Action research for improving medical education department practices in Pakistan
Submitted: 29 November 2024
Accepted: 22 September 2025
Published online: 7 April, TAPS 2026, 11(2), 102-113
https://doi.org/10.29060/TAPS.2026-11-2/OA3754
Juveria Arjumand1, Syed Muhammad Azfar2, Syeda Rubaba Azim3 & Rania Alkhadragy1,4
1Centre of Medical Education, School of Medicine, University of Dundee, United Kingdom; 2Department of Orthopaedic Surgery, Liaqat College of Medicine and Dentistry, Pakistan; 3Department of Medical Education, Dow University of Health Sciences, Pakistan; 4Suez Canal University, Egypt
Abstract
Introduction: The necessity for evaluating the effectiveness of medical education departments (DME) arises from the rapid technological advancements, frequent updates in healthcare paradigms and increasing societal demands. Such evaluations are crucial to understand how DMEs influence the future healthcare workforce and the quality of healthcare delivery. This research aims to explore the functions, procedures, and potential areas for innovation and improvement within DMEs.
Methods: A qualitative study was conducted at Liaquat College of Medicine and Dentistry’s Department of Medical Education, involving two focus groups of seven faculty members each. Participants included both junior and senior faculty. One session was held in person and the online one via Zoom. This was followed by inductive reflexive Thematic analysis.
Results: The study identified several strengths within the Liaquat College of Medicine and Dentistry DME, including robust faculty development programmes and strong student support services. However, areas of concern were highlighted such as research infrastructure and interdisciplinary connections. While faculty members expressed their satisfaction with the provided academic support services, they have reported the need for improving available research resources and faculty development programmes.
Conclusion: The study underscores the significant role of DMEs in medical education and suggests fostering joint research projects, encouraging faculty development, and enhancing student support services. Implementing these recommendations is crucial for advancing medical education and maintaining high standards of excellence. Continuous examination and implementation of these suggestions will ensure that DMEs can adapt to and meet the challenges of an ever-evolving healthcare landscape.
Keywords: Medical Education Department, Qualitative Study, Action Research, Focus Group
Practice Highlights
- Establish regular interdisciplinary workshops to foster innovative solutions in Medical Education.
- Provide training on innovative teaching techniques with emphasis on Technology Enhanced Learning integration.
- Introduce financial and non-financial rewards to motivate faculty for exceptional contribution.
- Provide comprehensive research training and encourage faculty participation in research activities.
- Develop a systematic student feedback process to continuously enhance teaching strategies and support services.
I. INTRODUCTION
A. Importance and Roles of Department of Medical Education (DME)
Medical education is an interdisciplinary specialty essential for the efficient operation of medical school. The roles of the Medical Education department vary based on institutional principles (Al Sheikh et al., 2022). A primary function of medical education department is to equip teaching staff with the necessary skills for effective role performance (Varpio et al., 2014). This includes course design experience, teaching practices, student assessment expertise, and instructional material development (Yusoff et al., 2014). A comprehensive faculty development programme, with clear goals and dedication, helps nurturing confident and competent staff who can support students’ career progression (Steinert et al., 2005).
The DME should also engage medical teachers in medical education research (Davis et al., 2005) and stimulate intra-departmental research and innovation. This can lead to proposals for action research to improve the teaching and learning environment (Yusoff et al., 2014). Additionally, the DME should organise educational activities that facilitate students’ engagement (Yusoff et al., 2014). These activities should address both personal and professional development, with emphasis on self-directed learning. The latter supports students to maximise their potential and strengthen their commitment to the medical field (Yusoff et al., 2010).
B. Worldwide Impact of DMEs in Medical Colleges
Departments of Medical Education (DMEs) have become integral in medical institutions globally (Alsheikh et al., 2022). DME evolution is shifting from the need to establish one to an increased public expectation (Davis et al., 2005).
The scope of DME activities varies expanding to undergraduates, postgraduates and continuing medical education. However, still flexibility is the key when planning for staffing at DME (Davis et al., 2005).
A study in four African medical universities revealed that medical education departments significantly enhance faculty abilities and student learning, support innovative teaching strategies, and advocate for improved assessment techniques (Kiguli-Malwadde et al., 2015). At the University of Michigan Medical School, DME has increased faculty engagement in scholarly activities through the Medical Education Scholars Program, fostering educational leadership and collaboration among faculty. This network has strengthened interdepartmental collaborations and reinforced education as a crucial element of faculty professional identity (Gruppen, 2004).
C. Context in Pakistan
In Pakistan, medical education requires significant reforms due to outdated practices and resource limitations (Nasim, 2011). Siddiqui & Shaikh (2014) noted a disconnect between basic and clinical sciences, with students lacking early patient contact. Khan et al. (2020) highlighted the need for systemic changes to maintain educational quality. Establishing DMEs is crucial for managing medical education systems (Latif & Wajid, 2018). However, challenges include inadequate infrastructure, qualified personnel, and resistance from management (Latif & Wajid, 2018). The Pakistan Medical and Dental Counsil (PMDC) and Higher Education Commission (HEC) have failed to provide clear guidelines for DME roles and responsibilities, complicating their establishment. The PMDC mandated the establishment of DMEs for accreditation in 2008, but many institutions struggle due to unclear guidelines and lack of skilled educators (Ali & Shamim, 2014). DMEs must develop strategic plans and align tasks with institutional goals. Faculty development programmes should be targeted and resource-efficient (Ali & Shamim, 2014). There is a significant need for faculty training in various skills, including self-directed learning, educational leadership, and research (Anwar & Humayun, 2015). Despite advancements, medical education and research in Pakistan are hindered by low funding and inadequate publication practices (Ghaffar et al., 2013). Improved assessment procedures and centralised evaluation offices are necessary for enhancing educational standards (Ali & Shamim, 2014).
