community and to be a good doctor, [and] according to me, that should be someone who is a good clinician, who is a leader and educator, who is socially accountable, compassionate, and cares about the well-being of the community in general. That is where I stand within the medical school trying to achieve that goal.’
-John (1st Interview)
They aspired to share their knowledge, skills, and attributes with their students to enable them to improve Pacific people’s health. Notwithstanding the struggles and barriers they faced through University processes and the COVID-19 pandemic, they strove to find new educational techniques to ensure students had the best learning opportunities possible.
‘I feel as an educational leader within this system, that we are bound by too many of these system issues, rules and regulations and principals…they feel restrictive, I don’t feel good about it and that is a continuing struggle.’
-John (1st Interview)
‘One thing that I have really appreciated is the multidisciplinary way of teaching. So that is something new, early stages.’
-Jasmine (1st Interview)
They valued the educational development they had received and advocated for future collaborations to develop this further, including structured courses, guidelines and mentorship.
‘Well, one important factor that I believe will influence me as an educator is continuing education. Getting that collegiality again. We need another project to work on.’
-Jeremiah (2nd Interview)
‘Being a Bridge’ focused on developing students as an HPE leader which was expanded on by leaders who were identified as ‘Being a Coconut Tree’.
B. Being a Coconut Tree
Jane and Judith exemplified ‘Being a Coconut Tree’ with their multiple responsibilities, experiences and resilience. Figure 3 illustrates the Rich Picture alongside an excerpt from the interview of Jane.

Figure 3. Being a Coconut Tree
The ‘coconut trees’ of HPE leadership had multiple roles and a passion for developing and helping others. Their multiple fronds as HPE leaders included primarily being a clinician and educator, alongside a researcher, administrator, committee lead, and organisation member. They are aiming to ensure excellence and achieve this by valuing both feedback and evaluation to improve themselves, others and the curriculum.
‘I am basically multitasking, I can wear different hats and can achieve a lot of things with the different activities. So, we are teaching, teaching, but we are also at the same time we are learning ourselves, and not just because of a one way delivery, it’s two ways, we get the feedback from the students’
-Judith (1st Interview)
They are rooted in the foundations of faculty development (GCME – Graduate Certificate of Medical Education) and have grown strong, sturdy and resilient, and yet adaptable to the constant changes and challenges they face. Their experiences have enabled them to grow in confidence but also to nurture others to develop their own leadership style. Jane and Judith understand the importance of working together towards a common goal and ensuring the team is committed and feels valued, providing the support that is required.
‘And I think the way GCME was structured and taught I think that really helped us. If you look at who’s holding these leadership roles, it’s those who did GCME’.
-Judith (2nd Interview)
‘We have a group of young faculty staff who wants to make a difference as medical educators and I believe my leadership style is more of a coach.’
-Judith (Reflective Journal)
Although they are juggling many roles and at times feel overwhelmed they are committed to improving health education in the Pacific. They enlist the assistance of experts in this quest.
‘I have liaised with my network to ask for supplementary teaching for our Postgraduate trainees.’
-Jane (Reflective Journal)
Overall, they know they need to ‘walk the talk’ to develop the next generation of HPE leaders, as they endeavour to promote excellence in HPE.
C. Being a Boat
Being a Boat was illustrated by Julie and James who were striving to sail to a vision on the horizon to improve HPE at the individual and organisational level. James describes this as a journey with his Rich Picture and interview excerpt (Figure 4).

Figure 4. Being a Boat
James and Julie visualised themselves on a leadership journey in a boat heading towards a vision of excellence in health professions education. They are both intrinsically motivated to do their best by building a strong leadership team, utilising the strengths of the group and collaborating with external stakeholders.
Identify the strengths in people that we can nurture and play to the people’s strengths. If we play to the strength of people and all the strengths complement each other it’s really good.
-James (1st Interview)
Although they are both consultants in their clinical domain, their identity is now more embedded in their leadership role in health professions education. Their focus is on ensuring good curriculum, development for faculty and leaders, and improving University processes.
What we need is some more basic foundational learning…health professions education for the whole college and so that would be something I would totally pursue to allow and to think of something that would be doable.
-Julie (1st Interview)
Their journey is fraught with navigating University obstacles and the storms of change, especially the COVID-19 pandemic. These frustrations have left them exhausted and overwhelmed, on the verge of burnout, and in need of respite and support.
I had been frustrated with the processes and felt so much more could be done to support staff and students.
-Julie (Reflective Journal)
Stress in an already uncertain environment in the midst of a Pandemic.
-James (Reflective Journal)
The boat’s overall aim is to grow the next generation of HPE leaders across the whole college through curriculum development and support from the University.
IV. DISCUSSION
In our Pacific setting, all the HPE leaders were aiming to develop excellent healthcare workers to make a difference to the health of the Pacific, however, they did this in different ways. Three styles of leadership were identified across the HPE leaders, which were given visual metaphors of ‘The Bridge, Coconut Tree and Boat’. ‘The Bridges’ focused on developing competent and caring students, ‘The Coconut Trees’ had multiple roles and nurtured their successors as well as the students, and ‘The Boats’ focused on the system level to provide the necessary supports for HPE leaders and the students.
These three styles of leadership could be conceptualised as levels, similar to Maxwell’s (2011) five levels of leadership which classifies leadership as a process through position – a leadership title, permission – developing relationships, production – getting things done, people development – empowering others, and pinnacle – growing the organisation, however, McKimm et al. (2022) argue that all HPEs can be leaders, they do not need to be in a position of leadership. Although our participants were primarily in positions of leadership, they did not specifically identify that their position assisted or deterred their leadership journey, therefore, it is difficult to say if this positional status impacted their leadership style. From their interviews and journals, the HPE leaders were more focused on relationship building, the second level: permission. Each style of leadership focused on different aspects of building relationships: ‘The Bridges’ nurturing their students, ‘The Coconut Trees’ developing both students and faculty and ‘The Boats’ collaborating with faculty and external stakeholders to support the college. Relationship building or the interpersonal aspects of leadership were key in all styles of leadership. This is well supported across the theoretical (McKimm et al., 2022; Pinder & Shabbits, 2018; Sandhu, 2019) and empirical research (Lieff & Albert, 2012; Varpio et al., 2017) around HPE leadership.
Focusing on the next level, production, that is getting results from others through influence and credibility, all styles of HPE leaders were respected consultants in their field and were able to influence students, faculty, and the institution. Indeed, evidence suggests that to be a respected HPE leader it is necessary to first have a reputation as an excellent clinician or researcher as being a good educator is often perceived as less esteemed (Maile et al., 2019; Sundberg et al., 2015). Did this hamper their progression to the fourth level, reproduction? All styles of leadership encouraged empowering others, whether that be at the student or faculty level, although they utilised different strategies. ‘The Bridge’ acted as a role model to develop novice students into competent health professionals, ‘The Coconut Tree’ utilised a coaching style to nurture the next generation of HPEs and ‘The Boats’ focused on developing structures and courses within the University to ensure succession planning. The HPE leaders displayed an authentic approach to developing others by often ‘walking the talk’ and being open to feedback, especially the coconut trees (Lieff & Yammarino, 2016; McKimm et al., 2022). Finally, the impact the leaders had on the organisation varied and this is perhaps where the styles of leadership differed most in comparison to the final level of pinnacle, developing future HPE leaders and growing the university. This was an ideal envisioned by ‘The Bridges’ but was actualised by ‘The Coconut Trees’ at a local departmental level and by ‘The Boats’ at the wider college level. Here a more adaptive style of leadership was portrayed by engaging with the challenges of a low-resource setting and the pandemic and seeking innovative solutions to address them (McKimm et al., 2022).
We would argue that rather than moving through levels of leadership that all these factors, bar level one, position, are evident in the different styles of leadership portrayed in this setting, albeit expressed in different ways. Additionally, although adaptive leadership has been advocated for HPE leaders during these challenging times (McKimm et al., 2022) some aspects were not evident in our HPE leaders. While they acknowledged being stressed and frustrated there was little evidence of them identifying ways to build resilience and perseverance and other intrapersonal aspects of emotional intelligence (Goleman, 2001). To build HPE leaders’ emotional intelligence capacities we would advocate utilising faculty development strategies that enhance reflection, such as Rich Pictures, and cultural ‘Talanoa’ discussions to assist future HPE leaders in reflecting on their experiences and developing strategies to overcome their obstacles (Cammock et al., 2021; Kado et al., 2023a). We also concur with Lyons et al. (2021) that ‘bespoke’ faculty development is recommended to encompass different styles of leadership encountered in the Pacific cultural setting, rather than using frameworks from an entirely Western perspective.
A. Strengths and Limitations of the Research
This study is the first to our knowledge, investigating HPE leadership in a Pacific setting and it followed leaders over a prolonged period to obtain rich, deep data, using novel data collection methods such as Rich Pictures and Talanoa interviews enabling unique perspectives to be captured.
Nevertheless, there are several limitations including, a small sample size of seven participants at only one institution. This study was also conducted during the Covid-19 pandemic limiting face-to-face interactions which may have affected the findings attributable to Zoom interviews and the unprecedented experiences of the HPE leaders. Additionally, although several measures were taken to increase the trustworthiness of the research there is the real possibility that the findings have been affected by the unconscious biases of the primary researcher (SK).
V. CONCLUSION
Pacific HPE leaders displayed three styles of leadership that were conceptualised as ‘Being a Bridge’ – focusing on being an effective educator and clinician; ‘Being a Coconut Tree’ – aiming to develop faculty whilst also maintaining their clinical and educator identities; and ‘Being a Boat’ who were mostly aiming for organisational change. They accomplished these styles through similar strategies based on developing relationships, being credible and empowering others that are advocated in the different levels of leadership, and which mirrored aspects of authentic and adaptable leadership. However, although the Pacific HPE leaders identified themselves as resilient and adaptable they also expressed significant challenges in relation to the University and the Covid-19 pandemic in this low-resource global south setting. Intrapersonal aspects of emotional intelligence could strengthen HPE leaders’ resilience in this cultural setting through faculty development that encourages reflection, such as Rich Pictures and Talanoa.
Notes on Contributors
Dr Sinead Kado is a doctor, medical educator and PhD candidate who reviewed the literature, designed the study, and then collected and analysed the research data, before drafting the original manuscript.
Professor Simon Clarke is a senior honorary research fellow at the University of Western Australia who reviewed and revised the study design, reviewed the data analysis and critically revised the manuscript.
Professor Sandra Carr is the Head of Health Professions Education at the University of Western Australia who revised the study design, analysed the data and then critically revised the manuscript.
All authors have read and approved the final manuscript.
Ethical Approval
Ethics approval was granted by the University of Western Australia (UWA – 2019/RA/4/20/6529) and the Fijian Ministry of Health (Fiji – FNHRERC 31/2020).
Data Availability
Supplementary data in the form of composite narratives – the combined narratives of several participants, and the data summaries interpreted by the researchers are available in Figshare at https://doi.org/10.6084/m9.figshare.24241195.v1. Original full transcripts are not available due to anonymity and confidentiality issues.
Acknowledgement
The authors would like to acknowledge the research participants for their commitment and engagement with the research.
Funding
The primary researcher (SK) was in receipt of an Australian Government Research Training Program (RTP) scholarship for this research.
Declaration of Interest
The researchers declare that they have no known conflicts of interest, including financial, consultant, institutional and other relationships that might lead to bias.
References
Alaszewski, A. (2006). Using diaries for social research. SAGE Publications Ltd. https://doi.org/10.4135/9780857020215
Amazonas, I. T., Kawa, N. C., Zanetti, V., Linke, I., & Sinisgalli, P. A. (2019). Using rich pictures to model the ‘good life’ in indigenous communities of the tumucumaque complex in Brazilian Amazonia. Human Ecology, 47, 341-354. https://doi.org/10.1007/s10745-019-0076-5
Bell, S., Berg, T., & Morse, S. (2019). Towards an understanding of rich picture interpretation. Systemic Practice and Action Research, 32(6), 601-614. https://doi.org/10.1007/s11213-018-9476-5
Brewer, M. L., Flavell, H. L., Trede, F., & Smith, M. (2016). A scoping review to understand “leadership” in interprofessional education and practice. Journal of Interprofessional Care, 30(4), 408-415. https://doi.org/10.3109/13561820.2016.1150260
Brocklesby, J., & Beall, E. (2018). Processes of engagement and methodology design in community operational research – insights from the indigenous peoples sector. European Journal of Operational Research, 268(3), 996-1005. https://doi.org/10.1016/j.ejor.2017.07.053
Cammock, R., Conn, C., & Nayar, S. (2021). Strengthening Pacific voices through Talanoa participatory action research. AlterNative: An International Journal of Indigenous Peoples, 17(1), 120-129. https://doi.org/10.1177/1177180121996321
Cristancho, S. M., & Helmich, E. (2019). Rich pictures: a companion method for qualitative research in medical education. Medical Education, 53(9), 916-924. https://doi.org/10.1111 /medu. 13890
Denzin, N. K., & Lincoln, Y. S. (2000). Handbook of qualitative research (2nd ed.). Sage Publications.
Dujeepa, D. S., Ashokka, B., Su-Ping, Y., & Shuh-Shing, L. (2019). Understanding leadership: Perceptions among health professions educational leaders in the Asian setting. Journal of Medical Education, 23(3), 154-174. https://doi.org/10.6145/jme.2 01909_23(3).0002
Evans, M. A., James, E. J., & Misa, M. (2023). Leadership training in undergraduate medical education: A systematic review. International Journal of Medical Students, 11(1), 58-66. https://doi.org/10.5195/ijms.2023.1717
Filep, C. V., Turner, S., Eidse, N., Thompson-Fawcett, M., & Fitzsimons, S. (2018). Advancing rigour in solicited diary research. Qualitative Research, 18(4), 451-470. https://doi.org/10.1177/14 68794117728411
Gisby, A., Ross, C., Francis-Smythe, J., & Anderson, K. (2023). The ‘Rich Pictures’ method: Its use and value, and the implications for HRD research and practice. Human Resource Development Review, 0(Ahead of Print). https://doi.org/10.1177/15344843221148044
Goleman, D. (2001). The emotionally intelligent workplace; How to select for, measure and improve emotional intelligence in individuals, groups and organisations (1st ed.). Jossey-Bass.
Gray, L. M., Wong-Wylie, G., Rempel, G. R., & Cook, K. (2020). Expanding qualitative research interviewing strategies: Zoom video communications. The Qualitative Report, 25(5), 1292-1301. https://search.proquest.com/scholarly-journals/expanding-qualitative-research-interviewing/docview/2405672296/se-2?accountid=14681
Hindley, P., November, N., Sturm, S., & Wolfgramm-Foliaki, E. (2020). Rolling out the mat: Talanoa as a higher education research methodology. Theory and method in higher education research. Emerald Publishing Limited. https://doi.org/10.1108/s2056-37522 0200000006007
Kado, S., Clarke, S., & Carr, S. (2023a). ‘I would have never told you that’ – Using rich pictures as a qualitative tool to uncover tacit perspectives on leadership. International Journal of Qualitative Methods, 22. https://doi.org/10.1177/16094069231182633
Kado, S., Clarke, S., & Carr, S. (2023b). Supplementary data for Pacific perspectives on health professions education (HPE) leadership. https://doi.org/10.6084/m9.figshare.24241195.v1
Kado, S., Lindemann, I., & Brand, G. (2022). Supporting Pacific clinicians’ medical education practice change through faculty development: A qualitative case study. Focus on Health Professional Education: A Multi-Professional Journal, 23(3), 1-17. https://fohpe.org/FoHPE/article/view/598
Lieff, S., & Albert, M. (2012). What do we do? Practices and learning strategies of medical education leaders. Medical Teacher, 34(4), 312-319. https://doi.org/10.3109/0142159x.2012.643835
Lieff, S., Banack, J. G.-P., Baker, L., Martimianakis, M. A., Verma, S., Whiteside, C., & Reeves, S. (2013). Understanding the needs of department chairs in academic medicine. Academic Medicine, 88(7), 960-966. https://doi.org/10.1097/ACM.0b013e318294ff36
Lieff, S. J. (2010). The mindsets of medical education leaders: How do they conceive of their work? Academic Medicine, 85(1), 57-62. https://doi.org/10.1097/ACM.0b013e3181c46e47
Lieff, S. J., & Yammarino, F. J. (2016). How to lead the way through complexity, constraint, and uncertainty in academic health science centers. Academic Medicine, 92(5), 614-621. https://doi.org/10.1097/acm.0000000000001475
Lyon, P. (2020). The SAGE handbook of visual research methods. SAGE Publications, Inc. https://doi.org/10.4135/9781526417015
Lyons, O., George, R., Galante, J. R., Mafi, A., Fordwoh, T., Frich, J., & Geerts, J. M. (2021). Evidence-based medical leadership development: A systematic review. BMJ Leader, 5(3), 206-213. https://doi.org/10.1136/leader-2020-000360
Lyons, O., Su’a, B., Locke, M., & Hill, A. (2018). A systematic review of leadership training for medical students. New Zealand Medical Journal, 131(1468), 75-84. https://www.proquest.com/scholarly-journals/systematic-review-leadership-training-medical/docview/2052768826/se-2
Maile, E., McKimm, J., & Till, A. (2019). Exploring medical leader identity and its formation. Leadership in Health Services, 32(4), 584-599. https://doi.org/http://dx.doi.org/10.1108/LHS-12-2018-0066
Maxwell, J. (2011). The 5 levels of leadership: Proven steps to maximize your potential. Hachette Book Group.