At Liaquat College of Medicine and Dentistry (LCMD), institution under study, the DME was established in 2011. It oversees undergraduate and postgraduate education, continuing professional development, and dental education. The department is responsible for curriculum planning, design, implementation, and monitoring. It also supports educational innovation through instructional techniques and student skill development. The DME collaborates in research programme evaluation and quality assurance of assessments, aligning with local, regional, and international medical councils and accreditation bodies (LCMD, 2023). To enhance the department’s practices, an action research project was conducted to explore faculty perspectives on the DME’s role. Action research involves a cyclical process of collaboration for improving traditional procedures and is effective for identifying issues and generating workable solutions (Meyer, 2000). This study focuses on faculty expectations from the DME at LCMD and their suggestions for future endeavors.
Successful change involves consulting stakeholders to elucidate the need for improvement, considering their input in planning, and involving them as team members with full ownership (Lindberg, 1998). Understanding faculty perceptions is crucial for sustainable change, helping align faculty expectations with the department’s scope and filling any gaps (Khalid, 2013).
D. Need for Change
There is a practical-knowledge gap in the literature regarding the effectiveness of DMEs. While many studies focus on theoretical aspects and expected roles, there is a need for practical investigations into current practices (Al Shawwa, 2012; AlSheikh et al., 2022; Al-Wardy, 2008; Batool et al., 2018; Davis et al., 2005; Gruppen, 2008; Khalid, 2013; Kiguli-Malwadde et al., 2015). This study aims to address this gap by evaluating existing practices and identifying areas for improvement.
E. Research Questions
The study will address the following research questions:
- What is the faculty’s perception of the roles of the medical education department?
- What are the positive and negative experiences of working with a medical education department?
- How should the medical education department function in the future?
II. METHODS
This study adopts a qualitative approach which aligns with the study’s aim at addressing and improving current practices in the Department of Medical Education (DME). The latter requires a comprehensive understanding of the research context and culture to tailor recommendations effectively. Participatory epistemology was adopted emphasising that knowledge is co-constructed through cooperation rather than imparted by researchers (Torre, 2009). This approach values participants’ lived experiences and insights, aiming to produce context-specific and practical knowledge to address real-world issues. This collaborative method, particularly relevant in medical education, involves continuous interaction between researchers, academics, students, and administrators, fostering an environment where knowledge evolves through ongoing dialogue and mutual learning (Peralta, 2017).
The study employs an action research approach, which involves the researcher in a structured process of planning, implementing, and reflecting on actions to bring about positive changes in a specific context (Meyer, 2000). Action research is well-suited for exploring and improving practices within the DME, as it emphasises collaboration, reflection, and iterative cycles to understand and enhance real-world practices (Soh et al., 2011). This methodology is increasingly used in health and education settings due to its applicability, stakeholder involvement, and focus on continuous development.
Action research in this study involves two main stages. Stage 1 consists of focus group discussions with faculty members to gather their opinions and recommendations for improvement. Focus groups facilitate the exchange and development of ideas among participants, generating diverse viewpoints essential for the study’s goals (Cleary et al., 2014). Stage 2 involves collecting and analysing the potential solutions identified in the focus groups for feasibility, with recommendations shared with stakeholders for review and further action.
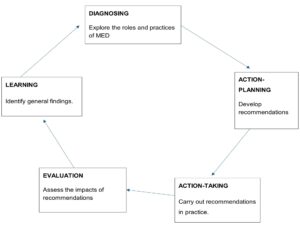
Figure 1. Five stages of action research (Everd, 1978)
A voluntary sampling technique was used to recruit participants. All faculty members were informed about the study’s objectives and invited to participate via email, resulting in 14 respondents. These participants were divided into two focus groups. Each focus group (n=7) included a mix of male and female participants with varying teaching experiences, ensuring a balanced representation of perspectives.
The first discussion took place in person, while the second was conducted online via Zoom. Each session lasted between 60 and 80 minutes, allowing for thorough exploration of the topics without causing participant fatigue (Tang et al., 1995). The discussions were guided by a set of open-ended questions designed to elicit detailed responses regarding the roles, practices, and improvement suggestions for the DME.
Transcripts of the discussions were analysed using thematic analysis (TA), using Braun & Clarke (2012). TA’s flexibility and accessibility make it suitable for novice researchers and for studies aiming to generate reports based on participants’ perceptions and viewpoints. The analysis followed Braun and Clarke’s (2006) six-phase framework, involving familiarisation with the data, generating initial codes, theme development, refining themes, defining themes and producing the report. This approach ensured a systematic and thorough examination of the data, leading to a comprehensive understanding of the issues and potential solutions within the DME.
A. Researcher Position and Ethical Considerations
Ethical approval was obtained from both Liaquat College of Medicine and Dentistry with the reference number IRB/M-000037/22 and the University of Dundee with reference number SMED REC 22/64. Participants were provided with an information sheet and consent form, ensuring informed consent, confidentiality, and anonymity (Illing, 2013). Data was securely stored, and pseudonyms were used to protect participants’ identities.
III. RESULTS
Two focus groups were conducted including 14 participants, 7 in each discussion. Thereafter transcripts were analysed using thematic analysis. Codes lead to themes, then further refinement was done, until finally reduced to 4 themes and 14 subthemes.

Figure 2. Mind map of themes and sub-themes
When presenting participants’ quotes “p5FG1” refers to participant number 5 in first focus group discussion.
A. Theme 1: Department Role and Activities
The Medical Education Department should encompass all important responsibilities such as teaching, research, and service providing, as well as supporting staff career development. However, the balance of these activities may vary within departments. When discussed the current state and impact of the medical education department in the college, the participants appreciated its role and activities. Hence two themes were generated.
1. Positive impact:
Participants highlighted the positive impact of the Medical Education Department and echoed department’s responsibility in improving teaching skills, supporting innovative approaches, encouraging interdisciplinary collaboration, and establishing a friendly and inclusive atmosphere for faculty members.
“The department’s current situation is pretty impressive. It has made great progress in improving medical education quality.” – p5FG1
“The department has played a critical role in raising medical education standards.” – p6FG2
2. Collaborative role:
Participants stressed the need for more communication and collaboration with other departments.
“While there have been some collaborative initiatives, I believe there is still potential for development.” – p6FG1
Especially, Collaborative opportunities for curriculum development among faculty members will not only bring diverse expertise, comprehensive approach, innovation, and creativity but will also enhance their engagement and sense of ownership.
“They should hold brainstorming sessions, curriculum mapping exercises, and curriculum review meetings to discuss ideas and viewpoints.” – p2FG2
B. Theme 2: Faculty Development
Faculty development initiatives planned by the college’s medical education department seem satisfactory. However, faculty members stressed the need to include innovative and trendy topics i.e., creative pedagogy, technology informed teaching practices and leadership and communication skills for the workshops.
1. Need for training for professional excellence:
The faculty believes that they have a legitimate need for pedagogical training.
“As I have decided to pursue my carrier as a medical teacher and for that yes I need to develop some pedagogical knowledge and skills.” – p3FG1
“We’re eager to succeed in our professions, these training can positively impact our carriers.” – p5FG2
2. Nature and scope of activities:
Participants highlighted the need to introduce new and updated topics in relevance faculty development activities (FDA) with emphasis on participants’ engagement and interactivity.
“But sometimes I feel that these workshops should also consider our educational needs like research and leadership skills.” – p4FG1
“More interactive and active learning techniques would help us understand the content and would be more beneficial in its application.” – p7FG1
3. Motivation to participate:
Most participants thought that faculty members’ contributions to these faculty development events should be acknowledged in some way, hence motivating them to participate.
“Like for young doctors like me, who are struggling to find some balance between family and work, the institute must consider some incentives or recognitions in any form. That I think can keep us motivated.” – p1FG1
4. Roadblocks to faculty development:
Despite the advantages of faculty development workshops mentioned, participants still highlighted some barriers to their development i.e., duration, challenging commitments.
“After the hectic clinical schedule, I sometimes literally drag myself for the workshops. I would suggest planning short duration workshops.” – p6FG1
“After fulfilling my teaching and clinical commitments, despite understanding its (FDA) importance, I hardly wish to spare any time for it.” – p3FG2
5. Challenges to the adaptation to new practices:
Adaptation to new practices can occur at various levels like content, pedagogical and assessment adaptations. Participants focused on pedagogical training, especially for the introduction of new integrated curriculum. One of the members responded as follows.
“…then there is the issue of matching our existing resources to the new curriculum’s requirements. This requires reconsideration of our lesson ideas, assessments, and even classroom layouts.” – p4FG2
C. Theme 3: Inadequate Contributions Towards Research
MEDs play an important role in creating a culture of research (i.e. prevailing attitudes, values, and practices regarding research activities) by innovating, developing new methodologies to medical education, and disseminating their findings (Al-Wardy, 2008). However, the participants seem quite unsatisfied with the current research culture of the institute.
“Well! I think this needs attention, as the research resources are not adequate.” – p5FG1
1. Workload balance:
Faculty find it difficult to balance between clinical and teaching responsibilities while conducting research work. Research work needs more commitment.
“The rigorous clinical workload leaves us with little time and energy to devote to research. Balancing clinical commitments and research can be difficult.” – p6FG2
2. Training and skills:
They also feel the need for research support offices to help and motivate the researchers and teach them research skills like conducting sound literature search strategies, data collection, analysis etc.
“I can see that faculty members who do not obtain proper research training usually have to struggle to initiate and carry out research projects.” – p7FG1
3. Limited resources:
Resources include financial as well as research resources. They feel that restricted financial and research resources (databases, journals, and libraries) are big impediments to the development of research culture in their institute.