McKimm, J., Ramani, S., Forrest, K., Bishop, J., Findyartini, A., Mills, C., Hassanien, M., Al-Hayani, A., Jones, P., Nadarajah, V. D., & Radu, G. (2022). Adaptive leadership during challenging times: Effective strategies for health professions educators: AMEE Guide No. 148. Medical Teacher, 1-11. https://doi.org/10.1080/01 42159X.2022.2057288
McKimm, J., & Swanwick, T. (2013). Educational leadership. In T. Swanwick (Ed.), Understanding medical education: Evidence, theory and practice. John Wiley & Sons. http://ebookcentral.proquest.com/lib/uwa/detail.action?docID=1547076
Merriam, S. B. (1988). Case study research in education: A qualitative approach (1st ed.). Jossey-Bass.
Merriam, S. B., & Tisdell, E. J. (2016). Qualitative Research: A guide to design and implementation. Jossey-Bass.
Miles, M. B., Huberman, A. M., & Saldaña, J. (2014). Qualitative data analysis: A methods sourcebook. SAGE Publications, Inc.
Milligan, C., & Bartlett, R. (2018). Solicited diary methods. In P. Liamputtong (Ed.), Handbook of research methods in health social sciences. Springer Singapore. https://doi.org/10.1007/978-981-10-2779-6_15-1
Onyura, B., Crann, S., Tannenbaum, D., Whittaker, M. K., Murdoch, S., & Freeman, R. (2019). Is postgraduate leadership education a match for the wicked problems of health systems leadership? A critical systematic review. Perspectives on Medical Education, 8(3), 133-142. https://doi.org/10.1007/s40037-019-05 17-2
Pinder, K. E., & Shabbits, J. A. (2018). Educational leadership during a decade of medical curricular innovation and renewal. Medical Teacher, 40(6), 578-581. https://doi.org/10.1080/014215 9x.2018.1440079
Ramani, S., McKimm, J., Thampy, H., O’Sullivan, P. S., Rogers, G. D., Turner, T. L., Chisolm, M. S., Kusurkar, R. A., Hays, R., Fornari, A., Kachur, E. K., Wilson, K. W., Filipe, H. P., & Schumacher, D. J. (2020). From clinical educators to educational scholars and leaders: Strategies for developing and advancing a career in health professions education. Clinical Teacher, 17(5), 477-482. https://doi.org/10.1111/tct.13144
Reed, B. N., Klutts, A. M., & Mattingly, T. J. (2019). A systematic review of leadership definitions, competencies, and assessment methods in pharmacy education. American Journal of Pharmaceutical Education, 83(9), 1873-1885.https://doi.org/10.5 688/ajpe7520
Rodríguez-Feria, P., Czabanowska, K., Babich, S., Rodríguez-Sánchez, D., Carreño Hernández, F. L., & Hernández Flórez, L. J. (2023). Defining leadership in undergraduate medical education, networks, and instructors: A scoping review. International Medical Education, 2(1), 49-70. https://doi.org/10.3390/ime2010006
Sadowski, B., Cantrell, S., Barelski, A., O’Malley, P. G., & Hartzell, J. D. (2018). Leadership training in graduate medical education: A systematic review. Journal of Graduate Medical Education, 10(2), 134-148. https://doi.org/10.4300/jgme-d-17-00194.1
Sandhu, D. (2019). Healthcare educational leadership in the twenty-first century. Medical Teacher, 41(6), 614-618. https://doi.org/10.1080/0142159x.2019.1595555
Saxena, A., Desanghere, L., Stobart, K., & Walker, K. (2017). Goleman’s leadership styles at different hierarchical levels in medical education. BMC Medical Education, 17(1), 169. https://doi.org/10.1186/s12909-017-0995-z
Schön, D. A. (1987). Educating the reflective practitioner. Jossey-Bass.
Silverman, D. (1997). Qualitative research – theory, method and practice. Sage.
Steinert, Y., Naismith, L., & Mann, K. (2012). Faculty development initiatives designed to promote leadership in medical education. A BEME systematic review: BEME Guide No. 19. Medical Teacher, 34(6), 483-503. https://doi.org/10.3109/01421 59x.2012.680937
Sultan, N., Torti, J., Haddara, W., Inayat, A., Inayat, H., & Lingard, L. (2019). Leadership development in postgraduate medical education: A systematic review of the literature. Academic Medicine, 94(3), 440-449. https://doi.org/10.1097/acm.0000000000002503
Sundberg, K., Josephson, A., Reeves, S., & Nordquist, J. (2015). Power and resistance: Leading change in medical education. Studies in Higher Education (Dorchester-on-Thames), 42(3), 445-462. https://doi.org/10.1080/03075079.2015.1052735
Sweet, L., Young, L., & Kado, S. (2018). Enhancing health professional education capacity in the Western Pacific region. Rural and Remote Health, 18(3), 4306-4311. https://doi.org/10.22605/RRH4306
Torti, J. M. I., Inayat, H., Inayat, A., Lingard, L., Haddara, W., & Sultan, N. (2022). Perspectives on physician leadership: The role of character-based leadership in medicine. Medical Education. https://doi.org/10.1111/medu.14875
Tunufa’i, L. (2016). Pacific research: Rethinking the Talanoa ‘methodology’. New Zealand Sociology, 31(7), 227-239. https://www.proquest.com/scholarly-journals/pacific-research-rethinking-talanoa-methodology/docview/1882017954/se-2?accountid=14681
van Diggele, C., Burgess, A., Roberts, C., & Mellis, C. (2020). Leadership in healthcare education. BMC Medical Education, 20(Suppl 2), 456-456. https://doi.org/10.1186/s12909-020-02288-x
Varpio, L., O’Brien, B., J. Durning, S., van der Vleuten, C., Gruppen, L., ten Cate, O., Humphrey-Murto, S., Irby, D. M., Hamstra, S. J., & Hu, W. (2017). Health professions education scholarship unit leaders as institutional entrepreneurs. Academic Medicine, 92(8), 1189-1195. https://doi.org/10.1097/acm.0000000000001576
Willis, R. (2018). The use of composite narratives to present interview findings. Qualitative Research, 19(4), 471-480. https://doi.org/10.1177/1468794118787711
*Sinead Kado
Division of Health Professions Education,
University of Western Australia
Perth, 6009, Australia
Email: sinead.kado@research.uwa.edu.au
Submitted: 16 July 2023
Accepted: 21 December 2023
Published online: 2 April, TAPS 2024, 9(2), 18-27
https://doi.org/10.29060/TAPS.2024-9-2/OA3098
Natalia Puspadewi
Medical Education Unit, School of Medicine and Health Sciences, Atma Jaya Catholic University of Indonesia, Indonesia
Abstract
Introduction: Developing a professional identity involves understanding what it means to be a professional in a certain sociocultural context. Hence, defining the characteristics and/or attributes of a professional (ideal) physician is an important step in developing educational strategies that support professional identity formation. To date, there are still limited studies that explore undergraduate medical students’ professional identity. This study aimed to define the characteristics and/or attributes of an ideal physician from five first-year and three fourth-year undergraduate medical students.
Methods: Qualitative case studies were conducted with eight undergraduate medical students from a private Catholic medical school in Jakarta, Indonesia. The study findings were generated from participants’ in-depth interviews using in vivo coding and thematic analysis. Findings were triangulated with supporting evidence obtained from classroom observations and faculty interviews.
Results: First-year participants modeled their professional identities based on their memorable prior interactions with one or more physicians. They mainly cited humanistic attributes as a part of their professional identity. Fourth-year participants emphasised clinical competence and excellence as a major part of their professional identities, while maintaining humanistic and social responsibilities as supporting attributes. Several characteristics unique to Indonesian’s physician identity were ‘Pengayom’ and ‘Jiwa Sosial’.
Conclusion: Study participants defined their professional identities based on Indonesian societal perceptions of physicians, prior interactions with healthcare, and interactions with medical educators during formal and informal learning activities.
Keywords: Professional Identity Formation, Indonesia Undergraduate Medical Students, Physician Identity
Practice Highlights
- Defining the attributes of ideal physicians is important for developing strategies that support PI.
- Prior interactions with healthcare and formal/informal learning activities influence PI definition.
I. INTRODUCTION
Supporting the (trans)formation of a medical student’s identity, from a layperson to a professional, is an important process in preparing future physicians (Cruess et al., 2014; Goldie, 2012; Wald, 2015). This process includes professional identity formation (PIF) throughout their medical education continuum. Professional identity (PI) refers to how someone represents their profession’s characteristics, values, and attributes through thoughts, actions, and behaviors (Cruess et al., 2014; Gee, 2003; Luehmann, 2011). It is highly related to professionalism, which influences and shapes one’s identity in a professional context (Forouzadeh et al., 2018). The formation of PI involves developing one’s understanding of their professional roles, responsibilities, and expectations that are socio-culturally dependent (Siebert & Siebert, 2007). Therefore, the process of forming one’s PI also involves developing one’s cultural identity (Forouzadeh et al., 2018).
Studies on PI formation in medical education tend to focus on educational strategies that support PI formation during medical training (Adema et al., 2019; Ahmad et al., 2018; Cruess et al., 2015; Foster & Roberts, 2016). These studies provide insights on how to support PI formation without really addressing what needs to be taught to support medical students’ PI formation. Several theories on identity and PI formation suggest that one’s identity is formed through dialectical conversations that facilitate the acceptance, rejection, or modification of the profession’s characteristics and/or attributes into one’s core identity (Cruess et al., 2015; Gee, 2003; Siebert & Siebert, 2007; Stets & Burke, 2000). These characteristics and/or attributes are usually context-dependent (Cruess et al., 2014). Thus, defining and understanding what it means to be a professional physician in a certain socio-cultural context is as important as finding out how best to facilitate its formation in an educational setting (Wacquant, 2013).
Altruism and humanism are the two most cited values expected from a physician, along with integrity and accountability, honesty, and morality (Cruess et al., 2014; Edgar et al., 2020; Hall, 2021). Additionally, care providers, researchers, and teachers are some professional roles of physicians often mentioned in the literature (Ahmad et al., 2018; Branch & Frankel, 2016; Carlberg-Racich et al., 2018; Hatem & Halpin, 2019). Nevertheless, there might be other roles and characteristics that have yet to be fully elucidated, especially considering that the current literature on PI formation is mainly dominated by the Western representation of the medical profession.
This study aimed to describe the characteristics and/or attributes of ideal (professional) physicians in Indonesia as defined by undergraduate medical students. Undergraduate medical students are unique as they have limited opportunities to interact with real patients in a real workplace. Through this study, we hope to gain new insights from undergraduate medical students on what it means to be a professional physician.
II. METHODS
This was a qualitative phenomenology research using case studies design at a private Catholic medical school in Jakarta, Indonesia. Participants were recruited using a purposive sampling method. Transitional phases in one’s life are often associated with identity renegotiation as they are exposed to changes in their roles, responsibilities, and expectations (Kay et al., 2019). Therefore, we sought to explore how Indonesian undergraduate medical students defined their professional identity at the beginning (first-year) and end (fourth-year) of their preclinical years. Ethical clearance was obtained from the school’s Research Ethics Committee prior to the study.
We set a quota of 5 participants for each study year (with a total of 10 study participants) to account for any possible socioeconomic status, ethnicity, religion, and gender variations. We recruited five first-year and five fourth-year preclinical students at the beginning of the study; however, two of the fourth-year participants dropped out during data collection; hence, only eight case studies constructed to depict the characteristics and/or attributes of an ideal Indonesian physician.
Each case study participant was interviewed twice using semi-structured interviews. The first interview was conducted at the beginning of school semester (August 2021) and the follow up interview was conducted one month after. The purpose of the first interview was to determined participants’ current understanding and views of what it meant to be a physician, while the second interview aimed to determine if there were any changes in their understanding or views and what precipitated the changes. Interview questions include: What kind of physician do you aspire to be? Was there one or more specific moment that prompted you to become a physician (if so, please describe it)? What characteristics and/or attributes should an ideal physician possess? Please explain. At the follow-up interviews, participants were asked to re-describe the characteristics and/or attributes of physicians that they aspired to be and what prompted the changes. Furthermore, participants were also asked to describe any specific learning moments that might influence their understanding of what it means to be a professional physician. Because of the COVID-19 physical distancing policy during the data collection phase, all data were obtained virtually or through electronic exchange via secured online platforms. All interviews were transcribed verbatim and analysed in vivo using abductive thematic analysis with Atlas.Ti 8
In addition to from the interviews, we also conducted several classroom observations. We observed the first- and fourth-year’s large classroom lecture, problem-based learning, and skills laboratory session once, focusing on the teacher-student interactions and made note on how, if any, the faculty member facilitated students’ PI formation in the classroom. We also interviewed several faculty members who interacted with the participants in teaching capacity during the data collection phase. Faculty members were asked to describe what kind of physicians they wanted their students to be based on institutional values and their own beliefs about what constitutes an ideal physician. They were also asked to elaborate on their efforts to facilitate those characteristics and/or attributes in the formal and informal curriculum.
Data obtained from classroom observation and faculty interviews were used to triangulate the findings from the participants’ interviews. Permission was obtained from all related parties to record and use the interviews and classroom interactions in the data analysis. Individual case study reports were generated by combining the data obtained from interviews and field notes. These case study reports were then cross-analysed to find commonalities across the case studies to define the characteristics and/or attributes of an ideal physician that the participants aspired to be at their current stage of education.
III. RESULTS
The majority of participants were either Chinese or of Chinese descent. Five participants were Christian Protestants, one was a Buddhist, and two refused to disclose their ethnicity and religion. Note that the names used in these case studies are pseudonyms.
A. Case Study #1: Celine (First-year Student)
Celine, a female of Chinese-Betawi descent from West Java, was raised in a devout Christian-Protestant family. Being a physician was not her childhood aspiration. Initially, she thought physicians tended to be “rude, bossy, had too much pride, unwilling to listen to suggestions” (Celine, Interview 1, Line 42-43), which contradicted her personal values to being humble and helping others as a form of service and manifestation of her faith. Nevertheless, she developed a new appreciation toward physicians when she found out that there were physicians who gave back to the surrounding community by providing free healthcare (see Appendix No. 1).
Humility, and self-reflectiveness—which Celine called “openness to criticism” (Celine, Interview 1, Line 39-44) were the characteristics she deemed important as a physician. She believed that a physician should engage in social actions and put the patient first. Furthermore, a physician should consider the patient’s personal circumstances while providing individualised healthcare based on the patient’s needs. A good physician should also believe that their most important role is to provide credible health information and educate the community to improve their health and well-being. Good communication skills, including active listening, empathy, building trust, and the ability to break bad news, were essential in supporting this role (see Appendix No. 2).
B. Case Study #2: Dimitri (First-year Student)
Dimitri, a Christian-Protestant female of Chinese descent, was quite familiar with medicine and the medical profession as she was surrounded by people who either worked as or studied to become a physician. Additionally, she helped caring for her visually impaired sibling since she was young, which gave her opportunities to interact with various care providers as she accompanied her sibling for treatment. Being a physician naturally became her aspiration since childhood. Dimitri was appointed as a ‘Dokter Kecil’ (or, ‘little doctor’) in elementary school, assigned to provide first aid treatment to fellow students and promote health efforts conducted by the school. Before entering medical school, Dimitri’s grandfather fell critically ill; therefore, she helped her family to care for him in the hospital. There, she met a cardiologist whom she respected. She recalled that she appreciated the way this cardiologist relayed which information could be shared with her grandfather to keep his spirit up and which information should be disclosed to her family to prepare for the worst possible outcome. She mentioned that her grandfather looked “calm and comfortable” in his last days, which helped the family to accept his departure peacefully (Dimitri, Interview 1, Line 77-80).
Dimitri highlighted a physician’s ability to handle the distribution of information as an important part of her ideal physician identity (See Appendix No. 3). She believed that it was acceptable for a physician to keep certain information from the patient if that information could add unnecessary stress or cause them to stop following the treatment (Dimitri, Interview 1, Line 90-98). Regardless, the physician should disclose all information to the patient’s relatives as the patient’s decision-maker. Dimitri aspired to be a caring and compassionate physician with good communication skills who can be held accountable for her actions. Aside from being a care provider, Dimitri believed that a physician should take on a role as ‘Pengayom’ (protector). She believed that patients were in vulnerable positions due to their health issues, and therefore the physician was responsible for protecting them like a parent would when their child was sick. Implied in the Pengayom role was the leader whose responsibility was to make the best decision for the patient’s health and well-being (See Appendix No. 4).
C. Case Study #3: Faustine (First-year Student)
Faustine, a Christian-Protestant female of Chinese descent, was born and raised in a remote area in Riau province, in the southern part of Sumatra Island. Her interest in biology and life sciences prompted her to browse online videos related to healthcare since she was young. She tended to feel sad if the people closest to her were suffering and she could not do anything to help. She made up her mind to study medicine when one of her high school friends was forced to seek treatment abroad because of limited healthcare access in her region. Prior to this, her father was misdiagnosed with a malignant tumor, which caused tremendous distress for her family. These incidents drove her to be a physician who could provide good quality care, especially to those closest to her (See Appendix No. 5).