“Faculty and students encounter problems performing strong investigations and generating significant findings without access to advanced laboratory equipment, research databases, and specialised research rooms.” – p4FG2
4. Motivation for research:
The institutional culture of a medical college can influence the emphasis and support for research efforts. If the college does not emphasise research or does not have a supportive research culture, faculty members may not receive appropriate recognition, incentives, or resources to engage in research. This can demotivate staff and result in low quality of research work. For instance, one of the participants said:
“Be it any field, lack of incentives, awards, and acknowledgment for research accomplishments might discourage academics and students from actively participating in research activities.” – p7FG2
D. Theme 4: Student Support Services
Planning and providing instructional activities that encourage students’ involvement in learning is another duty of the Medical Education Department. Yusoff. et. al (2014) argued that, to guarantee that medical students are engaged in their study, it is necessary to prepare and teach them to do so. Thus, at both the personal and professional levels, student development activities are essential and fundamental part of nurturing and preparing students for learning in the medical field.
1. Academic support:
The faculty agreed that students needed help and direction in their academic endeavours and appreciate the students’ services of the department.
“The current state of advising services, in my opinion, is fairly good. The department includes resolute advisers and mentors who help students with many aspects of their academic and personal lives. They are easily accessible and eager to respond to students’ problems and questions.” – p1FG1
2. Advisory of study:
The conversation emphasised the significance of addressing students’ emotional and mental health.
“There is a need for improved mental health support. Additional information and guidance on managing stress, building resilience, and obtaining counselling services would be great.” – p5FG2
The importance of educating medical students for their future careers options was underlined by the faculty.
3. Communication and feedback:
Establishing a successful mentoring programme requires thorough programme evaluation. As the programme’s focus, students’ expectations must be considered while evaluating the programme’s effectiveness in terms of its outcomes (Jayalakshmi et. al., 2011). Participants strongly felt that there is a need for a formalised feedback process to collect student perspectives and issues.
“Clearer communication lines, faster response times, and more proactive guidance suited to students’ specific needs and objectives would be advantageous.” – p4FG1
IV. DISCUSSION
A. Staff Perception of the Roles of the Medical Education Department
Staff generally perceive the Medical Education Department (MED) positively, particularly regarding its support for faculty development and student services. Faculty members appreciate the department’s commitment to assisting in teaching initiatives by offering tools, courses, and training opportunities, which help them enhance their teaching skills and stay current with pedagogical practices. This support contributes to providing high-quality education to students, contrasting findings by Latif & Wajid (2018), who reported difficulties in establishing DMEs due to a lack of consensus on their roles. Participants noted that MED encourages conference attendance and fosters professional development, benefiting both individual careers and institutional networking, research collaboration, and communication skills (Kamal et al., 2022). Additionally, MED’s role in organising extracurricular activities and mentorship programmes maximises students’ educational experiences, promoting personal development and teamwork (Yusoff et al., 2014). Khalid (2013) and Kiguli-Malwadde et al. (2015) found faculty viewing MED as a positive change and an agent of educational innovation. Rahman et al. (2019) reported faculty transfer knowledge from MED activities and use them in pedagogical and assessment techniques, hence classified them as beneficial activities. However, it was reported in other studies that faculty felt threatened by MED’s activities, perceiving them as taking over the curriculum (Batool, 2018).
Despite these positives, there is limited awareness among administration and students about MED’s role, leading to under-utilisation of its resources and lack of collaboration. Hence DMEs should actively promote their services through newsletters, workshops, and engagement with student and faculty organisations. Raising awareness ensures that MED’s resources and support reach those who can benefit, and therefore improve the educational experience for all involved stakeholders (Rahman et al., 2019; Khalid, 2013).
B. Staff Positive and Negative Experiences While Working with a Medical Education Department
Faculty members at LCMD view faculty development activities positively, appreciating their focus on teaching methods, assessment techniques, and curriculum development. Junior faculty members, in particular, value these activities as they transition from students to competent instructors, developing teaching abilities, communication skills, and interdepartmental collaboration through these programmes (Thorndyke et al., 2006; Whitcomb, 2004).
However, barriers include time constraints due to faculty members’ multiple responsibilities, passive learning methods in workshops, and a lack of incentives for participation. Studies in India found similar limitations, with debates on the effectiveness of incentives for attending workshops (Adkoli & Sood, 2009; Singh et al., 2008; Srinivas & Adkoli, 2009). While some argue for monetary incentives, others caution against misaligned motivations and ethical issues (Jessani et al., 2020).
Participants expressed dissatisfaction with research activities, with the limited research funding, lack of institutional support, and insufficient collaboration. Medical education research is essential for understanding teaching and learning in medicine, fostering innovation, and developing critical thinking skills (Magan, 2018; Susiani et al., 2018). Challenges include securing funding, lack of resources, and institutional prioritisation of clinical skills over educational research (Ghaffar et al., 2013; Sabzwari et al., 2009).
Regarding student services, faculty members are satisfied with advisory and mentoring activities but suggest improvements. Effective mentoring involves role modeling, career development advice, and direct interaction, evaluated through student feedback (Nimmons et al., 2019). The Kirkpatrick model offers a framework for assessing mentoring programme effectiveness, though evaluations should extend to the organisational level (Nimmons et al., 2019; Smidt et al., 2009).