Faustine aspired to be an empathetic physician, taking patients’ mental or psychological state into consideration when planning for their treatment. She did not want to be a physician who focused on financial gain at the cost of the patient’s wellbeing. Being aware of her limitations in providing care and continuously updating her knowledge and skills were characteristics she hoped to develop once she became a physician (Faustine, Interview 1, Line 103-115). Faustine also mentioned that a physician was responsible for being a reliable source of information and improving community wellbeing through education (See Appendix No. 6).
D. Case Study #4: Jasmine (First-year Student)
Jasmine originated from Rembang, a small regency on the northeast coast of Central Java. Being a physician had always been her childhood aspiration because she loved helping people and interacting with others. Jasmine tended to her grandmother’s health needs during middle school. This event confirmed her passion and desire to serve others. Putting others’ needs above herself was a value instilled by her father since she was young. She wanted to be a physician who focused on social services, and was driven to help others sincerely without expecting anything in return.
As Jasmine mentioned, an ideal physician should be honest, disciplined, possess high ‘Jiwa Sosial’ (an attitude that shows concern to perform actions that are beneficial for humanity and social community), and always put the patient’s needs first (Jasmine, Interview 1, Line 50-53). Jasmine viewed her work as an extension of her faith, and she wanted to reflect Christian values, particularly the value of servitude, in her professional life (See Appendix No. 7-8).
E. Case Study #5: Rose (First-year Student)
Rose, a Christian-Protestant female of Chinese descent, was born and raised in Ambon city, Maluku province, Eastern Indonesia. She was the oldest child in her family. Rose became interested in medicine when her mother was diagnosed with a serious illness and could not receive appropriate treatment. She disclosed that her mother ignored the early signs and symptoms of her illness until her condition became so severe that she could not be treated fully. From this experience, Rose was motivated to become a physician so that she could take better care of her family (See Appendix No. 9).
Growing up, Rose heard several stories in which a patient did not receive appropriate healthcare due to their socioeconomic status. She aspired to be a competent and non-discriminative physician. Putting the patient’s needs first, being responsible, helpful, patient, disciplined, and continuously improving her knowledge and skills were the characteristics that she hoped to develop by the time she became a physician. Aside from being a care provider, Rose believed that a physician was responsible for improving the wellbeing of the community through education (See Appendix No. 10).
F. Case Study #6: *Anton (Fourth-year Student)
*Anton, a Christian-Protestant male of Chinese-descent, had an interest in biology since childhood. He was dissatisfied with Indonesian healthcare services, particularly with the healthcare workers’ communication skills when treating his father. This incident occurred when he was in middle school. *Anton observed a power imbalance between the patients and physicians, where the healthcare providers held more power over their patients. As a patient, he felt disadvantaged because he could not demand a better quality of care nor asked for a lower cost of the care he received (See Appendix No. 11). He described the two roles of physicians: as a healthcare provider and educator. As a healthcare provider, one should be able to help patients understand what is best for them while still respecting their autonomy. As educators, physicians have the responsibility to provide valid evidence-based information for patients.
For *Anton, an ideal physician’s fundamental values and skills included providing good quality care that kept the patients’ best interest, respecting patients’ autonomy, doing no harm, having all necessary medical competencies as listed in the Competence Standards of Indonesian Physician, the drive to learn for a lifetime, patience, humility, competence, and the ability to engage in interprofessional collaboration (See Appendix No. 12).
G. Case Study #7: *R (Fourth-year Student)
*R is a Chinese Buddhist female from Sintang, central Indonesia. *R wanted to pursue medicine because physician was portrayed as a noble profession in Indonesia and as a ‘role model’ in her family. She wanted to serve marginalised areas in East Indonesia after hearing about the poor health situation in those areas from several alumni and fellow students who served there in various capacities. This experience, along with her formal learning experiences, shaped her ideal physician image, which included being detail-oriented, confident, honest, thorough, and caring. She believed that physicians should be able to fulfill the roles and responsibilities of a healthcare provider, which required good proficiency in medical competencies, based on several fundamental values such as honesty, willingness to serve marginalised and under-served communities, and being sensitive to patients’ needs (See Appendix No. 13).
H. Case Study #8: *Anastasia (Fourth-year Student)
*Anastasia, who identified as a female, wanted to be a physician since elementary school. She did not have a specific motivation to enter a medical school when she first started. Nevertheless, there were several past experiences that she claimed to have influenced her image of ideal physicians. She mentioned feeling comfortable being examined by her pediatrician during her childhood. This made her consider the pediatrician as her role model. She also followed several healthcare professionals’ whom she admired on their social media accounts. She claimed that these figures influenced her to be selfless and put the patients’ needs above her own. She acknowledged the importance of entrepreneurial skills in aiding her goal of being selfless yet still able to make a living for herself. Her ideal physician image is someone who has good communication skills, clinical competence, and willingness to learn continuously. She identified healthcare provider as the essential role of a physician, who was responsible for providing physical and mental healthcare, as well as participating in preventive and promotive healthcare. She particularly considered female medical teachers at her school as her role models because she admired the way these figures divide their time and energy to work professionally–both as healthcare practitioners and teachers–and keeping up with their personal and family time. She aspired to be someone who could divide her focus like these figures once she graduated (See Appendix No. 14).
IV. CROSS-CASE ANALYSIS AND DISCUSSION
Cross-case analysis revealed four major attributes of physician identity as defined by the first- and fourth-year participants (indicated by * behind their pseudonyms), including characteristics, values, roles and responsibilities, and skills. First-year participants drew their ideal image of a physician based on their interactions with one or more healthcare provider whom they met in their earlier lives. These interactions left a significant impression that further strengthened their motivation to study medicine and influenced the kind of values or other things that they held important and were willing to stand for as future physicians.
First-year participants mainly mentioned humanistic and altruistic values as the characteristics and/or attributes that define their professional identity. Honesty, humbleness/humility, accountability, patience, jiwa social, prioritising patients’ needs, empathy, care, and compassion are some of the characteristics mentioned by the first-year participants as characteristics of an ideal physician. These characteristics correspond to society’s expectations of professional physicians to put patient’s interest above all else, which is then further translated into medical professionalism and professional responsibilities (Alrumayyan et al., 2017; Elaine Saraiva Feitosa et al., 2019).
Different from their counterparts, fourth-year participants focused on clinical excellence and competence when citing the ideal characteristics and/or attributes of an ideal physician based on the national Competence Standards for Indonesian Physician. This indicates that fourth-year participants were aware of the standards as well as the ethical principles and physician’s code of conduct that were being enforced in Indonesia (See Appendix 15-16).
The way fourth-year participants described their physician identity aligned with the image of a professional physician painted by the school’s teaching faculty. According to interviews with several key faculty members, meeting the minimal standard of competence, being aware of one’s limitations, practicing evidence-based medicine, honesty, and discipline were some of the fundamental physician attributes/values/characteristics that they tried to instill in their students during education. These institutional values were most notably found in the way first-year participants described their physician identity during their second interview (See Appendix No. 17-18).
The attributes of Indonesian physicians mentioned by all case studies participants closely resemble China’s framework of professionalism, where they emphasise altruism, integrity and accountability, excellence, and religion/moral values (Al-Rumayyan et al., 2017). Possessing jiwa sosial (inherent sense of social responsibility, empathy, and engagement) and being a pengayom (mentor/guardian/protector) are two unique attributes that represent the Indonesian ideal physician.
There were minimal overlaps between the first- and fourth-year participants’ ideal physician images. First-year participants placed humanism/altruism and social responsibility as the focal points of their physician identity, whereas fourth-year participants chose clinical excellence and competence to represent their physician identities. Social interactions play a major role in identity formation (Thomas et al., 2016). This may explain the shift in the first- and fourth-year participants’ definition of an ideal physician. First-year participants modeled their ideal physician identity after their memorable interactions with physicians who provided care for them or their family members. Positive past interactions with healthcare providers shaped the characteristics and/or attributes that participants aspired to be, whereas negative past interactions motivated them to develop the opposite of observed characteristics and/or attributes. Fourth-year participants also integrated the characteristics and/or attributes they identified from the formal and informal learning experiences with their evolving understanding of an ideal physician. In these case studies, fourth-year participants cited clinical competencies and excellence, as well as discipline and honesty—which were emphasised by the teachers during their undergraduate medical training—as the major characteristics and/or attributes that defined their physician identity.

Figure 1. Shift in First-Year and Fourth-Year Participants’ Definition of Physician Identity
The first year of the medical curriculum was indicated to be an important transition point that shaped all participants’ PI. In particular, all participants mentioned the school orientation as one of the learning moments that triggered their identity negotiation. Participants were introduced to the school’s expectations of them as medical students and future physicians. These expectations include the characteristics of self-regulated and life-long learners and those of professional physicians (See Appendix No. 19-20). For example, Jasmine “learned to be disciplined and responsible and she believed that the school orientation “helped shape [her] basic personality as a physician [who needs] to be disciplined and responsible [as well as] trustworthy.” (Jasmine, Interview 1, Line 115-118).
The shifts in participants’ physician identity definition indicated that participants engaged in a dialectical conversation that stimulated them to merge their core or personal identity with the institution’s perception of ideal physicians (“virtual/ideal identity) as interpreted in their curriculum, which was a part of one’s identity negotiation process (Gee, 2003). In the cross-case analysis, we found that participants’ reactions toward the values, characteristics, and attributes instilled by the faculty varied. For example, some participants saw the importance of being on time (‘discipline’) as well as being academically honest by avoiding plagiarism and cheating during exams (‘honesty’), which they accepted as a part of their physician identity. On the other hand, other participants struggled to understand the relevance of being on time and academically honest with their future physician roles or aspirations. This became a major challenge for these participants in incorporating those values into their physician identity. Nevertheless, no participants rejected any characteristics/attributes instilled by the institution even if those characteristics/attributes were distinctly different from their personal beliefs system (See Appendix No. 21-23).
Any new or contradictory characteristics or attributes to one’s core identity pose a professional dilemma that triggers an identity negotiation (Spencer et al., 1997). During this identity negotiation process, the study participants tried to merge their core identity, which was represented by their definition of the ideal physician that they aspired to be, either by accepting, rejecting, or integrating the new characteristics/attributes into their core identity (Cruess et al., 2015).
The acceptance of new characteristics/attributes into one’s physician identity will be easier if it is consistent with one’s core identity; however, it is still possible to instill characteristics/attributes that contradict one’s core identity if they are provided with the long-term benefit of accepting those characteristics/attributes (Guillemot et al., 2022). This underlined the importance of providing students with the relevancy of developing certain characteristics/attributes desired from a professional physician during their educational phase to support their PIF.
V. CONCLUSION
This case study found that first-year participants prioritised humanistic characteristics as the foreground of their professional identity, and medical professionalism as their background. Meanwhile, fourth-year participants developed a projected identity that embodied the general values of the medical profession and those promoted by their institution. The perceived image of ideal physicians as constructed by the Indonesian society’s ideal image of a physician, prior interactions with Indonesian physicians that influenced their decisions to study medicine, and interactions with the medical teachers during formal and informal learning activities influenced the way participants defined their professional identity.
Notes on Contributors
Natalia Puspadewi contributed to the work’s conception and design by developing the study proposal, protocols and instruments, data collection, analysis, and interpretation. Further, Natalia also drafted and revised the manuscript and ensured that all aspects of the work were accountable, and followed all procedures to ensure data security and anonymity.
Ethical Approval
This study was a part of a doctoral dissertation. The University of Rochester acted as the author’s host institution, and Atma Jaya Catholic University of Indonesia, School of Medicine and Health Sciences, was the research site. Ethical approval was provided by the University of Rochester RSRB (a letter of exempt determination was obtained on July 8th, 2021 for Study ID 00006273) and the Atma Jaya Catholic University of Indonesia, School of Medicine and Health Sciences Ethics Committee (ethical clearance certificate No. 08/07/KEP-FKUAJ/2021).
Data Availability
The data supporting the findings of this study are openly available in the Figshare repository
https://doi.org/10.6084/m9.figshare.23684235. The data were not translated into English to preserve the Indonesian sociocultural nuances captured in the interviews. All data were coded and analysed in vivo in Bahasa Indonesia before being translated into English for presentation in this manuscript.
Acknowledgement
We would like to express our gratitude to those who have contributed to this study and article development: Dr. Rafaella Borasi as the head of the dissertation committee and advisor, Dr. Sarah Peyre as dissertation committee member, and Gracia Amanta, MD and Cristopher David, MD who helped with manuscript organisation and layouts.
Funding
This study was funded by the Atma Jaya Catholic University of Indonesia and American Indonesian Cultural and Education Foundation.
Declaration of Interest
The author has no conflicts of interest to disclose.
References
Adema, M., Dolmans, D., Raat, J. a. N., Scheele, F., Jaarsma, D., & Helmich, E. (2019). Social interactions of clerks: The role of engagement, imagination, and alignment as sources for professional identity formation. Academic Medicine, 94(10), 1567. https://doi.org/10.1097/ACM.0000000000002781
Ahmad, A., Yusoff, M. S. B., Mohammad, W. M. Z. W., & Nor, M. Z. M. (2018). Nurturing professional identity through a community based education program: Medical students experience. Journal of Taibah University Medical Sciences, 13(2), 113–122. https://doi.org/10.1016/j.jtumed.2017.12.001
Alrumayyan, A., Van Mook, W. N. K. A., Magzoub, M., Al-Eraky, M. M., Ferwana, M., Khan, M. A., & Dolmans, D. (2017). Medical professionalism frameworks across non-Western cultures: A narrative overview. Medical Teacher, 39(sup1), S8–S14. https://doi.org/10.1080/0142159X.2016.1254740
Branch, W. T., & Frankel, R. M. (2016). Not all stories of professional identity formation are equal: An analysis of formation narratives of highly humanistic physicians. Patient Education and Counseling, 99(8), 1394–1399. https://doi.org/10.1016/j.pec.2016 .03.018
Carlberg-Racich, S., Wagner, C. M. J., Alabduljabbar, S. A., Rivero, R., Hasnain, M., Sherer, R., & Linsk, N. L. (2018). Professional identity formation in HIV care: Development of clinician scholars in a longitudinal, mentored training program. Journal of Continuing Education in the Health Professions, 38(3), 158–164. https://doi.org/10.1097/CEH.0000000000000214
Cruess, R. L., Cruess, S. R., Boudreau, J. D., Snell, L., & Steinert, Y. (2014). Reframing medical education to support professional identity formation. Academic Medicine, 89(11), 1446-1451. https://doi.org/10.1097/ACM.0000000000000427
Cruess, R. L., Cruess, S. R., Boudreau, J. D., Snell, L., & Steinert, Y. (2015). A schematic representation of the professional identity formation and socialisation of medical students and residents: A guide for medical educators. Academic Medicine, 90(6), 718-725. https://doi.org/10.1097/ACM.0000000000000700
Edgar, L., McLean, S., Hogan, S. O., Hamstra, S., & Holmboe, E. S. (2020). The milestones guidebook. Accreditation Council for Graduate Medical Education (ACGME).
Feitosa, E. S., Brilhante, A. V. M., De Melo Cunha, S., Sá, R. B., Nunes, R. R., Carneiro, M. A., De Sousa Araújo Santos, Z. M., & Catrib, A. M. F. (2019). Professionalism in the training of medical specialists: An integrative literature review. Revista Brasileira De Educação Médica, 43(1), 692–699. https://doi.org/10.1590/1981-5271v43suplemento1-20190143.ING
Forouzadeh, M., Kiani, M., & Bazmi, S. (2018). Professionalism and its role in the formation of medical professional identity. Medical Journal of the Islamic Republic of Iran, 32(1), 765–768. https://doi.org/10.14196/mjiri.32.130
Foster, K., & Roberts, C. (2016). The heroic and the villainous: A qualitative study characterising the role models that shaped senior doctors’ professional identity. BMC Medical Education, 16(1), 206. https://doi.org/10.1186/s12909-016-0731-0
Gee, J. P. (2003). What video games have to teach us about learning and literacy. Computers in Entertainment, 1(1), 20. https://doi.org/10.1145/950566.950595
Goldie, J. (2012). The formation of professional identity in medical students: Considerations for educators. Medical Teacher, 34(9), e641–e648. https://doi.org/10.3109/0142159X.2012.687476
Guillemot, S., Dyen, M., & Tamaro, A. (2022). Vital service captivity: Coping strategies and identity negotiation. Journal of Service Research, 25(1), 66–85. https://doi.org/10.1177/10946705 211044838
Hall, C. (2021). Professional identity in nursing. In R. Ellis & E. Hogard (Eds.), Professional identity in the caring professions: Meaning, measurement and mastery. Routledge. https://www.taylorfrancis.com/books/9781003025610
Hatem, D. S., & Halpin, T. (2019). Becoming doctors: Examining student narratives to understand the process of professional identity formation within a learning community. Journal of Medical Education and Curricular Development, 6. https://doi.org/10.1177/2382120519834546
Kay, D., Berry, A., & Coles, N. A. (2019). What experiences in medical school trigger professional identity development? Teaching and Learning in Medicine, 31(1), 17–25. https://doi.org/10.1080/10401334.2018.1444487
Luehmann, A. (2011). The lens through which we looked. In A. Luehmann & R. Borasi (Eds.), Blogging as change: Transforming science & math education through new media literacies. Peter Lang Inc.
Siebert, D. C., & Siebert, C. F. (2007). Help seeking among helping professionals: A role identity perspective. American Journal of Orthopsychiatry, 77(1), 49–55. https://doi.org/10.1037/0002-9432 .77.1.49
Spencer, M. B., Dupree, D., & Hartmann, T. (1997). A Phenomenological Variant of Ecological Systems Theory (PVEST): A self-organisation perspective in context. Development and Psychopathology, 9(4), 817–833. https://doi.org/10.1017/S0954579497001454
Stets, J. E., & Burke, P. J. (2000). Identity theory and social identity theory. Social Psychology Quarterly, 63(3), 224–237. https://doi.org/10.2307/2695870
Thomas, E. F., McGarty, C., & Mavor, K. (2016). Group interaction as the crucible of social identity formation: A glimpse at the foundations of social identities for collective action. Group Processes & Intergroup Relations, 19(2), 137–151. https://doi.org/10.1177/1368430215612217
Wacquant, L. (2013). Homines in extremis: What fighting scholars teach us about habitus. Body & Society, 20(2), 3-17. https://doi.org/10.1177/1357034X13501348
Wald, H. S. (2015). Professional identity (trans)formation in medical education: Reflection, relationship, resilience. Academic Medicine, 90(6), 701. https://doi.org/10.1097/ACM.00000000000 00731
*Natalia Puspadewi
School of Medicine and Health Sciences,
Atma Jaya Catholic University of Indonesia,
Jl. Pluit Selatan Raya No. 19, Penjaringan,
Jakarta Utara, 14440
Email: natalia.puspadewi@atmajaya.ac.id
Submitted: 1 May 2023
Accepted: 21 December 2023
Published online: 2 April, TAPS 2024, 9(2), 5-17
https://doi.org/10.29060/TAPS.2024-9-2/OA3053
WCD Karunaratne1, Madawa Chandratilake2, Kosala Marambe3
1Centre for Medical Education, School of Medicine, University of Dundee, United Kingdom; 2Department of Medical Education, Faculty of Medicine, University of Kelaniya, Sri Lanka; 3Department of Medical Education, University of Peradeniya, Sri Lanka
Abstract
Introduction: The literature confirms the challenges of learning clinical reasoning experienced by junior doctors during their transition into the workplace. This study was conducted to explore junior doctors’ experiences of clinical reasoning development and recognise the necessary adjustments required to improve the development of clinical reasoning skills.
Methods: A hermeneutic phenomenological study was conducted using multiple methods of data collection, including semi-structured and narrative interviews (n=18) and post-consultation discussions (n=48). All interviews and post-consultation discussions were analysed to generate themes and identify patterns and associations to explain the dataset.
Results: During the transition, junior doctors’ approach to clinical reasoning changed from a ‘disease-oriented’ to a ‘practice-oriented’ approach, giving rise to the ‘Practice-oriented clinical skills development framework’ helpful in developing clinical reasoning skills. The freedom to reason within a supportive work environment, the trainees’ emotional commitment to patient care, and their early integration into the healthcare team were identified as particularly supportive. The service-oriented nature of the internship, the interrupted supervisory relationships, and early exposure to acute care settings posed challenges for learning clinical reasoning. These findings highlighted the clinical teachers’ role, possible teaching strategies, and the specific changes required at the system level to develop clinical reasoning skills among junior doctors.
Conclusion: The ‘Practice-oriented clinical skills development framework’ is a valuable reference point for clinical teachers to facilitate the development of clinical reasoning skills among junior doctors. In addition, this research has provided insights into the responsibilities of clinical teachers, teaching strategies, and the system-related changes that may be necessary to facilitate this process.
Keywords: Clinical Reasoning, Medical Decision Making, Medical Graduates, Junior Doctor Transition, Hermeneutic Phenomenology, Qualitative Research
Practice Highlights
- A safe environment and early healthcare team integration facilitate learning clinical reasoning.
- Adopting a comprehensive approach to reasoning can overcome specialty-specific reasoning challenges.
- Trainees’ emotional commitment toward patients could help them learn clinical reasoning skills.
- Interrupted supervisory relationships and early acute care exposure can hamper learning reasoning.
- Ensuring junior doctor training is both service and learning oriented is of paramount importance.
I. INTRODUCTION
Clinical reasoning is composed of cognitive processes, metacognitive processors, and behaviour during the application of critical thinking to a clinical situation and is heavily influenced by numerous contextual factors related to the doctor, patient, and the clinical environment (Durning et al., 2011; Durning et al., 2013; Norman, 2005).
The clinical reasoning of learners evolves along the continuum of medical education with unique challenges associated with major transition phases, the progression from non-clinical to clinical stage, medical graduate to junior doctor, and specialist trainee to medical specialist (Teunissen & Westerman, 2011). Notably, the medical graduate to junior doctor transition presents more pronounced difficulties (Brennan et al., 2010), primarily due to changing roles and responsibilities towards patient care, limited experience in navigating clinical uncertainties, and the need to work within multi-professional teams with limited support. Consequently, these factors have contributed to a steep learning curve for developing clinical reasoning skills (Brennan et al., 2010; Lempp et al., 2005; Prince et al., 2004; Tallentire et al., 2017). The challenges in developing reasoning skills are associated with the reduced applicability of undergraduate training in clinical practice (Cave et al., 2009; Monrouxe et al., 2017), coordinating and organising clinical and administrative responsibilities (Cameron et al., 2014; Teunissen & Westerman, 2011), and dealing with diverse contextual factors in practice. These factors encompass navigating hierarchical relationships and meeting the expectations of seniors, difficulties in recognising disease severity, uncertainty regarding their role, and tension in interpersonal relationships with team members (Cameron et al., 2014; Tallentire et al., 2011, 2017). When these challenges are not resolved, they could boil down to deficits in clinical reasoning and diagnostic error leading to adverse patient outcomes (Graber et al., 2005; Huckman & Barro, 2005; Jen et al., 2009).
The challenging nature of the junior doctor transition is shared across many similar contexts globally (Prince et al., 2000; Teunissen & Westerman, 2011) calling for a coherent approach to facilitate learning clinical reasoning. Concerns around clinical reasoning deficits of doctors continue to soar even today in resourceful developed countries (Health Services Safety Investigation Body, 2022; Huckman & Barro, 2005; Jen et al., 2009), emphasising the need for faculty to take decisive actions to resolve it! Unless for the limited research on clinical reasoning outside the western region (Lee et al., 2021), the situation could have been the same elsewhere.
There is ample evidence of numerous factors that may improve the development of clinical reasoning skills. Accordingly, work experience (Ericsson, 2004; Norman, 2005; Norman et al., 2007), a strong foundation on basic biomedical concepts (Woods, 2007), reflective practice (Mamede et al., 2008, 2012), feedback (Hattie & Timperley, 2007), learning from others during practice, and conducive organisational context for learning (Goldacre et al., 2003; Hattie & Timperley, 2007; Lempp et al., 2005) are found to be central in learning clinical reasoning. This evidence, however, is not specific to junior doctors. The learning needs of junior doctors in transition may vary from other trainee doctors and other health professions staff. Therefore, it has become critical that the clinical reasoning experiences, challenges, and practices of junior doctors as a vulnerable group of trainees are understood well to be able to better support their development of clinical reasoning.
When exploring this period of transition, the five-stage model of adult skill acquisition from novice to expert (Dreyfus, 2004), can help understand how junior doctors progress in relation to these stages. The situated learning theory (S. J. Durning & Artino, 2011; Lave, 1991) can provide the basis for understanding the social nature of learning clinical reasoning. The influence of contextual factors on mediating internal motivation for learning clinical reasoning can be understood through the self-determination theory (Ryan & Deci, 2000; Taylor & Hamdy, 2013). Therefore, to gain a better understanding of the transition experiences from medical graduates to junior doctors, a longitudinal study was designed using the above theoretical models as the conceptual framework to explore the following research questions:
(1) How do junior doctors evaluate their learning experiences of clinical reasoning development?
(2) What adjustments in the application of different educational means into the learning environment are necessary to improve the development of clinical reasoning skills?
II. METHODS
A. Methodology
The methodological approach of hermeneutic phenomenology (Crotty, 1998; Laverty, 2003) was employed in this study (Kafle, 2011; Laverty, 2003). Such an approach to clinical reasoning was adopted by other researchers exploring clinical reasoning (Ajjawi & Higgs, 2007; Langridge et al., 2015; Robertson, 2012).
B. Study Setting
The study was conducted at the North Colombo Teaching Hospital, Ragama, Sri Lanka with ethical clearance (P/11/01/16) from the Faculty of Medicine, University of Kelaniya.
In Sri Lanka, medical undergraduate training is a five-year programme with two pre-clinical and three clinical years. After graduation, medical graduates follow a 12-month internship where they work under a consultant for six months each in any of the two main clinical specialities, namely, Medicine, Surgery, Paediatrics, and Gynaecology & Obstetrics before obtaining full registration as a medical doctor.
C. Study Design and Sampling
The study participants were junior doctors during the 12 months of internship following graduation. Maximum variation sampling (Cohen et al., 2017), which enabled purposefully selecting the widest range of variation on dimensions of interest relevant to learning and practicing clinical reasoning was employed. The concept of ‘information power’ which sought not theoretical saturation but sufficient information to address the research questions informed the sample size (Malterud et al., 2016; Varpio et al., 2017). Hence, junior doctors working in the four main clinical specialties, in both university clinical wards staffed by university clinical academics and other clinical wards composed of medical consultants under the Ministry of Health and according to gender were enrolled in the study following informed consent.
Accordingly, eighteen junior doctors (n=18, males=8, females=10) from the four main clinical specialities (Medicine-4, Surgery-5, Paediatrics-4, Obstetrics and Gynaecology-5) were enrolled in the first stage of the study. The second stage of the study imposed heavy demands on the study participants because it involved recording multiple doctor-patient encounters and subsequent discussions based on stimulated recall. Therefore, out of the initially recruited participants, only the well-articulated consenting participants (n=8), who could proficiently express their thoughts and reasoning to obtain a good insight into the nature of practicing clinical reasoning were enrolled in this stage.
D. Data Collection
The data collection proceeded in two stages.
During the first stage, a combination of individual semi-structured interviews with narrative interviews were conducted. Semi-structured interviews allowed probing where necessary (Cohen et al., 2017), while the narratives allowed participants to tell their stories of clinical reasoning (Muylaert et al., 2014). Each lasted for 45-50 minutes.
The second stage included audio-recording the patient consultations of the selected participants on predefined dates during the first and second six months of their internship. The consultations were replayed, and post-consultation discussions were conducted soon afterward by employing a stimulated recall method, to account for a total of 48 post-consultation discussions. As clinical reasoning is a concept revealed only in action (Charlin et al., 2000), employing such an approach was considered essential during this study.
E. Data Analysis
All interviews and discussions were transcribed verbatim. The data analysis followed phenomenological and hermeneutic strategies, which required a thorough description of lived experiences (Ajjawi & Higgs, 2007) and employing a hermeneutic circle for data interpretation by moving back and forth between the parts and the whole of the experience to reach a deeper understanding of the experience (Laverty, 2003).
Thematic data analysis (Braun & Clarke, 2012) was conducted to generate themes explaining the data set as a whole.
The principal researcher developed two thematic frameworks for the two stages of the study. The two supervisors of the project re-coded selected transcripts from each stage. These independently derived frameworks were discussed, themes refined, and new themes identified until an agreement was reached. The finalised thematic framework was employed to code all the transcripts using the Atlas.ti qualitative data analysis tool.
III. RESULTS
A total of 18 individual interviews and 48 post-consultation discussions were analysed giving rise to seven themes. During analysis, it was noted that the factors that inform the development of clinical reasoning could be condensed together as a model. This is presented later in the text.
Each theme is elaborated below with quotations. When more than one quotation is required to describe a theme, these are presented within a table. Additional supportive quotations are openly available in Figshare at https://doi.org/10.6084/m9.figshare.23536548.v2 (Karunaratne et al., 2023).
A. A Safe and Supportive Working Environment Empowers Junior Doctors to Develop Clinical Reasoning Skills
It was the collective view that a ‘safe’ work environment is characterised by easy access to more experienced doctors, and the presence of a safety net of seniors who review junior doctors’ work and understand their reasoning challenges. It provided junior doctors the opportunity and freedom to practice clinical reasoning independently, learn from errors, and arrive at their own reasoning decisions.
Such a conducive work environment also provided them with opportunities to emulate seniors and receive real-time feedback while actively participating in authentic tasks and applying knowledge and skills acquired during their undergraduate training.
“I’m working in a unit where each admission is clerked by the registrar. So, in that case, we are always in feedback…What I usually do is sometimes I clerk the patients first, and after that, I compare it with the registrar’s clerking. So, in that case, we can easily adapt their clerking.”
(MP3, Medicine, Male, Phase-1)
B. Learning to Reason with Clinical Problems is Situated and Facilitated by Work Experience
Work experience provided the opportunity to learn from repeated exposure to clinical presentations and their variations, learn from seniors, and lapses of reasoning. However, work experience alone is not solely sufficient, and it is the collective influence of many other factors that help learn clinical reasoning. These factors are captured by the model developed from this study.
With work experience, junior doctors’ approach to reasoning changed from a ‘disease-oriented approach’ developed through undergraduate education to a ‘practice-oriented approach’. In the practice-oriented approach, junior doctors actively analyse clinical problems instead of matching them with memorised configurations of disease presentations.
They also developed ‘instincts’ for swift decision-making, sharpened through experience in recognising contextual factors in patient presentations. This was especially valuable for identifying acute cases requiring urgent care. In addition, they recognised the impact of the previous disease burden in formulating differential diagnoses, leading to a broader approach in their clinical reasoning.
Table 1 illustrates participant quotations that shed light on the role of work experience in learning clinical reasoning skills.
|
“…This approach in the ward is always problem-based. We’re dealing with problems. We try to solve the problems. That approach as a student was trying to fit the history into one of the long cases we have studied…Now we are not worried about that broad category. We will instead deal with the different problems that they have.” (MP2, Medicine, Male, Phase-1) |
|
“I think it’s just being with the patients. You realise that … it’s not just what’s written in the book…I mean now, if you’re just walking past a patient, you realise that this patient is not well. Whereas initially, you would have to go through the ward round and… go through the records, and then only you’ll see it. I don’t know how you get that but…” (MP2, Medicine, Male, Phase-1) |
|
“…Once a child with hypovolemic shock came to the ward. I was in the ward alone. I was very afraid at that time as I was in my first week of internship. So, nothing was on my mind, and I called my senior and he asked me to give (fluid) boluses until he came…. (There was another emergency at the same time). An Angioedema child came to the ward. I thought of (laughing)… running away from the ward. Because it was the initial period, it was very difficult, and our clinical knowledge was also poor. But now, we can manage any emergencies until the senior comes.” (PP, Paediatrics, Female, Phase-1) |
|
(When enquired on the reasons for commencing consultations with comorbidities?) “… Even the presenting complaint may be related to past medical conditions as well…and even this patient has diabetes… so, they can present in various ways… As an intern, I developed that. As an undergraduate, we are asking for name, age, where are you from, and then go on to take the history first…” (MP4, Medicine, Female, Phase-2) |
Table 1. Quotes illuminating that learning clinical reasoning is situated and facilitated by work experience
C. Internal Motivation and the Ability to Reflect and Employ Self-directed Learning are Powerful Tools for Developing Clinical Reasoning Skills
Learning clinical reasoning necessitated junior doctors to be internally driven for learning. Such internal motivation made them willing to learn from any source and be self-directed in their own learning. These individuals progressed rapidly in learning to reason with clinical problems compared to others who were not internally motivated.
Maintenance of internal motivation throughout the internship necessitated external encouragement even for the motivated particularly from the senior staff. There was a similar effect when the work environment fostered a culture of learning with the inclusion and recognition of junior doctors as a group of learners.
Table 2 presents participant quotations that highlight the significance of internal motivation in developing clinical reasoning skills.
|
“(reasoning with a complicated presentation) …With this kind of patient, it’ll refresh our memory. Going through how to take the history, how to use the basics, and how you investigate and manage…It is not like people coming with gastritis, or headache. Those are just simple things. (MP3, Medicine, Male, Phase-2) |
|
“I think you don’t need people who are good at what they do, I mean, you need people who are competent, but er…, you need a pleasant environment. Even if, there are, like 50 patients, if the people you work with are good, you can go through it. But then, if someone is really unpleasant, then that day is ruined.” (MP1, Medicine, Female, Phase-1) |
Table 2. Quotes illuminating internal motivation, reflective practice, and being self-directed as central to learning clinical reasoning skills
D. Caring and Compassionate Attitudes towards Patients Facilitate Developing Clinical Reasoning Skills
The individual caring and compassionate attitudes towards patients and the positive role modeling of senior doctors motivated junior doctors to learn clinical reasoning. Work experience nurtured these attitudes irrespective of gender, reflecting the potential to learn them during practice. However, a heavy workload and orientation towards efficiency in practice hindered the development of such attitudes among junior doctors.