C. How Should the Medical Education Department Function in the Future?
To address time constraints, MED should offer flexible scheduling for faculty development activities, including evening and weekend classes, and online resources. Integrating these activities into ongoing events and establishing mentorship programmes can further support faculty development. Journal clubs can promote knowledge exchange and research interest, addressing time constraints through peer group discussions (Bhattacharya, 2017; Linzer et al., 1988).
Active learning methods, such as workshops, case studies, and role-play, should be incorporated into faculty development programmes, underpinned by Knowles’ adult learning theory principles to promote internal motivation and self-directed learning (Kaufman, 2003; Norcini et al., 2005; Steinert et al., 2000). Monetary incentives and recognition for contributions should be allocated to motivate participation, with a framework for regular evaluation of teachers’ performance (Adkoli & Sood, 2009; Shah et al., 2018; Srinivas & Adkoli, 2009).
Customised workshops, though challenging, can be facilitated through self-assessed pathways like the COINNS model, identifying key issues and opportunities for professional development (Swanwick & McKimm, 2010). Research training, financial support, and acknowledgment for research accomplishments are crucial for fostering a research culture. Creating research support offices can streamline research processes, mentor researchers, uncover funding opportunities, and support collaborative research (Albanese et al., 2001; Eder & Pierce, 2011; Gisondi et al., 2022).
For student support, more academic services like stress management and study skills activities are needed. Ensuring student engagement and development through well-planned instructional activities can improve outcomes (Prebble et al., 2004; Yusoff et al., 2014). Resilience workshops and cognitive-behavioral training can address the mental and physical health pressures faced by medical students (Rogers, 2016).
V. CONCLUSION
This action research study highlights several key findings and recommendations based on faculty perceptions of their medical education department’s practices and policies. Faculty members expressed a positive attitude towards current policies, indicating a strong foundation for further advancements. However, the need for greater collaboration through multidisciplinary projects and cross-departmental connections was emphasised to enhance overall efficacy.
While existing faculty development programmes meet some demands, a stronger focus on motivational rewards is necessary to maintain participation and commitment. Incentives or acknowledgment for outstanding achievements can renew faculty devotion to departmental goals. Faculty development should also include interactive workshops on advanced pedagogical methods, technological integration, interdisciplinary teaching partnerships, and assessment strategies. These workshops ensure that faculty stay updated with educational advancements, benefiting both teachers and students.
Concerns about workload and its impact on research and scholarship were noted. Addressing the lack of research-related training and resources is crucial to fostering an academic culture of inquiry. Providing skill-enhancement programmes and seeking additional funding can empower faculty to pursue research initiatives.
Lastly, while faculty are satisfied with academic mentoring and support services, the student feedback system needs improvement. A more organised and proactive mechanism is required to effectively capture student insights and ensure continuous improvement.
A. Study Recommendations
Study recommends encouraging regular interactions with other departments via interdisciplinary/ multidisciplinary workshops; providing innovative pedagogical techniques; fostering Financial and Non-Financial Incentives. The latter could be planned by implementing a merit-based system, which rewards exceptional contributions with stipends, bonuses, and research funding. Recognising outstanding faculty annually for their achievements is a key in inspiring others and igniting their motivation. Moreover, aiming at improving DME practices, institutional research profile should be strengthened by organising research activities focused on grant writing, research publication, data analysis.
B. Study Limitations
Being localised to a single institute limits data generalisability. The findings are specific to unique context and may not apply to other institutions (Braydon-Miller et al., 2003). Voluntary faculty participation introduces selection bias, as the sample may not represent all faculty viewpoints (Gill, 2020; Berndt, 2020). Additionally, the study focused on faculty opinions, potentially missing insights from other stakeholders such as students, graduates, and recruiters, which could provide a more comprehensive understanding of the department’s strengths and areas for improvement.
Notes on Contributors
Dr Juveria Arjumand contributed to conceived the study, drafted the study proposal, conducted online Zoom focus group discussion, analysed the data as per her master proposal, and prepared the manuscript for submission.
Dr Syed Muhammad Azfar obtained ethical approval and assisted in conducting focus group discussion and data collection.
Dr Rubaba Azim assisted in conducting focus group discussions and data collection.
Dr Rania Alkhadragy reviewed the study proposal, planned for study design, followed data collection and analysis, gave critical review and edited the final version of the manuscript.
All authors read and approved the final manuscript.
Ethical Approval
Ethical approval was issued from Liaquat College of Medicine and Dentistry with the reference number IRB/M-000037/22 and from University of Dundee with the reference number SMED REC 22/64.
Data Availability
All relevant data are within the manuscript. Data has sensitive information form participants’ quotes that should not be publicly available.
Acknowledgement
We would like to thank all the faculty members at LCMD who participated in the study.
Funding
The author did not receive any funding to conduct this study.
Declaration of Interest
All authors have no conflict of interest.