“We’ve realised that although we’re members of a team, even individually, we can always do something for the patients. So, we always try to do something at our level. But we’re always willing to take the feeling from everyone above us to help.”
(MP1, Medicine, Female, Phase-1)
E. Collaborating within a Healthcare Team and Engaging in Ward Activities and Procedures Help Expedite the Development of Clinical Reasoning Skills
Junior doctors learn mostly from registrars, who are the immediate seniors and near-peers. In addition, peers and other healthcare staff contribute to their learning by timely sharing of information and working as a team. Patients’ unique characteristics which demand variation in reasoning also provide learning opportunities.
“I think the main influence is probably the registrars. Because we’re mostly in contact with them…So, in a way through working with them, I think I have learned quite a lot. Different ones will teach you different skills. Some are good at acute medicine and how to do that, and some are very willing to teach us how to do a pleural tap… So, from different people, we have learned different things.”
(MP2, Medicine, Male, Phase-1)
F. The Increasing Recognition of Professional Responsibility and Accountability towards Patient Care Drives Learning Clinical Reasoning
This was a strong theme commonly experienced by all junior doctors. During this transition, junior doctors recognised the patient care responsibilities vested in them and experienced a change of role from an undergraduate to a medical doctor. This led them to internalise their role and work towards meeting these expectations, whilst learning from all opportunities.
“We realise that somehow, we’ve got to do something. It wasn’t like that as students. (Now, as doctors) If we can’t take an ABG (Arterial Blood Gas) once, we will try ten times and somehow take the ABG. We realise- we have that ownership, “This is my patient. I will do something for her.” So, I think that’s a good thing. We didn’t have that as students.”
(MP1, Medicine, Female, Phase-1)
Parallel to the change of role, they were accepted as members of a community of doctors actively involved in providing patient care, which gave them a sense of inclusion and prestige and they worked hard towards meeting the expectations, which in turn helped them learn clinical reasoning.
G. Diversity of Personal, Interpersonal, and Contextual Factors Impede the Development of Clinical Reasoning Skills
Several negative influences on learning clinical reasoning exist.
The personal factors that can diminish learning clinical reasoning are related to a lack of internal motivation to learn and limited use of reflective practice.
In addition, external factors such as lack of encouragement and limited recognition of their contribution as doctors further demotivate junior doctors. Settings supervised by several senior clinicians provide better learning opportunities, but they also expose them to experience individual variations of reasoning due to staff working patterns and hinder their ability to appreciate the continuity of care.
Moreover, as junior doctors, they handle a heavy workload and work under time constraints, which gives them limited opportunity to reflect and learn from experience. Junior doctors also experience the presence of a power gap between juniors and seniors within the healthcare team and maintenance of this hierarchy is a barrier to learning during practice.
Table 3 presents participant quotes highlighting the diversity of contextual factors that hinder learning clinical reasoning skills.
|
“…usually hiccups occur with failures of… all types of failures… I do not have much knowledge about those things. Actually, I got to know that hiccups occur due to organ failure also, after this patient… (laughs)” (no intentions to learn more expressed) (SP2, Medicine, Male, Phase-2) |
|
“…here I think, in our unit, because the consultant changes daily, I think that is a negative point. The fact that you don’t have that connection with one person, and the fact that there is no continuity in care…” (MP1, Medicine, Female, Phase-1) |
|
“…I mean, there are too many admissions some days and you’re just trying to get through from one patient to the next one. So, you don’t really have that much time to analyse the problem as such. I mean, when the ward is less heavy, I’m trying to figure out what’s wrong but some days it’s a little bit… like going through.” (MP2, Medicine, Male) |
Table 3. Quotes illuminating contextual factors that impede the development of clinical reasoning skills
In addition, the discussions with junior doctors revealed that their main goal during the internship was to arrive at a diagnosis and/or manage patients’ clinical problems. No learning-related goals were readily verbalised.
(When enquired about the goals of reasoning during the internship)
“That…..err…is… coming to a final diagnosis and starting the treatment…Basically, we are supposed to recognise life-threatening conditions and treat them.”
(MP3, Medicine, Male, Phase-2)
Similarly, the informal discussions with senior clinicians revealed their limited expectations of the contribution of the internship towards facilitating the development of clinical reasoning skills among juniors. This could be due to the service orientation of the internship leaving ‘learning to happen’ concurrently without being actively encouraged. This is not conducive to learning clinical reasoning.
H. The Construction of the ‘practice-oriented clinical reasoning skills development framework’
Embedded within the seven themes were a multitude of factors that could be clearly categorised as ‘Facilitators’, ‘Drivers’, ‘Sources’, and ‘Challenges’ of developing clinical reasoning skills. These factors helped junior doctors to migrate from a disease-oriented to a practice-oriented approach to clinical reasoning (Figure 1).
The categorisation was informed by how these factors influenced the development of clinical reasoning skills. ‘Facilitators’ actively support learning, while ‘drivers’ exert strong internal pressure to motivate learning clinical reasoning. A ‘source’ is an individual or an activity, that helps learn clinical reasoning through interacting with them. ‘Challenges’ are either internal or external to an individual and negatively influence the development of clinical reasoning skills.
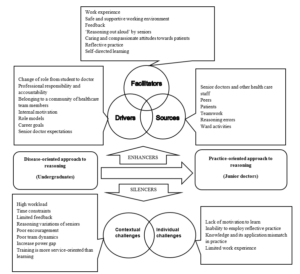
Figure 1. ‘Practice-oriented clinical reasoning skills development framework’ highlighting the factors that influence the development of clinical reasoning skills during the transition from medical graduates to junior doctors
IV. DISCUSSION
Aligned with existing literature (Brennan et al., 2010; Lempp et al., 2005; Prince et al., 2000; Teunissen & Westerman, 2011), this study identified a steep learning curve for junior doctors in developing clinical reasoning skills upon commencing the internship. A ‘disjunction’ (Koufidis et al., 2020) was evident between knowledge acquired during medical undergraduate education and the demands of effective reasoning in clinical practice (Cave et al., 2009; Monrouxe et al., 2017). The ‘practice-oriented clinical reasoning skills development framework’ derived from this study shed light on the factors serving as ‘enhancers’ and ‘silencers’ of learning clinical reasoning skills during this critical period. This classification helps consolidate existing knowledge specific to this period and offers insights for addressing disconnections and facilitating the development of clinical reasoning skills.
In this study, novice doctors initially faced clinical reasoning challenges due to limited contextual understanding and reliance on rule-based reasoning comparable to the Dreyfus model of adult skill acquisition (2004). With increased work experience, they were able to promptly recognise contextual features distinguishing acute from non-acute presentations requiring urgent care. Additionally, they acknowledged the significance of the patient’s past medical history in forming a broader approach to reasoning. Some even acquired instincts for prompt clinical decision-making, a form of non-analytic reasoning identified by clinical experts (Norman et al., 2007) and blending non-analytic reasoning with occasional rule-based confirmation (analytic reasoning). This dual-process approach (Croskerry, 2009; Eva, 2004; Pelaccia et al., 2011), incorporating both analytic and non-analytic reasoning is recognised to overcome challenges associated with each approach. Such development of clinical reasoning skills with work experience is reflective of the advancement of reasoning skills along the first four stages of the Dreyfus model, from novice to proficiency stages. This contrasts with the limited value placed on the internship for developing clinical reasoning skills among some clinical supervisors and needs addressing during staff development initiatives.
It was also noted that junior doctors revert to the novice stage using more analytical rule-based reasoning with uncommon presentations or at the start of a new rotation in another specialty (Groves, 2012). This highlights the complexity of developing clinical reasoning skills, varying with the nature of the presentation and the clinical specialty, requiring more support for its development. This aligns with the ‘context-specific nature’ of clinical reasoning (Eva et al., 1998), the variation of reasoning outcomes of an individual due to contextual factors unique to clinical situations. The study revealed a clear influence of clinical specialty on reasoning, confining the development of clinical reasoning to a few focused clinical problems common to a particular specialty. This limits the overall development of clinical reasoning and hinders the momentum of clinical reasoning development entering a new clinical specialty. Therefore, clinical teachers should promote a comprehensive approach, considering differential diagnoses beyond a single specialty. Given the need for promptly recognising contextual features of disease severity in acute care settings coupled with early internship challenges, delaying trainees’ placement in acute care settings until later in a clinical rotation is a reasonable approach, contrary to current clinical practice.
Work experience was central to developing clinical reasoning skills (Charlin et al., 2007; Schmidt & Rikers, 2007; Schmidt & Boshuizen, 1993), but benefiting from experience required junior doctors to be internally motivated. According to the self-determination theory, when an individual experiences a feeling of being able to do something successfully (competence), when their actions are controlled internally or self-determined (autonomy), and when there is a sense of safety, belonging, and supportive relationships (relatedness), it enhances the intrinsic motivation of an individual (Ryan & Deci, 2000) and this was clearly noted during this study. The ‘drivers’, ‘facilitators’, and ‘sources’ of learning clinical reasoning identified during this study enabled fulfilling these three basic psychological needs required to be motivated to learn clinical reasoning. Hence, the ‘practice-oriented clinical skills development framework’ could serve as a valuable reference for clinical teachers supporting junior doctors in developing clinical reasoning skills during their transition to the workplace.
Echoing the evidence in the field (Ajjawi & Higgs, 2008; Gruppetta & Mallia, 2020), junior doctors recognised the change in their role from student to medical doctor and subsequent absorption into the healthcare team which made them internalise their responsibility and accountability towards patient care. Their engagement in patient care gradually increased to finally becoming valued members of this community, collaborating with other like-minded colleagues to develop a more deliberate understanding of reasoning and methods of using it. This aligns with the principles of legitimate peripheral participation and community of practice of the Situated Learning Theory (O’Brien & Battista, 2020). The community of practice created a safe learning environment, motivating junior doctors to learn clinical reasoning actively. This emphasises the significance of early integration of junior doctors as valued members of the healthcare team. A team-oriented approach to patient care, acknowledging every team member’s contribution, proves more beneficial here than an individual-focused hierarchical approach.
The junior doctors of this study learned through their interactions with senior doctors, peers, and other healthcare staff, as well as by actively participating in ward activities, revealing learning as a dynamic social act. The opportunity to observe, listen to, and emulate senior colleagues as they engaged in clinical reasoning with authentic patient presentations, followed by the application of the newly acquired skills, significantly influenced the development of their clinical reasoning skills. This highlights the continued relevance of apprenticeship as a pedagogical tool today (Dornan, 2005), facilitating the ongoing development of clinical reasoning skills among junior doctors. It also provides a unique opportunity to witness firsthand the decision-making processes of junior doctors operating independently in clinical practice, aligning with the highest level of clinical skills assessment in Miller’s pyramid (Miller, 1990). This presents a potential opening for formative assessment of clinical reasoning, whether conducted formally or informally, as part of junior doctor training.
Junior doctors also constructed knowledge through interpersonal interactions in the workplace by engaging in an iterative process of learning, application, and consolidation of knowledge with each experience contributing to the refinement of their clinical reasoning skills. Learning from these experiences required them to reflect on these experiences and arrive at new understandings by integrating and building on previous knowledge. This is aligned with the principles of experiential learning theory (Morris, 2020; Yardley et al., 2012) and the constructivism learning theory (Olusegun, 2015). This highlights the importance of encouraging reflection by proactively including junior doctors in all pertinent patient-related discussions. Also, the value of implementing a reflective portfolio to acknowledge junior doctors’ learning needs at the outset of the internship, with formative assessments conducted midway and at its conclusion by clinical supervisors. This could also introduce a learning orientation to the already service-focused internship placement.
Junior doctors found collaborative learning, including referrals to other specialties and engaging in those discussions or working in partnerships with peers, beneficial for developing clinical reasoning (Laal & Laal, 2012; Tolsgaard et al., 2016). This highlights the value of involving junior doctors in collaborative work within or across disciplines. Simulation-based training (Khan et al., 2011) offers similar opportunities for collaborative learning within a safe environment, without compromising patient safety. Integrating simulation-based training for junior doctors immediately after graduation or before the internship can equip them with reasoning skills for authentic practice, addressing challenges during their transition to the workplace.
The caring and compassionate attitudes instilled in junior doctors by their seniors and further nurtured through close patient interactions, served as indirect motivators for learning clinical reasoning skills. This is an area not widely discussed in literature. While there is acknowledgment of the potential influence of clinicians’ emotions on clinical reasoning (Kozlowski et al., 2017), the specific impact of emotional closeness in patient care, and whether it aligns with the conventions of a more objective, rule-based healthcare delivery system, remains an area that merits more comprehensive investigation (Dreyfus, 2004). However, the study findings support that the more emotionally closer the junior doctors are to their patients, the more they are invested in learning clinical reasoning to ensure healthier outcomes for their patients. Clinical teachers could nurture such attitudes through role modeling as noted in this study.
The interrupted supervisory relationships due to work rotations of the senior staff challenged learning clinical reasoning. Such system-related factors deprived junior doctors of learning by emulating senior practice. It also hampered their ability to appreciate the continuity of patient care due to individual variations of reasoning among senior staff and prevented developing closer relationships with seniors, which could have been more emotionally satisfying (Ryan & Deci, 2000). This underlines the need to take necessary steps to prevent any adverse effects of staff working patterns on trainee doctors, while simultaneously ensuring extended periods of supervision within a consistent healthcare team.
The collective findings of this study not only confirm but also add valuable insights to the clinical reasoning pathway for teaching clinical reasoning skills (Linn et al., 2012). According to this framework, the teaching of clinical reasoning occurs in three stages through three consultations. Stage 1- Demonstration and deconstruction, Stage 2- Comprehension, and Stage 3- Performance. The transition in focus from the teacher’s approach to the student’s performance occurs in the last stage. In junior doctor training, this framework is ideally applied within a team context during daily clinical ward rounds focusing on selected patient presentations as afforded by the time constraints. The three stages of the framework can be combined, and the reasoning discussions can be brief and can take place within the ward round after the selected presentations with increasing junior doctors’ involvement as they gain experience. This could allow junior doctors to learn from verbalised reasoning from the team, reflect and actively contribute to the discussion, and feel valued as team members. They can apply newly acquired reasoning skills in subsequent patient consultations independently, in addition to the opportunity to demonstrate these during the ward rounds. Based on the study findings, additional considerations for analysing patient presentations could be proposed as enhancements to the clinical reasoning pathway (Linn et al., 2012). These aspects are detailed within the overall structure of this framework in Figure 2.
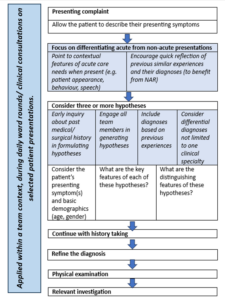
Figure 2. Proposed additions to the deconstructed consultation according to the clinical reasoning pathway (Linn et al., 2012) for teaching clinical reasoning to junior doctors as part of daily clinical ward rounds
Additions are presented in italics and highlighted. (NAR- non-analytic reasoning)
V. CONCLUSION
The ‘practice-oriented clinical skills development framework’ has brought together factors that act as ‘enhancers’ and ‘silencers’ of learning clinical reasoning specific to this period of transition from medical graduates to junior doctors. These findings offer practical insights that can prove invaluable for clinical educators in their teaching practices to facilitate the development of clinical reasoning skills.
This research also offers insights into the responsibilities of clinical teachers in supporting the development of clinical reasoning skills among junior doctors during their internship. It provides suggestions for teaching these skills in practice and highlights potential system-related changes needed to facilitate this process.
A. Limitations of the Study
The reader needs to determine the applicability of the findings to their context to overcome the limitations of qualitative research. To facilitate this process, the methodology and the data analysis are appropriately detailed.
The study focused on immediate medical graduates, and therefore, it did not delve into the clinical reasoning experiences of junior doctors at different levels of seniority and training, although this could have added to our understanding. This lack of comparative analysis is another limitation of this study.
Notes on Contributors
Dr WCD Karunaratne conceptualised the study, prepared the study proposal, conducted all interviews, analysed them and developed the manuscript for this submission.
Professor Madawa Chandratilake was a supervisor of this study and he contributed to the study design, guided initial interviews, and analysed selected transcripts to finalise the final coding framework for the study. He also reviewed and provided feedback on different versions of the manuscript.
Professor Kosala Marambe was also a supervisor of the study. She contributed to the study design and analysis of selected transcripts to finalise the final coding framework for the study and provided feedback on different versions of the manuscript.
Ethical Approval
Ethical clearance (P/11/01/16) was obtained from the Faculty of Medicine, University of Kelaniya, Sri Lanka.
Data Availability
Institutional ethical clearance was given to maintain the data in the secure storage of the principal investigator of the study. However, additional supportive quotations are deposited in the repository (Karunaratne et al., 2023) and are available from this URL – https://doi.org/10.6084/m9.figshare.23536548.v2.
Readers may contact the principal researcher for additional data and details if required.
Acknowledgement
We would like to acknowledge Dr Pavithra Godamunne (Faculty of Medicine, University of Kelaniya, Sri Lanka) who applied and secured funding for the project and Dr Paul Crampton (Hull York Medical School, UK) who reviewed the manuscript and provided constructive comments.
Funding
University of Kelaniya, Sri Lanka funded this research study (No. RP/03/04/17/01/16).
Declaration of Interest
The authors have no conflicts of interest to disclose.
References
Ajjawi, R., & Higgs, J. (2007). Using hermeneutic phenomenology to investigate how experienced practitioners learn to communicate clinical reasoning. The Qualitative Report, 12(4), 612–638. https://doi.org/10.46743/2160-3715/2007.1616
Ajjawi, R., & Higgs, J. (2008). Learning to reason: A journey of professional socialisation. Advances in Health Sciences Education, 13, 133–150. https://doi.org/10.1007/s10459-006-9032-4
Braun, V., & Clarke, V. (2012). Thematic Analysis. In APA Handbook of Research Methods in Psychology, 2, 57-71. https://doi.org/10.1037/13620-004
Brennan, N., Corrigan, O., Allard, J., Archer, J., Barnes, R., Bleakley, A., Collett, T., & De Bere, S. R. (2010). The transition from medical student to junior doctor: Today’s experiences of tomorrow’s doctors. Medical Education, 44(5), 449–458. https://doi.org/10.1111/j.1365-2923.2009.03604.x
Cameron, A., Millar, J., Szmidt, N., Hanlon, K., & Cleland, J. (2014). Can new doctors be prepared for practice? A review. Clinical Teacher, 11(3), 188–192. https://doi.org/10.1111/tct.12127
Cave, J., Woolf, K., Jones, A., & Dacre, J. (2009). Easing the transition from student to doctor: How can medical schools help prepare their graduates for starting work? Medical Teacher, 31(5), 403–408. https://doi.org/10.1080/01421590802348127
Charlin, B., Boshuizen, H. P. A., Custers, E. J., & Feltovich, P. J. (2007). Scripts and clinical reasoning. Medical Education, 41(12), 1178–1184. https://doi.org/10.1111/j.1365-2923.2007.02924.x
Charlin, B., Tardif, J., & Boshuizen, H. P. A. (2000). Scripts and medical diagnostic knowledge: Theory and applications for clinical reasoning instruction and research. Academic Medicine, 75(2), 182–190. https://doi.org/10.1097/00001888-200002000-00020
Cohen, L., Manion, L., & Morrison, K. (2017). Research methods in education (8th ed.). Routledge. https://doi.org/10.4324/9781315456539
Croskerry, P. (2009). A universal model of diagnostic reasoning. Academic Medicine, 84(8), 1022–1028. https://doi.org/10.1097/ACM.0b013e3181ace703
Crotty, M. (1998). Foundations of social research: Meaning and perspective in the research process (1st ed.). Routledge. https://doi.org/10.4324/9781003115700
Dornan, T. (2005). Osler, Flexner, apprenticeship and “the new medical education.” Journal of the Royal Society of Medicine, 98(3), 91–95. https://doi.org/10.1177/014107680509800302
Dreyfus, S. E. (2004). The five-stage model of adult skill acquisition. Bulletin of Science, Technology and Society, 24(3), 177–181. https://doi.org/10.1177/0270467604264992
Durning, S., Artino, A. R., Jr., Pangaro, L., van der Vleuten, C. P. M., & Schuwirth, L. (2011). Context and clinical reasoning: Understanding the perspective of the expert’s voice. Medical Education, 45(9), 927–938. https://doi.org/10.1111/j.1365-2923.2011.04053.x
Durning, S. J., & Artino, A. R. (2011). Situativity theory: A perspective on how participants and the environment can interact: AMEE guide no. 52. Medical Teacher, 33(3), 188-199. https://doi.org/10.3109/0142159x.2011.550965
Durning, S. J., Artino, A. R., Jr., Schuwirth, L., & van der Vleuten, C. (2013). Clarifying assumptions to enhance our understanding and assessment of clinical reasoning. Academic Medicine, 88(4), 442-448. https://doi.org/10.1097/acm.0b013e3182851b5b
Ericsson, K. A. (2004). Deliberate practice and the acquisition and maintenance of expert performance in medicine and related domains. Academic Medicine, 79(10 Suppl), S70–S81. https://doi.org/10.1097/00001888-200410001-00022
Eva, K., Neville, J., & Norman, G. (1998). Exploring the etiology of content specificity: Factors influencing analogic transfer and problem solving. Academic medicine, 73(10), S1-S5. https://doi.org/10.1097/00001888-199810000-00028
Eva, K. W. (2004). What every teacher needs to know about clinical reasoning. Medical Education, 39(1), 98–106. https://doi.org/10.1111/j.1365-2929.2004.01972.x
Goldacre, M. J., Davidson, J. M., & Lambert, T. W. (2003). Doctors’ views of their first year of medical work and postgraduate training in the UK: Questionnaire surveys. Medical Education, 37(9), 802–808. https://doi.org/10.1046/j.1365-2923.2003.01611.x
Graber, M. L., Franklin, N., & Gordon, R. (2005). Diagnostic error in internal medicine. Archives of Internal Medicine, 165(13), 1493–1499. https://doi.org/10.1001/archinte.165.13.1493
Groves, M. (2012). Understanding clinical reasoning: The next step in working out how it really works. Medical Education, 46(5), 444–446. https://doi.org/10.1111/j.1365-2923.2012.04244.x
Gruppetta, M., & Mallia, M. (2020). Clinical reasoning: Exploring its characteristics and enhancing its learning. British Journal of Hospital Medicine, 81(10), 1–9. https://doi.org/10.12968/hmed.2020.0227
Hattie, J., & Timperley, H. (2007). The power of feedback. Review of Educational Research, 77(1), 81–112. https://doi.org/10.3102/003465430298487
Health Services Safety Investigation Body. (2022). Investigation report: Clinical decision making- diagnosis and treatment of pulmonary embolism in emergency departments. Retrieved from https://www.hssib.org.uk/patient-safety-investigations/clinical-decision-making-diagnosis-of-pulmonary-embolism-in-emergency-departments/investigation-report/
Huckman, R. S., & Barro, J. R. (2005). NBER working paper series cohort turnover and productivity: The July phenomenon in teaching hospitals. Retrieved from http://www.nber.org/papers/ w11182
Jen, M. H., Bottle, A., Majeed, A., Bell, D., & Aylin, P. (2009). Early in-hospital mortality following trainee doctors’ first day at work. PLoS ONE, 4(9), Article e7103. https://doi.org/10.1371/jo urnal.pone.0007103
Kafle, N. P. (2011). Hermeneutic phenomenological research method simplified. Bodhi: An Interdisciplinary Journal, 5(1), 181–200. https://doi.org/10.3126/bodhi.v5i1.8053
Karunaratne, D., Chandratilake, M., & Marambe, K. (2023). Annexure-1 Additional supportive quotations (Version 2). [Data set]. Figshare. https://doi.org/10.6084/m9.figshare.23536548.v2
Khan, K., Pattison, T., & Sherwood, M. (2011). Simulation in medical education. Medical Teacher 33(1), 1-3. https://doi.org/10.3109/0142159X.2010.519412
Koufidis, C., Manninen, K., Nieminen, J., Wohlin, M., & Silén, C. (2020). Grounding judgement in context: A conceptual learning model of clinical reasoning. Medical Education, 54(11), 1019–1028. https://doi.org/10.1111/medu.14222
Kozlowski, D., Hutchinson, M., Hurley, J., Rowley, J., & Sutherland, J. (2017). The role of emotion in clinical decision making: An integrative literature review. BMC Medical Education, 17(1), Article 255. https://doi.org/10.1186/s12909-017-1089-7
Laal, M., & Laal, M. (2012). Collaborative learning: What is it? Procedia Social and Behavioral Sciences, 31, 491–495. https://doi.org/10.1016/j.sbspro.2011.12.092
Langridge, N., Roberts, L., & Pope, C. (2015). The clinical reasoning processes of extended scope physiotherapists assessing patients with low back pain. Manual Therapy, 20(6), 745-750. https://doi.org/10.1016/j.math.2015.01.005
Lave, J. (1991). Situating learning in communities of practice. In L. B. Resnick, J. M. Levine, & S. D. Teasley (Eds.), Perspectives on socially shared cognition (pp. 63–82). American Psychological Association. https://doi.org/10.1037/10096-003
Laverty, S. M. (2003). Hermeneutic phenomenology and phenomenology: A comparison of historical and methodological considerations. International Journal of Qualitative Methods, 2(3), 21–35. https://doi.org/10.1177/160940690300200303
Lee, C. Y., Jenq, C. C., Chandratilake, M., Chen, J., Chen, M. M., Nishigori, H., Wajid, G., Yang, P. H., Yusoff, M. S. B., & Monrouxe, L. (2021). A scoping review of clinical reasoning research with Asian healthcare professionals. Advances in Health Sciences Education, 26(5), 1555–1579. https://doi.org/10.1007/s10459-021-10060-z
Lempp, H., Seabrook, M., Cochrane, M., & Rees, J. (2005). The transition from medical student to doctor: Perceptions of final year students and preregistration house officers related to expected learning outcomes. International Journal of Clinical Practice, 59(3), 324–329. https://doi.org/10.1111/j.1742-1241.2005.00 438. x
Linn, A., Khaw, C., Kildea, H., & Tonkin, A. (2012). Clinical reasoning: A guide to improving teaching and practice. Australian Family Physician, 41(1), 18–20. https://search.informit.org/doi/10. 3316/informit.875577247352301
Malterud, K., Siersma, V. D., & Guassora, A. D. (2016). Sample size in qualitative interview studies: Guided by information power. Qualitative Health Research, 26(13), 1753-1760. https://doi.org/10.1177/1049732315617444
Mamede, S., Schmidt, H. G., & Penaforte, J. C. (2008). Effects of reflective practice on the accuracy of medical diagnoses. Medical Education, 42(5), 468–475. https://doi.org/10.1111/j.1365-2923. 2008.03030.x
Mamede, S., van Gog, T., Moura, A. S., de Faria, R. M. D., Peixoto, J. M., Rikers, R. M. J. P., & Schmidt, H. G. (2012). Reflection as a strategy to foster medical students’ acquisition of diagnostic competence. Medical Education, 46(5), 464–472. https://doi.org/10.1111/j.1365-2923.2012.04217.x
Miller, G. (1990). The assessment of clinical skills/competence/performance. Academic Medicine, 65(9), S63–S67. https://doi.org/10.1097/00001888-199009000-00045
Monrouxe, L. V., Grundy, L., Mann, M., John, Z., Panagoulas, E., Bullock, A., & Mattick, K. (2017). How prepared are UK medical graduates for practice? A rapid review of the literature 2009-2014. British Medical Journal Open, 7, Article e013656. https://doi.org/10.1136/bmjopen-2016-013656
Morris, T. H. (2020). Experiential learning – A systematic review and revision of Kolb’s model. Interactive Learning Environments, 28(8), 1064–1077. https://doi.org/10.1080/10494820.2019.15702 79
Muylaert, C. J., Sarubbi, V., Jr., Gallo, P. R., Neto, M. L. R., & Reis, A. O. A. (2014). Narrative interviews: An important resource in qualitative research. Revista Da Escola de Enfermagem Da USP, 48, 184–189. https://doi.org/10.1590/s0080-623420140000800027
Norman, G. (2005). Research in clinical reasoning: Past history and current trends. Medical Education, 39(4), 418–427. https://doi.org/10.1111/j.1365-2929.2005.02127.x
Norman, G., Young, M., & Brooks, L. (2007). Non-analytical models of clinical reasoning: The role of experience. Medical Education, 41(12), 1140–1145. https://doi.org/10.1111/j.1365-292 3.2007.02914.x
O’Brien, B. C., & Battista, A. (2020). Situated learning theory in health professions education research: A scoping review. Advances in Health Sciences Education, 25(2), 483–509. https://doi.org/10.1007/s10459-019-09900-w
Olusegun, S. (2015). Constructivism learning theory: A paradigm for teaching and learning. IOSR Journal of Research & Medical Edication, 5(6), 66–70.
Pelaccia, T., Tardif, J., Triby, E., & Charlin, B. (2011). An analysis of clinical reasoning through a recent and comprehensive approach: The dual-process theory. Medical Education Online, 16(1), Article 5890. https://doi.org/10.3402/meo.v16i0.5890
Prince, K. J. A. H., Van de Wiel, M. W. J., Scherpbier, A. J. J. A., Van der Vleuten, C. P. M., & Boshuizen, H. P. A. (2000). A qualitative analysis of the transition from theory to practice in undergraduate training in a PBL-medical school. Advances in Health Sciences Education, 5, 105–116. https://doi.org/10.1023/a:1009873003677
Prince, K. J. A. H., Van de Wiel, M. W. J., Van der Vleuten, C. P. M., Boshuizen, H. P. A., & Scherpbier, A. J. J. A. (2004). Junior doctors’ opinions about the transition from medical school to clinical practice: A change of environment. Education for Health, 17(3), 323–331. https://doi.org/10.1080/13576280400002510
Robertson, D. (2012). Critical thinking and clinical reasoning in new graduate Occupational therapists: A phenomenological study. [Doctoral Dissertation, Robert Gordan University]. OpenAIR@RGU. http://hdl.handle.net/10059/792
Ryan, R. M., & Deci, E. L. (2000). Self-determination theory and the facilitation of intrinsic motivation, social development, and well-being. American Psychologist, 55(1), 68–78. https://doi.org/10.1037/0003-066X.55.1.68
Schmidt, H., & Rikers, R. (2007). How expertise develops in medicine: Knowledge encapsulation and illness script formation. Medical Education, 41(12), 1133–1139. https://doi.org/10.1111/j. 1365-2923.2007.02915.x
Schmidt, H. G., & Boshuizen, H. P. A. (1993). On acquiring expertise in medicine. Educational Psychology Review, 5(3), 205–221. https://doi.org/10.1007/BF01323044
Tallentire, V. R., Smith, S. E., Facey, A. D., & Rotstein, L. (2017). Exploring newly qualified doctors’ workplace stressors: An interview study from Australia. British Medical Journal Open, 7, e015890. https://doi.org/10.1136/bmjopen-2017-015890
Tallentire, V. R., Smith, S. E., Skinner, J., & Cameron, H. S. (2011). Understanding the behaviour of newly qualified doctors in acute care contexts. Medical Education, 45(10), 995–1005. https://doi.org/10.1111/j.1365-2923.2011.04024.x
Taylor, D. C. M., & Hamdy, H. (2013). Adult learning theories: Implications for learning and teaching in medical education: AMEE Guide No. 83. Medical Teacher, 35(11), e1561–e1572. https://doi.org/10.3109/0142159X.2013.828153
Teunissen, P. W., & Westerman, M. (2011). Opportunity or threat: The ambiguity of the consequences of transitions in medical education. Medical Education, 45(1), 51–59. https://doi.org/10.1111/j.1365-2923.2010.03755.x
Tolsgaard, M. G., Kulasegaram, K. M., & Ringsted, C. V. (2016). Collaborative learning of clinical skills in health professions education: The why, how, when and for whom. Medical Education, 50(1), 69–78. https://doi.org/10.1111/medu.12814
Varpio, L., Ajjawi, R., Monrouxe, L. V., O’Brien, B. C., & Rees, C. E. (2017). Shedding the cobra effect: Problematising thematic emergence, triangulation, saturation and member checking. Medical Education, 51, 40–50. https://doi.org/10.1111/medu.13124
Woods, N. N. (2007). Science is fundamental: The role of biomedical knowledge in clinical reasoning. Medical Education, 41(12), 1173–1177. https://doi.org/10.1111/j.1365-2923.2007.029 11.x
Yardley, S., Teunissen, P. W., & Dornan, T. (2012). Experiential learning: AMEE Guide No. 63. Medical Teacher, 34(2), e102–e115. https://doi.org/10.3109/0142159X.2012.650741
*WCD Karunaratne
Centre for Medical Education,
University of Dundee
Scotland, DD2 4BF
+44 7594 504928
Email: dilminikarunaratne@gmail.com / Wkarunaratne001@dundee.ac.uk
Submitted: 8 July 2023
Accepted: 21 September 2023
Published online: 2 April, TAPS 2024, 9(2), 1-4
https://doi.org/10.29060/TAPS.2024-9-2/GP3089
Lamiaa Mohsen1, Marwa Shabrawy1, Waleed Hassan1, Zakia Arfeen2 & Mohammed Ahmed Rashid2
1School of Medicine, Newgiza University, Cairo, Egypt; 2UCL Medical School, Faculty of Medical Sciences, University College London, London, United Kingdom
Abstract
Introduction: In 2016, a new university opened in Egypt that sought to ‘challenge the ordinary’ in a country with a long and rich heritage of knowledge production. Newgiza University (NGU), located adjacent to the ancient pyramids of Giza outside Cairo, launched with a foundational focus on health sciences, through undergraduate courses in medicine, dentistry, and pharmacy. Each programme was co-developed through an academic collaboration with University College London (UCL), a high-ranking, research-intensive, UK university.
Methods: As the collaboration passes a key juncture of graduating the first cohorts of doctors, dentists, and pharmacists from these courses who embark on their professional careers, we examine and reflect on the journey to date. In particular, this article reviews the growing academic literature about international partnerships in medical education, describes how curricula, assessments, and management structures in the three NGU healthcare courses were adapted and finessed to fit the Egyptian context, and shares the lessons learnt by the academic leadership teams responsible for this challenging but stimulating collaboration project.