References
Adkoli, B. V., & Sood, R. (2009). Faculty development and medical education units in India: A survey. National Medical Journal of India, 22(1), 28-32. https://pubmed.ncbi.nlm.nih.gov/19761158/
Al Shawwa, L. A. (2012). The establishment and roles of the medical education department in the faculty of medicine, King Abdul Aziz University, Jeddah Saudi Arabia. Oman Medical Journal, 27(1), 4. https://doi.org/10.5001/omj.2012.02
Albanese, M. A., Dottl, S., & Nowacek, G. A. (2001). Offices of research in medical education: Accomplishments and added value contributions. Teaching and Learning in Medicine, 13(4), 258-267. https://doi.org/10.1207/s15328015tlm1304_08
Ali, S. M., & Shamim, M. S. (2014). Way forward for departments of medical education in Pakistan. Journal Pakistan Medical Association, 64(7), 732-733. https://doi.org/10.12669/pjms.314.8575
AlSheikh, M. H., Zaini, R., Abdalla, M. E., & Magzoub, M. E. (2022). The wicked role of the medical education department. Health Professions Education, 8(1), 3-8. https://doi.org/10.55890/2452-3011.1014
Al-Wardy, N. M. (2008). Medical education units: History, functions, and organisation. Sultan Qaboos University Medical Journal, 8(2), 149.
Anwar, M. I., & Humayun, A. (2015). Faculty development – Looking through different lenses. Pakistan Armed Forces Medical Journal, 65(1), 110-117. https://pafmj.org/PAFMJ/article/view/701
Batool, S., Raza, M. A., & Khan, R. A. (2018). Roles of medical education department: What are expectations of the faculty? Pakistan Journal of Medical Sciences, 34(4), 864. https://doi.org/10.12669/pjms.344.14609
Berndt, A. E. (2020). Sampling methods. Journal of Human Lactation, 36(2), 224-226. https://doi.org/10.1177/0890334420906850
Bhattacharya, S. (2017). Journal club and post-graduate medical education. Indian Journal of Plastic Surgery, 50(3), 302-305. https://doi.org/10.4103/ijps.ijps_222_17
Braun, V., & Clarke, V. (2006). Using thematic analysis in psychology. Qualitative Research in Psychology, 3(2), 77-101. https://doi.org/10.1191/1478088706qp063oa
Braun, V., & Clarke, V. (2012). Thematic analysis. In H. Cooper (Ed.), APA handbook of research methods in psychology (Vol. 2, pp. 57-71). American Psychological Association. https://psycnet.apa.org/doi/10.1037/13620-004
Brydon-Miller, M., Greenwood, D., & Maguire, P. (2003). Why action research? Action Research, 1(1), 9-28. https://doi.org/10.1177/14767503030011002
Cleary, M., Horsfall, J., & Hayter, M. (2014). Data collection and sampling in qualitative research: Does size matter? Journal of Advanced Nursing, 70(3), 473-475. https://doi.org/10.1111/jan.12163
Davis, M. H., Karunathilake, I., & Harden, R. M. (2005). AMEE education guide no. 28: The development and role of departments of medical education. Medical Teacher, 27(8), 665-675. https://doi.org/10.1080/01421590500398788
Eder, M., & Pierce, J. R. (2011). Innovations in faculty development: Study of a research assistance unit designed to assist clinician-educators with research. Southern Medical Journal, 104(9), 647-650. https://doi.org/10.1097/smj.0b013e3182294e82
Evered, R. D., & Susman, G. I. (1978). An assessment of the scientific merits of action research. Administrative Science Quarterly, 23(4), 582-603. https://doi.org/10.2307/2392581
Ghaffar, A., Zaidi, S., Qureshi, H., & Hafeez, A. (2013). Medical education and research in Pakistan. The Lancet, 381(9885), 2234-2236. https://doi.org/10.1016/s0140-6736(13)60146-4
Gill, S. L. (2020). Qualitative sampling methods. Journal of Human Lactation, 36(4), 579-581. https://doi.org/10.1177/0890334420949218
Gisondi, M. A., Michael, S., Li-Sauerwine, S., Brazil, V., Caretta-Weyer, H. A., Issenberg, B., … & Chan, T. M. (2022). The purpose, design, and promise of medical education research labs. Academic Medicine, 97(9), 1281-1288. https://doi.org/10.1097/acm.0000000000004746
Gruppen, L. (2008). Creating and sustaining centres for medical education research and development. Medical Education, 42(2), 121-123. https://doi.org/10.1111/j.1365-2923.2007.02931.x
Gruppen, L. D. (2004). The department of medical education at the University of Michigan Medical School: A case study in medical education research productivity. Academic Medicine, 79(10), 997-1002. https://doi.org/10.1097/00001888-200410000-00023
Illing, J. (2013). Thinking about research: Theoretical perspectives, ethics, and scholarship. In T. Swanwick (Ed.), Understanding medical education: Evidence, theory, and practice (2nd ed., pp. 331-348). Chichester: Wiley Blackwell. https://doi.org/10.1002/9781118472361.ch24