Results: The collaboration between NGU and UCL is an example of an international education partnership approach that seems to be growing in popularity globally. The overriding importance of building trust and respect between partners was clear in this collaboration, as was the need for clear communication channels to guide the necessarily complex decision-making that underpinned it.
Conclusion: Given inevitable power imbalances in such collaborations, critical examinations of their impacts on organisations, staff, and students are an important research priority in the future.
Practice Highlights
- International education partnerships are growing in popularity and there is a growing academic literature exploring different collaboration models.
- Co-development of healthcare professions education curricula across national borders requires attention to relational factors including trust and respect.
- Power differentials make it crucial to evaluate such partnerships using a critical lens.
I. INTRODUCTION
Egypt has a long and rich intellectual and cultural heritage dating back millennia. In the last century, Egyptian higher education sector has been shaped both by globalisation and a series of governmental policies (Reid, 2002). Against this backdrop, a new university was conceptualised that would ‘challenge the ordinary’ by creating a diverse community of staff and students to spearhead academic and scientific advancement in Egypt and beyond. Endorsed by Presidential Decree as a non-profit, private university in April 2010, Newgiza University (NGU) officially opened in 2016 with an initial focus on healthcare sciences, launching schools in Medicine, Dentistry, and Pharmacy.
As part of its mission to create an exciting learning environment that is filled with energy, talent, and cultural diversity to redefine the future of Egypt, NGU had a strategic objective to partner with a leading overseas university with a strong track-record in health professions education (HPE) to co-develop these new programmes. After briefly considering the literature on international education partnerships, this article will describe the experiences of an academic collaboration between NGU and University College London (UCL) to co-develop new undergraduate programmes in Medicine, Dentistry, and Pharmacy, that graduated their first cohorts in early 2023.
An emerging phenomenon in recent decades has been the delivery of curricula outside of the country in which they were developed. A variety of terms have been used to describe such arrangements, including ‘offshore education’, ‘transnational education’, and ‘crossborder curriculum partnerships’. The purpose of these partnerships is to provide comparable educational experiences in both institutions and can be attractive for students who are seeking a foreign qualification but do not wish to move overseas.
A literature review on international curriculum partnerships noted that almost all identified articles were about early-stage developments, reflecting that this is a growing and evolving topic (Waterval et al., 2015). It found that the most common reason for partnerships to deteriorate is mistrust and ‘disturbed relationships’, going on to conclude that there are no quick fixes to resolve cultural differences and that personal collaborations at all levels should be prioritised. As was noted in a subsequent systematic review, the academic literature is currently dominated by single case studies and there are many possible directions for future research (Kosmützky et al., 2016). Within HPE, Hodges et al. (2009) observed the growing trend of international education partnerships within a rapidly evolving globalisation discourse within the field more broadly. A later study that focussed on challenges and solutions in the context of international education partnerships in medicine suggested that there are both financial and academic advantages to both institutions (Waterval et al., 2016).
II. METHODS
From its inception, the stated vision of NGU has been to establish healthcare programmes that inspire and educate a new generation of clinicians by moving away from structures and practices of traditional universities in the region that limit effective learning. The NGU leadership team sought to reduce class sizes, focus on innovation and leadership, and move away from didactic and theoretical teaching, and towards a more patient-centred and practice-focused model of education. University College London (UCL) is based in the heart of London in the UK and is consistently ranked as one of the world’s best universities. It has schools of medicine, dentistry, and pharmacy, which each focuses on providing integrated and patient-focused education.
The underlying ethos of this collaboration has been of respectful co-development, with each team mindful of what they bring ‘to the table’ by way of expertise and experience. As such, a paradoxical success of this collaboration has been that it has shrunk and scaled back since the outset, as NGU academic, managerial, and administrative teams have taken on increasing levels of independent responsibility and their counterpart UCL teams have evolved to play roles of advisor and mentor accordingly. Although UCL curricula, assessments, and policies have been the basis for the corresponding NGU programmes in each of the three disciplines, these have gradually been adapted and contextualised to fit with the vision and operating environment of NGU.
The collaboration was structured around a three-phase approach. Phase one involved an exercise to clarify the vision and high-level structure for the three programmes and agree the legal and academic basis for the collaboration project. Phase two involved the detailed co-design and implementation of curricula and assessments across the three programmes to support their launch and delivery. Phase three, which is currently in progress, involves the ongoing operationalisation and continuous improvement of the programmes and the further development of the schools in other domains, including postgraduate education and research. These three phases are underpinned by a service contract between the two universities that takes the shape of work packages, which set the parameters and arrangements for each aspect of the collaboration.
III. RESULTS
Although geopolitical unrest was identified as a risk by both parties at the outset, this has not affected the project thus far. Instead, it has been a pandemic, COVID-19, that has proved to be the greatest disruption. Restrictions to air travel and international movement meant that for almost two years, the UCL-NGU collaboration shifted to an entirely virtual format.
This period of physical distance between the respective teams illuminated the importance of in-person visits. Seeing each other’s campuses and witnessing the contexts in which the two universities function was undoubtedly an important part of strengthening the relationship. That the project had been established for four years at the time of the onset of the pandemic meant that this was fortunately already well developed. As well as the important contextual understanding that these visits provided, it also allowed teams to socialise together and rich conversations over coffee breaks and meals often blurred the boundaries between professional and personal relationships. Indeed, close relationships between NGU and UCL counterparts was central to the success of the collaboration.
A particularly intellectually engaging aspect of this collaboration has been the adaptation of curricula content for a context that differs in social, political, cultural, epidemiological, and clinical domains. Whilst many scientific and technical aspects of HPE curricula seemingly transfer across countries readily, collaborators on both sides were surprised by the extent to which they required modification. For example, the many epidemiological and health system differences between the UK and Egypt meant there were important differences in disease patterns, drug availability, and technical equipment that need to be reflected in curricula to prepare students adequately for clinical practice. Likewise, significant areas of each curricula focus on topics linked to professional practice, including communication, healthcare ethics and law, and patient safety and clinical governance. These topic areas required significant adaptation to align with Egyptian legal and social practices, often prompting stimulating discussions and several iterative stages of development to contextualise individual teaching resources.
As well as drawing on UCL curricula structure and teaching resources to establish the new courses across the three healthcare schools, NGU also utilised UCL assessment policies and items to develop NGU assessments in each of the schools. There were, though, important adaptations. For example, the regulatory context in Egyptian higher education meant that a greater proportion of assessment weighting had to be given to ‘in semester’ assessment, necessitating a shift in emphasis from the UCL approach. Rather than using UCL assessment items directly in summative exams, the approach from the NGU schools was instead to use these to help their own faculty recognise the characteristics of high-quality items as they developed their own items. This was supplemented by many assessment writing workshops, which were often cross-disciplinary in the early phases of the collaboration as each faculty grew in size. Assessment tools used at UCL, including objective structured clinical examinations and workplace-based assessments, are not widely used in undergraduate education in Egypt and took time to embed.
One of the benefits of designing three undergraduate healthcare programmes together, launching simultaneously on a purpose-built modern campus, was the opportunity to maximise interprofessional education opportunities. This was realised through an ambitious introductory module for students from all three programmes. Not only did this provide an opportunity for students from all three NGU healthcare courses to learn together and from each other, it also embedded an inter-disciplinary approach across the three NGU schools, with faculty members from different schools often co-leading particular sessions or components of the module. On top of these benefits, it also enabled the three UCL schools to work much more closely and ensure alignment across all of their approaches. This interprofessional collaboration helped to foster closer working between schools at both NGU and UCL in other domains, which was an unexpected but pleasing consequence of this collaboration.
IV. DISCUSSION
A striking finding for teams from both universities was the central importance of human and relational factors to the collaboration. The formation of a new university creates distinct requirements in terms of leadership and culture, which can be challenging for any education leader or team. The additional layer of complexity of managing an international partner heightens this challenge, and meant the NGU leadership teams had to manage many more stakeholders than one might ordinarily have to contend with. This was especially so given the history and prestige associated with UCL, being from a high-income country with a reputation for academic excellence. The history of the UK as a former colonising country and Egypt as a former colonised country can also not be ignored. Together, these power imbalances and perceived knowledge hierarchies inevitably created a context that can easily slip to being unequal and exploitative.
By recognising the tensions faced by the NGU leadership and the potentially problematic power structures inherent to this collaboration, the teams in this collaboration acutely recognised the need for flexibility and understanding. The principle of respect and friendship was of overriding importance as it framed this collaboration not as one underpinned by ‘neutrality’, as such a thing does not exist, but rather through an outlook of deeply caring about the experiences and success of your partner team. Throughout the operational and academic aspects of the collaboration, this overriding focus on co-development and respect allowed both partners to ensure they were holding themselves and one another to account for the sake of the project mission.
Another crucial area of learning for both teams has been a sense of regret at the lack of formal scholarship and research that has been embedded in this collaboration. From the outset, the unwavering focus has been to help NGU achieve high-quality education programmes and to ensure that NGU students have an excellent student experience. This relentless focus on educational delivery, assessment, and quality management of the programmes left little time to focus on scholarship, despite a clear desire from both sides to do so. In particular, both teams recognise the many avenues of research that could have been explored through the collaboration thus far, including psychometric analyses comparing assessment performance between NGU and UCL cohorts all the way through to in-depth work using theories that help understand the complex relational factors through lenses of power and globalisation, and much between. Fortunately, this has become a priority as the collaboration moves to its next stage.
V. CONCLUSION
As the first student cohorts from its three healthcare courses graduate, NGU will enter a new stage of its development, and plans are underway to extend and deepen the collaboration with UCL across these schools. This article has summarised the dearth of academic literature on international partnerships in HPE and juxtaposed this with a complex and rich story that highlights the many different insights that can emerge from a single multi-professional collaboration. In our increasingly globalised world, the cross-cultural and relational issues raised through these partnerships have the potential to have wide-ranging and beneficial findings that extend beyond those communities working specifically on international partnerships. The importance of embedding scholarship into international HPE collaborations is clear to the academic teams on both sides of the UCL-NGU collaboration. As we plan for this in the next stages of our work together, we encourage others involved in international education partnerships to do the same and contribute to a scholarly area of growing importance in the field.
Notes on Contributors
LM led the collaboration on behalf of the NGU school of medicine, conceptualised the study, analysed the literature, and co-wrote the manuscript.
MS co-ordinated the collaboration on behalf of NGU, conceptualised the study, and developed the manuscript.
WH managed the collaboration on behalf of the NGU school of medicine, conceptualised the study, and developed the manuscript.
ZA co-ordinated the collaboration on behalf of UCL medical school, conceptualised the study, and developed the manuscript.
MAR led the collaboration on behalf of UCL medical school, reviewed the literature, conceptualised the study, and co-wrote the manuscript.
Funding
No funding was received.
Declaration of Interest
All authors were engaged in the academic collaboration described in this article.
References
Hodges, B. D., Maniate, J. M., Martimianakis, M. A., Alsuwaidan, M., & Segouin, C. (2009). Cracks and crevices: Globalization discourse and medical education. Medical teacher, 31(10), 910-917.
Kosmützky, A., & Putty, R. (2016). Transcending borders and traversing boundaries: A systematic review of the literature on transnational, offshore, cross-border, and borderless higher education. Journal of Studies in International Education, 20(1), 8-33.
Reid, D. M. (2002). Cairo University and the making of modern Egypt (Vol. 23). Cambridge University Press.
Waterval, D. G., Frambach, J. M., Driessen, E. W., & Scherpbier, A. J. (2015). Copy but not paste: A literature review of crossborder curriculum partnerships. Journal of Studies in International Education, 19(1), 65-85.
Waterval, D. G., Frambach, J. M., Oudkerk Pool, A., Driessen, E. W., & Scherpbier, A. J. (2016). An exploration of crossborder medical curriculum partnerships: Balancing curriculum equiva- lence and local adaptation. Medical teacher, 38(3), 255-262.
*Mohammed Ahmed Rashid
University College London,
Gower Street, London,
WC1E 6AE, United Kingdom
Email: ahmed.rashid@ucl.ac.uk
Submitted: 27 April 2023
Accepted: 17 August 2023
Published online: 2 January, TAPS 2024, 9(1), 36-41
https://doi.org/10.29060/TAPS.2024-9-1/OA3051
Mae Yue Tan1,2, Zong Jie Koh1,3, Shoban Krishna Kumar4, Rui Min Foo5, Rou An Tan6, Nisha Suyien Chandran7,8 Jeremy Bingyuan Lin1,2, Malcolm Mahadevan9 & Eng Loon Tng5
1Department of Paediatrics, Khoo Teck Puat – National University Children’s Medical Institute, National University Health System, Singapore; 2Department of Paediatrics & 8Department of Medicine, Yong Loo Lin School of Medicine, National University of Singapore, Singapore; 3Department of General Surgery, University Surgical Cluster, National University Health System, Singapore; 4Division of Advanced Internal Medicine, Department of Medicine, National University Hospital, National University Health System, Singapore; 5Department of Medicine & 6Department of Intensive Care Medicine, Ng Teng Fong General Hospital, National University Health System, Singapore; 7Division of Dermatology, Department of Medicine, National University Hospital, National University Health System, Singapore; 9Emergency Medicine Department, National University Hospital, National University Health System, Singapore
Abstract
Introduction: The night float (NF) system has been instituted in some hospitals in Singapore to improve the working hours and wellbeing of junior doctors. There have been concerns of compromised learning and patient safety with NF. The objective of this study is to compare clinical competency outcomes, based on existing assessment framework, between post-graduate year 1 (PGY1) doctors working on NF versus traditional call (TC) systems. The secondary aim was to explore patient safety outcomes between these groups of PGY1s.
Methods: Data on the formal assessments of PGY1s using the Entrustable Professional Activities (EPAs) and medical errors were prospectively collected between May 2021 and April 2022 from two hospitals that employed different on-call systems. Data was analysed descriptively. Categorical data was analysed using the Chi-square test or Fisher’s exact test where appropriate.
Results: One hundred and ninety-three PGY1s consented to the study. There was no statistically significant difference in the clinical competency of PGY1s in both groups. The number of PGY1s who had ‘needs improvement’ scores in a detailed EPA was not significantly different (9.0% in the NF group versus vs 3.7% in the TC group (p = 0.14)). They nonetheless passed the overall core EPA and no PGY1 failed their postings. No serious reportable medical errors occurred in either group.
Conclusion: PGY1s who worked on NF are equally competent compared to those who worked on TC based on the EPA assessment matrix. Patient safety is not compromised by PGY1s working on NF.
Keywords: Clinical competence, Float, Junior doctor, Patient safety, Wellbeing
Practice Highlights
- Night float did not affect competency of post-graduate Year 1 doctors on current assessments.
- Night float did not lead to compromised patient safety.
- We provide objective data in consideration of restructuring working hours for junior doctors.
I. INTRODUCTION
Post graduate year 1 (PGY1) doctors are fresh graduates who are in their transitional year where they learn clinical decision-making skills and how to perform simple medical procedures independently. In Singapore, following the Medical Registration Act, PGY1s are required to complete 4 months of Internal Medicine and 4 months of General Surgery or Orthopaedic Surgery, with another 4-month posting of their choice in their 12 months as a PGY1 (Ministry of Health Holdings Pte Ltd, 2018). As part of the national PGY1 training framework (Ministry of Health, 2019), each hospital is required to provide training (teaching activities) to allow PGY1s to achieve their learning and competency outcomes. PGY1s are assessed via a standardized matrix which is used across all hospital rotations and institutions. They are expected to achieve competency in situations where senior supervision is less readily available, for example, while working on-call. PGY1 duties are similar regardless of discipline as they focus on core medical competencies common to general medical practice.
In Singapore, some hospitals have instituted the night float (NF) system as a service model where a dedicated team of doctors, including PGY1s, take over the care of patients for consecutive nights in a week. A different team of doctors will resume care of patients the following day. This facilitates timely handovers of patient management, eliminates the need for prolonged post-night call working hours and provides junior doctors with adequate rest, avoiding sleep deprivation. Conversely, in the traditional call (TC) system, junior doctors commence night duties immediately after their daytime routines. Frequently, at the end of their night calls, PGY1s continue with daytime work till mid-day or later, resulting in shifts of up to 36 hours.
The Accreditation Council for Graduate Medical Education (ACGME) guidelines recommended a maximum of 80 hours of duties per week based on extant literature on the impact of prolonged duty hours on burnout and fatigue (Singapore Medical Council, 2017), medical errors and adverse events (Barger et al., 2006; Landrigan et al., 2004; Trockel et al., 2020). Departments that have instituted the NF system have significantly improved their compliance to duty hour recommendations. However, concerns were raised regarding reduced training opportunities, specifically during the after-office hour period due to the reduced working hours with NF as well as potential compromises in patient safety arising from communication lapses associated with frequent handovers (Desai et al., 2013; Sun et al., 2016). These concerns have prevented widespread adoption of NF in Singapore hospital systems.