Jessani, N. S., Valmeekanathan, A., Babcock, C. M., & Ling, B. (2020). Academic incentives for enhancing faculty engagement with decision-makers – Considerations and recommendations from one School of Public Health. Humanities and Social Sciences Communications, 7(1), 1-13. https://doi.org/10.1057/s41599-020-00629-1
Kamal, M., Bhargava, S., & Katyal, S. (2022). Role of conferences and continuing medical education (CME) in post-graduate anaesthesia education. Indian Journal of Anaesthesia, 66(1), 82. https://doi.org/10.4103/ija.ija_1102_21
Kaufman, D. M. (2003). Applying educational theory in practice. British Medical Journal, 326(7382), 213-216. https://doi.org/10.1136/bmj.326.7382.213
Khalid, T. (2013). Faculty perceptions about roles and functions of a department of medical education. Journal of College of Physicians and Surgeons Pakistan, 23(1), 56-61. https://pesquisa.bvsalud.org/portal/resource/pt/emr-140581
Khan, A. W., Sethi, A., Wajid, G., & Yasmeen, R. (2020). Challenges towards quality assurance of basic medical education in Pakistan. Pakistan Journal of Medical Sciences, 36(2), 4. https://doi.org/10.12669/pjms.36.2.1319
Kiguli-Malwadde, E., Talib, Z. M., Wohltjen, H., Connors, S. C., Gandari, J., Banda, S. S., & Van Schalkwyk, S. C. (2015). Medical education departments: A study of four medical schools in Sub-Saharan Africa. British Medical Council medical education, 15(1), 1-9. https://doi.org/10.1186/s12909-015-0398-y
Latif, M. Z., & Wajid, G. (2018). Reforming medical education in Pakistan through strengthening departments of medical education. Pakistan Journal of Medical Sciences, 34(6), 1439. https://doi.org/10.12669/pjms.346.15942
Liaquat College of Medicine and Dentistry [LCMD]. (2023). Department of health professions education. Retrieved January 22, 2023, from https://www.lcmd.edu.pk/dhpe
Lindberg, M. A. (1998). The process of change: Stories of the journey. Academic Medicine, 73(9), S4-S10. https://doi.org/10.1097/00001888-199809000-00029
Linzer, M., Brown, J., Frazier, L., Delong, E., & Siegel, W. (1988). Impact of a medical journal club on house-staff reading habits, knowledge, and critical appraisal skills. A randomized control trials. The Journal of the American Medical Association, 260(17), 2537-2541. https://doi.org/10.1001/jama.260.17.2537
Magan, D. (2018). Importance of research in medical education. Journal of Medical Education, 17(3). https://brieflands.com/articles/jme-105647
Meyer, J. (2000). Using qualitative methods in health-related action research. British Medical Journal, 320(7228), 178-181. https://doi.org/10.7748/nop.12.1.22.s12
Nasim, M. (2011). Medical education needs to change in Pakistan. Journal of the Pakistan Medical Association, 61(8), 808. https://europepmc.org/article/med/22356007
Nimmons, D., Giny, S., & Rosenthal, J. (2019). Medical student mentoring programs: Current insights. Advances in Medical Education and Practice, 10, 113-123. https://doi.org/10.2147/amep.s154974
Norcini, J., Burdick, W., & Morahan, P. (2005). The FAIMER Institute: Creating international networks of medical educators. Medical Teacher, 27(3), 214-218. https://doi.org/10.1080/01421590500126379
Peralta, K. J. (2017). Toward a deeper appreciation of participatory epistemology in community-based participatory research. PRISM: A Journal of Regional Engagement, 6(1), 4. https://encompass.eku.edu/prism/vol6/iss1/4/
Prebble, T., Hargraves, H., Leach, L., Naidoo, K., Suddaby, G., & Zepke, N. (2004). Impact of student support services and academic development programmes on student outcomes in undergraduate tertiary study: A synthesis of the research: Report to the Ministry of Education. Wellington: Ministry of Education. https://rb.gy/fd8mpf
Rahman, S., Talukder, M. H. K., & Alam, K. K. (2019). Activities of Medical Education Unit (MEU) in medical colleges of Bangladesh and some challenges faced. Bangladesh Journal of Medical Education, 10(2), 12-18. https://doi.org/10.3329/bjme.v10i2.44637
Rogers, D. (2016). Which educational interventions improve healthcare professionals’ resilience? Medical Teacher, 38(12), 1236-1241. https://doi.org/10.1080/0142159x.2016.1210111
Sabzwari, S., Kauser, S., & Khuwaja, A. K. (2009). Experiences, attitudes and barriers towards research amongst junior faculty of Pakistani medical universities. BMC Medical Education, 9(1), 1-7. https://doi.org/10.1186/1472-6920-9-68
Shah, N., Tabassum, A., & Shah, N. (2018). A needs assessment for faculty development at two medical colleges of Dow University of Health Sciences, Karachi. Pakistan Journal of Medical Sciences, 34(6), 1386. https://doi.org/10.12669/pjms.346.16302
Siddiqui, F. G., & Shaikh, N. A. (2014). Challenges and issues in medical education in Pakistan. Journal of Liaquat University of Medical Health Sciences, 13(3), 91-92.
Singh, T., Bansal, P., & Sharma, M. (2008). A need and necessity for faculty development: The role of medical education units in the Indian context. South East Asian Journal of Medical Education, 2(1), 2-6. https://doi.org/10.4038/seajme.v2i1.484
Smidt, A., Balandin, S., Sigafoos, J., & Reed, V. A. (2009). The Kirkpatrick model: A useful tool for evaluating training outcomes. Journal of Intellectual and Developmental Disability, 34(3), 266-274. https://doi.org/10.1080/13668250903093125
Soh, K. L., Davidson, P. M., Leslie, G., & Rahman, A. B. A. (2011). Action research studies in the intensive care setting: A systematic review. International Journal of Nursing Studies, 48(2), 258-268. https://doi.org/10.1016/j.ijnurstu.2010.09.014
Srinivas, D. K., & Adkoli, B. V. (2009). Faculty development in medical education in India: The need of the day. Al Ameen Journal of Medical Sciences, 2(1), 6-13. https://www.cabidigitallibrary.org/doi/full/10.5555/20103114268
Steinert, Y., Cruess, S., Cruess, R., & Snell, L. (2005). Faculty development for teaching and evaluating professionalism: From programme design to curriculum change. Medical Education, 39(2), 127-136. https://doi.org/10.1111/j.1365-2929.2004.02069.x
Susiani, T. S., Salimi, M., & Hidayah, R. (2018). Research based learning (RBL): How to improve critical thinking skills? Social Human Science Web of Conferences, 42, 00042. https://doi.org/10.1051/shsconf/20184200042
Tang, K. C., Davis, A., Sullivan, S., & Fisher, J. (1995). A review of 5 existing guidelines for planning focus groups in GP research. Australian Family Physician, 24(2), 184-186. https://europepmc.org/article/med/7880138
Thorndyke, L. E., Gusic, M. E., George, J. H., Quillen, D. A., & Milner, R. J. (2006). Empowering junior faculty: Penn State’s faculty development and mentoring program. Academic Medicine, 81(7), 668-673. https://doi.org/10.1097/01.acm.0000232424.88922.df
Torre, M. E. (2009). Participatory action research and critical race theory: Fueling spaces for nos-otras to research. The Urban Review, 41, 106-120. https://doi.org/10.1007/s11256-008-0097-7
Varpio, L., Bidlake, E., Humphrey-Murto, S., Sutherland, S., & Hamstra, S. J. (2014). Key considerations for the success of medical education research and innovation units in Canada: Unit director perceptions. Advances in Health Sciences Education, 19(3), 361-377. https://doi.org/10.1007/s10459-013-9479-z
Whitcomb, M. E., & Cohen, J. J. (2004). The future of primary care medicine. New England Journal of Medicine, 351(7), 710-712.
Wolcott, L. L., & Betts, K. S. (1999). What’s in it for me? Incentives for faculty participation in distance education. Journal of Distance Education, 14(2), 34-49. https://www.ijede.ca/index.php/jde/article/download/156/340?inline=1
Yusoff, M. S. B., Rahim, A. F. A., & Jaafar, R. (2014). Medical education department roles and initiatives towards achieving APEX agenda. Education in Medicine Journal, 6(2), e1-e7. https://doi.org/10.5959/eimj.v6i2.261
Yusoff, M. S. B., Rahim, A. F. A., Noor, A. R., Yaacob, N., & Hussin, Z. (2010). Evaluation of medical students’ perception towards the Big Sib Programme in the School of Medical Sciences, USM. Education in Medicine Journal, 2(1), e2-e11.
*Dr Rania Alkhadragy
University of Dundee,
Nethergate Dundee,
Scotland, United Kingdom
Email: ryalkhadragy@dundee.ac.uk
Announcements
- Best Reviewer Awards 2025
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2025.
Refer here for the list of recipients. - Most Accessed Article 2025
The Most Accessed Article of 2025 goes to Analyses of self-care agency and mindset: A pilot study on Malaysian undergraduate medical students.
Congratulations, Dr Reshma Mohamed Ansari and co-authors! - Best Article Award 2025
The Best Article Award of 2025 goes to From disparity to inclusivity: Narrative review of strategies in medical education to bridge gender inequality.
Congratulations, Dr Han Ting Jillian Yeo and co-authors! - Best Reviewer Awards 2024
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2024.
Refer here for the list of recipients. - Most Accessed Article 2024
The Most Accessed Article of 2024 goes to Persons with Disabilities (PWD) as patient educators: Effects on medical student attitudes.
Congratulations, Dr Vivien Lee and co-authors! - Best Article Award 2024
The Best Article Award of 2024 goes to Achieving Competency for Year 1 Doctors in Singapore: Comparing Night Float or Traditional Call.
Congratulations, Dr Tan Mae Yue and co-authors! - Best Reviewer Awards 2023
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2023.
Refer here for the list of recipients. - Most Accessed Article 2023
The Most Accessed Article of 2023 goes to Small, sustainable, steps to success as a scholar in Health Professions Education – Micro (macro and meta) matters.
Congratulations, A/Prof Goh Poh-Sun & Dr Elisabeth Schlegel! - Best Article Award 2023
The Best Article Award of 2023 goes to Increasing the value of Community-Based Education through Interprofessional Education.
Congratulations, Dr Tri Nur Kristina and co-authors! - Best Reviewer Awards 2022
TAPS would like to express gratitude and thanks to an extraordinary group of reviewers who are awarded the Best Reviewer Awards for 2022.
Refer here for the list of recipients. - Most Accessed Article 2022
The Most Accessed Article of 2022 goes to An urgent need to teach complexity science to health science students.
Congratulations, Dr Bhuvan KC and Dr Ravi Shankar. - Best Article Award 2022
The Best Article Award of 2022 goes to From clinician to educator: A scoping review of professional identity and the influence of impostor phenomenon.
Congratulations, Ms Freeman and co-authors.