Two studies in Singapore have shown that residents who worked on NF felt that it did not affect their learning outcomes or compromise patient safety (Loo et al., 2020; Tan et al., 2019). However, these studies assessed the perceptions of junior doctors and provided no objective data for comparison of NF against TC. We thus aimed to compare clinical competency outcomes between PGY1s who worked on NF and those who worked on TC, across similar specialties. The secondary aim was to explore any differences in patient safety and medical errors between these two groups. We chose the PGY1 group for this study for the following reasons. Firstly, PGY1 training outcomes and assessments are standardized nationwide thus allowing for direct comparisons across institutions. Additionally, any policy implementation or change would impact all PGY1s across the board equally. In contrast, physicians in their later years of training (PGY2 and above) are a heterogenous group with their training assessment frameworks dependent on the relevant speciality programmes. Secondly, PGY1s are considered to have the one of the highest risks of burnout among physicians and are likely to benefit most from well-being initiatives. Lastly, the PGY1 year is a compulsory year of formative training with PGY1s subsequently graduating as fully licensed physicians. This decisive and important transitional year from medical training to clinical practice underscores the importance of considerations for their training and competency.
II. METHODS
This study was conducted over three rotations (each PGY1 rotation spans 4 months) from May 2021 to April 2022. PGY1s working in National University Health System cluster (either in National University Hospital where NF is the structure for PGY1s rotating through General Surgery, Internal Medicine, and Orthopaedics (since January 2022), or Ng Teng Fong General Hospital where TC is practiced) were invited to participate via emails. PGY1s could opt out of the study. Ethics approval was obtained [National Healthcare Group Domain Specific Review Board (NHG DSRB), Singapore; Reference No.: 2021/00536].
Prospective data was collected from formal educational and workplace-based assessments. Currently, the Entrustable Professional Activities (EPAs) framework, which describes professional activities that a trainee can be entrusted to perform at varying levels of supervision, is used for this purpose. EPAs are established milestones in post graduate medical education to gauge whether trainees have achieved necessary skill sets that are appropriate for their level of training. In its current form, the local EPA framework for PGY1s includes 7 ‘core EPA’ groups. Each ‘core EPA’ group further encompasses a list of ‘detailed EPAs’. An example of a ‘core EPA’ and its ‘detailed EPAs’ is shown in Table 1. At the end of a rotation during their final evaluation, PGY1s are evaluated by their supervisors for each ‘detailed EPA’ as part of their ‘Learning Needs’. A grading of ‘needs improvement’ for a detailed EPA indicates that the PGY1 has not demonstrated sufficient competence in that specific activity. No input is required if a PGY1 is deemed to have met expectations for the detailed EPA. In performing this evaluation, the supervisor is expected to canvass feedback from other team and faculty members who have worked with the PGY1. At the end of the rotation, should all EPAs (core and detailed) be assessed as competent, the supervisor would grade the posting outcome as a pass, with the opportunity to nominate the PGY1 for the national outstanding PGY1 award.
|
Core Entrustable Professional Activity (EPA) |
Detailed EPAs |
|
Manage patients by obtaining a detailed history, performing appropriate physical examination, requesting & follow-through relevant diagnostic evaluation & therapeutic interventions. |
|
Table 1. Example of an Entrustable Professional Activity (EPA), with detailed EPAs within the core EPA
Data on medical errors or patient safety issues involving PGY1s, including near-miss events, were also collected from the medical error reporting systems of both hospitals. All data were anonymized prior to data analysis. Data was analysed descriptively and with comparative statistics. Chi-square test or Fisher’s exact test were used for analysis of categorical data where appropriate.
III. RESULTS
A total of 193 PGY1s consented to this study with no opt-outs. There was no statistically significant difference in the proportion of PGY1s with ‘needs improvement’ between the 2 groups: 9.0% of PGY1s in the NF group compared to 3.7% in the TC group had ‘needs improvement’ in any of the ‘detailed EPAs’ (p = 0.16) (Table 2). All PGY1s with ‘needs improvement’ were deemed competent in the ‘core EPA’. Notably, three PGY1s in the NF group who had ‘needs improvement’ in the ‘detailed EPAs’ were nominated for the Outstanding PGY1 Award by the Ministry of Health. All PGY1s in this study passed their postings satisfactorily.
|
|
Night Float (NF) |
Traditional On-Call (TC) |
P-value |
|
Total number of PGY1s who had ‘needs improvement’ for a detailed EPA / total number of PGY1s (%) |
10 / 111 (9.0) |
3 / 82 (3.7) |
0.16 |
|
1st rotation (%) |
3 / 36 (8.3) |
2 / 29 (6.9) |
0.99 |
|
2nd rotation (%) |
2a / 32 (6.3) |
0 / 22 (0.0) |
0.51 |
|
3rd rotation (%) |
5b /43 (11.6) |
1 / 31 (3.2) |
0.39 |
Table 2. Proportion of post graduate year 1 (PGY1) doctors who had detailed EPAs that were marked as ‘needs improvement’
aBoth these PGY1s were nominated for the outstanding PGY1 award.
bOne PGY1 was nominated for the outstanding PGY1 award.
In terms of medical errors, there were 25 reported events in the NF group and 12 in the TC group. To account for the difference in number of PGY1s between both groups, we reported the average event rate per PGY1, i.e. event rate over the number of PGY1s in the rotation. There was no statistically significant difference in the average event rate per PGY1 between the two groups (0.23 vs 0.15, p = 0.20) (Table 3). There was also no statistically significant difference between the two groups when comparison was made for each rotation. All reported errors regardless of NF or TC, were in the ‘No Harm’, or ‘Minor Harm’ categories with no serious reportable events: 24.3% of all errors were needle stick-related events while 24.3% were for wrongly labelled blood tubes.
|
|
Night Float (NF) |
Traditional On-Call (TC) |
P-value |
|
Average event rate per PGY1 |
0.23 |
0.15 |
0.20 |
|
1st rotation |
0.11 |
0.14 |
0.99 |
|
2nd rotation |
0.25 |
0.14 |
0.49 |
|
3rd rotation |
0.30 |
0.16 |
0.18 |
Table 3. Event rates for reported events (either medical errors or patient safety issues) in post graduate year 1 (PGY1) doctors over the study period.
IV. DISCUSSION
Our study revealed insights on the effects of the NF system on the clinical training of PGY1s and impact on patient safety. There was no statistically significant difference in objective clinical competency between PGY1s working on NF or TC. This refutes the concern of inadequate training opportunities arising from shorter working hours during after-office-hours shifts. These objective findings are in line with the subjective evaluation and perceptions of junior doctors on the impact of the local night float system on their training (Loo et al., 2020; Tan et al., 2019).
Though the time spent for emergency-related work or ‘on-call’ situations where senior supervision is less readily is reduced on the NF compared to the TC groups, the training outcomes were similar and not compromised. We postulate that this is because of the robust formal training programme during the daytime which is consistent across hospitals given the national framework guidelines. In addition, the high number of emergency cases being admitted after office hours in both the NF and TC groups provide ample learning opportunities for the PGY1s. Regardless of which service model the PGY1s practice in, formal training during daytime work is consistent across hospitals given the national framework guidelines. PGY1s have protected teaching time each week and they are able to catch up with the teaching topics through e-learning modules when they are post call. As such, the NF system does not negatively affect their learning through the formal teaching program. While hours spent on training activities are important, it is just one component that contributes to learning outcomes. Previous literature has shown that shorter training hours can also optimize learning as it allows between-session and post-training learning to occur (Molloy et al., 2012).
Though not statistically significant, the NF group did have a higher number of PGY1s who were flagged for ‘needs improvement’ in their ‘detailed EPA’ as compared to the TC group (9.0% vs 3.7%, p = 0.16). We believe this was a result of the limitations with the EPA assessment matrix rather than poor clinical training in the PGY1s in the NF group. The standardized assessment matrix in the overall evaluation form provides only two options in the grading of each ‘detailed EPA’; PGY1s who are deemed to have failed the task should be graded as ‘needs improvement’ whilst the section is left blank by the supervisors for PGY1s who are deemed to be competent in the task. Thus, the grade of ‘needs improvement’ is in reality that of failure, but is commonly misconstrued as having room for improvement in an already competent PGY1. Hence, supervisors may mistakenly grade the ‘detailed EPA’ domains as ‘needs improvement’ without any intent that the PGY1 is in any way incompetent. Supervisors may even grade the PGY1s as ‘needs improvement’ in an effort to spur them to greater heights, and we suspect this to be the case as seen in the 3 PGY1s who were nominated for the Outstanding Award on their overall assessment despite having a “needs improvement” grade for a detailed EPA. Additionally, as with any assessment matrix, the utility and accuracy of EPAs in reflecting competency is heavily dependent on how well it is used by the supervisor and PGY1, and its refinement and standardization continue to be work in progress.
Our study showed that the NF system does not affect patient safety adversely. There were no major clinical errors or adverse patient events in both groups. There were also no statistically significant differences in the minor clinical errors, categorized as ‘No Harm’ and ‘Minor Harm’, that were made by PGY1s between the two groups (0.23 vs 0.15, p = 0.20). Given the anonymity of data on the medical error reporting systems, we were unable to discern whether errors were made while on call or if certain PGY1s were making repeated errors. As these numbers are small, comparative analysis is not meaningful and thus not performed. There were no medical errors arising from miscommunications because of increased handovers in our study. We believe that PGY1s were able to provide better quality handovers in a timelier fashion due to the structured work-hour cycles in NF. NF reduces PGY1 fatigue and the associations between fatigue and its impact on judgement, competency and risk of mistakes has been demonstrated (Trockel et al., 2020).
V. CONCLUSION
In conclusion, our study supports existing evidence that the NF system does not compromise clinical training for PGY1s or patient safety. The NF system emphasizes the importance of training quality over quantity and enhances PGY1 wellbeing. We believe our study provides objective data for the medical fraternity for consideration in the restructuring of working hours for junior doctors (Abu Baker, 2022).
Notes on Contributors
MYT contributed to design and conception of the work, data analysis and interpretation, drafted the article and revised it critically for important intellectual content. ZJK contributed to design and conception of the work, data analysis and interpretation, drafted the article and revised it critically for important intellectual content. SKK contributed to design and conception of the work, data analysis and interpretation, drafted the article and revised it critically for important intellectual content. RMF contributed to data acquisition and revised the article critically for important intellectual content. RAT contributed to data acquisition and revised the article critically for important intellectual content. NSC contributed to study conception, data interpretation and revised the article critically for important intellectual content. JBL contributed to design and conception of the work and revised the article critically for important intellectual content. MM contributed to conception of work, data interpretation and revised the article critically for important intellectual content. ELT contributed design and conception of the work, data acquisition and revised the article critically for important intellectual content. All authors read and approved the final version, and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Ethical Approval
This study was performed in line with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. Ethics approval for the study was obtained from the National Healthcare Group Domain Specific Review Board (NHG DSRB), Singapore; Reference No.: 2021/00536.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Acknowledgement
The authors would like to thank the Ministry of Health, Singapore, for supporting the implementation of the night float call system for junior doctors in our institution. We would also like to thank our PGY1s for consenting to this study, and our program coordinators for providing administrative assistance for this project. Lastly, we would like to thank Ms Sheena Nishanti Ramasamy for her assistance in editing and formatting the manuscript for submission.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Interest
The authors declare no relevant financial or non-financial competing interests with respect to the research, authorship and/or publication of this article.
References
Abu Baker, J. (2022, March 9). Review of junior doctors’ work hours among steps to improve healthcare workers’ well-being. Channel News Asia. https://www.channelnewsasia.com/singapore /review-junior-doctors-work-hours-among-steps-improve-healthcare-workers-well-being-2551376
Barger, L. K., Ayas, N. T., Cade, B. E., Cronin, J. W., Rosner, B., Speizer, F. E., & Czeisler, C. A. (2006). Impact of extended-duration shifts on medical errors, adverse events, and attentional failures. PLoS Medicine, 3(12), Article e487. https://doi.org/10.1371/journal.pmed.0030487
Desai, S. V., Feldman, L., Brown, L., Dezube, R., Yeh, H. C., Punjabi, N., Afshar, K., Grunwald, M. R., Harrington, C., Naik, R., & Cofrancesco, J., Jr (2013). Effect of the 2011 vs 2003 duty hour regulation-compliant models on sleep duration, trainee education, and continuity of patient care among internal medicine house staff: A randomized trial. JAMA Internal Medicine, 173(8), 649–655. https://doi.org/10.1001/jamainternmed.2013.2973
Landrigan, C. P., Rothschild, J. M., Cronin, J. W., Kaushal, R., Burdick, E., Katz, J. T., Lilly, C. M., Stone, P. H., Lockley, S. W., Bates, D. W., & Czeisler, C. A. (2004). Effect of reducing interns’ work hours on serious medical errors in intensive care units. The New England Journal of Medicine, 351(18), 1838–1848. https://doi.org/10.1056/NEJMoa041406
Loo, B. K. G., Ng, C. L., Chin, R. T., Davies, L. J., Yong, J., Ang, A. E. L., Chong, Y. W., & Tambyah, P. A. (2020). Nationwide survey comparing residents’ perceptions of overnight duty systems in Singapore: Night float versus full overnight call. Singapore Medical Journal, 61(10), 559–562. https://doi.org/10.11622/sme dj.2020149
Ministry of Health Holdings Pte Ltd. (2018). Medical service career path. https://www.physician.mohh.com.sg/medicine/medi cal-service-career-path
Ministry of Health Singapore. (2019, January 16). The national PGY1 training and assessment framework. https://www.moh.gov.sg/hpp/all-healthcareprofessionals/news/NewsArticleDetails/nationalpgy1_training_assessment_framework
Molloy, K., Moore, D. R., Sohoglu, E., & Amitay, S. (2012). Less is more: Latent learning is maximized by shorter training sessions in auditory perceptual learning. PloS One, 7(5), Article e36929. https://doi.org/10.1371/journal.pone.0036929
Singapore Medical Council. (2017). SMC circular – Guidelines on Postgraduate Year 1 (PGY1) training and postings for the accreditation of PGY1 training posts.
Sun, N. Z., Gan, R., Snell, L., & Dolmans, D. (2016). Use of a night float system to comply with resident duty hours restrictions: Perceptions of workplace changes and their effects on professionalism. Academic Medicine: Journal of the Association of American Medical Colleges, 91(3), 401–408. https://doi.org/10.1097/ACM.0000000000000949
Tan, B. Y., Ngiam, N. J., Chang, Z. Y., Tan, S. M. Y., Shen, X., Mok, S. F., Subramanian, S., Ooi, S. B. S., & Kee, A. C. (2019). Perceptions of a night float system for intern doctors in an internal medicine program: An Asian perspective. Korean Journal of Medical Education, 31(3), 271–276. https://doi.org/10.3946/kjme.2019.137
Trockel, M. T., Menon, N. K., Rowe, S. G., Stewart, M. T., Smith, R., Lu, M., Kim, P. K., Quinn, M. A., Lawrence, E., Marchalik, D., Farley, H., Normand, P., Felder, M., Dudley, J. C., & Shanafelt, T. D. (2020). Assessment of physician sleep and wellness, burnout, and clinically significant medical errors. JAMA Network Open, 3(12), Article e2028111. https://doi.org/10.1001/jamanet work open.2020.28111
*Dr Mae Yue TAN
Department of Paediatrics,
Khoo Teck Puat-National University
Children’s Medical Institute,
National University Health System, Singapore
Department of Paediatrics,
Yong Loo Lin School of Medicine,
National University of Singapore, Singapore
NUHS Tower Block Level 12,
1E Kent Ridge Rd, Singapore 119228
Email: mae_yue_tan@nuhs.edu.sg
Announcements
- Best Reviewer Awards 2025
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2025.
Refer here for the list of recipients. - Most Accessed Article 2025
The Most Accessed Article of 2025 goes to Analyses of self-care agency and mindset: A pilot study on Malaysian undergraduate medical students.
Congratulations, Dr Reshma Mohamed Ansari and co-authors! - Best Article Award 2025
The Best Article Award of 2025 goes to From disparity to inclusivity: Narrative review of strategies in medical education to bridge gender inequality.
Congratulations, Dr Han Ting Jillian Yeo and co-authors! - Best Reviewer Awards 2024
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2024.
Refer here for the list of recipients. - Most Accessed Article 2024
The Most Accessed Article of 2024 goes to Persons with Disabilities (PWD) as patient educators: Effects on medical student attitudes.
Congratulations, Dr Vivien Lee and co-authors! - Best Article Award 2024
The Best Article Award of 2024 goes to Achieving Competency for Year 1 Doctors in Singapore: Comparing Night Float or Traditional Call.
Congratulations, Dr Tan Mae Yue and co-authors! - Best Reviewer Awards 2023
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2023.
Refer here for the list of recipients. - Most Accessed Article 2023
The Most Accessed Article of 2023 goes to Small, sustainable, steps to success as a scholar in Health Professions Education – Micro (macro and meta) matters.
Congratulations, A/Prof Goh Poh-Sun & Dr Elisabeth Schlegel! - Best Article Award 2023
The Best Article Award of 2023 goes to Increasing the value of Community-Based Education through Interprofessional Education.
Congratulations, Dr Tri Nur Kristina and co-authors! - Best Reviewer Awards 2022
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2022.
Refer here for the list of recipients. - Most Accessed Article 2022
The Most Accessed Article of 2022 goes to An urgent need to teach complexity science to health science students.
Congratulations, Dr Bhuvan KC and Dr Ravi Shankar. - Best Article Award 2022
The Best Article Award of 2022 goes to From clinician to educator: A scoping review of professional identity and the influence of impostor phenomenon.
Congratulations, Ms Freeman and co-authors.









